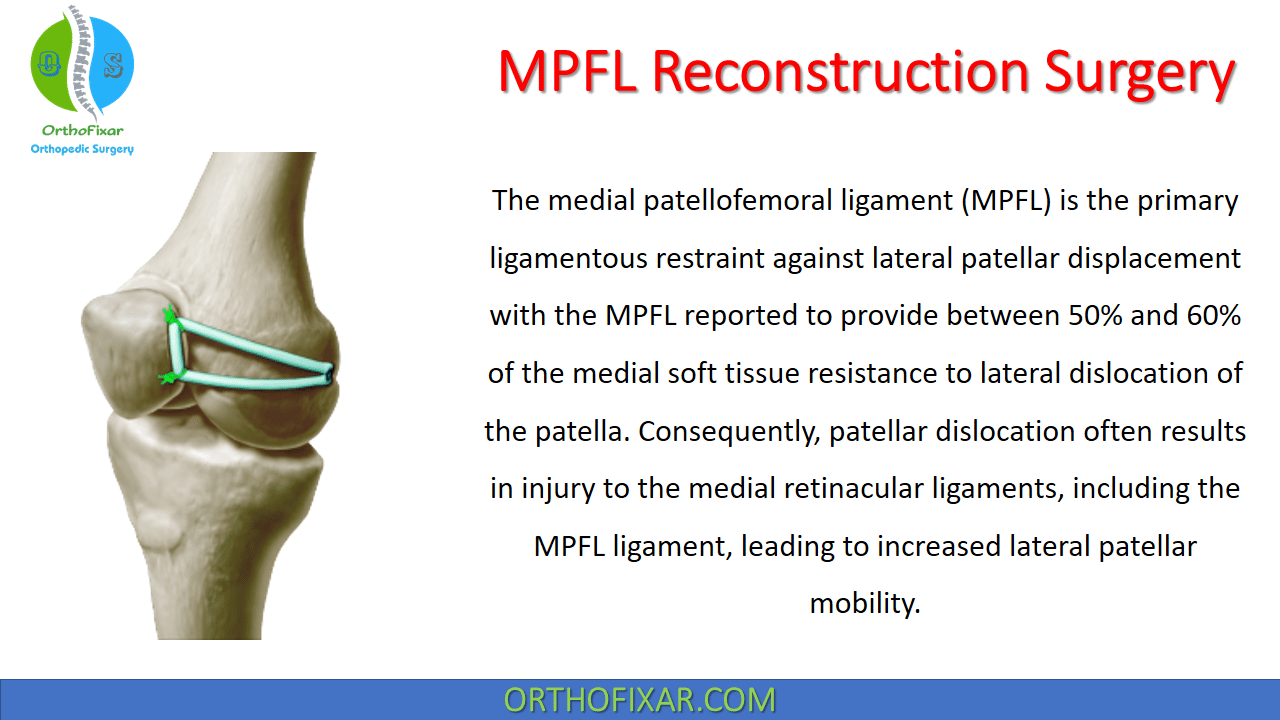
MPFL Reconstruction is a procedure used in patellar instability to restore lateral patellar mobility to a normal range.
The medial patellofemoral ligament (MPFL) is the primary ligamentous restraint against lateral patellar displacement with the MPFL reported to provide between 50% and 60% of the medial soft tissue resistance to lateral dislocation of the patella. Consequently, patellar dislocation often results in injury to the medial retinacular ligaments, including the MPFL ligament, leading to increased lateral patellar mobility. Competency of the MPFL is necessary and sufficient to restore lateral patellar mobility to a normal range; consequently, surgical treatment should aim for restoration of a functional MPFL.
MPFL Reconstruction Indications
Nonoperative treatment is typically indicated for acute, first-time dislocators without associated osteochondral fracture or loose bodies. Surgical management is indicated for the following:
- Recurrent patellar instability (at least 2 documented instability events) and a confirmatory physical examination demonstrating excessive lateral patellar laxity: For these recurrent dislocators, MPFL reconstruction is the current procedure of choice.
- Osteochondral fracture or a loose body that is potentially repairable or causing mechanical symptoms: Consideration must be given to the size and location of the donor fragment and the presence of adequate subchondral bone when considering fragment repair. In the presence of osteochondral injury being addressed surgically, one can perform concomitant MPFL reconstruction.
- Smaller, isolated chondral injuries: Surgery may be indicated if mechanical symptoms are present. Nonoperative treatment is appropriate in the absence of mechanical symptoms.
See Also: Patellar Instability
MPFL Reconstruction Procedure
Important Imaging Considerations for Preoperative Planning
Patellar height
- Preferred method of measurement is that of Caton and Deschamps (ie, the ratio between the distance from the lower edge of the patellar articular surface to the upper edge of the tibial plateau and the length of the patellar articular surface).
- A ratio of 1.2 or greater indicates patella alta, which predisposes the patient to patellar instability due to late engagement of the patella in the trochlea as the knee flexes.
- If patella alta is present, tibial tubercle osteotomy and distalization should be considered as an additional procedure.
Tibial tubercle–trochlear groove (TT-TG) distance
- The TT-TG offset is the transverse distance between the anterior tibial tuberosity and the center of the trochlear groove.
- Distance can be measured on axial CT or MRI, although some argue that these imaging modalities are not interchangeable as MRI has been reported to underestimate the TT-TG offset when compared with CT.
- When lateral offset measures 20 mm or more, medialization of the tibial tubercle can be considered as an additional procedure to address patellofemoral instability.
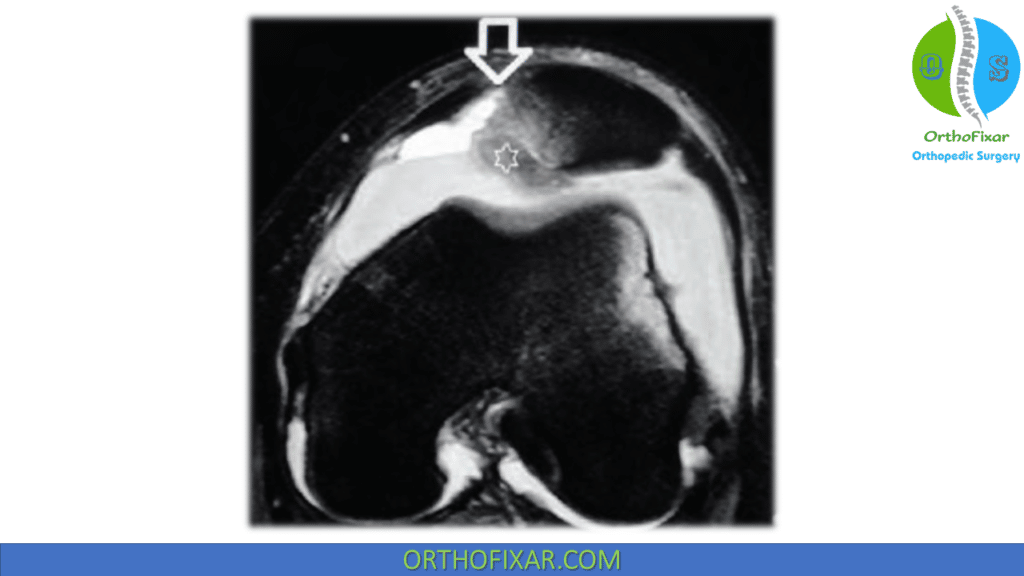
Trochlear morphology
- Important consideration as severe cases of trochlear dysplasia can challenge the long-term success of MPFL repair.
- Can be assessed on a true lateral x-ray (the posterior borders of both femoral condyles are strictly superimposed)
- A crossing sign occurs when the floor of the trochlea crosses the anterior border of both femoral condyles, thus indicating trochlear dysplasia.
- A positive trochlear prominence (ie, the sagittal distance between the trochlear groove and the anterior femoral cortex) greater than 3 mm on the lateral view has been shown to correlate well with trochlear dysplasia.
- Axial MRI has been shown to more accurately classify trochlear groove anatomy (in comparison to axial x-rays or CT) when assessing trochlear dysplasia.
Equipment
The following equipment is recommended in addition to standard soft tissue retractors for the authors’ preferred method of MPFL reconstruction:
- Knee arthroscopy equipment if knee arthroscopy is to be performed prior to MPFL reconstruction
- Soft tissue tendon stripper for the harvest of semitendinosus graft (the authors prefer a closed tendon stripper)
- 4.5-mm drill with guide for drilling tunnels in the patella for each end of the semitendinosus tendon graft
- Small curved curette to clear the patellar tunnels of debris for graft passage
- 18-gauge steel wire to be fashioned to retrieve suture through the patellar tunnels. Alternative options include commercially produced curved suture passer devices.
- Smooth 2.4-mm guide wire pin (Beath pin equivalent) diameter, and if applicable, with eyelet for suture. This pin is used to drill into the center of the femoral MPFL footprint and guide the reamer for MPFL femoral tunnel creation. If the pin is too long, it can interfere with obtaining fluoroscopy to confirm anatomic positioning of the pin in the MPFL origin.
- Fluoroscopy for checking the position of the guide pin in the femoral footprint of the MPFL. The authors prefer to use a Mini-C arm equivalent.
- Cannulated reamers of various diameters from 5 to 8 mm for drilling the femoral tunnel
- Interference screws for fixation of grafts in the femoral tunnel. Typically, screws run from lengths of 20 to 25 mm and diameters of 5 to 8 mm.
- #0 or #1 absorbable suture
- #5 braided polyethylene suture
- #2 nonabsorbable sutures.
Positioning and Portals
The patient is positioned supine. A small bump may be placed under the hip to prevent external rotation. A sterile bump may also be placed under the knee to maintain slight flexion. If performing knee arthroscopy prior to MPFL reconstruction, it is recommended to do so with the bed kept flat, allowing the knee to be flexed over the side of the bed in lieu of dropping the foot of the bed for knee flexion.
Arthroscopy can be performed to stage or address articular cartilage lesions and rule out preexisting severe arthritis if there is any question about the cartilage health of the patellofemoral joint. Fluoroscopy can be brought in from the ipsilateral side of the bed when needed to obtain a lateral view of the distal femur to confirm anatomic placement of the guide pin in the MPFL femoral footprint.
Description of the Procedure
Examination Under Anesthesia
Perform an examination under anesthesia to confirm excessive lateral patellar mobility. Increased laxity is signified by more than 10 mm of lateral translation and the absence of an endpoint with the knee at 30 degrees of flexion.
Semitendinosus Tendon Graft Harvest and Preparation
- The sartorial fascia is exposed through a 2- to 3-cm skin incision made 2 cm medial and distal to the medial border of the tibial tubercle.
- The sartorial fascia is incised in line with the palpable gracilis tendon.: Avoid making this incision too deep to avoid injury to the underlying superficial medial collateral ligament.
- Identify and isolate the gracilis (proximal) and semitendinosus (distal) tendons from their deep aspect (ie, from within the bursal layer).
- Apply tension to the semitendinosus while freeing it from the crural fascia at the posteromedial corner with tissue scissors.
- Place stay sutures of #0 or #1 absorbable suture on a tapered needle, and then divide the tendon from the tibial insertion.
- Once all tendinous slips have been freed, harvest the semitendinosus tendon using a closed (preferred) or open tendon stripper.
- Baseball stitches are placed on both free ends with #2 nonabsorbable suture for later graft passage through the 2 patellar tunnels.
- The graft is prepared on the back table by first sizing the graft to 240 mm and then folding it in half, leaving a doubled graft of 120 mm. It is recommended to make the doubled graft length no less than 120 mm to ensure adequate graft length.
- A #5 polyethylene suture is placed through the loop to be used for pulling the doubled graft into the blind femoral tunnel.
- A baseball stitch 25 mm in length with #0 or #1 absorbable suture is placed in the looped end of the graft to sew together the 2 graft strands that will be in the femoral tunnel.
Patellar Tunnel Placement
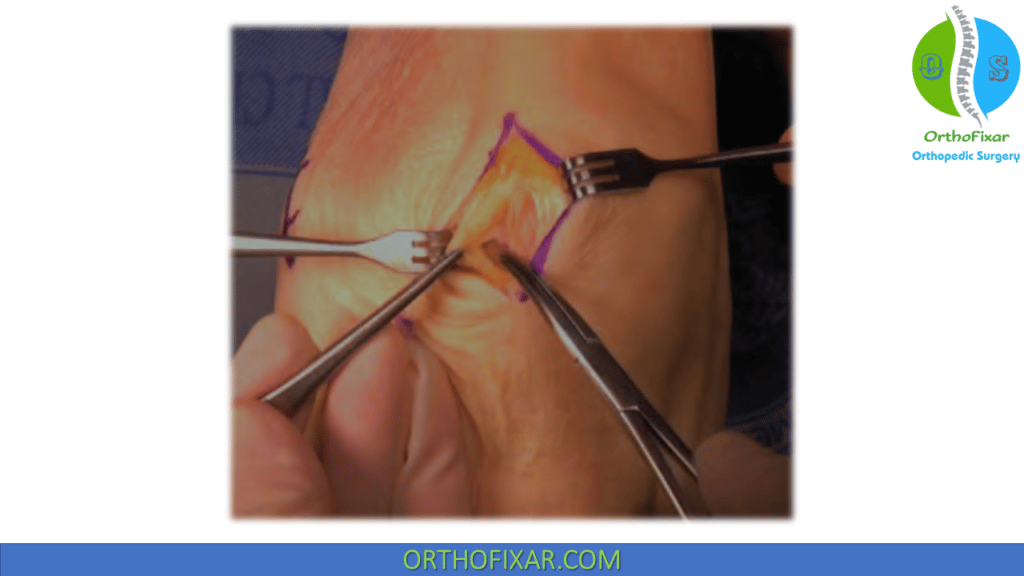
- A longitudinal incision the length of the patella is made at the junction of the medial and middle thirds of the patella (in line with the medial border of the patellar tendon at the distal patellar pole).
- The medial 8 to 10 mm of the patella is exposed by subperiosteal dissection with a #15 scalpel.
- The dissection extends medially and dorsally around the patella through layers 1 (longitudinal retinaculum) and 2 (native MPFL), stopping after the transverse fibers of the native MPFL have been cut. The capsule (layer 3) is left intact.
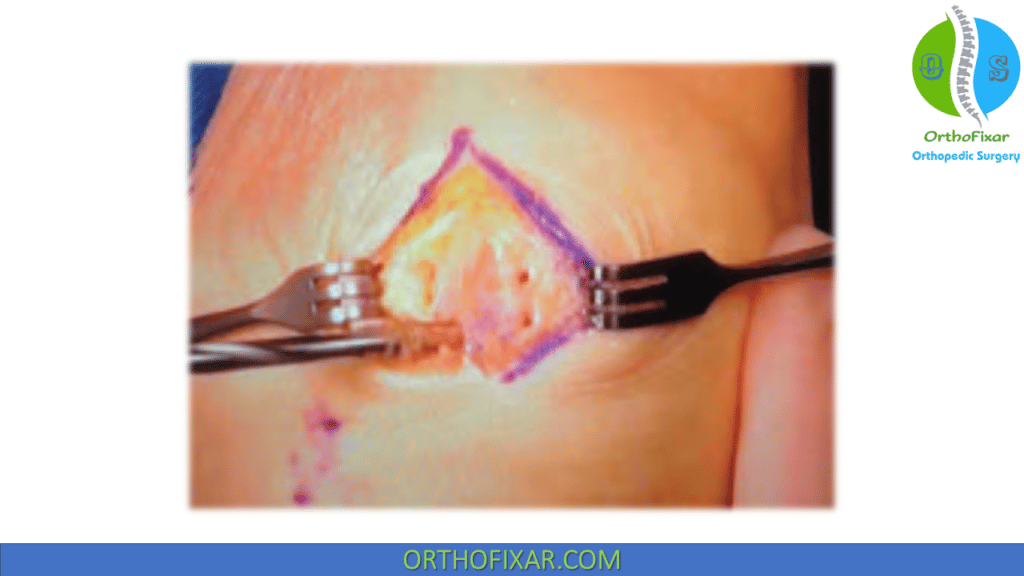
- A 4.5-mm drill hole is placed on the medial side of the upper pole of the patella adjacent to the articular margin.
- A corresponding drill hole is placed on the anterior surface of the patella approximately 8 mm from the medial border. (This point corresponds to the lateral edge of the original retinacular dissection.)
- The 2 drill holes are connected with a curved curette.
- A second 4.5-mm drill hole is placed on the medial side of the patella at a point two-thirdsdown the length of the patella.
- A corresponding drill hole is placed on the anterior surface of the patella about 8 mm from the medial border, and the 2 holes are connected with a curved curette.
- If the semitendinosus graft is more than 4.5 mm in diameter, the drill holes are enlarged slightly to facilitate graft passage.
- It is important to avoid placing the distal patellar tunnel distal to the native insertion of the MPFL to avoid constraining the distal pole of the patella.
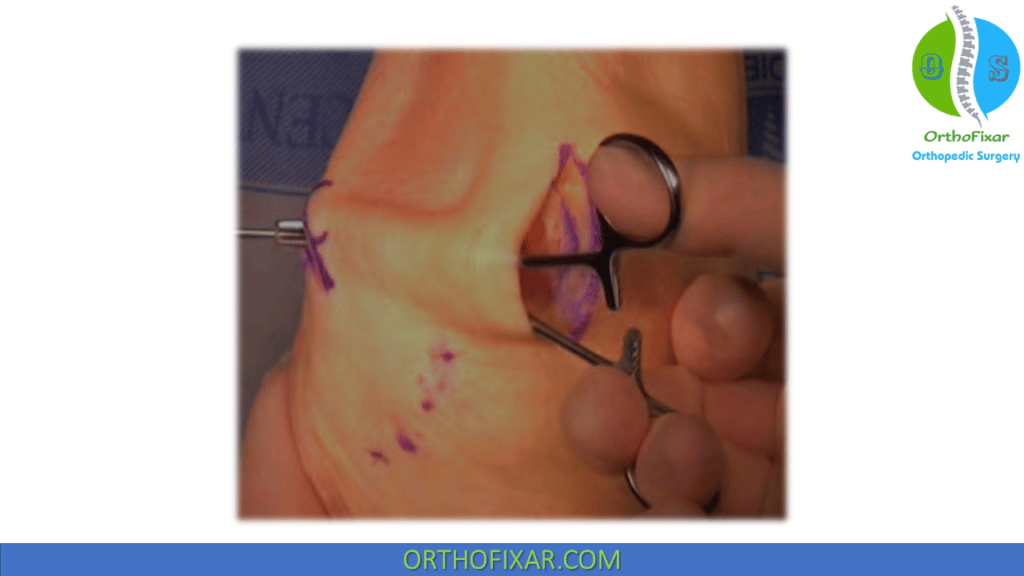
Femoral Tunnel Placement and Checking Isometry
- A skin incision is made just anterior to the palpable ridge connecting the medial femoral epicondyle and the adductor tubercle.
- The knee is flexed slightly to facilitate palpation of this landmark (flexion moves the hamstrings posteriorly away from the medial epicondyle).
- If the landmarks are difficult to palpate, a small skin incision is made, and palpation is done through the wound to identify the ridge.
- The graft may be placed between layers 1 and 2 or between layers 2 and 3 (joint capsule) (ie, it may lie superficial or deep to the native MPFL).
- Placing the graft between layers 2 and 3 is preferred because blind dissection superficial to the native MPFL may disrupt the insertion of the vastus medialis oblique into the anterior portion of the MPFL; in addition, by placing the graft deep to the native MPFL, the latter may be repaired to the graft during wound closure.
- The graft should not be placed deep to the capsule because it should remain extra-articular to avoid graft abrasion and facilitate complete healing.
- Using a long, curved clamp, the selected interval is developed (preferably between layers 2 and 3) from the patellar incision anteriorly to the medial femoral epicondyle posteriorly.
- With the tip of the clamp overlying the ridge between the medial epicondyle and adductor tubercle, layers 1 and 2 are incised using a #15 blade.
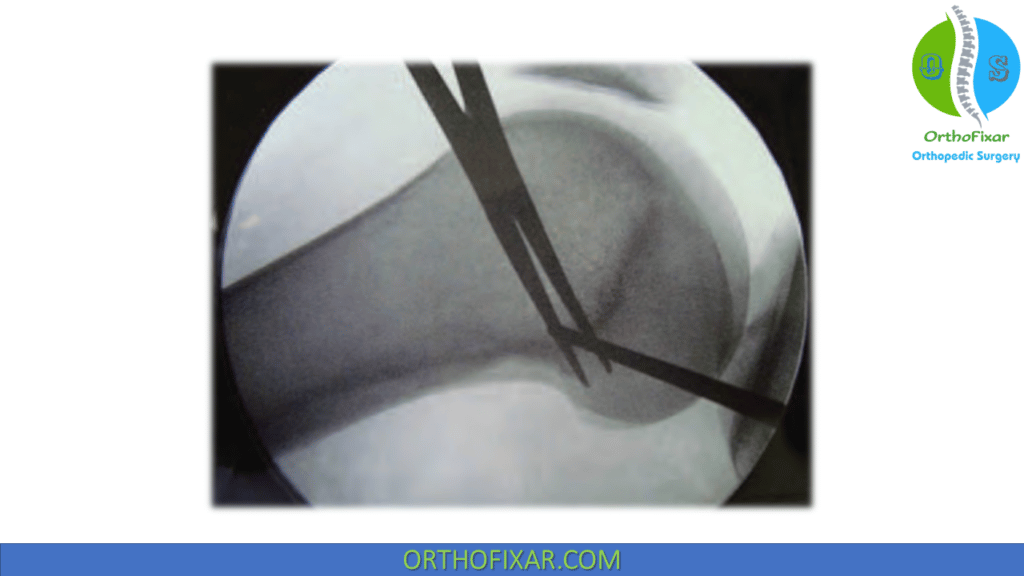
- The tip of a Beath pin is placed at a point approximately 9 mm proximal and 5 mm posterior to the medial epicondyle; the pin is then passed toward the lateral side of the femur. Accuracy of pin placement should be confirmed by lateral fluoroscopic imaging, with ideal tunnel location approximately 1 mm anterior to the posterior cortex extension line, 2.5 mm distal to the posterior origin of the medial femoral condyle, and proximal to the level of the posterior point of the Blumensaat line on a lateral x-ray with both posterior condyles projected in the same plane.
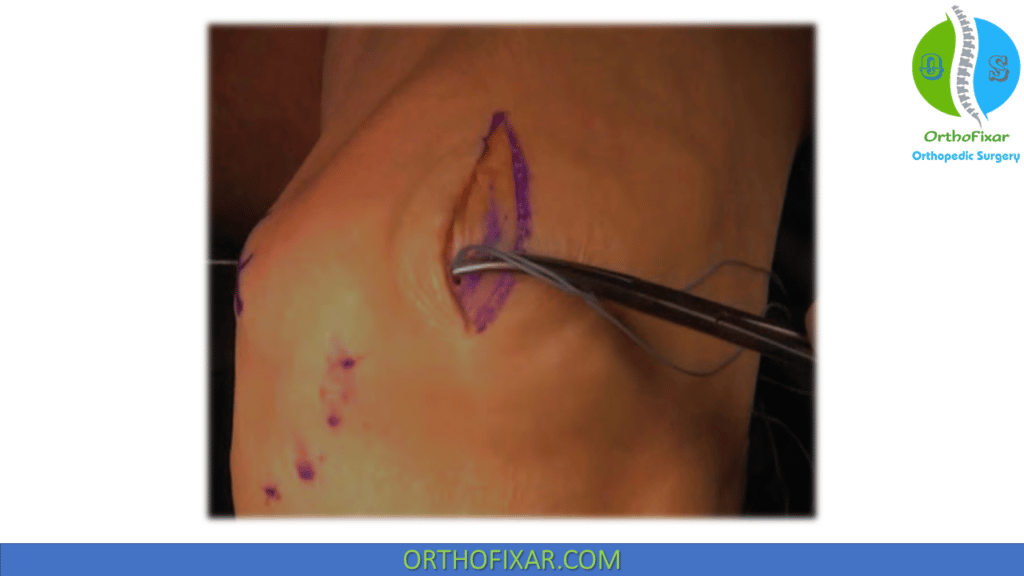
- A loop of #5 braided polyethylene suture is passed around the Beath pin, through the dissected retinacular tunnel, and then through one of the patellar tunnels.
- The knee is taken through ROM to evaluate isometry while holding the suture at the anterior aspect of the patellar tunnel to evaluate for length changes of the suture during ROM.
- If lengthening occurs in flexion, a second Beath pin is placed more distally toward the medial epicondyle. The first pin is left in place to facilitate repositioning while drilling the second Beath pin. The loop of #5 suture is passed around the second Beath pin, and the knee is put through ROM again. If isometry is acceptable, the first Beath pin is removed.
- If lengthening occurs in extension, a second Beath pin is placed more proximally toward the adductor tubercle. The first pin is left in place to facilitate repositioning while drilling the second Beath pin. The loop of #5 suture is passed around the second Beath pin, and the knee is put through ROM again. If isometry is acceptable, the first Beath pin is removed.
- Once the femoral pin site is accepted, a blind tunnel is reamed into the femur the size of the doubled graft. For a semitendinosus graft, this usually is 6 to 7 mm in diameter.
- The femur is reamed to a depth of at least 20 mm, with a preferred depth of 25 mm.
Graft Passage and Fixation
- The #5 suture placed through the loop of the graft is passed through the Beath pin, and the pin is then advanced out the lateral femoral cortex to pass the graft into the femoral tunnel.
- Fixation to the femur may be achieved reliably with a 20- to 25-mm interference screw.
- The looped isometry suture, if left in place in the retinacular tunnel, may be used to pass the free ends of the graft through the retinacular interval created previously.
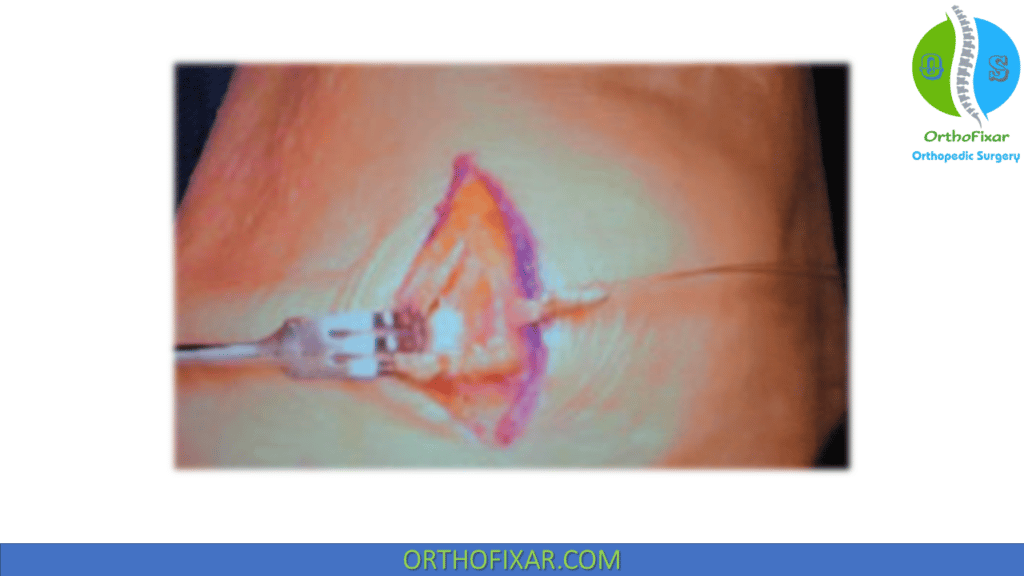
- The free graft arms are passed individually through their respective patellar tunnels using double 18-gauge stainless steel wire or a curved suture passer.
- The graft arms enter the medial border of the patella and exit anteriorly to be doubled over themselves for suture fixation.
- The free graft arms are doubled back and sutured on themselves just medial to the patella using 2 figure-8 mattress sutures of #2 nonabsorbable suture on a tapered needle.
- Patellar mobility is checked after the first suture is placed. There should be a good endpoint, or checkrein, with the knee in full extension and at 30 degrees of flexion, full knee ROM, and 7 to 9 mm of lateral patellar displacement from the centered position at 30 degrees of flexion.
- Excess graft is sharply removed.
- The native MPFL is sutured to the graft, and then the retinaculum is closed over the graft.
- The wounds are closed in standard fashion.
Postoperative Protocol
For MPFL Surgery Recovery, these protocols should be followed after MPFL Reconstruction:
- Weightbearing as tolerated is allowed immediately postoperatively in a drop-lock or knee extension brace.
- Passive ROM and resisted closed chain exercises are started as soon as possible to restore ROM and quadriceps control. Preserving motion is key after MPFL surgery.
- Bracing may be continued for up to 6 weeks during ambulation to prevent falls until quadriceps control is restored. Circumferential measurement of quadriceps 10 cm above the superior pole of the patella can aid in evaluating restoration of the quadriceps.
- Patients are allowed to return to stressful activities, including sports, when they attain full ROM and have regained at least 80% of their quadriceps strength compared to the noninjured limb.
- If at least 90 degrees of flexion is not achieved by 6 postoperative weeks, then the intensity of the therapy program must be increased. Manipulation under anesthesia may be needed between 9 and 12 weeks postoperatively if stiffness does not resolve with therapy alone.
References
- Conlan T, Garth WP Jr, Lemons JE. Evaluation of the medial soft-tissue restraints of the extensor mechanism of the knee. J Bone Joint Surg Am. 1993 May;75(5):682-93. doi: 10.2106/00004623-199305000-00007. PMID: 8501083.
- Panagiotopoulos E, Strzelczyk P, Herrmann M, Scuderi G. Cadaveric study on static medial patellar stabilizers: the dynamizing role of the vastus medialis obliquus on medial patellofemoral ligament. Knee Surg Sports Traumatol Arthrosc. 2006;14(1):7-12.
- Hautamaa PV, Fithian DC, Kaufman KR, Daniel DM, Pohlmeyer AM. Medial soft tissue restraints in lateral patellar instability and repair. Clin Orthop Rel Res. 1998;(349):174-182.
- Fithian DC, Gupta N. Patellar instability: principals of soft tissue repair and reconstruction. Tech Knee Surg. 2006;5:19-26.
- Mäenpää H, Lehto MU. Patellar dislocation. The long-term results of nonoperative management in 100 patients. Am J Sports Med. 1997;25(2):213-217.
- Nikku R, Nietosvaara Y, Aalto K, Kallio PE. Operative treatment of primary patellar dislocation does not improve medium-term outcome: a 7-year follow-up report and risk analysis of 127 randomized patients. Acta Orthop. 2005;76(5):699-704.
- Nikku R, Nietosvaara Y, Kallio PE, Aalto K, Michelsson JE. Operative versus closed treatment of primary dislocation of the patella: similar 2-year results in 125 randomized patients. Acta Orthop Scand. 1997;68(5):419-423.
- Fithian DC, Paxton WE, Stone ML, et al. Epidemiology and natural history of acute patellar dislocation. Am J Sports Med. 2004;32(5):1114-1121.
- Teitge RA, Faerber WW, Des Madryl P, Matelic TM. Stress radiographs of the patellofemoral joint. J Bone Joint Surg Am. 1996;78(2):193-203.
- Panagiotopoulos E, Strzelczyk P, Herrmann M, Scuderi G. Cadaveric study on static medial patellar stabilizers: the dynamizing role of the vastus medialis obliquus on medial patellofemoral ligament. Knee Surg Sports Traumatol Arthrosc. 2006;14(1):7-12.
- Elias DA, White LM, Fithian DC. Acute lateral patellar dislocation at MR imaging: injury patterns of medial patellar soft-tissue restraints and osteochondral injuries of the inferomedial patella. Radiology. 2002;225(3):736-743.
- Caton J, Deschamps G, Chambat P, Lerat JL, Dejour H. Patella infera. Apropos of 128 cases [in French]. Rev Chir Orthop Reparatrice Appar Mot. 1982;68(5):317-325.
- Dejour H, Walch G, Nove-Josserand L, Guier C. Factors of patellar instability: an anatomic radiographic study. Knee Surg Sports Traumatol Arthrosc. 1994;2(1):19-26.
- Camp CL, Stuart MJ, Krych AJ, et al. CT and MRI measurements of tibial tubercle-trochlear groove distances are not equivalent in patients with patellar instability. Am J Sports Med. 2013;41(8):1835-1840.
- Salzmann GM, Weber TS, Spang JT, Imhoff AB, Schöttle PB. Comparison of native axial radiographs with axial MR imaging for determination of the trochlear morphology in patients with trochlear dysplasia. Arch Orthop Trauma Surg. 2010;130(3):335-340
- Schöttle PB, Schmeling A, Rosenstiel N, Weiler A. Radiographic landmarks for femoral tunnel placement in medial patellofemoral ligament reconstruction. Am J Sports Med. 2007;35(5):801-804.
- Elias JJ, Cosgarea AJ. Technical errors during medial patellofemoral ligament reconstruction could overload medial patellofemoral cartilage: a computational analysis. Am J Sports Med. 2006;34(9):1478-1485.
- Muneta T, Sekiya I, Tsuchiya M, Shinomiya K. A technique for reconstruction of the medial patellofemoral ligament. Clin Orthop Rel Res. 1999;(359):151-155.
- Nomura E, Horiuchi Y, Kihara M. Medial patellofemoral ligament restraint in lateral patellar translation and reconstruction. Knee. 2000;7(2):121-127.