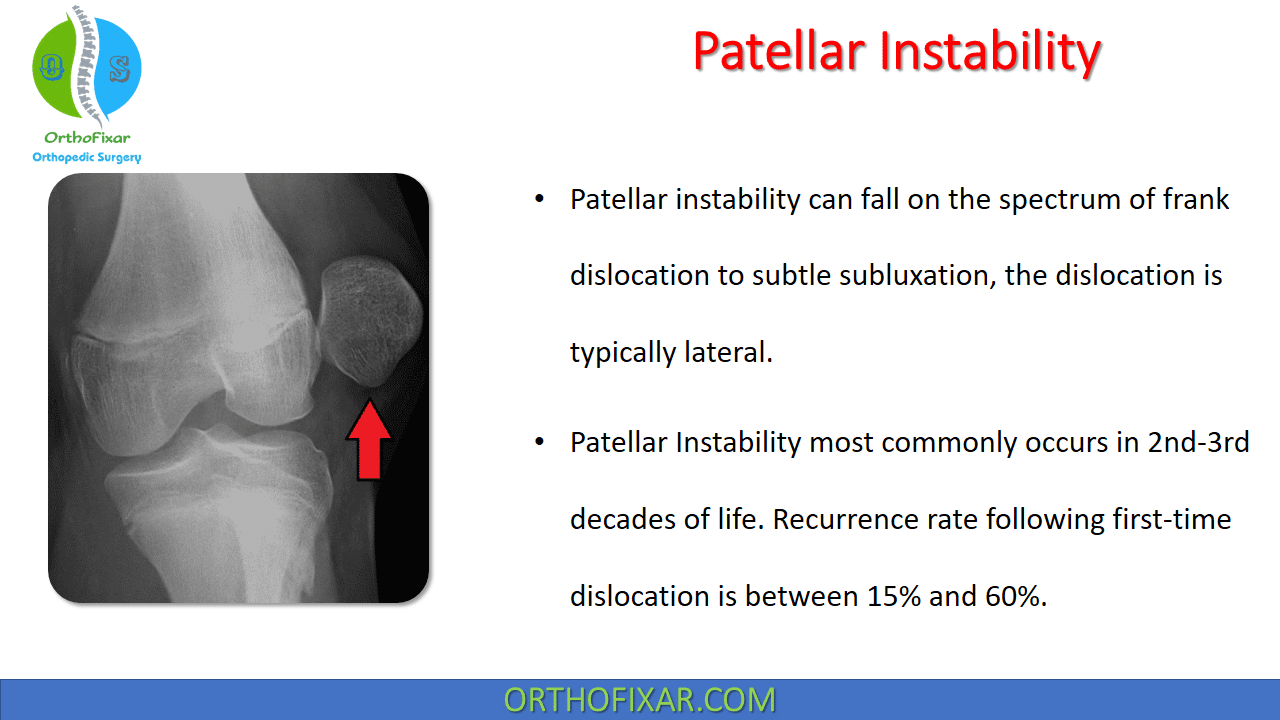
Patellar instability can fall on the spectrum of frank dislocation to subtle subluxation, the dislocation is typically lateral.
Patellar Instability most commonly occurs in 2nd-3rd decades of life. Recurrence rate following first-time dislocation is between 15% and 60%.
Risk factors for Patellar Instability include:
- Incompetence of the medial patellofemoral ligament (MPFL): The main factor that results in recurrent patellar dislocation.
- Ligamentous laxity (Ehlers-Danlos syndrome).
- Increased Q angle.
- Patella alta: causes patella to not articulate with sulcus, losing its constraint effects.
- Trochlear dysplasia.
- Excessive lateral patellar tilt.
- Lateral femoral condyle hypoplasia.
- Dysplastic vastus medialis oblique (VMO) muscle.
- Overpull (contracture) of lateral structures: iliotibial band and vastus lateralis muscle.
Mechanism of injury is usually noncontact twisting injury with the knee extended and foot externally rotated or a direct blow to medial aspect of the knee.
See Also: Anterior Shoulder Instability
Patella Anatomy & Biomechanics
Patella is the largest sesamoid bone, proximally it’s attached the the quadriceps tendons, while distally it’s attached to the patellar tendon.
Patella functions include the following:
- Fulcrum for quadriceps to facilitate knee extension.
- Protects knee joint.
- Enhances lubrication and nutrition of knee.
Patella Ligaments:
- Medial patellofemoral ligament (MPFL): it is attached proximally between adductor tubercle and medial femoral epicondyle (Schottle point), and distally to superomedial patella. It resists lateral translation of patella.
- Retinacular Ligament: it is attached proximally to Vastus medialis and vastus lateralis and tibial condyles, and distally to medial and lateral patella.
Q Angle:
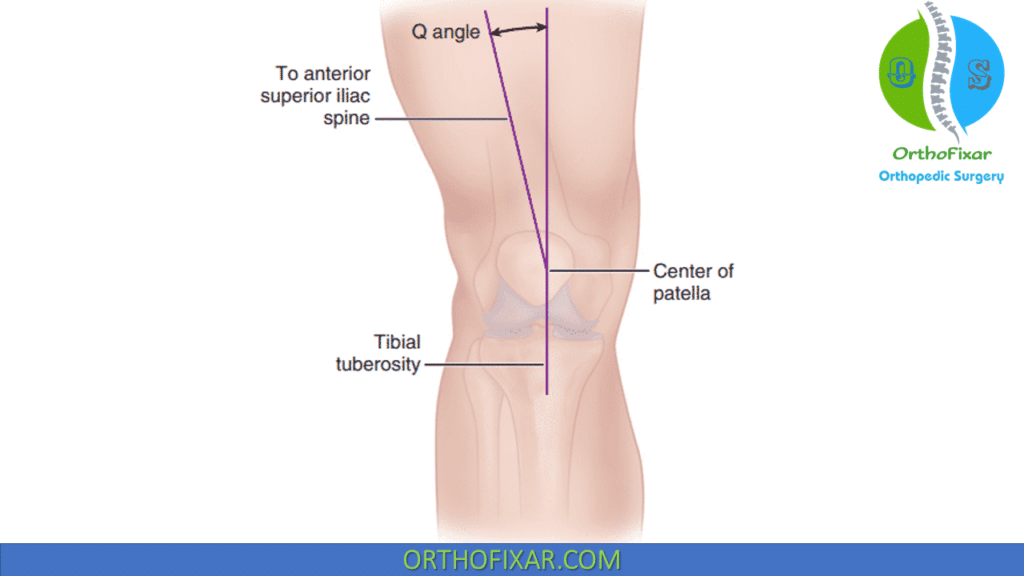
Brattström described the Q angle as an angle formed by the line of pull of the quadriceps mechanism and that of the patellar tendon as they intersect at the center of the patella.
- Clinically, this angle is represented by the intersection of a line drawn from the anterior superior iliac spine to the center of the patella with a second line drawn from the center of the tibial tuberosity to the center of the patella. For this measurement to be accurate, the patella must be centered on the trochlea by flexing the knee 30 degrees. This valgus angle gives a lateral force vector to the patellofemoral joint as the knee is extended.
Normal Q angle:
- In males it should be 8 to 10 degrees.
- In females, the normal angle is 15 degrees ± 5 degrees.
The factors that can increase this Q angle are:
- Genu valgum.
- Increased femoral anteversion.
- External tibial torsion.
- A laterally positioned tibial tuberosity.
- A tight lateral retinaculum.
Any of these factors that increase the Q angle can be a contributing factor in Patellar Instability.
Miserable Malalignment Syndrome: 3 anatomic characteristics that lead to an increased Q angle:
- Femoral anteversion.
- Genu valgum.
- Pronated feet.
See Also: Knee Q Angle Definition
Biomechanics:
The vastus lateralis pulls laterally to the frontal plane of the femur.
The vastus medialis is divided into two parts, the vastus medialis longus and the vastus medialis obliquus.
Patella bone has static and dynamic stabilizers:
Static Stabilizers:
Static stabilizers of the patella include:
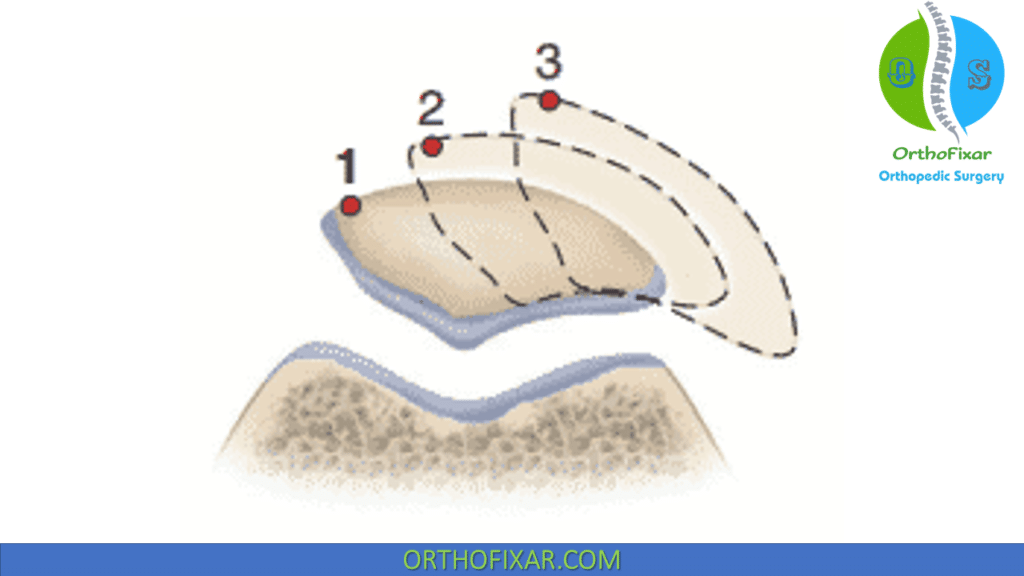
- Shape of the patella
- The femoral sulcus
- A patellar tendon of appropriate length
- Medial patellofemoral ligament (MPFL)
Dynamic Stabilizers:
Dynamic stabilizers of the patella include:
- The vastus medialis obliquus muscle.
Static and dynamic forces tend to displace the patella laterally.
Clinical Evaluation
Patients who have Patellar Instability frequently report diffuse pain around the knee (usually is located anterior in the knee) that is aggravated by going up and down stairs or hills.
Patellar crepitation and swelling of the knee are common.
A feeling of insecurity in the knee and occasionally of “giving way” or “going out” of the knee may be present.
Physical Examination includes:
- Large hemarthrosis in acute dislocation.
- A positive patellar apprehension test.
- A positive J sign.
- Passive patellar translation
Passive patellar translation is measured in quadrants of translation (midline of patella is considered “0”). It should be compared to contralateral side. Normal motion is <2 quadrants of patellar translation. Lateral translation of medial border of patella to lateral edge of trochlear groove is considered “2” quadrants and is considered abnormal amount of translation.
See Also: Knee Examination
Patellar Instability Radiology
Radiographs:
Radiographs are necessary to identify fracture, loose bodies, arthritis, malalignment and abnormal anatomy.
The anteroposterior AP radiograph rarely provides any information regarding patellofemoral problems. It may reveal a bipartite patella, which is a variant of normal, and evaluate lower extremity alignment and version.
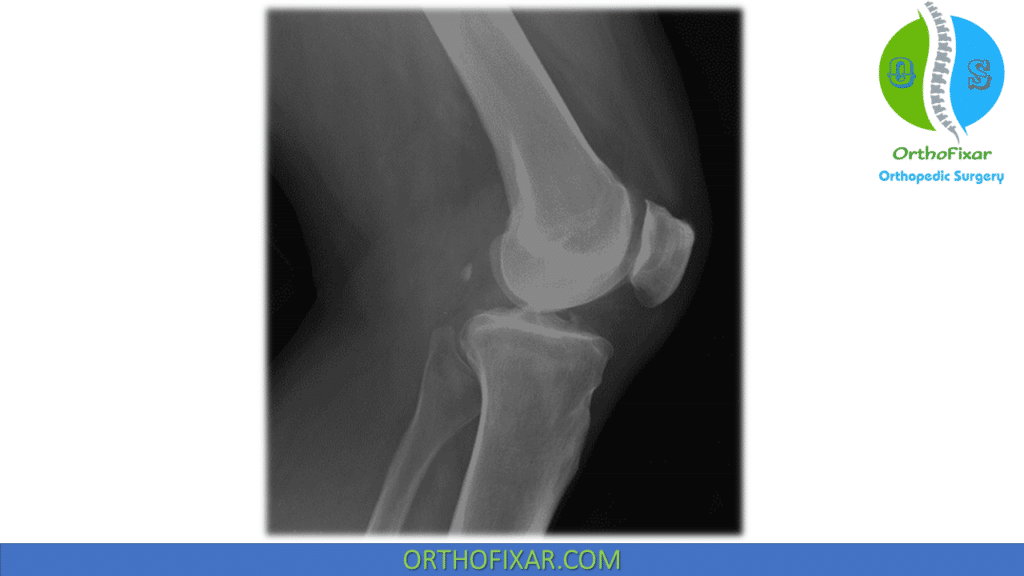
The lateral view of the knee is more helpful in determining patella alta and Trochlea dysplasia.
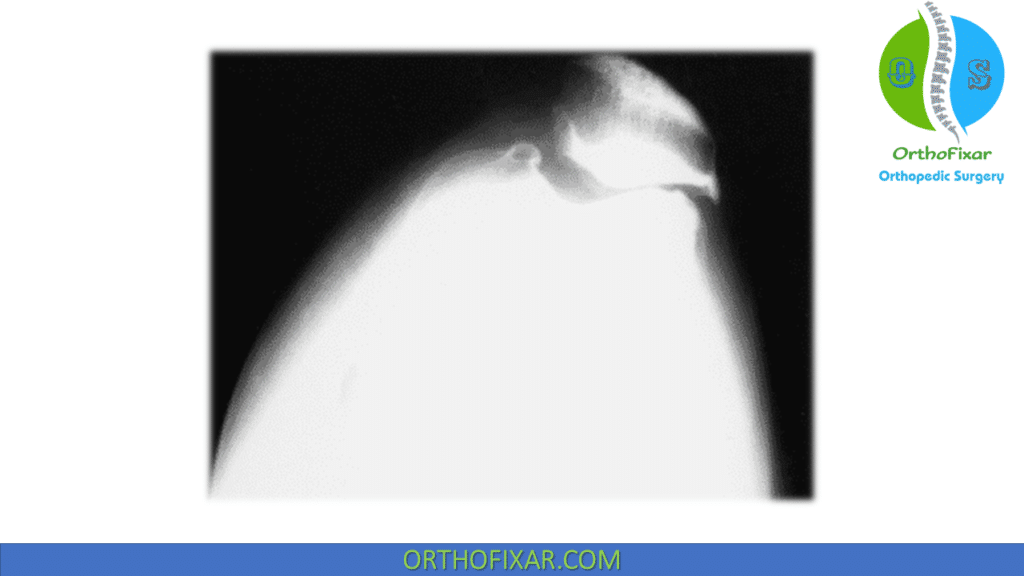
Sunrise / Merchant views: assess for lateral patellar tilt, the shape of the patella, the shape of the femoral trochlea and the relationship of the patella to the femur.
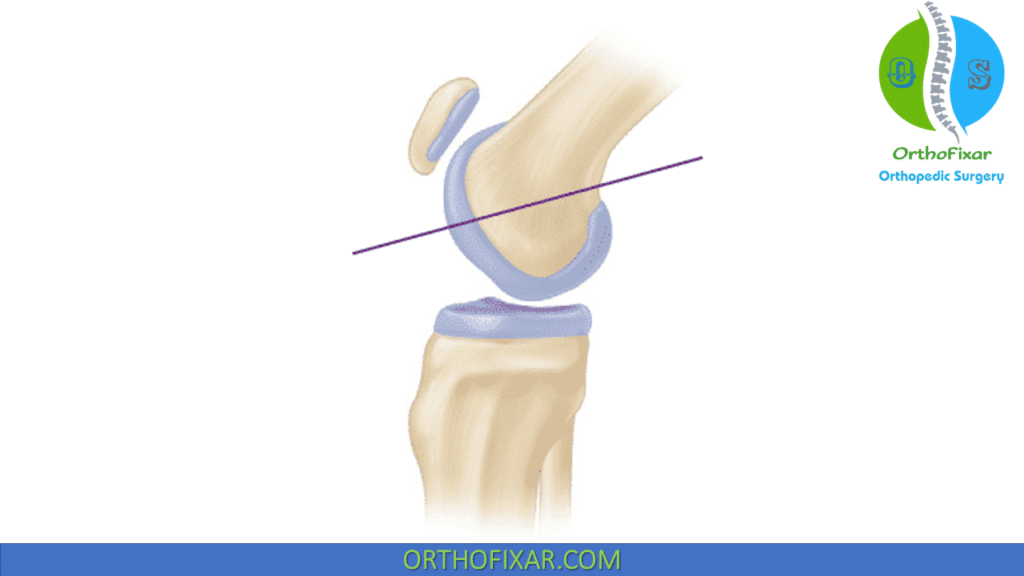
CT scan:
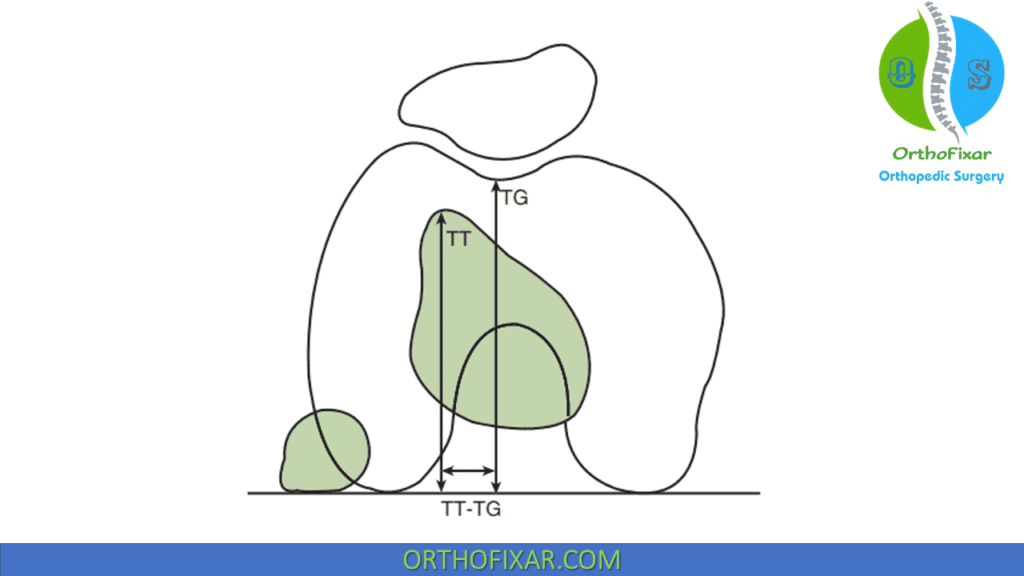
Most frequently used to obtain patellar tilt and measure the tibial tubercle-trochlear groove distance (TT-TG):
- A measurement of the lateralization of the tibial tubercle.
- Normal values between 9 and 13 mm.
- TT-TG 15 to 20 mm questionably abnormal.
- TT-TG over 20 mm highly associated with patellar instability.
MRI:
MRI is indicated for acute dislocations in high-level athletes and when an osteochondral loose body or tear of MPFL is suspected.
Radiographic Measurements of the Patella
| TECHNIQUE | MEASUREMENT | CHARACTERISTICS |
|---|---|---|
| Blumensaat line lateral radiograph to determine patella alta | With knee flexed 30 degrees, line is drawn through intercondylar notch | Should approximate the lower pole of the patella |
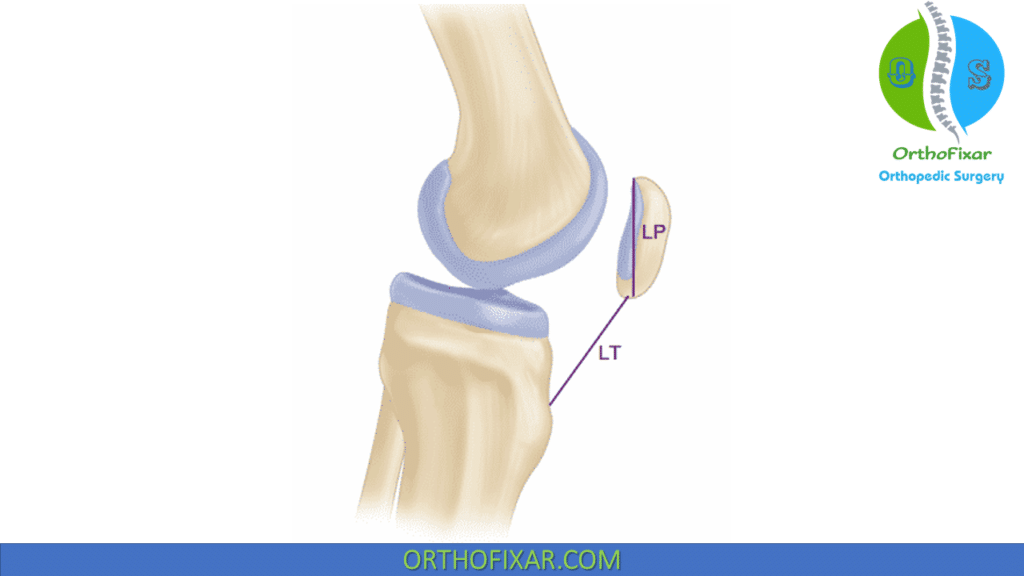
| Insall-Salvati index lateral radiograph | LT:LP = 1.0 | Patella alta if ratio ≥ 1.2 |
| Trochlear depth (Dejour) lateral radiograph | Trochlear depth measured 1 cm from top of groove | Should be ≥ 5 mm |
| Patellar height (Caton Deschamps) lateral radiograph | Ratio between articular facet length of patella (AP) and distance between articular facet of patella and anterior corner of superior tibial epiphysis (AT). Knee flexed 30 degrees. | AP/AT ratio—normal 0.6-1.3 Patella infera—ratio < 0.6 Patella alta—ratio >1.3 |
| Blackburne-Peel ratio | Length of articular surface of patella to length measured from articular surface of tibia to inferior pole of patella | Normal ratio 0.54-1.06 |
| Patellar tilt (CT scan) | Angle formed by intersection of the tangent of the posterior condyles and the major axis of the patella on 20-degree flexion scan | Normal angle: < 20 degrees Angle > 20 degrees: dysplasia |
| TT-TG (axial radiograph, CT scan) | Two lines drawn perpendicular to posterior bicondylar line, one line through middle of trochlear groove (TG) and second through tibial tuberosity (TT). Distance between the lines is measured | 20 mm = malalignment |
| Crossing sign | Anterior cortical outline of condyle intersects trochlear outline | Dysplastic sulcus |
| Trochlear bump | Trochlear line extends anterior to femoral cortex | Dysplastic sulcus |
Patellar Instability Treatment
Nonoperative treatment:
Nonoperative treatment in patellar instability is indicated in:
- Acute first-time patella dislocation (if there is no loose body).
- Habitual dislocation.
- Patellofemoral malalignment or recurrent subluxation of the patella.
Acute first-time patella dislocation treatment include:
- Knee immobilization for 3 to 5 days.
- Hemarthrosis aspiration.
- Ice is applied for 20 minutes every 2 to 3 hours to reduce swelling.
- Rehabilitation after immobilization removal with closed-chain exercises for quadriceps and hamstring muscles.
- Generally, a patellar stabilizing brace is prescribed for the first 6 to 8 weeks during rehabilitation and long-term for sports activity
Some surgeons preferred early surgical treatment with arthroscopic evaluation or débridement and acute repair of the medial patellofemoral ligament (controversial).
Operative Treatment:
Surgical Patellar Instability treatment indications include:
- Acute patellar dislocation with osteochondral fracture and a loose body formation.
- Recurrent Patellar Instability.
- TT-TG >20mm on CT.
- Patella alta.
- Excessive lateral tilt or tightness after medialization
Surgical Procedures for Treatment of Patellar Instability
| Procedures | Indications and Characteristics |
|---|---|
| Medial repair/imbrication | 30% failure rate, approximately the same as conservative treatment. Indication: first dislocation + repairable chondral defect. Instability in skeletally mature. In combination with distal realignment. |
| Lateral release | Excessive lateral pressure syndrome. In combination with realignment procedure when excessive tightness prevents patellar centering. May increase risk for both medial and lateral patellar subluxation. |
| MPFL reconstruction | Indicated for recurrent MPFL deficiency ± trochlear dysplasia. Proximal or anterior femoral placement or overtightening results in medial facet overload. May combine with distal realignment. |
| Elmslie-Trillat procedure | Indicated for instability TT-TG > 20 mm + strong repairable medial structures. Healing time and risk for stress or contact fracture of proximal tibia much less than Fulkerson procedure. |
| Fulkerson distal realignment | Indicated for symptomatic lateral facet or distal pole arthritis + TT-TG > 20 mm. Contraindicated with proximal/medial facet arthritis. Long healing time, increased risk of proximal tibial fracture with sports. |
| Rotational high tibial osteotomy | Indicated for Patellar Instability + severe rotational deformity. More normalized gait compared with distal realignment. |
| Trochleoplasty | Indicated for dysplastic trochlea. Low recurrence rate. Increased risk for osteonecrosis, DJD, arthrofibrosis. Lateral condyle: increased pressure; increased DJD of lateral facet. |
| Grooveplasty | Increased DJD. Good results with less risk reported with MPFL reconstruction. |
| 3-in-1 procedure: extensor mechanism realignment + VMO advancement + transfer of the medial third of the patellar tendon to the MCL. | Patellar Instability, TT-TG > 20 mm. Open physes. |
References & More
- Campbel’s Operative Orthopaedics 12th edition Book.
- Millers Review of Orthopaedics -7th Edition Book.
- Hayat Z, El Bitar Y, Case JL. Patella Dislocation. [Updated 2022 Jul 4]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK538288/
- Wolfe S, Varacallo M, Thomas JD, et al. Patellar Instability. [Updated 2022 Sep 18]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK482427/