Knee Meniscus Tear Surgery techniques have evolved over the past several decades in an attempt to improve outcomes. Unfortunately, the vast majority of meniscus tears cannot be treated with meniscus repair, and arthroscopic partial meniscectomy remains the best procedure in patients with symptomatic meniscal tears.
Arthroscopic partial meniscectomy is an outpatient procedure that can be done under a variety of anesthetic techniques (general, spinal, or regional with or without sedation). Prior to surgical intervention, nonoperative management is the mainstay of initial treatment in the majority of cases. Nonoperative management consists of ice, nonsteroidal anti-inflammatory drugs in patients in whom they are not contraindicated, physical therapy, activity modification, with the possible addition of intra-articular injection of steroids.
Arthroscopic Meniscal Resection Indications
- Persistent pain despite conservative treatment
- Presence of mechanical symptoms
- Younger physiologic age
- Increased activity demands
- Failure of previous meniscus repair
Controversial Indications
- Tear amendable to repair
- Asymptomatic tear
- Stable tear (typically < 1.5 cm in length and incomplete, particularly in a patient with an anterior cruciate ligament [ACL]-deficient knee)
- Degenerative tear in patients with evidence of osteoarthritis (30% nonoperative failure rate requiring conversion to surgery)
See Also: Knee Meniscus Tear

Arthroscopic Meniscus Surgery
Equipment
- Arthroscopic pump
- 30-degree arthroscope
- 70-degree arthroscope available
- Arthroscopic probe
- Array of arthroscopic punches (often termed biters)
- Motorized shaver 4.0 mm (3.5 or 3.0 mm for smaller or tighter knees)
- Arthroscopic knives (straight, banana, and back-cutting) may assist with meniscal resection

Positioning and Portals
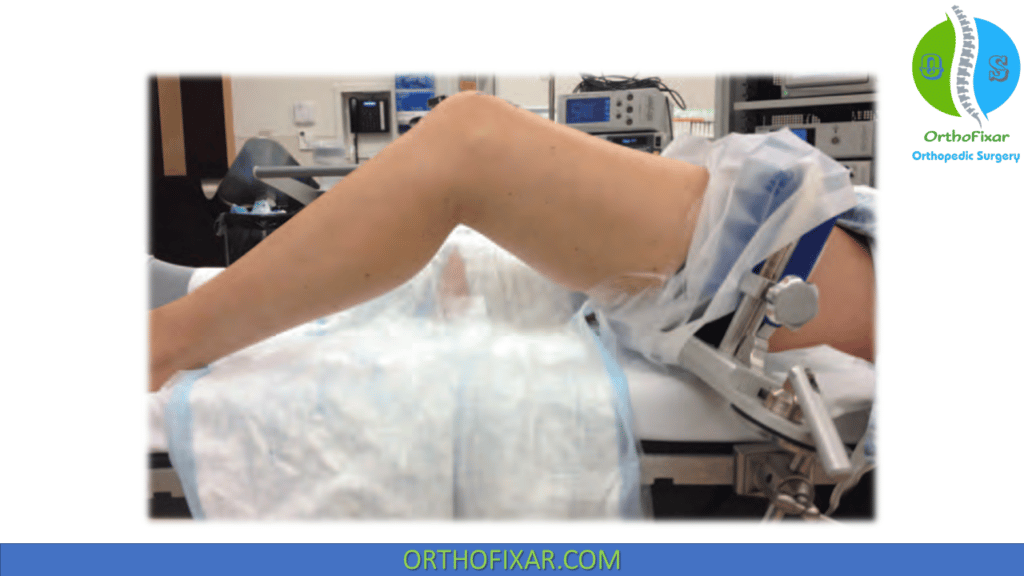
The patient is positioned supine on the operating room table. A leg holder or a post is used to exert valgus and varus pressure during the procedure.
There are multiple options for anesthesia for meniscectomy, but spinal or general anesthetics are generally preferred.
The foot of the table can be left extended or dropped. If the foot is not dropped and a leg holder is used, it is important to have the leg holder positioned so the hip is flexed 30 degrees in order to keep the knee free and allow ready access for the arthroscopic instruments.
Routine knee arthroscopy can be performed without the use of a tourniquet. This is facilitated by distending the joint prior to portal placement with a local anesthetic with epinephrine. Infiltration of the sites for portal placement with local anesthetic with epinephrine also facilitates knee arthroscopy without the use of a tourniquet.
There are multiple possible portals for arthroscopic meniscectomy. The vertical portal just lateral to the proximal patellar tendon for the arthroscope and a relatively low oblique portal anteromedially for instrumentation.
The anterolateral portal should be developed with the knee flexed at least 50 degrees to protect the articular surfaces. Once the capsule and synovium have been penetrated using a blunt obturator, the knee is extended to facilitate positioning of the sheath in the suprapatellar pouch. The use of a spinal needle for localization of the anteromedial portal while visualizing from the anterolateral portal is often beneficial to optimize portal placement.
The surgeon should be prepared to use multiple other portals if necessary; specifically, the posteromedial or posterolateral portals may be helpful to remove a retained meniscal fragment that gets into the posterior compartment. These must be developed with the knee flexed to 90 degrees. Protection of the neurovascular structures when one of these portals is being established and used is paramount.
The posterolateral portal must always be developed well anterior to the biceps tendon to avoid the peroneal nerve. These portals are most safely developed by initially using a spinal needle for localization. Placement of the cannula with a blunt obturator through the capsule should be done while directly visualizing the capsule.
Description of the Procedure
The arthroscope is placed into the knee through the standard anterolateral portal with the use of a blunt obturator. With the use of a pump, a distension pressure of 30 to 40 mm Hg is typically all that is necessary. A complete diagnostic examination should be performed at the beginning of any arthroscopic knee procedure.
The anteromedial portal is next established as previously described, and the arthroscopic probe is introduced to inspect the menisci. The medial meniscus should first be probed superiorly and inferiorly to identify any area of tearing and to define the length and width of any tear. Tear stability and proximity to the peripheral blood supply should be assessed as they are important aspects of the treatment decision.
The cruciates should be inspected after the medial compartment and, again, palpation is necessary not only to define anatomy but also the tension. Finally, the lateral compartment is inspected in the figure-4 position. Rotation of the 30-degree scope allows visualization of the posterior, mid, and anterior horns of the lateral meniscus in sequence. The offset should be aimed posteriorly to visualize the posterior horn and then carefully rotated as the inspection proceeds to lateral and anterior. Again, defining the extent and anatomy of the tear is the first step.
The classic arthroscopic surgical technique for resection of unstable longitudinal, flap, and parrot beak tears is termed the cut and avulse technique. In this technique, cutting or biting instruments are used to nearly completely detach the large unstable fragment from the remaining meniscus. Maintaining a few fibers intact prevents the formation of a free fragment that may float away. A grasping device is then used to grasp this large fragment and it is then avulsed, typically by repetitive rolling motions that wind up the stress to the small residual area of attachment.
Medial Meniscus Tear Surgery
Multiple tear patterns have been described in the medial meniscus. The more common ones are vertical longitudinal, horizontal cleavage, flap or parrot beak tear, radial tear, and complex tear. Complex tears incorporate at least 2 of the other tear patterns. Tears can also be broken down by their etiology (traumatic or degenerative).
The goal of any meniscal resection is to remove the unstable and damaged meniscus substance while preserving as much normal or nearly normal meniscus as can be reasonably retained. The margins of the tear resection need to be carefully tapered such that there are no sharp transitions at the resection margin.
The first step in any meniscal resection is to define the anatomy of the tear. If the tear cannot be adequately visualized through the use of a post or leg holder and valgus stress, a relaxation technique of needling the medial collateral ligament (MCL) can be of benefit. This can be done through the joint with an 18-gauge spinal needle or percutaneously with a 1.5-in needle with the bevel maintained perpendicular to the MCL fibers. Multiple perforations of the MCL are made just above the meniscus, then gentle to increasingly firm valgus stress is applied until the MCL releases adequately for visualization. This step is key in preventing damage to the articular cartilage during the performance of a meniscectomy. It is only necessary if there is inadequate space to visualize and instrument the meniscus without the release.
Medial Tear Patterns
Vertical longitudinal tears typically occur in the posterior horn and may propagate along the circumferential fibers of the meniscus to the mid and anterior portion. Adequate valgus stress must be applied to facilitate visualization. External rotation of the leg may also assist in visualization by bringing the posterior tibia and attached medial meniscus forward in relationship to the femoral condyle. Attention is typically focused on the posterior lateral extent of the tear for the initial cut. Using scissors or a punch, the far lateral attachment of the unstable segment is cut such that there are only a few remaining fibers. Attention is then focused on the most medial or anterior locus of the tear, which should be completely released using a biter tapered into the axilla of the tear. The released portion of the meniscus can then be grasped and avulsed, typically by repetitive rolling motions. A small motorized shaver (3 to 4 mm) is then used to suction any debris from the release and then to smooth and balance the residual meniscus.
If the vertical longitudinal tear extends too far anteriorly to be able to adequately begin the taper from the anteromedial portal, the anterior release is more easily fashioned with the arthroscope in the anteromedial portal and the cutting instrumented in the anterolateral portal. If a vertical longitudinal tear extends from the posterior horn anterior to the mid or anterior portion of the meniscus, it can be termed a bucket handle tear and may displace to lock the knee. The easiest way to resect a locked bucket handle tear is to reduce it by using valgus stress and a blunt obturator to manipulate it back into a reduced position. In a tight joint with a long-standing displaced segment, reduction of the displaced segment may not be possible. Using the needling technique described to relax the MCL can facilitate the reduction.

Flap tears of the posterior and mid portion of the medial meniscus are relatively common. They can result from a small vertical longitudinal tear that has propagated out through the free border of the meniscus. The resection technique for flap tears is identical to that of a vertical longitudinal tear, except if one is preferentially using the cut and avulse technique, there is only one attachment site and that should not be cut through completely. Tapering of the resection margins is crucial. Flap tears tend to occur more centrally located than the vertical longitudinal tears and are, therefore, in relatively softer, less dense meniscus tissue, which means they may often be readily resected by just the use of a shaver.
Horizontal cleavage tears typically occur in the older population and are more of a degenerative tear pattern. They can typically be thought of with central degeneration within the meniscus that propagates through to the undersurface through a rotation shear. They often cause pain but rarely mechanical symptoms. Typically, these tears are resected using a punch. Since the smaller leaflet is usually the inferior leaflet, that is the preferential one to remove. It is also technically more easily reached because the superior surface of the meniscus tends to ride up behind the condyle when there is a horizontal split. The leaflet that is selected to be removed should be resected back to the level such that there is no longer any pathologic motion between it and the remaining leaflet.
Complex tears are a result of a tear pattern that includes multiple planes. They are more common in older patients in whom the meniscus tissue is somewhat abnormal already. The meniscus should be probed and evaluated to identify the tear pattern as closely as possible prior to resection. Flap tears and vertical longitudinal tears are resected using the techniques previously identified. It is important to be certain that a flap is not left folded under the meniscus. This is typically the case if there is an undersurface flap that is located at the mid portion of the meniscus.

Lateral Meniscal Tear Surgery
The figure-4 position facilitates visualization and instrumentation of the lateral compartment. It is of benefit when anticipating a lateral meniscal tear that the anteromedial portal be slightly higher to facilitate crossing above the tibial spine to instrument the lateral meniscus. If one has a portal that is too low to readily accomplish this, the skin can be retracted somewhat proximally and a new capsular portal cut, allowing ready instrumentation of the lateral compartment.
Lateral Tear Patterns
Different than the posterior horn medial meniscal tear, the vertical longitudinal tear in the posterior horn of the lateral meniscus may be asymptomatic. These should be probed and assessed. If they can be subluxed out from under the condyle anteriorly, they present an issue for recurrent symptoms. Shelbourne and Heinrich demonstrated that if the tears are stable and behind the popliteus hiatus, they rarely cause symptoms and can be left in situ.
The cut and avulse technique remains appropriate for lateral meniscal resections. Because the arthroscope is typically located in the anterolateral portion for visualization of a lateral meniscal tear, attention to the more anterior axilla of the tear is readily accomplished with this position of the arthroscope, and the resection instrumentation is brought in from the anteromedial portal. It is technically difficult to release the posterior axilla of a vertical longitudinal tear in the lateral meniscus if the ACL is intact because the ACL will block access to this area when instruments are used through the anteromedial portal. In this case, it is optimal to switch portals with the arthroscope medial and instrumentation brought in laterally to facilitate an appropriate tapered release.
Flap tears of the lateral meniscus commonly have a flap at the posterior bony attachment of the meniscus. This is frequently associated with an ACL tear, and care must be taken that the bony attachment of the remaining meniscus stays intact. If these tears are small, resection is not necessary. If they are large and could potentially cause mechanical symptoms, resection should be accomplished.
Horizontal tears are less common in the lateral meniscus than on the medial side. This is a degenerative tear pattern, and resection should be based on removing the smaller leaflet as is done on the medial side.
Radial tears are common in the lateral meniscus. They are typically in the mid portion or slightly anterior to mid. If they extend out to the meniscosynovial junction in the vascular area of the meniscus, the deeper portions of these can be repaired with a complex repair. If they are entirely within the thin central portion of the meniscus, resection should be accomplished. The anterior leaflet can be done with the instruments brought in from the anteromedial portal using a side biter. The posterior leaflet can be accomplished through the same portal using a regular biter. Shaving to remove any site that may propagate is appropriate.
Lateral Meniscal Tear With a Meniscal Cyst
Meniscal cysts are more commonly associated with lateral meniscal tears than they are with medial tears. They are typically identified with a degenerative meniscal tear and usually arise from a tear that is just anterior to the mid meniscus. They present with a relatively firm rubbery nodule that may be painful and can be transilluminated. They are readily identifiable by MRI scan. The degenerative torn portion of the meniscus should be resected, and then penetration into the cyst with a small (3.0- to 3.5-mm) shaver is appropriate. One should open the entrance to this cyst adequately so that it will not reform.
Torn Discoid Lateral Meniscus
A discoid meniscus should not be resected unless it is causing mechanical symptoms. If the tear breaks through to the superior surface, it can be readily visualized. If the tear is entirely horizontal within the body of the meniscus or penetrates inferiorly, it can be difficult to visualize. Resection of a discoid meniscus should be carefully contoured to try to create as near a normal meniscus as can be accomplished.
Postoperative Protocol
With the use of supplementary local anesthesia into the portal sites and potentially into the joint, immediate postoperative pain from a partial meniscectomy is minimal. Closure of the incisions can be accomplished in several ways. Cryotherapy can be of benefit in reducing the swelling during the postoperative period. Range of motion exercises, quadriceps setting exercises, and straight leg lifts are appropriate early on to try to maintain quadriceps tone.
Deep vein thrombophlebitis (DVT), although uncommon after a routine meniscectomy, can occur. It is appropriate to take steps to minimize the chance of this. Use elastic compression stockings as a mechanical means to reduce the risk of DVT. Chemoprophylaxis with 325 mg of aspirin once or twice a day for several weeks post knee arthroscopy is also reasonable.
At the first postoperative visit, one should be careful to assess for any signs of DVT. It’s considered to referral to a physical therapist to regain strength and function in select patients. If they are capable of accomplishing this on their own, physical therapy is not a necessity following arthroscopic meniscectomy.
References
- Englund M, Roos EM, Lohmander LS. Impact of type of meniscal tear on radiographic and symptomatic knee osteoarthritis: a sixteen-year followup of meniscectomy with matched controls. Arthritis Rheum. 2003 Aug;48(8):2178-87. doi: 10.1002/art.11088. PMID: 12905471.
- Englund M, Lohmander LS. Risk factors for symptomatic knee osteoarthritis fifteen to twenty‐two years after meniscectomy. Arthritis Rheum. 2004;50(9):2811-2819.
- Roos H, Laurén M, Adalberth T, Roos EM, Jonsson K, Lohmander LS. Knee osteoarthritis after meniscectomy: prevalence of radiographic changes after twenty‐one years, compared with matched controls. Arthritis Rheum. 1998;41(4):687-693.
- Neyret P, Donell ST, Dejour H. Results of partial meniscectomy related to the state of the anterior cruciate ligament. Review at 20 to 35 years. J Bone Joint Surg Br. 1993;75(1):36-40.
- Allen CR, Wong EK, Livesay GA, Sakane M, Fu FH, Woo SL. Importance of the medial meniscus in the anterior cruciate ligament‐deficient knee. J Orthop Res. 2000;18(1):109-115.
- Katz JN, Brophy RH, Chaisson CE, et al. Surgery versus physical therapy for a meniscal tear and osteoarthritis. N Engl J Med. 2013;368(18):1675-1684.
- Terry GC, Tagert BE, Young MJ. Reliability of the clinical assessment in predicting the cause of internal derangements of the knee. Arthroscopy. 1995;11(5):568-576.
- Eren OT. The accuracy of joint line tenderness by physical examination in the diagnosis of meniscal tears. Arthroscopy. 2003;19(8):850-854.
- Evans PJ, Bell GD, Frank C. Prospective evaluation of the McMurray test. Am J Sports Med. 1993;21(4):604-608.
- Rosenberg TD, Paulos LE, Parker RD, Coward DB, Scott SM. The forty-five-degree posteroanterior flexion weight-bearing radiograph of the knee. J Bone Joint Surg Am. 1988;70(10):1479-1483.
- Konan S, Rayan F, Haddad FS. Do physical diagnostic tests accurately detect meniscal tears? Knee Surg Sports Traumatol Arthrosc. 2009;17(7):806-811.
- Shetty AA, Tindall AJ, James KD, Relwani J, Fernando KW. Accuracy of hand-held ultrasound scanning in detecting meniscal tears. J Bone Joint Surg Br. 2008;90(8):1045-1048.
- Shelbourne KD, Heinrich J. The long-term evaluation of lateral meniscus tears left in situ at the time of anterior cruciate ligament reconstruction. Arthroscopy. 2004;20(4):346-351.
- Goodwin PC, Morrissey MC, Omar RZ, Brown M, Southall K, McAuliffe TB. Effectiveness of supervised physical therapy in the early period after arthroscopic partial meniscectomy. Phys Ther. 2003;83(6):520-535.
- Sherman OH, Fox JM, Snyder SJ, et al. Arthroscopy—“no-problem surgery.” An analysis of complications in two thousand six hundred and 40 cases. J Bone Joint Surg Am. 1986;68(2):256-265.
- Son IJ, Kim MK, Kim JY, Kim JG. Osteonecrosis of the knee after arthroscopic partial meniscectomy. Knee Surg Relat Res. 2013;25(3):150-154.