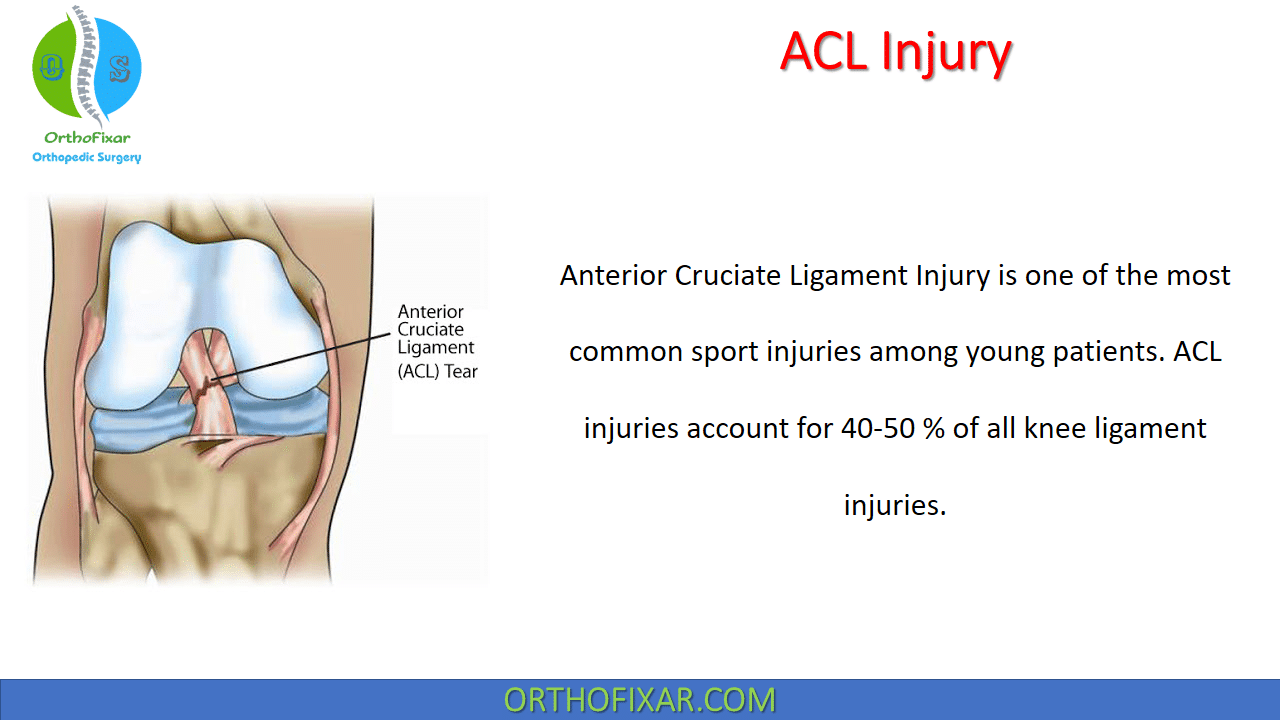
Anterior Cruciate Ligament Injury is one of the most common sport injuries among young patients. ACL injury accounts for 40-50 % of all knee ligament injuries.
Female athletes have a 2 to 8 times higher risk of ACL tear compared to male athletes because:
- Women have a greater total valgus knee loading in landing.
- Women land more erect.
- Women have increased quadriceps-to-hamstring strength, causing increased anterior sheer.
- Smaller notches, smaller ligaments (reduced area in cross section), increased generalized ligament laxity, and increased knee laxity are additional proposed factors.
Anatomy of the ACL:
The anterior cruciate ligament is composed of longitudinally oriented bundles of collagen tissue (90% type I collagen and 10% type III collagen). The ligament is surrounded by synovium making it extrasynovial structure. The ligament is 31 to 35 mm in length, and 11 mm in diameter.
The anterior cruciate ligament originates from a semicircular area on the posteromedial aspect of the lateral femoral condyle and inserts on the tibial plateau, on a broad, irregular, oval area anterior and between the spines of the tibia. The tibial attachment site is larger and more secure than the femoral site.
Tension in the anterior cruciate ligament is least at 30 to 40 degrees of knee flexion.
See Also: Knee Meniscus Anatomy
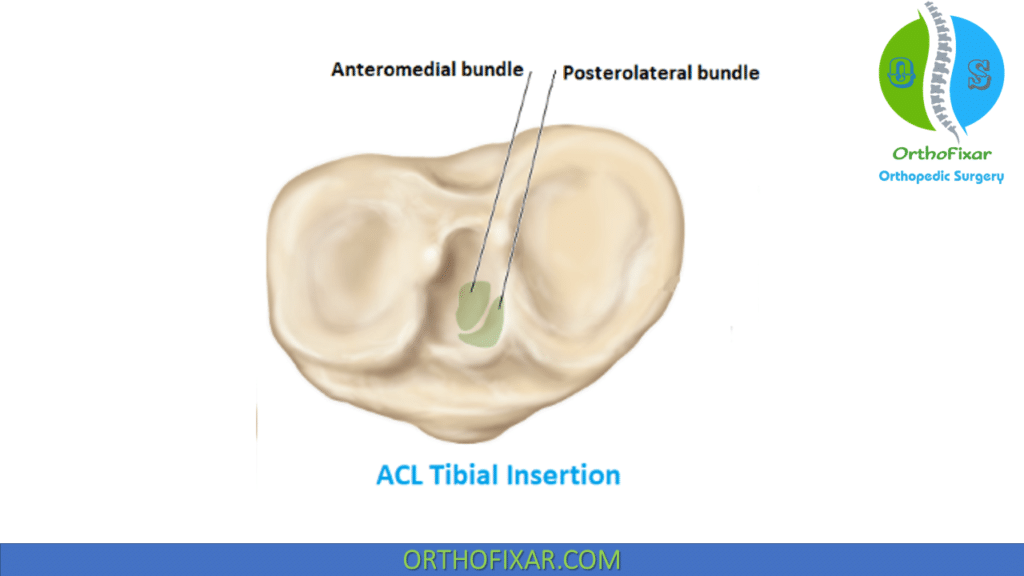
The ACL has two bundles:
- Anteromedial bundle:
- It is tight in flexion.
- Primarily an anterior restraint.
- Evaluated by Lachman test and anterior drawer test.
- Posterolateral bundle:
- Tight in extension.
- Primarily a rotatory restraint.
- Evaluated by pivot shift test.
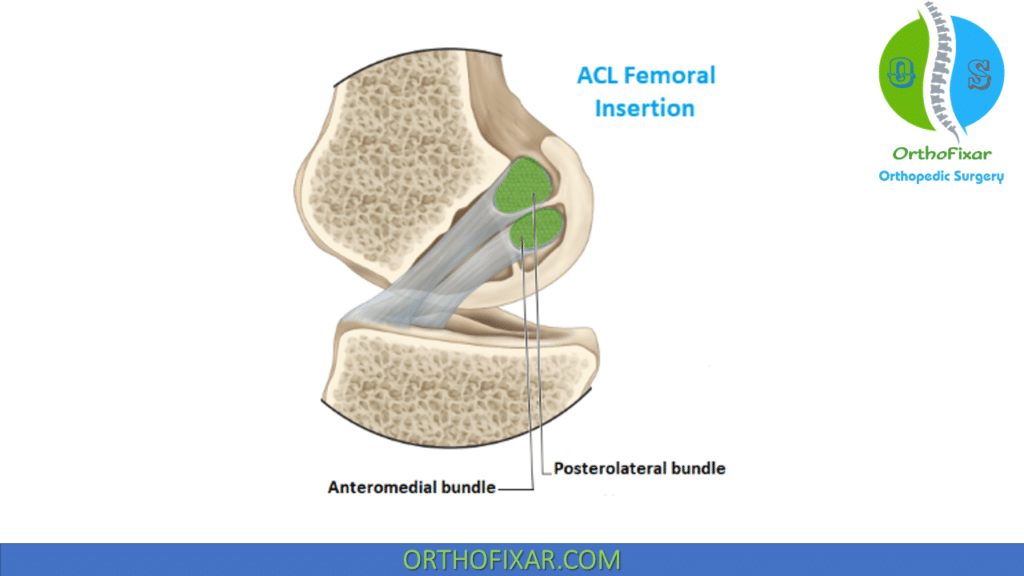
The ACL secondary function is to resist tibial rotation and varus-valgus angulation at full extension. The anterior cruciate ligament has proprioceptive function, as evidenced by the presence of mechanoreceptors in the ligament.
ACL Blood Supply and Innervation:
Anterior cruciate ligament receives its blood supply via branches of the middle genicular artery. Additional supply comes from the retro-patellar fat pad via the inferior medial and lateral geniculate arteries.
The osseous attachments of the anterior cruciate ligament contribute little to its vascularity. The posterior articular nerve, a branch of the tibial nerve, innervates the anterior cruciate ligament.
Mechanism of injury
Mechanism of ACL injury is typically a valgus load with internal tibial rotation and anterior tibial translation while the knee is in almost full extension.
Associated injuries
- Acute lateral meniscus tears are more common than acute medial tears.
- Medial meniscus tears occur more often with chronic anterior cruciate ligament deficiency.
- Medial collateral ligament injuries occur in approximately 25% of cases.
- Posterolateral corner (PLC) injuries occur in approximately 10% of cases.
See Also: Knee Meniscus Tear
Clinical Evaluation
Symptoms & Signs:
ACL injury is commonly associated with an audible felt “pop”. Hemarthrosis usually begins within 12 hours of injury.
Pain, instability and inability to return to sport are also important symptoms of ACL injury.
Physical Examination:
ACL injuries can be detected using these special tests:
- The Lachman test is the most sensitive examination for acute anterior cruciate ligament injuries.
- The pivot shift test.
- The anterior drawer test of the knee.
Imaging Evaluation
Plain radiographs:
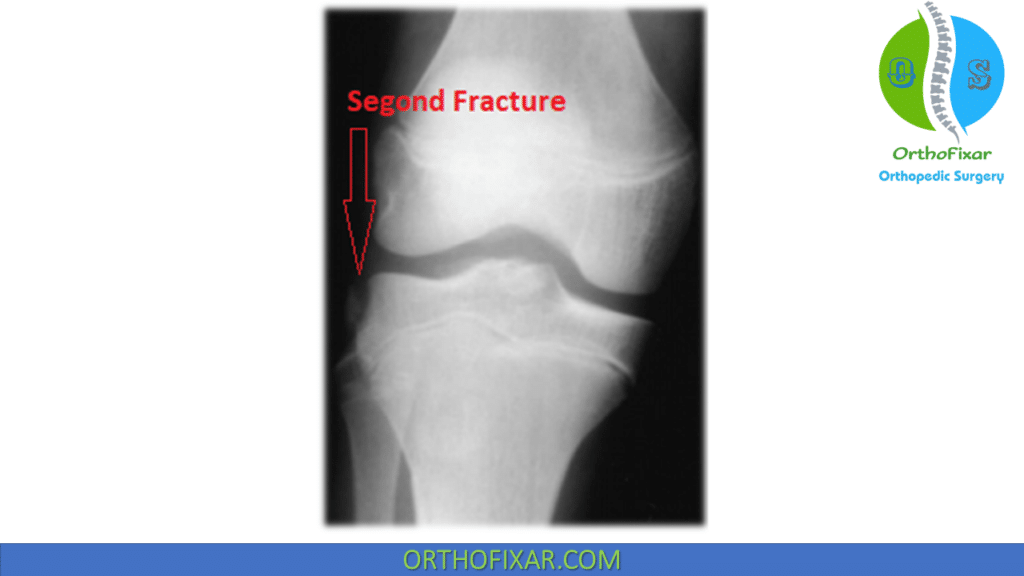
AP View: Segond fracture (an avulsion fracture of the lateral capsule) is pathognomonic for an ACL tear.
Lateral View: look for the degree of posterior tibial slope. Values greater than 13 degrees have been associated with ACL failure.
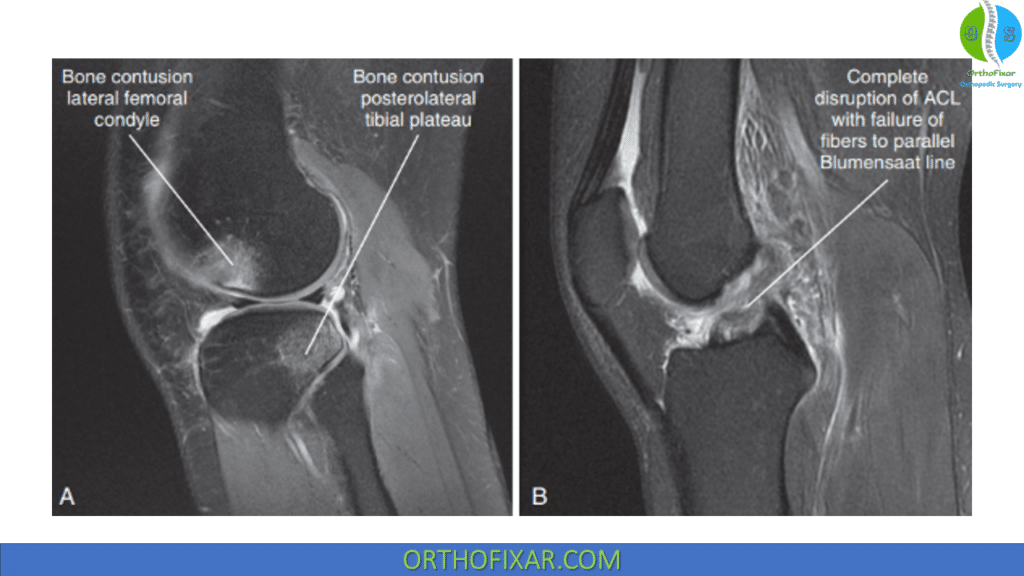
MRI: it is useful in confirming the diagnosis of ACL tear. Signs of an ACL tear that are seen on MRI include:
- Disruption of ACL fibers.
- Fibers no longer parallel to Blumensaat line.
- Inability to visualize fibers of ACL.
- “Empty lateral wall” or “empty notch” sign indicating avulsion of ACL from the femoral origin
- Bone bruises (trabecular microfractures) occur in more than half of acute ACL tears.
On sagittal imaging, fibers of an intact ACL should parallel the Blumensaat line.
Treatment Of ACL Tear
Treatment choice of ACL tear should be selected based on:
- The age.
- Activity level.
- Instability.
- Associated injuries.
- Other medical factors.
Primary repair of ACL tears is not currently recommended, because myofibroblasts cover the end of the ACL stumps, making primary healing impossible.
Initial treatment of ACL tear consists of:
- Physical therapy for mobilization (Immobilization is avoided).
- Full ROM and good quadriceps control should be achieved prior to surgery.
ACL Surgical Treatment:
ACL surgery with reconstruction indications include:
- Younger age.
- Older but active patients.
- Active patients.
- Children.
- Prior ACL reconstruction failure.
ACL reconstruction Methodes:
Single-bundle graft reconstruction is the most commonly performed reconstruction. Graft selection depends on patient factors and surgeon’s preference.
Graft types include:
- A bone-patella-tendon-bone (BPTB) autograft.
- A four-strand hamstring autograft.
- A quadriceps tendon autograft.
- An allograft.
1. Bone-Patella-Tendon-Bone (BPTB) Autograft:
Bone-Patella-Tendon-Bone (BPTB) Autograft demonstrates faster incorporation into the bone tunnels than does hamstring autograft. It’s often the graft of choice for patients who desire an early return to sports activity.
There is a higher incidence of arthritis associated with the use of BPTB autograft than with hamstring autograft 5 to 7 years after ACL reconstruction.

BPTB autograft harvest risks include:
- Anterior knee pain.
- Pain with kneeling.
- Loss of extension.
- Poorer recovery of quadriceps strength.
2. Hamstring Autograft:
Its advantages include:
- Smaller incision.
- Less peri-operative pain.
- Less anterior knee pain.
Fixation strength may be less than Bone-Patella-Tendon-Bone (BPTB). It carries the risk of weakness of knee flexion and internal rotation, along with injury to branches of the saphenous nerve.
3. Allograft:
Allograft may be associated with a higher rate of rupture in younger, more active patients.
Chemical-processed or irradiated allografts have demonstrated increased rates of failure compared to fresh-frozen allografts.
Allografts have been demonstrated to incorporate into bone tunnels more slowly.
Allograft risk also includes infection risk.
Associated injuries treatment:
- MCL injury: Allow MCL to heal (varus/valgus stability) and then perform ACL reconstruction.
- Meniscus tear: Meniscal repair should be performed at same time as ACL reconstruction. This increases meniscal healing rate when repaired at the same time with ACL tear.
- Posterolateral corner injury: Reconstruct at the same time as ACL or as 1st stage of a 2 stage reconstruction.
Postoperative Rehabilitation:
Exercises that do not endanger the ACL graft:
- Exercises dominated by the hamstrings (isometric hamstrings) .
- Exercises that result in quadriceps activity with the knee flexed beyond 60 degrees.
- Exercises involving active knee ROM between 35 and 90 degrees of flexion.
Closed-chain rehabilitation (fixation of terminal segment of extremity [i.e., foot planted]) and compressive loading have been emphasized because they allow physiologic contraction of the muscles around the knee.
Open-chain extension exercises place increased stress on the reconstructed ACL and should be avoided for the first 6 weeks.
Early progressive eccentric exercise has yielded good initial results in terms of quadriceps and gluteus maximus muscle size and function after ACL reconstruction
Complications after ACL reconstruction:
- Tunnel malposition: the most common technical error:
- Vertical graft placement results in decreased rotational stability.
- Anterior placement of the femoral tunnel results in limited flexion.
- Arthrofibrosis: often occurs with reconstruction for acute ACL tears.
- Aberrant hardware placement
- Infection: occurs in less than 1% of cases.
- Graft contamination:
- Graft contamination by dropping on the floor is rare.
- The majority of surgeon favored retention of the graft with disinfection rather than harvesting a new autograft or switching to allograft.
- A combination of chlorhexidine gluconate and triple antibiotic solution (gentamicin, clindamycin, polymyxin) in sterile saline appears to be the most effective disinfecting regime.
- Infrapatellar contracture syndrome.
- Patella Tendon Rupture.
- Patella fracture.
- Late arthritis.
- Tunnel osteolysis.
- Local nerve irritation : saphenous nerve.
References & More
- Campbel’s Operative Orthopaedics 12th edition Book.
- Millers Review of Orthopaedics -7th Edition Book.
- Evans J, Nielson Jl. Anterior Cruciate Ligament Knee Injuries. [Updated 2022 May 5]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK499848/