Patellofemoral Pain Syndrome (PFPS), commonly known as Runner’s Knee, is a common condition characterized by anterior knee pain. This condition particularly affects athletes and active individuals, with females being more than twice as likely to develop PFPS compared to males.
Patellofemoral Pain Syndrome Causes
The development of PFPS is multifactorial, involving several anatomical and biomechanical factors:
Local Factors
- Abnormal patellar tracking due to femoral geometry
- Patella alta (high-riding kneecap)
- Patella baja (low-riding kneecap)
- Shallow trochlear groove
- Increased Q-angle
See Also: Knee Q Angle Measurement
Proximal Factors
- Poor hip muscle control
- Insufficient hip adduction control
- Internal rotation issues
- Contralateral pelvic drop
Distal Factors
- Excessive foot pronation
- Tibial internal rotation
- Increased knee valgus
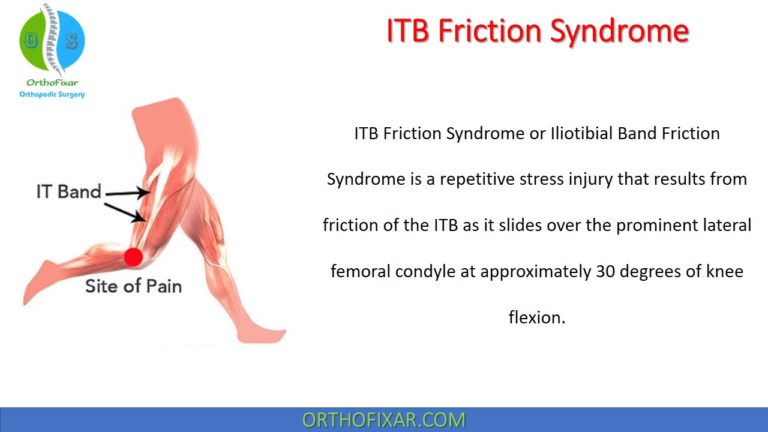
- IT band tightness
See Also: Patellofemoral Joint
For example, a tight IT band creates lateral tension on the patella, influencing its tracking. Effective intervention for PFPS is particularly important, as recent evidence suggests that PFPS at a younger age is associated with the development of patellofemoral OA later in life.
Many of the predisposing factors for patellofemoral pain syndrome are congenital:
- Increased Q-angle,
- shallow trochlear groove,
- patella alta,
- patella baja,
- increased angle of inclination.
However, injury to the patella or knee may cause a change in one of the variables:
- For example, a lateral dislocation of the patella results in tearing of the medial restraints, causing increased laxity and increased lateral migration of the patella during knee extension.
- Likewise, an injury to the knee can cause atrophy of the Vastus Medialis Oblique (VMO), increasing the amount of lateral patellar glide with subsequent shortening of the lateral restraints.
Other variables affecting the equation are increased body weight and gait mechanics. In healthy individuals, the VMO contracts simultaneously with or before vastus lateralis contraction. This contractile pattern results in normal patellar tracking.
When the knee is effused, a fluid buildup of 20 to 30 mL of excess fluid neurologically inhibits the VMO. With an effusion of 50 to 60 mL, the rest of the extensor mechanism is inhibited. When the VMO is inhibited, the relatively unopposed pull from the VL can cause excessive lateral tracking and increase compressive forces on the lateral facet. Activation of the VMO is delayed in patients demonstrating the signs and symptoms of patellofemoral pain syndrome and a group of patients who are symptom free.
See Also: Knee Effusion Tests
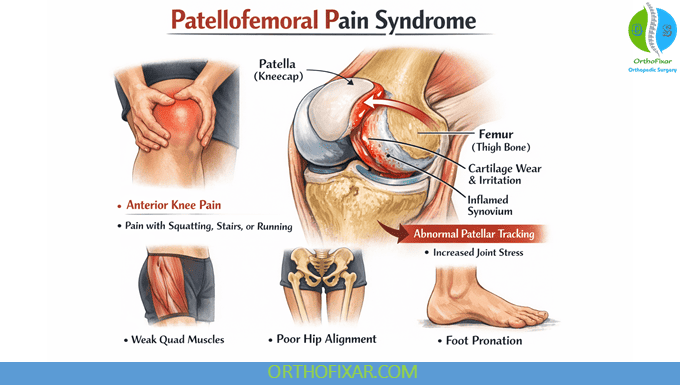
Patellofemoral Syndrome Symptoms
Patients suffering from PFPS describe a gradual onset with symptoms related to an increase or change in activity.
- Complaints of pain are usually associated with descending stairs, sitting for long periods of time, and other activities in which the knee is flexed for prolonged periods.
- Occurring more frequently in females, patients may describe “popping” and “clicking,” and palpation during active motion will reveal that this is occurring at the patellofemoral articulation.
- Mild swelling in the peripatellar region may be present.
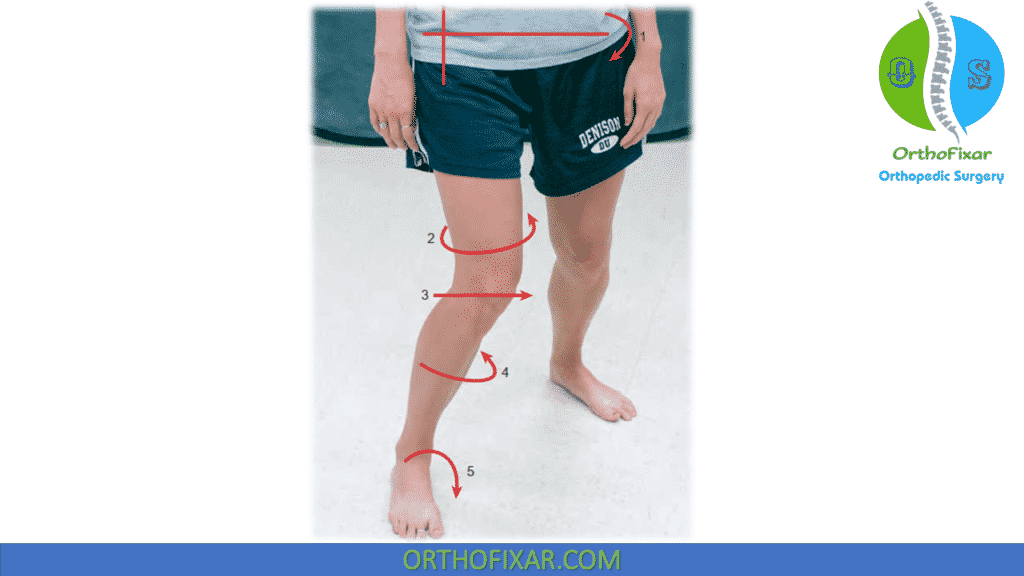
The functional examination may reveal increased and prolonged pronation and an inability to control medial rotation and adduction of the hip when accepting weight during the stance phase of gait. This aberration may become more apparent with fatigue, which associates with increased complaints of pain with a longer duration of activity.
Lower extremity internal rotation is also demonstrated when the excessive valgus occurs when stepping down, such as descending stairs. Both of these functional deviations result in increased lateral tracking of the patella.
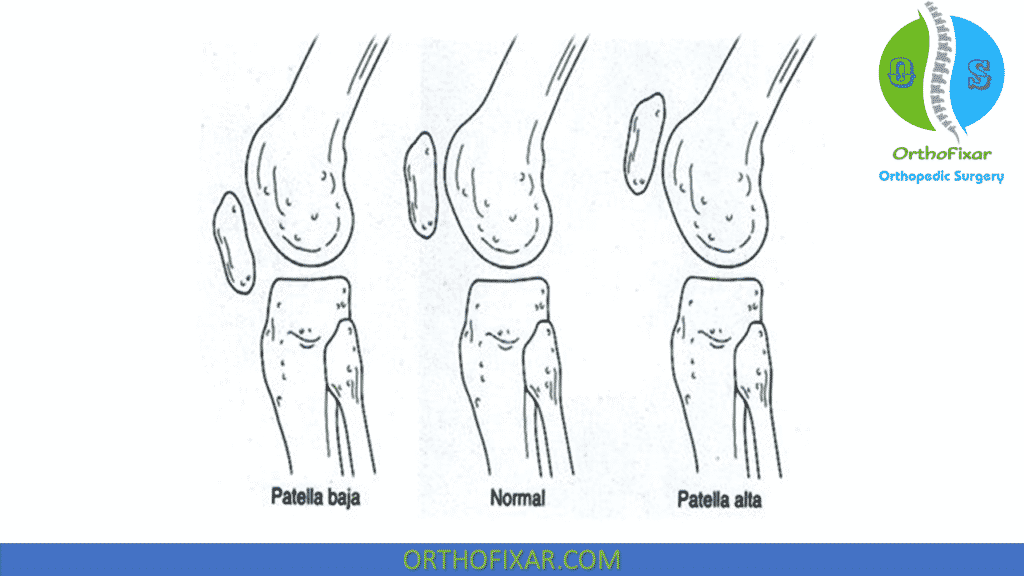
Physical examination of the joint may reveal patella baja or alta, both of which contribute to atypical joint function. Patella baja increases joint compressive forces and subsequent stiffness; patella alta leads to decreased patellofemoral joint stability as the patella has reduced contact with the stabilizing trochlea.
At rest, lateral tilt and glide of the patella may be present, signifying tight lateral restraints and/or lax medial restraints.
See Also: Patellar Glide Test
During joint play, lateral glide may be excessive, with medial glide restricted. Tightness of the lateral retinaculum may increase the tightness of the IT band and biceps femoris, also contributing to excessive lateral forces.
Examination of the ankle, foot, and hip is needed to understand fully the contributions to PFPS. An assessment of the foot and ankle in subtalar joint neutral frequently reveals a forefoot varus alignment, the cause of the increased and prolonged pronation. Reduced passive extension of the great toe in a relaxed stance also signifies a pronated foot and is predictive of patellofemoral pathology.
Strength and endurance of the hip external rotators and abductors is frequently diminished. Pain increases with active and resisted extension of the knee and during the end-range of passive flexion.
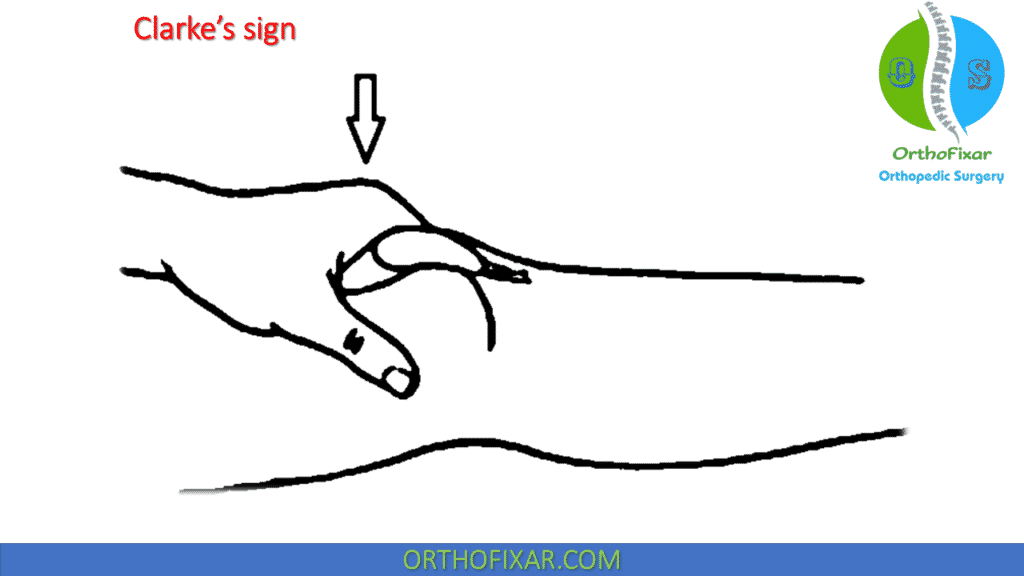
Clarke’s sign, where the patient contracts the quadriceps while the clinician applies an inferior force, produces an unreliably high rate of false-positive results, causing pain in otherwise healthy individuals, and its use is NOT recommended.
Risk Factors
Several factors can increase your risk of developing PFPS:
- Female gender
- Increased body weight
- Congenital alignment issues
- Previous knee injuries
- Weak hip muscles
- Poor biomechanics during activities
- VMO (Vastus Medialis Oblique) dysfunction
Imaging
Recommended view is Skyline view radiograph.
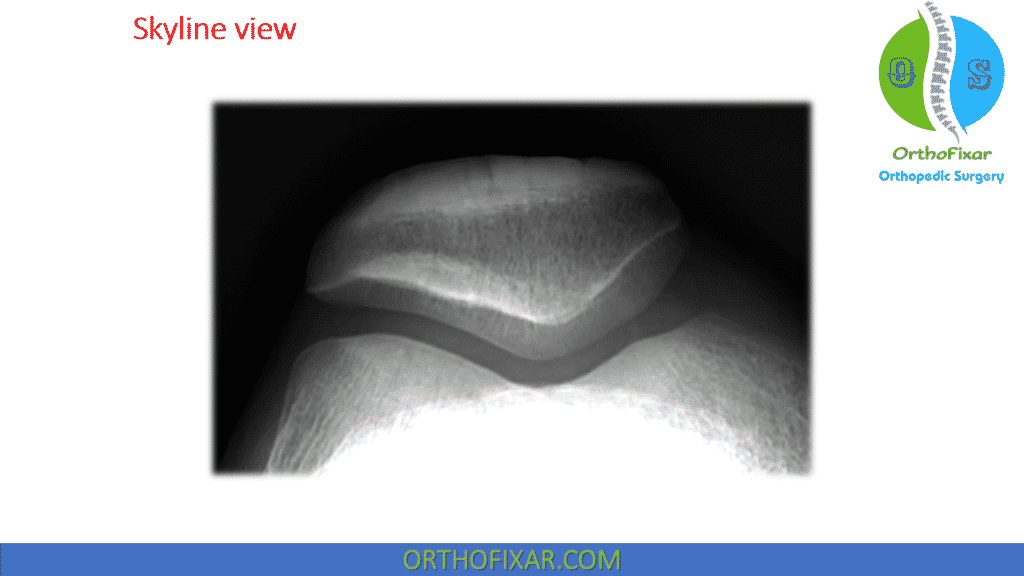
Patellofemoral Syndrome Treatment
Because of its multifactorial nature, this syndrome must be treated with an individualized approach.
PFPS Treatments include:
- Use of orthotics,
- Change of footwear,
- Alteration of gait patterns,
- Restoration of normal neuromuscular control and strength of the hip muscles,
- Stretching,
- Patellar taping,
- Anti-inflammatory medications,
- Weight loss,
- Lumbopelvic manipulation,
- Modification of activity.
Because the scope of treatment is so broad, it is necessary to delineate subgroups of patients who might benefit from specific treatments. Clinical prediction rules to identify these subgroups have been identified for taping, orthotic use, and lumbopelvic manipulation.
References
- Powers CM. The influence of altered lower-extremity kinematics on patellofemoral joint dysfunction: a theoretical perspective. J Orthop Sports Phys Ther. 2003 Nov;33(11):639-46. doi: 10.2519/jospt.2003.33.11.639. PMID: 14669959. Pubmed
- Davis, IS, and Powers, C: Patellofemoral pain syndrome: proximal, distal, and local factors: an international research retreat. J Orthop Sports Phys Ther, 40:A1, 2010. Pubmed
- Pal, S, et al: Patellar maltracking correlates with vastus medialis activation delay in patellofemoral pain patients. Am J Sports Med, 39:590, 2011.
- Cook, C, et al: Diagnostic accuracy and association to disability of clinical test findings associated with patellofemoral pain syndrome. Physiother Can, 62:17, 2010.
- Khayambashi, K, Mohammadkhani, Z, and Ghaznavi, K: The effects of isolated hip abductor and external rotator muscle strengthening on pain, health status, and hip strength in females with patellofemoral pain: a randomized controlled trial. J Orthop Sports Phys Ther, 42:22, 2012.
- Hopkins, JT: Knee joint effusion and cryotherapy alter lower chain kinetics and muscle activity. J Athl Train, 41:177, 2006.
- Sutlive, TG, et al: Identification of individuals with patellofemoral pain whose symptoms improved after a combined program of foot orthosis use and modified activity: a preliminary investigation. Phys Ther, 84:49, 2004.
- Lesher, JD, et al: Development of a clinical prediction rule for classifying patients with patellofemoral pain syndrome who respond to patellar taping. J Orthop Sports Phys Ther, 36:854, 2006.
- Noehren, B, and Davis, I: Effect of gait retraining on hip mechanics, pain and function in runners with patellofemoral pain syndrome. PFPS Retreat. Baltimore, MD, 2009.
- Iverson, CA, et al: Lumbopelvic manipulation for the treatment of patients with patellofemoral pain syndrome: development of a clinical prediction rule. J Orthop Sports Phys Ther, 38:297, 2008.
- Nijs, J, et al: Diagnostic value of five clinical tests in patellofemoral pain syndrome. Man Ther, 11:69, 2006.