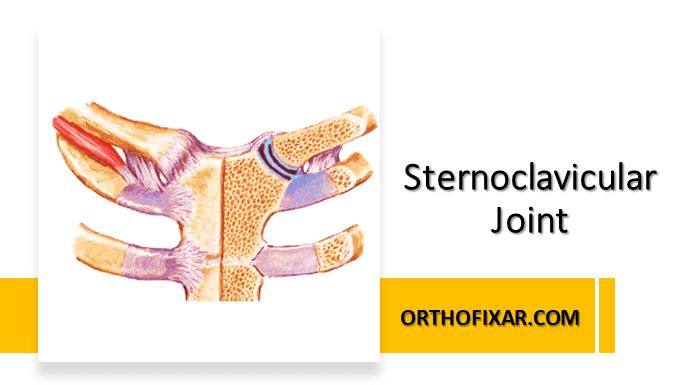
Sternoclavicular joint is a saddle-shaped synovial joint, it’s made up of the medial end of clavicle, manubrium of the sternum, and cartilage of the first rib. It is the joint that joins the appendicular skeleton to the axial skeleton. The sternoclavicular joint, along with the acromioclavicular joint, enables the humerus in the glenoid to move through a full 180° of abduction
The sternoclavicular joint (SC Joint) is a complex articulation that can have significant anatomic variations within individuals, between individuals, and throughout a population. Nevertheless, the inherent stability and biomechanics of the SC joint remain relatively unchanged.
While an acute traumatic injury can lead to an anterior or posterior SC joint dislocation, repetitive micromotion and shear can lead to Sternoclavicular arthritis changes which may produce chronic symptomatology. Clinicians should be familiar with the anatomy, biomechanics, and process of diagnostic evaluation in patients with pain or disability related to the SC joint such that an accurate diagnosis and effective treatment modality can be chosen.
Sternoclavicular Joint Osseous Anatomy
Although the clavicle is the first bone to ossify (fifth gestational week), the medial clavicular physis typically does not close until at least 25 years of age. In fact, some studies have shown that physeal closure may not actually occur until 31 years of age in some patients. Therefore, patients younger than 31 years of age who present with possible SC joint dislocations should be evaluated for both ligamentous integrity and patency of the medial clavicular physis.
The Sternoclavicular Joint type is a diarthrodial joint lined with synovium that primarily functions to connect the shoulder girdle to the axial skeleton. Because the articular surface of the medial clavicle is highly incongruent with the manubrium, joint stability is maintained primarily by strong ligamentous attachments.
Specifically, the articular surface of the medial clavicle is much larger than that of the manubrium and has been described as having a “saddle-like” configuration (i.e., concave in the axial plane and convex in the coronal plane) which biomechanically functions similarly to a ball-and-socket joint.
Both the manubrium and the medial clavicle can have a variety of different anatomic configurations which may vary across populations, between genders and, potentially, within the same patient.
Osseous asymmetry of the SC joint should be expected in the clinical setting to prevent misdiagnoses and unnecessary surgery.
See Also: Clavicle Anatomy

Chondral Surfaces
The articular surfaces of the medial clavicle and the manubrium are covered with hyaline cartilage that eventually become fibrocartilage with increasing age. Recent dissections performed at this institution revealed that only approximately two-thirds of the medial clavicle was covered with articular cartilage: the majority of this cartilage was found anteriorly and inferiorly where the medial clavicle was devoid of capsuloligamentous attachments.
A substantial disc lies between the two bony joint surfaces, and the capsule is thicker anteriorly than posteriorly. The disc separates the articular surfaces of the clavicle and sternum and adds significant strength to the joint because of its attachments, thereby preventing medial displacement of the clavicle.

Sternoclavicular Ligaments
As mentioned above, the articular surfaces of the SC joint are highly incongruent and rely primarily on the patency of static capsuloligamentous structures to maintain stability. These structures include the capsular ligaments, costoclavicular ligament, interclavicular ligament, and the intraarticular disc ligament.
Capsular Ligaments
Integrated within the SC joint capsule are discrete thickenings that represent the anterior and posterior capsular ligaments:
- The anterior capsular ligament runs from an area just superior to the articular cartilage of the medial clavicle to an area just superior to the articular cartilage of the manubrium.
- The posterior capsular ligament is essentially a thickening of the entire posterior capsule and spans between the posterosuperior aspect of the medial clavicle to the posterior aspect of the manubrium.
Several studies have shown that the posterior capsule is most important for the maintenance of horizontal stability, thus preventing anterior and posterior translation of the medial clavicle. The anterior capsular ligament most likely plays a secondary role in the maintenance of horizontal stability.
Costoclavicular Ligament
The costoclavicular ligament is a thick, robust fibrous band that inserts across the costochondral junction of the first rib and travels towards the inferior aspect of the medial clavicle to insert on the costoclavicular tubercle. The ligament is commonly described as being composed of two separate fascicles (anterior and posterior) oriented in a “twisted” configuration with an interposed bursa spanning between the first rib and the medial clavicle.
However, our recent cadaveric dissections revealed that the costoclavicular ligament may actually exist as a single ligament since we were unable to identify or separate the previously described anterior and posterior fascicles. The costoclavicular ligament may be the most important ligamentous stabilizer of the SC joint in both the vertical and the horizontal axes.
Interclavicular Ligament
The interclavicular ligament is a thick, fibrous band that lies over the superior aspect of the manubrium as it runs between the superomedial aspect of each SC joint capsule. Despite its anatomic position and thickness, the interclavicular ligament actually does not significantly contribute to vertical stability of the SC joint.
Although we were able to identify the ligament in all of our recent cadaveric dissections, its attachments to the manubrium and the SC joint capsules are quite weak and could potentially be removed during the reflection of overlying soft tissues.
Intra-Articular Disc Ligament
The intra-articular disc ligament attaches near the chondral junction of the first rib, passes through the SC joint (thus creating two separate joint spaces), and inserts along the superior margin of the articular cartilage of the medial clavicle. This ligament does not confer joint stability. Rather, it probably functions to diminish the force transmission between the manubrium and the medial clavicle which is thought to decrease the detrimental effects of bony incongruity on the health of the articular surfaces.
The morphology of the intra-articular disc has also been shown to vary considerably between individuals. Although DePalma found the intra-articular disc to be complete in 97 % of his specimens, others have found that as many was 52 % of specimens may have disc degeneration which is often clinically associated with symptomatic osteoarthritis of the SC joint.

Mediastinal Vessels
Traumatic injuries to the SC joint can result in severe complications due to the proximity of the mediastinal vessels, especially in those with posterior SC joint dislocations. These mediastinal vessels include the subclavian vessels, the right and left brachiocephalic veins, the brachiocephalic artery and the left carotid artery
In some cases, the subclavian vein may actually cross over the first rib along the posterolateral aspect of the costoclavicular ligament before merging with the brachiocephalic vein.
In the event of posterior dislocation , the sternohyoid and sternothyroid muscle bellies may become disrupted, placing the posterior vessels at an increased risk for iatrogenic injury during posterior surgical dissection of the SC joint. Disruption of the sternohyoid and sternothyroid muscle bellies can easily be identified on diagnostic axial MRI scans.

SC Joint Biomechanics
For every 10° of humeral elevation, the SC joint contributes approximately 4° of rotation. The SC joint also contributes approximately 50° of posterior rotation with every 35° of elevation, flexion and extension of the humerus.
Therefore, surgical procedures involving rigid fixation of the SC joint have largely been abandoned due to the potential for poor functional outcomes in addition to the high reported incidence of hardware failure. Large resections of the medial clavicle have also been reported; however, this can result in uncontrollable scapulothoracic motion and, therefore, may require subsequent scapulothoracic fusion.
In a biomechanical study performed to evaluate the structures involved in resisting vertical displacement of the medial clavicle, Bearn applied a downward force to the distal clavicle and determined the structures providing the most resistance to upward migration of the medial clavicle after sequential ligament sectioning. In that study, the posterosuperior capsule was found to be the primary restraint to superior migration of the medial clavicle while the interclavicular ligament, the intra-articular disc ligament, and the anterior joint capsule provided little resistance to vertical displacement.

More recently, Spencer et al. evaluated the ligamentous restraints to horizontal translation of the medial clavicle. In their study, 24 cadaveric SC joints were dissected and sub-failure horizontal loads were applied to the medial clavicle to measure anteroposterior joint translation. They found that the costoclavicular and interclavicular ligaments did not significantly contribute to the resistance of horizontal translation of the medial clavicle.
However, transection of posterior capsule resulted in an increased posterior translation of 106 % and an increased anterior translation of 41 % relative to an intact control specimen. Division of the anterior capsule resulted in an increased anterior translation of 25 %; however, this degree of anterior translation was less than that which was observed after sectioning of the posterior capsule. The results of these studies indicate that the posterior capsule is important for both vertical and horizontal stability and restoring its function should be the primary goal of ligamentous reconstruction.

References
- Koch MJ, Wells L. Proximal clavicle physeal fracture with posterior displacement: diagnosis, treatment, and prevention. Orthopedics. 2012 Jan 16;35(1):e108-11. doi: 10.3928/01477447-20111122-39. PMID: 22229601. Pubmed
- Webb PA, Schuey JM. Epiphyseal union of the anterior iliac crest and medial clavicle in a modern multiracial sample of American males and females. Am J Phys Anthropol. 1985;68(4):457–66.
- Martetschläger F, Warth RJ, Millett PJ. Instability and degenerative arthritis of the sternoclavicular joint: a current concepts review. Am J Sports Med. 2014; 42(4):999–1007.
- Hobbs DW. Sternoclavicular joint: a new axial radiographic view. Radiology. 1968;90:801.
- Lowman CL. Operative correction of old sternoclavicular dislocation. J Bone Joint Surg. 1928;10:740–1.
- Ponce BA, Kundukulam JA, Pflugner R, McGwin G, Meyer R, Carroll W, Minnich DJ, Larrison MC. Sternoclavicular joint surgery: how far does danger lurk below? J Shoulder Elbow Surg. 2013;22(7): 993–9.
- Tuscano D, Banerjee S, Terk MR. Variations in normal sternoclavicular joints; a retrospective study to quantify SCJ asymmetry. Skeletal Radiol. 2009; 38(10):997–1001.
- Wijertna MD, Turmezei TD, Tytherleigh-Strong G. Novel assessment of the sternoclavicular joint with computed tomography for planning interventional approach. Skeletal Radiol. 2013;42(4):473–8.
- DePalma AF. Surgical anatomy of the acromioclavicular and sternoclavicular joints. Surg Clin North Am. 1963;43:1541–50.
- van Tongel A, van Hoof T, Pouliart N, Debeer P, D’Herde K, De Wilde L. Arthroscopy of the sternoclavicular joint: an anatomic evaluation of structures at risk. Surg Radiol Anat. 2014;36(4):375–81.
- Lee JT, Campbell K, Michalski M, Wilson K, Spiegl U, Wijdicks C, Millett PJ. Surgical anatomy of the sternoclavicular joint: a qualitative and quantitative anatomical study. J Bone Joint Surg. 2014; 96(19):e166.
- Bearn JG. Direct observations on the function of the capsule of the sternoclavicular joint in the clavicular support. J Anat. 1967;101(Pt 1):159–70.
- Spencer EE, Kuhn JE, Huston LJ, Carpenter JE, Hughes RE. Ligamentous restraints to anterior and posterior translation of the sternoclavicular joint. J Shoulder Elbow Surg. 2002;11(1):43–7.
- Cave AJ. The nature and morphology of the costoclavicular ligament. J Anat. 1961;95:170–9.
- Tubbs RS, Shah NA, Sullivan BP, Marchase ND, Cömert A, Acar HI, Tekdemir I, Loukas M, Shoja MM. The costoclavicular ligament revisited: a functional and anatomic study. Rom J Morphol Embryol. 2009;50(3):475–9.
- Brossman J, Stäbler A, Preidler K, Trudell D, Resnick D. Sternoclavicular joint: MR imaging–anatomic correlation. Radiology. 1996;198(1):193–8.
- Emura K, Arakawa T, Terashima T, Miki A. Macroscopic and histological observations on the human sternoclavicular joint disc. Anat Sci Int. 2009; 84(3):182–8.
- Barbaix E, Lapierre M, Van Roy P, Clarijs JP. The sternoclavicular joint: variants of the discus articularis. Clin Biomech (Bristol, Avon). 2000;15 Suppl 1:S3–7.
- Renfree KJ, Wright KW. Anatomy and biomechanics of the acromioclavicular and sternoclavicular joints. Clin Sports Med. 2003;22:219–37.
- Inman VT, Saunders DM, Abbott LC. Observations on the function of the shoulder joint. J Bone Joint Surg. 1944;26:1–30.
- Rockwood CA, Williams GR, Young DC. Disorders of the acromioclavicular joint. In: Rockwood Jr CA, Mattson FA, editors. The shoulder. 2nd ed. Philadelphia: WB Saunders; 1998.
- Elhassan B, Chung ST, Ozbaydar M, Diller D, Warner JJ. Scapulothoracic fusion for clavicular insufficiency. A report of two cases. J Bone Joint Surg Am. 2008;90(4):875–80.