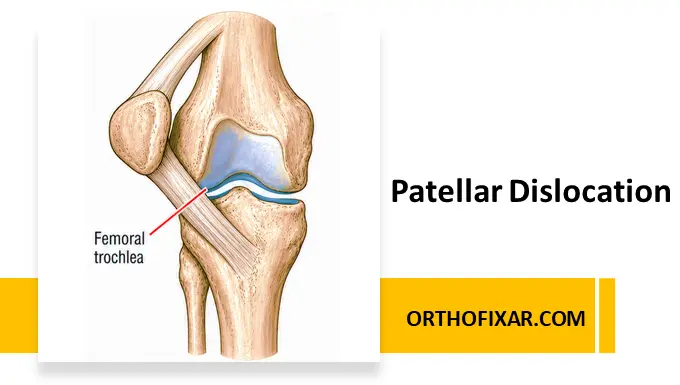
Traumatic patellar dislocation is a common knee injury, particularly affecting young active individuals and females. It occurs when the patella (kneecap) is displaced from its normal position within the trochlear groove of the femur. Understanding its mechanism, risk factors, and management is essential for preventing recurrence and long-term complications.
Epidemiology of Patellar Dislocation
Patellar dislocation is more common in:
- Women (due to increased physiological ligamentous laxity)
- Patients with connective tissue disorders such as Ehlers–Danlos syndrome and Marfan syndrome
- Individuals with generalized joint hypermobility
Younger patients, especially adolescents and athletes, are at higher risk of recurrent instability.
Anatomy and Risk Factors
Q Angle and Patellar Stability
The Q angle plays a critical role in patellar tracking. It is formed by:
- A line from the anterior superior iliac spine (ASIS) to the center of the patella
- A line from the patella to the tibial tubercle
An increased Q angle creates a lateral vector force, predisposing the patella to dislocation.
Predisposing Factors
- Patella alta (high-riding patella)
- Trochlear dysplasia (shallow groove)
- Vastus medialis obliquus (VMO) weakness or hypoplasia
- Tight lateral retinaculum
- Congenital abnormalities
See Also: Patellar Instability
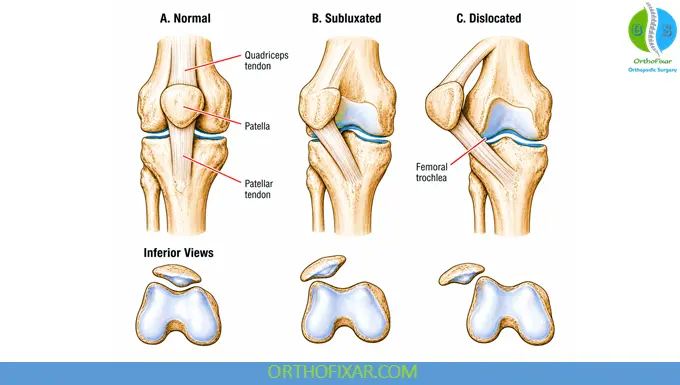
Mechanism of Injury
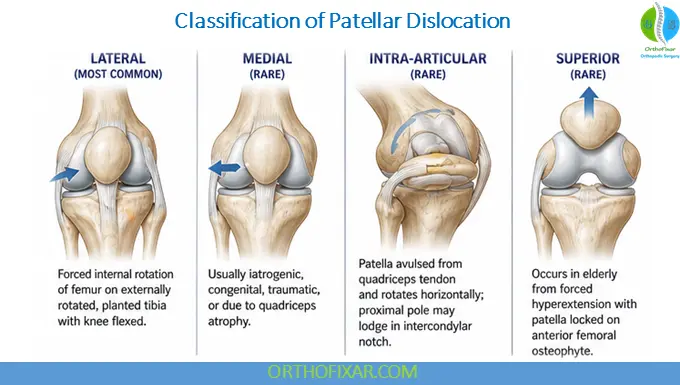
Patellar dislocations are classified based on direction:
1. Lateral Patellar Dislocation (Most Common)
- Occurs due to forced internal rotation of the femur on an externally rotated, planted tibia with the knee flexed
- Associated with ~5% risk of osteochondral fractures
2. Medial Patellar Dislocation (Rare)
- Usually iatrogenic (post-surgical)
- Can also result from trauma or quadriceps atrophy
3. Intra-articular Dislocation
- Rare injury, typically in adolescents
- Patella rotates horizontally after quadriceps tendon avulsion
- The proximal pole may become lodged in the intercondylar notch
4. Superior Patellar Dislocation
- Seen in elderly patients
- Caused by hyperextension injuries
- Patella becomes locked on an anterior femoral osteophyte
See Also: Patellar Tendinitis (Jumper’s knee)
Clinical Evaluation
Acute (Unreduced) Dislocation
Patients typically present with:
- Severe knee pain
- Inability to flex the knee
- Difficulty bearing weight
- Hemarthrosis (joint swelling)
- Visible or palpable patellar displacement
Lateral Dislocation Findings
- Tenderness over the medial retinaculum
- Injury to the medial patellofemoral ligament (MPFL)
Apprehension Test
In recurrent or reduced cases:
- Lateral pressure on the patella causes fear of redislocation
- Patient resists movement with quadriceps contraction
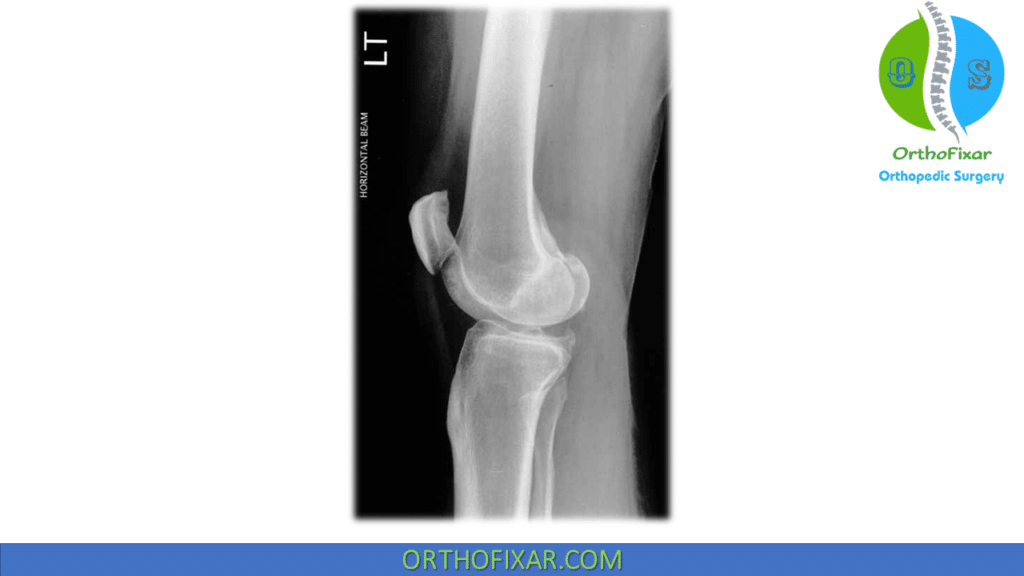
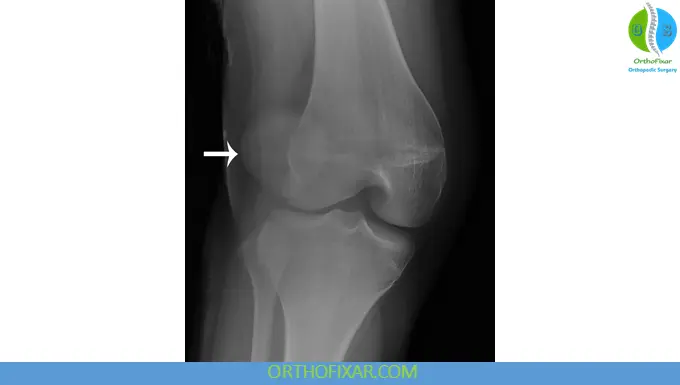
Radiology
Standard Imaging
- Anteroposterior (AP) view
- Lateral view
- Axial (sunrise) view
Axial View Techniques
- Hughston view (55° flexion): evaluates sulcus angle
- Merchant view (45° flexion): assesses congruence angle
- Laurin view (20° flexion): measures patellofemoral alignment
Assessment of Patellar Height
- Insall–Salvati Ratio:
- Normal: 0.8–1.2
- 1.2 → Patella alta
- <0.8 → Patella baja
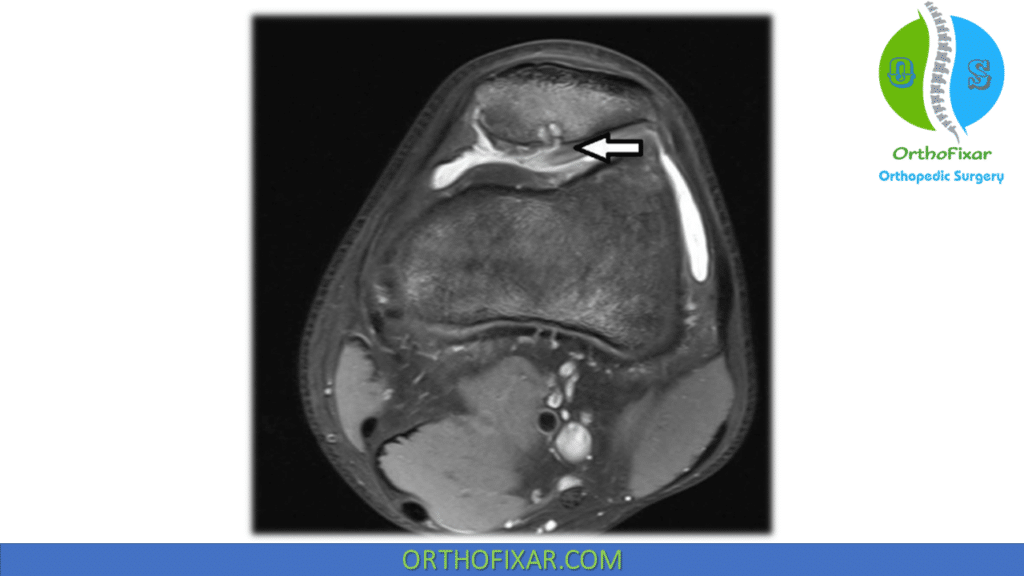
MRI Indications
MRI is recommended when:
- Osteochondral injury is suspected
- Soft tissue damage (e.g., MPFL tear) needs evaluation
Studies show 39–71% incidence of chondral or osteochondral injury after acute dislocation.
Classification of Patellar Dislocation
Patellar dislocations can be categorized as:
- Acute vs chronic (recurrent)
- Reduced vs unreduced
- Congenital vs acquired
- Direction-based (lateral, medial, intra-articular, superior)
Patellar Dislocation Treatment
Nonoperative Management (First-Line)
- Closed reduction (if dislocated)
- Immobilization in knee extension using brace or cast
- Weight-bearing allowed in extension
Rehabilitation Timeline:
- 0–3 weeks: Immobilization
- 3–6 weeks: Gradual knee flexion
- 6–8 weeks: Brace weaning + strengthening
Focus on:
- Quadriceps strengthening (especially VMO)
- Restoring range of motion
- Preventing recurrence
Surgical Management
Indicated in:
- Recurrent dislocations
- Displaced osteochondral fractures
- Failure of conservative treatment
Surgical Options:
- MPFL reconstruction (preferred over repair due to better outcomes)
- Lateral release (for lateral tightness and tilt)
- Medial plication
- Proximal realignment procedures
- Distal realignment (tibial tubercle transfer)
No single procedure fits all—treatment is individualized.
Complications
1. Recurrent Dislocation
- More common in patients <20 years
- Often requires surgical stabilization
2. Loss of Knee Motion
- Caused by prolonged immobilization or arthrofibrosis
3. Patellofemoral Pain Syndrome
- Due to cartilage (chondral) damage
- May persist long-term
Conclusion
Traumatic patellar dislocation is a multifactorial injury influenced by anatomical, biomechanical, and traumatic factors. Early diagnosis, appropriate imaging, and structured rehabilitation are essential for optimal outcomes. While most cases are managed conservatively, recurrent instability often necessitates surgical intervention, particularly MPFL reconstruction.

References & More
- Mercer’s Textbook of Orthopaedics and Trauma, Tenth edition.
- Sallay PI, Poggi J, Speer KP, et al. Acute dislocation of the patella: a correlative pathoanatomic study. American Journal of Sports Medicine 1996;24:52. PubMed
- Nsouli AZ, Nahabedian AM. Intraarticular dislocation of the patella. Journal of Trauma 1988;28:256. PubMed
- Cash JD, Hughston JC. Treatment of acute patellar dislocation. American Journal of Sports Medicine 1988;16:244. PubMed