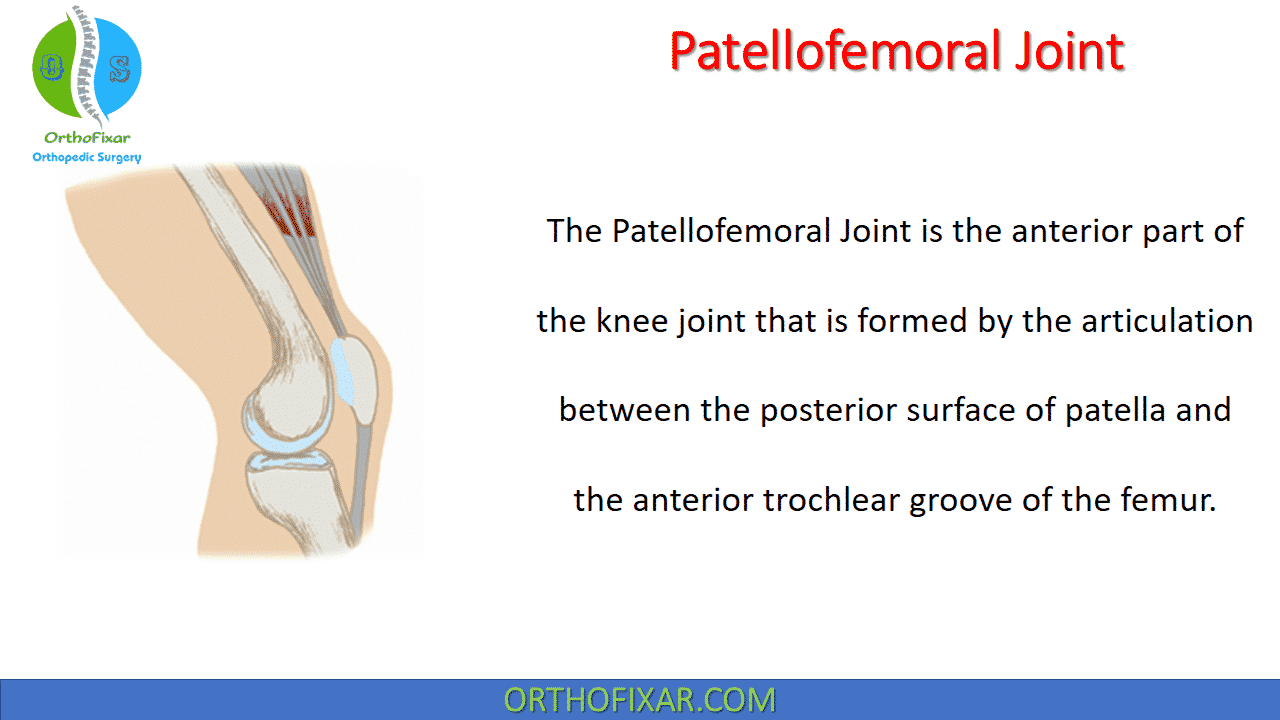
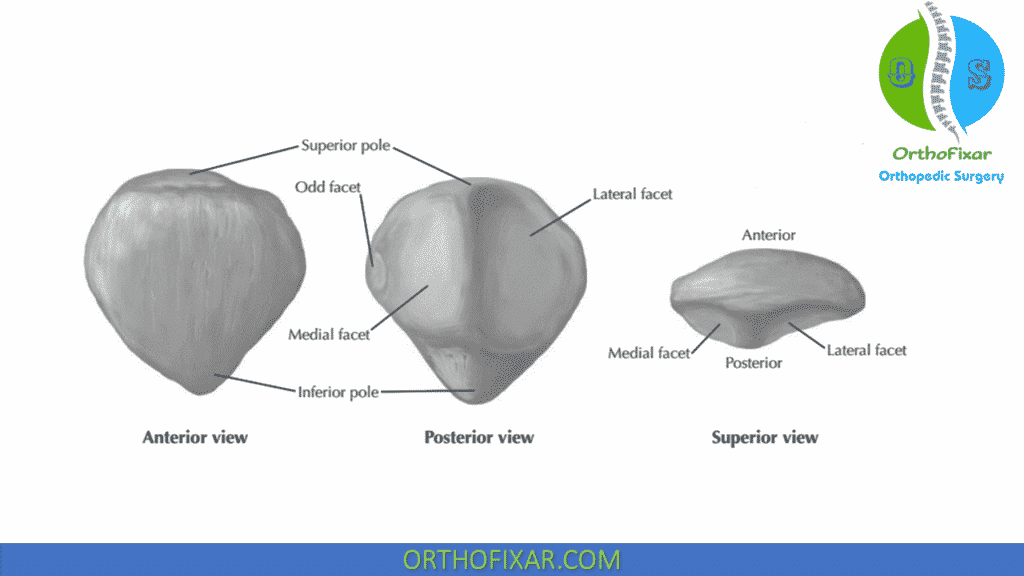
Patellofemoral Joint, the anterior part of the knee, is formed by articulation between posterior surface of patella and anterior trochlear groove of the femur.
Patellofemoral Joint Stability
[tele]
The patella is an inactive component of the knee extensor mechanism, in which the static and dynamic interactions of the underlying tibia and femur determine the patellar tracking pattern. As the knee flexes, the compression forces between the patella and the femur increase as the contact surface area increases, in an attempt to normalize the contact stress unit load. Even though the surface area increases with knee flexion, it cannot keep up with these increased joint reaction forces. To assist in the control of the forces around the patellofemoral joint, there are a number of static and dynamic restraints.
See Also: Knee Muscles Anatomy
Static Restraints
The static restraints of the Patellofemoral Joint include the following:
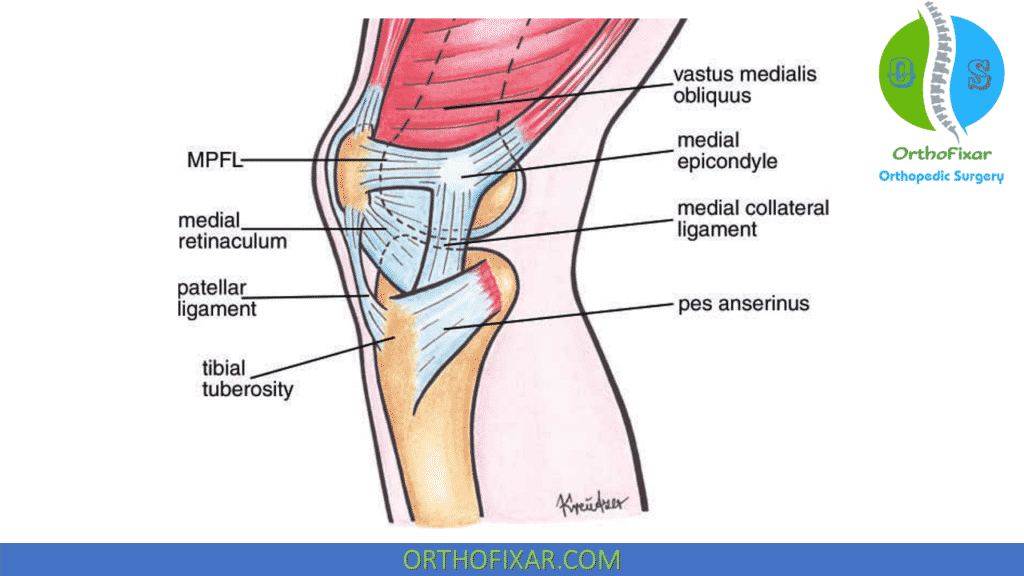
Medial retinaculum:
Although not as robust as its lateral counterpart, the medial retinaculum is the primary static restraint to lateral patellar displacement at 20 degrees of knee flexion, contributing 60% of the total restraining force.
Bony configuration of the trochlea:
The patellofemoral joint is intrinsically unstable because the tibial tubercle lies lateral to the long axis of the femur and the quadriceps muscle and the patella is therefore subject to a laterally directed force. If the patella fails to engage securely in the patellar groove at the start of flexion, it slips laterally, and as flexion continues, it can dislocate completely or slip back medially to its correct position.
The causes of insufficient engagement include:
- Abnormally high patella,
- Patellar dysplasia,
- Poorly developed patellar groove (trochlea).
Medial patellomeniscal ligament and lateral retinaculum:
These structures contribute 13% and 10% of the restraint to translation of the patella, respectively.
Passive restraints:
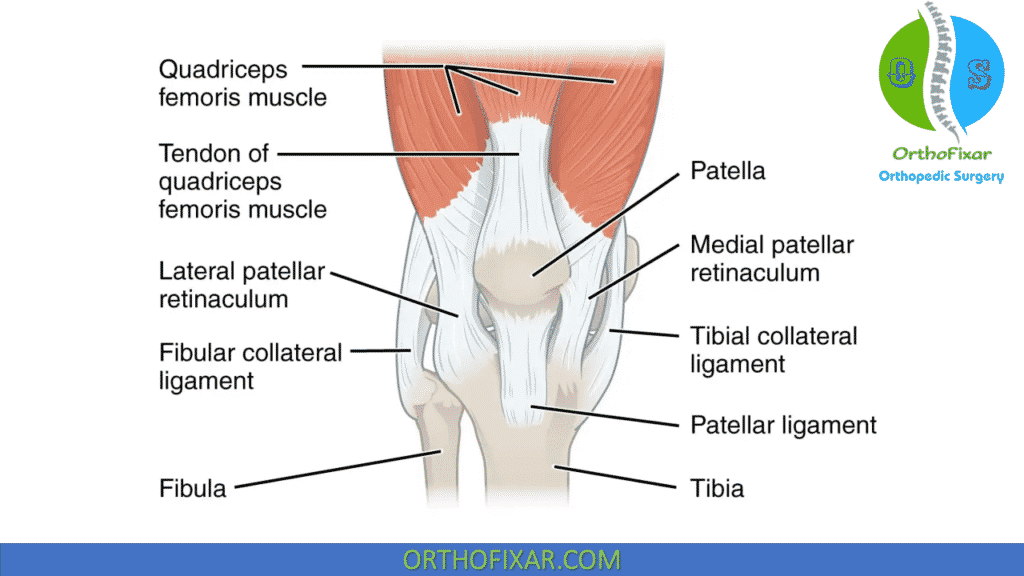
The passive restraints to translation of the patella are provided by the structures that form the superficial and deep lateral retinaculum.
[tele]
Dynamic Restraints
The primary dynamic restraints to patellar motion are the quadriceps muscles, particularly the Vastus Medialis Oblique (VMO). The activity of the VMO increases as the torque around the knee increases, and it provides the only dynamic medial stability for the patella. However, the muscle vector of the VMO is more vertical than normal when a patellar malalignment is present, making it less effective as a dynamic stabilizer.
The timing of the VMO contractions relative to those of other muscles, especially the Vastus Lateralis (VL), also appears to be critical and has been found to be abnormal with patellar malalignment.
Deficits in the timing of muscle activity have been identified in other musculoskeletal conditions such as lower back pain, in which the EMG activity of transversus abdominus has been shown to be delayed compared with a control group.
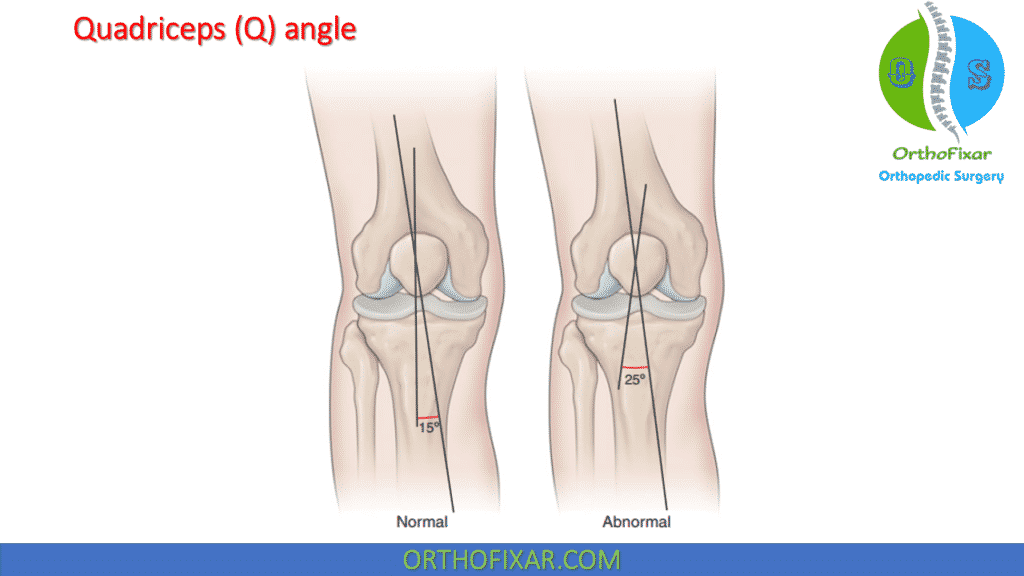
Quadriceps (Q) angle
The quadriceps (Q) angle can be described as the angle formed by the bisection of two lines, one line drawn from the ASIS to the center of the patella, and the other line drawn from the center of the patella to the tibial tubercle.
The normal values are 8–14 degrees for males and 15–17 degrees for females.
See Also: Knee Q Angle
Patella–Femur Contact and Loading
In view of the frequent problems associated with the patellofemoral joint, it is remarkable that, for much of the time, the articulating surfaces of this joint are not even in contact. Indeed, there is no bone-to-bone contact with the femur in full knee extension, or during standing or walking on level ground.
The amount of contact between the patella and the femur appears to vary according to a number of factors, including:
- Angle of knee flexion,
- Location of contact,
- Surface area of contact,
- Patellofemoral joint reaction force (PJRF)
Angle of Knee Flexion
As knee flexion proceeds, the quadriceps vector becomes more perpendicular, and the force on the patella gradually increases. This increasing force is somewhat dissipated by the increased patellofemoral contact with increasing flexion (see later discussion). However, because the force increases more rapidly than the surface area, the stress on the patella increases significantly with flexion.
Any muscle imbalance between the lateral and medial quadriceps muscles can affect the patellar alignment and distribution of pressure in the lower flexion angles of less than 60 degrees. This can produce a rotation of the patella in the coronal plane. At higher flexion angles, imbalances are likely to produce a tilt of the patella in the sagittal plane.
Location of Contact
In the normal knee, as the knee flexes from 10 to 90 degrees, the contact area shifts gradually from the distal to the proximal pole of the patella:
- At full extension, the patella is not in contact with the femur, but rests on the supratrochlear fat pad.
- From full extension to 10 degrees of flexion, the tibia internally rotates, allowing the patella to move into the trochlea. This brings the distal third of the patellar into contact with the femur.
- From 10 to 20 degrees of flexion, the patella contacts the lateral surface of the femur on the inferior patellar surface.
- At around 30–60 degrees of flexion, the middle surfaces of the inferior aspect of the patellar come into contact with the femur, at which point the patella is well seated in the groove.
- As the knee continues to flex to 90 degrees, the patella moves laterally, and the area of patella contact moves proximally.
- At 90 degrees of knee flexion, the entire articular surface of the patella (except the odd facet) is in contact with the femur.
- Beyond 90 degrees, the patella rides down into the intercondylar notch. At this point, the medial and lateral surfaces of the patella are in contact with the femur, and the quadriceps tendon articulates with the patellar groove of the femur.
- At approximately 120 degrees of knee flexion, there is no contact between the patella and the medial femoral condyle.
- At 135 degrees of knee flexion, the odd facet of the patella makes contact with the medial femoral condyle.
Surface Area of Contact
Knowledge of the patellofemoral contact pattern is useful for determining the limits of motion when patients with patellofemoral symptoms perform open kinetic chain (OKC) and closed kinetic chain (CKC) exercises. Some authors have proposed that the contact area quadruples as the knee flexes from 20 to 90 degrees.
Patellofemoral Joint Reaction Force
The PJRF is a function of quadriceps and patellar tendon tension and of the angle formed between the quadriceps and patellar tendon. These forces are caused by the increase in patellar and quadriceps tendon tension and the increase in the acuity of the Q-angle that occurs during knee flexion.
OKC and CKC exercises produce different effects on PJRF and contact stress per unit area:
- During OKC extension, the flexion moment arm for the knee increases as the knee extends from 90 degrees of flexion to full extension (0 degree), resulting in increased quadriceps and patellar tendon tension and increasing PJRFs. Clinicians most often allow OKC exercises at 90–40 degrees of knee flexion as this range provides the lowest PJRF while producing the greatest amount of patellofemoral contact area.
- During CKC exercises, the flexion moment arm of the knee increases as the angle of knee flexion increases. Maximum force in the quadriceps muscle and patellar tendon is generated at 60 degrees of flexion with values approaching 3000 N. CKC, such as the leg press and wall squat, are typically prescribed initially at 0–16 degrees and then progressed to 0–30 degrees where the PJRFs are lower.
Patellar Tracking
Patellar tracking, specifically patella maltracking, continues to be the subject of much study.
In the normal knee, the patella glides in a sinuous path inferiorly and superiorly during flexion and extension, respectively, covering a distance of 5–7 cm with respect to the femur. A concave, lateral, C-shaped curve is produced by the patella as it moves from approximately 120 degrees of knee flexion toward approximately 30 degrees of knee extension. The lateral curve produces a gradual medial glide of the patella from 45 to 15 degrees of knee flexion in the frontal plane and a medial tilt (from 45 to 0 degrees of knee extension) in the sagittal plane.
Further extension of the knee (between 15 and 0 degrees) produces a lateral glide of the patella in the frontal plane and a lateral tilt in the sagittal plane.
One proposed mechanism for abnormal patellar tracking is an imbalance in the activity or tension of the medial and lateral restraints. The cause of the imbalance tends to be hypertonus of the VL, or an excessively tight TFL or ITB. Other joints within the lower kinetic chain can also influence the tracking of the patella.

Clinical Significance of OKC and CKC Activities
Closed-Kinetic Chain Motion
During CKCEs, the flexion moment of the arm increases as the angle of knee flexion increases. In addition, the joint-reaction force increases proportionately more during knee flexion than the magnitude of the contact area. Thus, the articular pressure gradually increases as the knee flexes from 0 to 90 degrees, with maximum values occurring at 90 degrees of flexion.
However, because this increasing force is distributed over a larger patellofemoral contact area, the contact stress per unit area is minimized. Changes in the Q-angle of 10 degrees can increase patellofemoral contact pressures by 45% at 20 degrees of flexion. As the Q-angle increases, the patella tends to track more laterally. A 50% decrease in tension in the VMO can displace the patella laterally by up to 5 mm.
From 90 to 120 degrees of flexion, the articular pressure remains essentially unchanged because the quadriceps tendon is in contact with the trochlea, which effectively increases the contact area. Thus, for the patellofemoral joint, CKCEs are performed in the 0–45-degree range of flexion, with caution used when exercising between 90 and 50 degrees of knee flexion, where the PJRFs can be significantly greater.
Open-Chain Motion
In an OKC activity, the forces across the patella are their lowest at 90 degrees of flexion. As the knee extends from this position, the flexion moment arm (contact stress/unit) for the knee increases, peaking between 35 and 40 degrees of flexion, while the patella contact area decreases. This produces an increase in the PJRF at a point when the contact area is very small.
At 0 degrees of flexion (full knee extension), the quadriceps force is high, but the contact stress/unit is low. Thus OKCEs for the patellofemoral joint should be performed from 25 to 90 degrees of flexion (60–90 degrees if there are distal patellar lesions), or at 0 degree of extension (or hyperextension) from a point of view of cartilage stress.
OKCEs are not recommended for the patellofemoral joint between 0 and 45 degrees of knee flexion, especially if there are proximal patellar lesions, as the PJRFs are significantly greater.
References
- Desio SM, Burks RT, Bachus KN. Soft tissue restraints to lateral patellar translation in the human knee. Am J Sports Med. 1998 Jan-Feb;26(1):59-65. doi: 10.1177/03635465980260012701. PMID: 9474403.
- Dandy DJ: Chronic patellofemoral instability. J Bone Joint Surg Br 78:328–335, 1996.
- Fulkerson JP: Disorders of the Patellofemoral Joint. Baltimore, MD: Williams & Wilkins, 1997.
- Grelsamer RP, McConnell J: The Patella: A Team Approach. Gaithersburg, MD: Aspen, 1998.
- McConnell J: Conservative management of patellofemoral problems, The Patella. A Team Approach. Gaithersburg, MD: Aspen, 1998:119– 136.
- Voight M, Weider D: Comparative reflex response times of the vastus medialis and the vastus lateralis in normal subjects and subjects with extensor mechanism dysfunction. Am J Sports Med 10:131–137, 1991.
- Cowan SM, Bennell KL, Hodges PW, et al: Delayed onset of electromyographic activity of vastus medialis obliquus relative to vastus lateralis in subjects with patellofemoral pain syndrome. Arch Phys Med Rehab 82:183–189, 2001.
- Insall JN, Falvo KA, Wise DW: Chondromalacia patellae. A prospective study. J Bone Joint Surg 58A:1–8, 1976.
- Grana WA, Kriegshauser LA: Scientific basis of extensor mechanism disorders. Clin Sports Med 4:247–257, 1985.
- Hughston JC, Walsh WM, Puddu G: Patellar Subluxation and Dislocation, Saunders Monographs in Clinical Orthopaedics. Philadelphia, PA: W.B. Saunders, 1984.
- Brattstrom H: Shape of the intercondylar groove normally and in recurrent dislocation of the patella. Acta Orthop Scand 68:1–48, 1964.
- Aglietti P, Insall JN, Cerulli G: Patellar pain and incongruence. Clin Orthop 176:217–224, 1983.
- Horton MG, Hall TL: Quadriceps femoris muscle angle: Normal values and relationships with gender and selected skeletal measures. Phys Ther 69:897–901, 1989.
- Hsu RWW, Himeno S, CoventryMB, et al: Normal axial alignment of the lower extremity and load-bearing distribution at the knee. Clin Orthop 255:215–227, 1990.
- Woodland LH, Francis RS: Parameters and comparisons of the quadriceps angle of college aged men and women in the supine and standing positions. Am J Sports Med 20:208–211, 1992.
- Kernozek TW, Greer NL: Quadriceps angle and rearfoot motion: Relationships in walking. Arch Phys Med Rehab 74:407–410, 1993.
- Cox JS: Patellofemoral problems in runners. Clin J Sports Med 4:699–715, 1985.
- Percy EC, Strother RT: Patellalgia. Phys Sportsmed 13:43–59, 1985.
- Carson WG: Diagnosis of extensor mechanism disorders. Clin Sports Med 4:231–246, 1985.
- Olerud C, Berg P: The variation of the quadriceps angle with different positions of the foot. Clin Orthop 191:162–165, 1984.
- Huberti HH, HayesWC: Patellofemoral contact pressures. The influence of Q-angle and tendofemoral contact. J Bone and Joint Surg 66-A:715– 724, 1984.
- Greene CC, Edwards TB, Wade MR, et al: Reliability of the quadriceps angle measurement. Am J Knee Surg 14:97–103, 2001.
- Harrison MM, Cooke TDV, Fisher SB, et al: Patterns of knee arthrosis and patellar subluxation. Clin Orthop 309:56–63, 1994.
- Ehrat M, Edwards J, Hastings D, et al: Reliability of assessing patellar alignment: The A angle. J Orthop Sports Phys Ther 19:22–27, 1994.
- Rand JA: The patellofemoral joint in total knee arthroplasty. J Bone Joint Surg Am 76:612–620, 1994.
- Aglietti P, Insall JN, Walker PS, et al: A new patella prosthesis. Clin Orthop 107:175–187, 1975.
- Goodfellow JW, Hungerford DS, Woods C: Patellofemoral joint mechanics and pathology: I and II. J Bone Joint Surg 58B:287–299, 1976.
- Kaufer H: Patellar biomechanics. Clin Orthop 144:51–54, 1979.
- McConnell J, Fulkerson JP: The Knee: Patellofemoral and Soft Tissue Injuries. In: Zachazewski JE, Magee DJ, Quillen WS, eds. Athletic Injuries and Rehabilitation. Philadelphia, PA: W.B. Saunders, 1996:693–728.
- Hehne H-J: Biomechanics of the patellofemoral joint and its clinical relevance. Clin Orthop 258:73–85, 1990.
- Huberti HH, Hayes WC, Stone JL, et al: Force ratios in the quadriceps tendon and ligamentum patellae. J Orthop Res 21:49–54, 1984.
- Fujikawa K, Seedholm BB,Wright V: Biomechanics of the patellofemoral joint. Parts 1 and 2. Study of the patellofemoral compartment and movement of the patella. Eng Med 12:3–21, 1983.
- Kwak SD, Colman WW, Ateshian GA, et al: Anatomy of the human patellofemoral joint articular cartilage: surface curvature analysis. J Orthop. Res 15:468–472, 1997.
- Bishop RED, Denham RA: A note on the ratio between tensions in the quadriceps tendon and infrapatellar ligament. Eng Med 6:53–54, 1977.
- Buff HU, Jones JC, Hungerford DS: Experimental determination of forces transmitted through the patello-femoral joint. J Biomech 21:17– 23, 1988.
- Lloyd-Robert GC, ThomasTG: The etiology of quadriceps contracture in children. British J Bone Joint Surg 46-B:498–502, 1964.
- Heegaard J, Leyvraz P-F, Van Kampen A, et al: Influence of soft structures on patellar three-dimensional tracking. Clin Orthop 299:235– 243, 1994.
- van Kampen A, Huiskes R: The three-dimensional tracking pattern of the human patella. J Orthop Res 8:372–382, 1990.
- Ateshian GA, Kwak SD, Soslowsky LJ, et al: A stereophotogrammetric method for determining in situ contact areas in diarthrodial joints, and a comparison with other methods. J Biomech 27:111–124, 1994
- Carson WG, James SL, Larson RL, et al: Patellofemoral disorders— Physical and radiographic examination. Part I. Physical examination. Clin Orthop 185:178–186, 1984.
- Insall JN: Patellar pain: Current concepts review. J Bone Joint Surg 64A:147–152, 1982.
- Irrgang JJ, Rivera J: Closed kinetic chain exercises for the lower extremity: Theory and application. Sports Physical Therapy Section Home Study Course: Current Concepts in Rehabilitation of the Knee. Home Study Course. La Crosse, WI: Orthopaedic Section, APTA, Inc., 2001.
- Hungerford DS, Barry M: Biomechanics of the patellofemoral joint. Clin Orthop 144:9–15, 1979.
- Reilly DT, Martens M: Experimental analysis of the quadriceps muscle force and patello-femoral joint reaction force for various activities. Acta Orthop Scand 43:126–137, 1972.
- Grelsamer RP, McConnell J: Applied Mechanics of the Patellofemoral Joint, The Patella: A Team Approach. Gaithersburg, MD: Aspen, 1998:25–41.