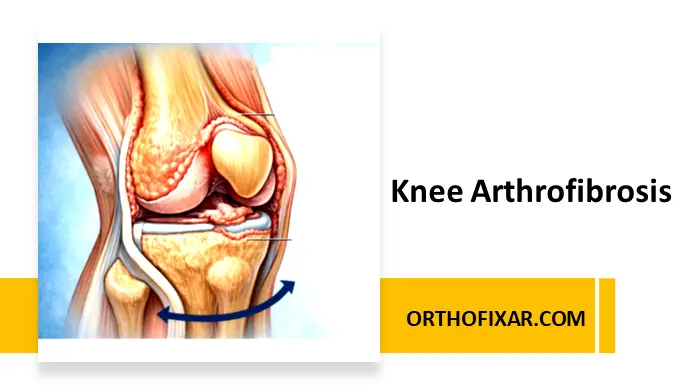
Knee arthrofibrosis refers to a spectrum of pathological knee conditions in which loss of joint motion is the primary clinical feature. It is characterized by excessive fibrous scar tissue formation, leading to progressive stiffness and restricted mobility of the knee joint.
This condition involves a proliferative fibroplastic response, where dense adhesions develop both intra-articularly and extra-articularly. Over time, these adhesions can extend and significantly impair normal joint mechanics.
In advanced cases, the accumulation of scar tissue may obliterate key anatomical spaces within the knee, including:
- Parapatellar recesses
- Suprapatellar pouch
- Intercondylar notch
- Articular surfaces
As the disease progresses, secondary complications such as patella infera (low-lying patella) and chronic patellar entrapment may occur, further contributing to functional limitation and pain.
Historically, Arthrofibrosis of the knee was first described in 1951 as a fibroplastic response of the joint following trauma, highlighting its strong association with injury, surgery, or inflammation.

Knee Arthrofibrosis Causes
Knee arthrofibrosis commonly develops as a result of an exaggerated inflammatory response following knee injury or surgical intervention. This inflammatory cascade triggers excessive fibrous tissue formation, leading to progressive joint stiffness and restricted range of motion.
Although inflammation occurs in many patients after trauma or surgery, it remains unclear why some individuals develop a more aggressive form of knee arthrofibrosis with severe motion limitation.
Diagnosis of Knee Arthrofibrosis
Accurate diagnosis of knee arthrofibrosis requires careful clinical evaluation and the exclusion of other causes of limited knee motion. Both active and passive range of motion should be assessed, and alternative mechanical factors must be ruled out.
Common mechanical causes of restricted knee motion include:
- Loss of articular congruency (e.g., due to fractures or joint surface irregularities)
- Meniscal tears
- Presence of a loose body within the joint
- Disruption of the extensor or flexor mechanism
- Significant joint effusion (swelling)
- Improper (non-isometric) placement of grafts during ACL reconstruction
Risk Factors for Knee Arthrofibrosis
Several factors may increase the risk of developing knee arthrofibrosis, particularly after surgery:
- Early ACL reconstruction (within 3 weeks of injury): Some studies suggest this may increase risk, although evidence remains controversial
- Poor or inadequate rehabilitation before or after surgery
- Delayed mobilization protocols, leading to prolonged joint stiffness
- Lack of supervised physiotherapy, which is essential for maintaining knee range of motion

Clinical Evaluation
Patients with knee arthrofibrosis typically present with persistent knee stiffness, pain, and a characteristic painful flexed-knee gait. During the active inflammatory phase, clinical signs such as joint warmth, swelling, and periarticular muscle atrophy are commonly observed.
Key Clinical Signs
The most important physical examination findings in knee arthrofibrosis include:
- Reduced range of motion (ROM) affecting both flexion and extension
- Decreased patellar mobility (patellar glide restriction)
- Painful and stiff knee movement
- Muscle wasting, particularly of the quadriceps
It is important to note that some degree of reduced patellar mobility can occur as part of the normal healing process—typically between weeks 4 and 12—with gradual improvement expected by week 16. This distinction is crucial to avoid overdiagnosis.
See Also: Complex Regional Pain Syndrome (CRPS)
Quadriceps Weakness and Functional Impact
Quadriceps inhibition or weakness is a common finding, often due to pain and joint dysfunction. As quadriceps function declines, its role as a shock absorber is compromised, potentially leading to increased stress on the articular cartilage and further joint degeneration.
Patients frequently hold the knee in a flexed position, which contributes to:
- Tightening of the posterior joint capsule
- Shortening of the hamstring muscles
- Worsening of knee stiffness over time
Additional Symptoms
Other commonly reported symptoms include:
- Crepitus (joint grinding or clicking)
- Knee swelling, especially after prolonged standing or walking
- Generalized weakness and fatigue in the affected limb
Even in the absence of significant pain, loss of motion and quadriceps weakness can severely impair activities of daily living (ADLs) such as walking, climbing stairs, or standing for extended periods.
Gait and Movement Abnormalities
A typical finding is an antalgic gait with a flexed knee posture, reflecting both pain avoidance and mechanical restriction.
On examination:
- Both active and passive knee movements are restricted
- Motion limitation often follows a capsular pattern
- Patellar glides (mediolateral and superoinferior) are reduced
Passive motion may demonstrate a characteristic “springy” or firm end-feel, which reflects the presence of dense, fibrotic, and inflamed periarticular tissue.
Imaging
Imaging plays a key role in the diagnosis and assessment of knee arthrofibrosis, helping to identify structural abnormalities and rule out other causes of restricted knee motion.
Standard X-rays for Knee Arthrofibrosis
A complete radiographic evaluation of the knee should include:
- Anteroposterior (AP) view
- Bent-knee posteroanterior (PA) view
- Merchant (axial patellofemoral) view
- Lateral view at 30° of knee flexion
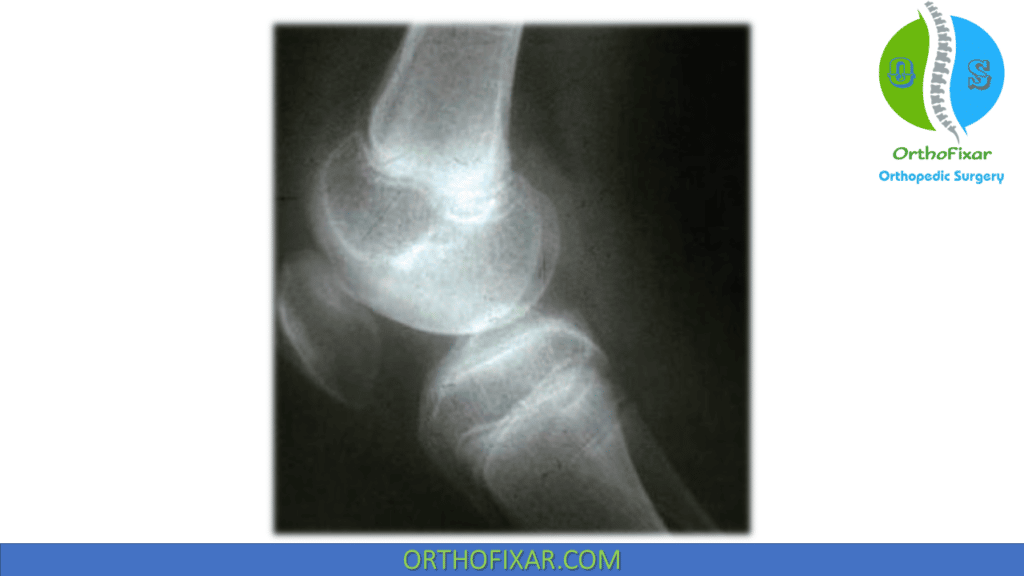
The lateral X-ray is particularly important for assessing patella infera (patella baja), a common complication of knee arthrofibrosis.
Modified Insall–Salvati Ratio
The position of the patella is evaluated using the modified Insall–Salvati ratio, which compares:
- Patellar tendon length: measured from the inferior pole of the patella to the tibial tubercle
- Patellar length: measured along its greatest diagonal (superior to inferior pole)
A normal ratio is approximately 1:1, with slight variations between individuals.
- A ratio < 0.8 is indicative of patella infera, which may contribute to anterior knee pain and limited motion.
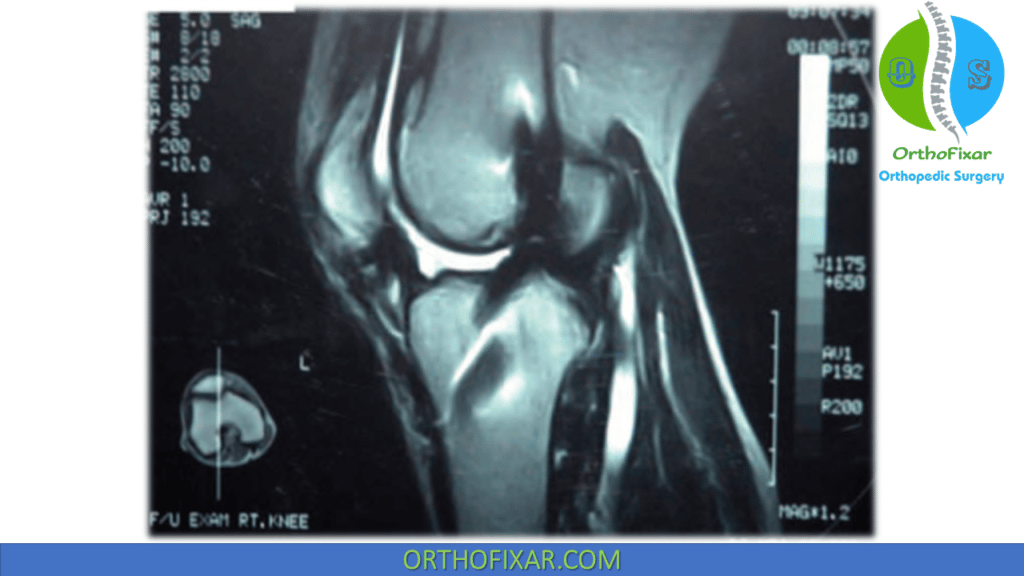
MRI in Knee Arthrofibrosis
Magnetic resonance imaging (MRI) is a valuable adjunct in evaluating soft tissue pathology associated with knee arthrofibrosis. It is particularly useful for identifying:
- Anterior knee impingement
- Excessive (exuberant) scar tissue formation
- Improper graft placement, especially after ACL reconstruction
- Presence of a “pseudopatellar tendon”, representing fibrotic tissue mimicking the normal tendon
MRI provides detailed visualization of both intra-articular and periarticular structures, making it essential in complex or unclear cases.
Arthrofibrosis Classification
Knee motion loss can be graded based on deviation from normal flexion and extension or by the pathoanatomy causing the motion loss. Del Pizzo et al classified motion loss into the following 3 groups:
- Group 1 consisted of knees with extension less than 5 degrees and flexion greater than 110 degrees,
- Group 2 had extension of 5 to 10 degrees with flexion between 90 and 110 degrees,
- Group 3 was limited to extension greater than 10 degrees or flexion less than 90 degrees.
These were characterized as mild, moderate, and severe, respectively.
Knee Arthrofibrosis has also been classified by its pathoanatomy:
In the suprapatellar classification by Sprague et al:
- Group 1 consisted of discreet bands or a single sheet of adhesions traversing the suprapatellar pouch.
- Group 2 involved complete obliteration of the suprapatellar pouch and peripatellar gutters with masses of adhesions,
- Group 3 included the above with extracapsular involvement with bands of tissue from the proximal patella to anterior femur. Suprapatellar adhesions result in flexion loss only.
Infrapatellar entrapment may be associated with atypical pain, loss of extension and flexion, and sometimes patella infera. It can be classified as primary or secondary, such as entrapment caused by nonisometric graft placement. It can also be divided into 3 distinct stages:
- Stage I, the prodromal stage, there is periarticular inflammation and swelling combined with immobility and quadriceps weakness as demonstrated by an extension lag. Tenderness is noted about the patellar tendon and active ROM is painful. There is decreased excursion of patellar glide tests and patellar tilt, although not rigidly fixed in the early stage.
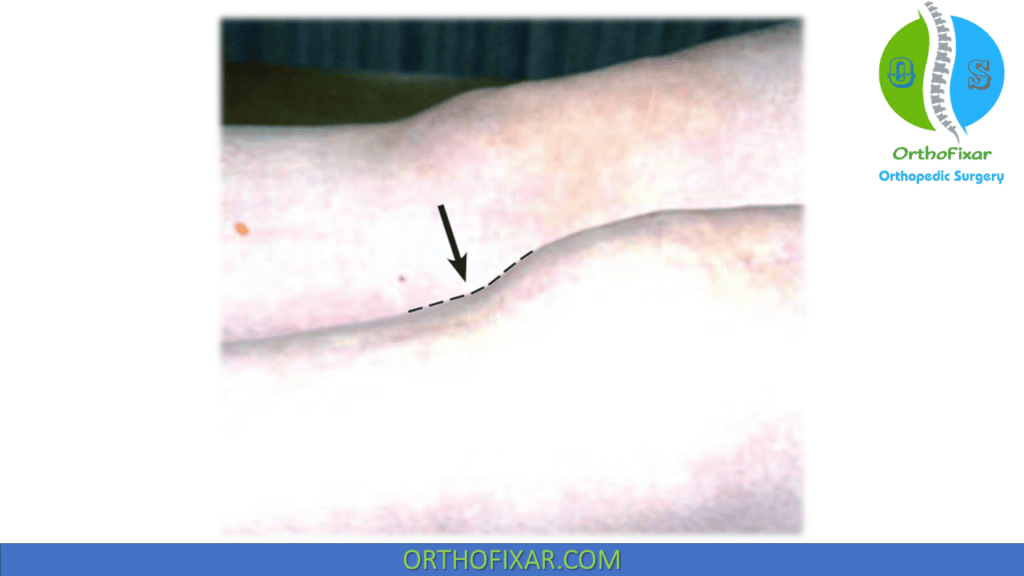
- Stage II, the active stage, there is essentially no patellar tilt, decreased medial to lateral glide, and loss of anterior tilt. There may be a positive shelf sign. A positive shelf sign is characterized by an increased slope between the inferior pole of the patella and the proximal tibia with the knee in extension. A positive shelf sign is typically a late finding that indicates significant chronicity and possible patella infera. Its appearance is due to the adhesion of the patella tendon to the anterior tibia.
- Stage III, the residual stage, is characterized by slightly more supple peripatellar and retinacular tissues but with more significant patellofemoral arthrosis as demonstrated by patellofemoral crepitation on examination and decreased joint space seen on x-rays. Patella infera is usually present.
Knee Arthrofibrosis Treatment
Knee Arthrofibrosis Treatment includes:
- Anti-inflammatory drugs
- ROM exercises and the stretching of specific structures.
- When a plateau has been reached during rehabilitative efforts to restore motion or when there is progressive loss of motion, additional intervention of a gentle manipulation of the knee under anesthesia may result in improvement. Closed manipulation or vigorous attempts to gain passive motion may cause indiscriminate tearing of intraarticular tissue, excessive tibiofemoral and patellofemoral compression with the risk of chondral damage or fracture, rupture of the patellar ligament, and even femoral fracture. Manipulation has also been noted to initiate complex regional pain syndrome (CRPS).
Operative treatment of Knee Arthrofibrosis indications include:
- Decreased ROM: Pain and decreased ROM after ligament reconstruction surgery, especially when performed during the acute phase and in combination with extra-articular procedures.
- Failure of nonoperative treatment or manipulation alone: Patients who have failed to regain full ROM within 4 to 6 weeks after surgery should be counseled regarding possible intervention for Knee arthrofibrosis.
- If manipulation followed by judicious physical therapy, anti-inflammatory drugs, and hamstring stretching exercises between weeks 6 and 12 fails to bring about progress, then arthroscopic management is indicated typically between weeks 10 and 12.
Active inflammation: Surgical intervention should not be considered if the knee is still actively inflamed.
Extensor lag: Surgery should be delayed when there is an extensor lag. There should be full quad activation and strength prior to consideration of arthroscopic lysis of adhesions in the joint so as to maintain extension gains.
References
- Usher KM, Zhu S, Mavropalias G, Carrino JA, Zhao J, Xu J. Pathological mechanisms and therapeutic outlooks for arthrofibrosis. Bone Res. 2019 Mar 26;7:9. doi: 10.1038/s41413-019-0047-x. PMID: 30937213; PMCID: PMC6433953. Pubmed
- Shelbourne KD, Patel DV, Martini DJ. Classification and management of arthrofibrosis of the knee after anterior cruciate ligament reconstruction. Am J Sports Med. 1996 Nov-Dec;24(6):857-62. doi: 10.1177/036354659602400625. PMID: 8947412.
- Sprague NF, III.: Motion-limiting arthrofibrosis of the knee: the role of arthroscopic management. Clin Sports Med 6:537–549, 1987.
- Steadman JR, Burns TP, Peloza J, et al: Surgical treatment of arthrofibrosis of the knee. J Orthop Tech 1:119–127, 1993
- Cosgarea AJ, DeHaven KE, Lovelock JE: The surgical treatment of arthrofibrosis of the knee. Am J Sports Med 22:184–191, 1994
- Klein W, Shah N, Gassen A: Arthroscopic management of postoperative arthrofibrosis of the knee joint: Indication, technique, and results. Arthroscopy 10:591–597, 1994.
- Sebastianelli WJ, Gillespie MJ, Hicks DG, et al: The histopathology of arthrofibrosis. Arthroscopy 9:359–360, 1993.
- Shelbourne KD, Johnson GE: Outpatient surgical management of arthrofibrosis after anterior cruciate ligament surgery. Am J Sports Med 22:192–197, 1994.
- Lindenfeld TN, Wojtys EM, Husain A: Operative Treatment of Arthrofibrosis of the Knee. J Bone Joint Surg Am 81-A:1772–1784, 1999.
- Delcogliano A, Franzese S, Branca A, et al: Light and scan electron microscopic analysis of cyclops syndrome: Etiopathogenic hypothesis and technical solutions. Knee Surg Sports Traumatol Arthrosc 4:194–199, 1996.
- Jackson DW, Schaefer RK: Cyclops syndrome: Loss of extension following intra-articular anterior cruciate ligament reconstruction. Arthroscopy 6:171–178, 1990.
- Shelbourne KD, Wilckens JH, Mollabashy A, et al: Arthrofibrosis in acute anterior cruciate ligament reconstruction. The effect of timing of reconstruction and rehabilitation. Am J Sports Med 19:332–336, 1991.