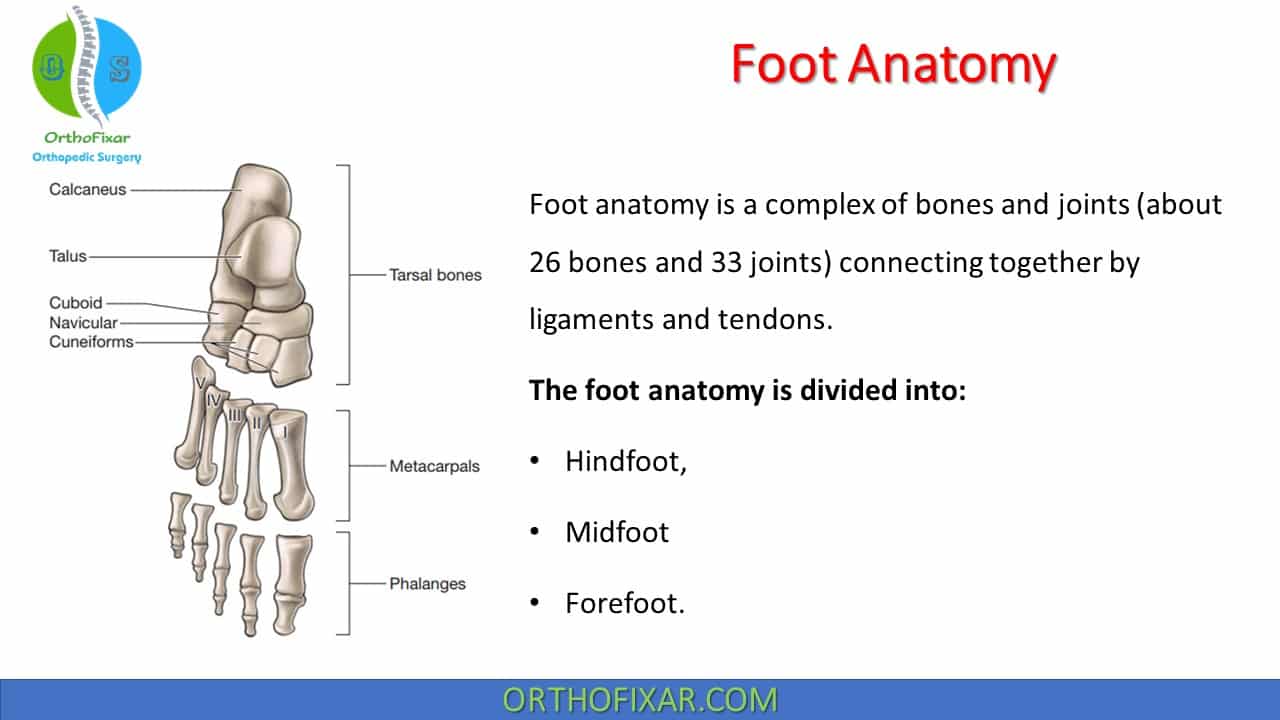
Foot anatomy is a complex of bones and joints connecting together by ligaments and tendons. Each human foot has about 26 bones and 33 joints, in addition to many muscles, tendons and ligaments.
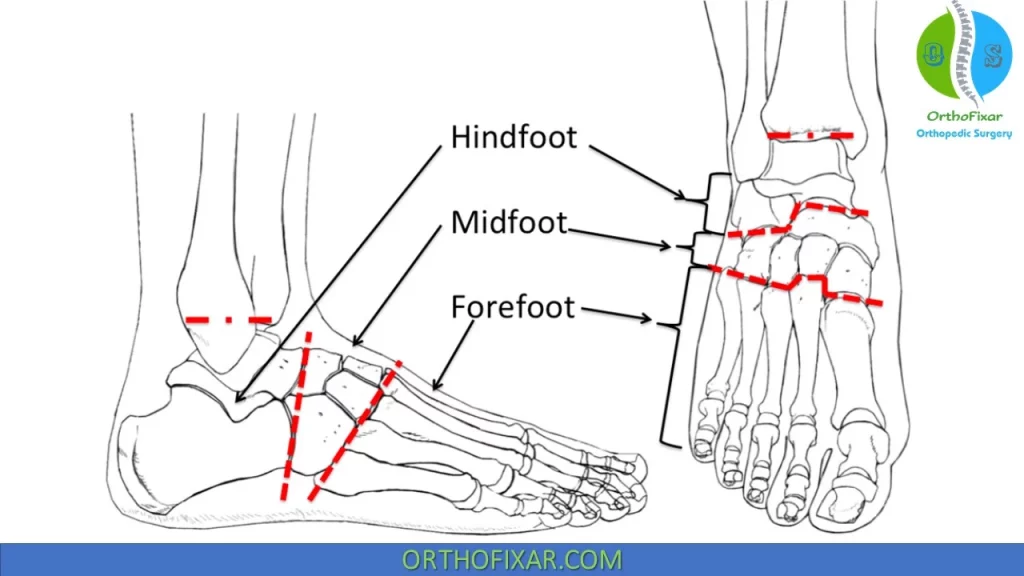
The foot anatomy is divided into 3 parts:
- Hindfoot.
- Midfoot.
- Forefoot.
See Also: Ankle Anatomy
Hindfoot Anatomy
Hindfoot Anatomy includes talus, calcaneus, and cuboid bones.
The joints of the Hindfoot are the subtalar (talocalcaneal) joint and the transverse tarsal joint (Chopart joint) that consists of talonavicular joint and calcaneocuboid joint.
The function of the hindfoot is as follows:
- to influence the function and movement of the midfoot and forefoot;
- to convert the transverse rotations of the lower extremity into sagittal, transverse, and frontal plane movements.
- Hindfoot is responsible primarily of inversion and eversion movement.
1. Subtalar Joint (TaloCalcaneal):
The subtalar joint consists of two separate, modified ovoid surfaces with their own joint cavities. The two anterior and posterior articulations are connected by an interosseous membrane.
- The anterior joint consists of a concave facet on the calcaneus and a convex facet on the talus. The anterior component is situated more medial than the posterior, giving the plane of the joint an average 42 degrees (+/- 9 degrees) superior from the transverse foot plane and 23 degrees (+/- 11 degrees) medial from the sagittal foot plane.
- The posterior joint consists of a convex facet on the calcaneus and a concave facet on the talus.
The calcaneus, the largest tarsal bone and the most frequently fractured, projects further posteriorly than the tibia and fibula. It serves as a weight-bearing bone and as a short lever for muscles of the calf, which are attached to its posterior surface. The skin and fat over the distal-inferior area of the calcaneus are specialized for friction and shock absorption.
The retrocalcaneal bursa lies anterior to the posterosuperior calcaneal tuberosity of the calcaneus. It lubricates the Achilles tendon anteriorly, as well as the superior aspect of the calcaneus.
The superior or proximal surface of the calcaneus is divisible into 3 thirds:
- The posterior third: This is a roughened surface that is concavoconvex in extension, the convexity transverse. It supports fibroadipose tissue between the calcaneal tendon and the ankle joint. Distal to the posterior articular facet is a rough depression that narrows into a groove on the medial side —the sulcus calcanei— which completes the sinus tarsi with the talus.
- The middle third: This surface carries the posterior talar facet and is oval and convex anteroposteriorly.
- The anterior third: This surface is only partly articular.
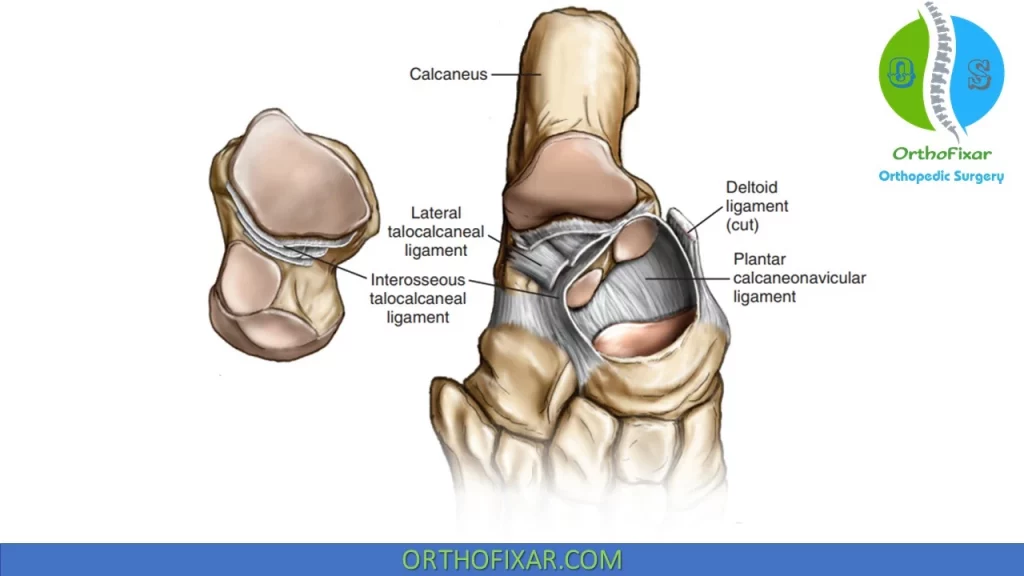
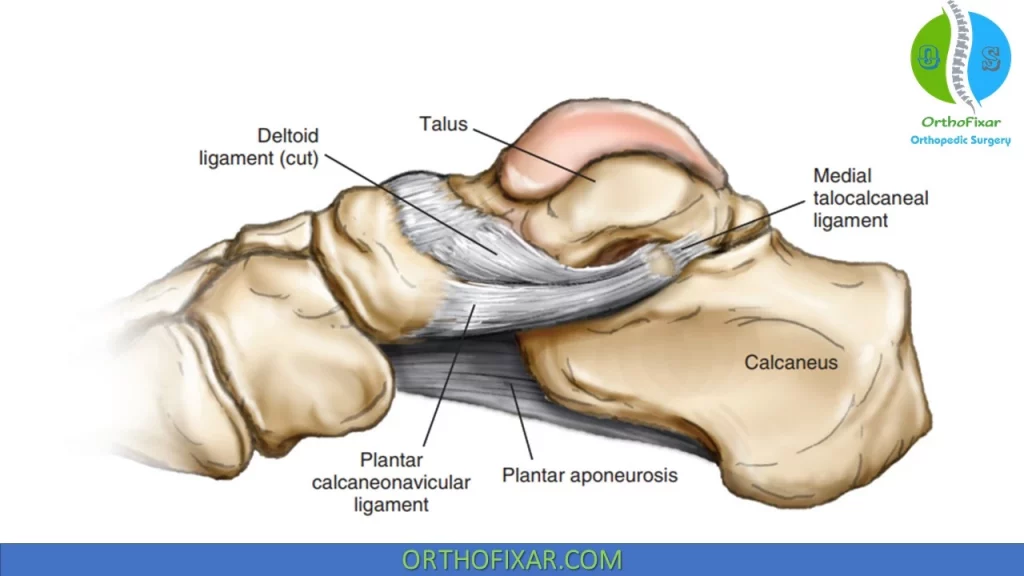
Talocalcaneal Ligaments:
In relation to the sinus tarsi, the most medial ligament is the talocalcaneal interosseous ligament, which branches superiorly into medial and lateral bands. The cervical ligament and portions of the retinaculum are located more laterally. The talocalcaneal interosseous and cervical ligaments are often collectively referred to as the interosseous ligaments.
1. Medial (Posterior) Talocalcaneal Interosseous:
The medial talocalcaneal interosseous ligament extends from the medial tubercle of the talus to the posterior aspect of the sustentaculum tali and the area of the calcaneus just posterior to the sustentaculum tali.
It functions to stabilize against anterior translation of the talus (especially at the initial contact phase of the gait cycle) by producing passive eversion of the talus.
Damage to this ligament, which typically occurs with inversion sprains and rotational compression fractures of the calcaneus, can permit excessive anterior motion of the talus. This excessive motion may result in posterior tibialis tendinitis and on occasion, Achilles tendon tendinitis.
2. Lateral (Anterior) Talocalcaneal Interosseous:
The lateral (anterior) talocalcaneal interosseous ligament (LTCIL) originates from the roof of the sinus tarsi and extends in a posteroinferior direction from the lateral process of the talus to the lateral surface of the calcaneus, just anterior to the CFL.
This ligament functions to prevent the talus and the calcaneus from separating during inversion movements. This highly innervated structure is typically injured with a dorsiflexion and inversion mechanism.
2. Talonavicular Joint:
The talonavicular joint is classified as a synovial, compound, modified ovoid joint.
The joint is actually formed by components of the talus, navicular, calcaneus, and plantar calcaneonavicular (spring) ligament.
The rounded convex anterior head of the talus fits into the concavity of the posterior navicular and the anterior component of the subtalar joint and rests on the posterior (dorsal) surface of the spring ligament.
The joint capsule is only well developed posteriorly, where it forms the anterior part of the interosseus ligament.
3. Calcaneocuboid Joint:
The calcaneocuboid joint is classified as a simple, synovial, modified sellar joint.
The anterior surface of the calcaneus, which articulates with the reciprocally shaped posterior surface of the cuboid, is relatively convex in an oblique horizontal direction and relatively concave in an oblique vertical direction.
The cuboid, most lateral in the distal tarsal row, is located between the calcaneus proximally and the fourth and fifth metatarsals distally.
To the posterior (dorsal) surface are attached posterior (dorsal) calcaneocuboid, cubonavicular, cuneocuboid, and cubometatarsal ligaments, and to the proximal edge of the plantar ridge, deep fibers of the long plantar ligament.
To the projecting proximal–medial part of the plantar surface are attached a slip of the tendon of tibialis posterior and flexor hallucis brevis (FHB).
To the rough part of the medial cuboidal surface are attached the interosseous, cuneocuboid, and cubonavicular ligaments, and proximally the medial calcaneocuboid ligament, which is the lateral limb of the bifurcated ligament.
The capsule is thickened posteriorly (dorsally) to form the posterior (dorsal) calcaneocuboid ligament.
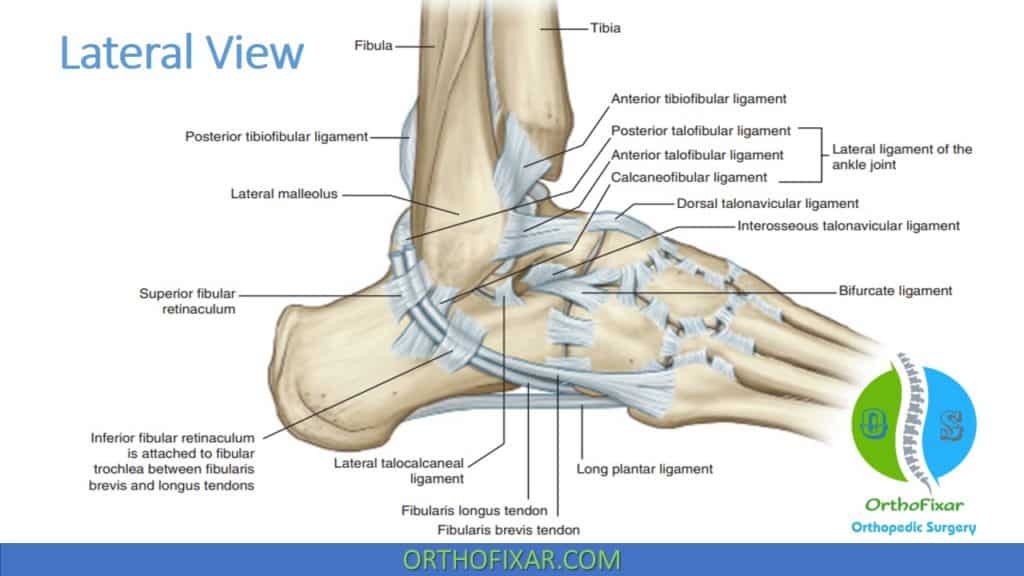
A number of ligaments help provide support to this region. The spring ligament (plantar calcaneonavicular) connects the navicular bone to the sustentaculum tali on the calcaneus.
The ligaments of the calcaneocuboid joint include the long plantar ligament and a portion of the bifurcate ligament posterior (dorsally):
- The long and strong plantar ligament attaches to the plantar surface of the calcaneus, the tuberosity on the plantar surface of the cuboid bone, and to the bases of the second, third, and fourth (and possibly fifth) metatarsals. The plantar ligament functions to provide indirect plantar support to the joint, by limiting the amount of flattening of the lateral longitudinal arch of the foot. Together with the groove in the cuboid bone, it forms a tunnel for the passage of the fibularis (peroneus) longus tendon across the plantar surface of the foot.
- The bifurcate ligament functions to support the medial and lateral aspects of the foot when weight-bearing in a plantar flexed position (twisted). The plantar calcaneocuboid ligament, sometimes referred to as the short plantar ligament, is a relatively broad and strong strap-like structure that extends from the area of the anterior tubercle of the calcaneus to the adjacent plantar surface of the cuboid bone. It provides plantar support to the joint and possibly helps to limit flattening of the lateral longitudinal arch.
Midfoot Anatomy:
The joints of the midfoot include:
- cuneonavicular joint,
- cuboideonavicular joint,
- intercuneiform joints,
- cuneocuboid joint,
Midfoot Anatomy starts at the articulation between navicular and cuneiforms, along with cuboid and fourth and fifth metatarsals. It also includes tarsometatarsal (TMT) joints.
The distal tarsal row contains, medial to lateral, the medial, intermediate, and lateral cuneiforms and the cuboid, which is roughly in parallel with the proximal row and which forms a transverse arch, posteriorly (dorsally) convex.
Medially, the navicular is positioned between the talus and the cuneiforms.
Laterally, the cuboid is positioned between the calcaneus and the lateral cuneiform and the fourth and fifth metatarsals.
A subluxation of the cuboid bone is called Cuboid Syndrome.
Midfoot functions as a transverse roman arch in the axial plane:
- Dorsal surface of the arch is wider than the plantar surface
- The second metatarsal base acts as a keystone to this arch.
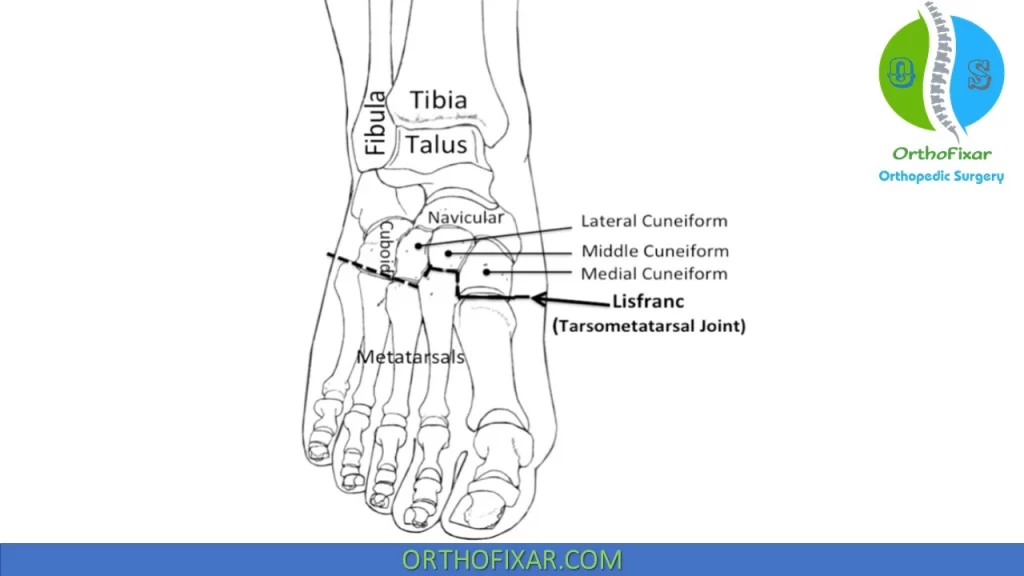
Lisfranc joint: (Tarsometatarsal joint) consists of 1st, 2nd and 3rd metatarsocuneiform joints and 4th and 5th metatarsocuboid joints. It connects the midfoot and the forefoot.
Ligamentous stability to midfoot is provided by longitudinal and transverse ligaments on plantar and dorsal aspects of each joint:
- Plantar ligaments are thicker and stronger than the dorsal ligaments.
- The Primary stabilizer of longitudinal arch is the interosseous ligaments while the plantar fascia is a secondary stabilizer.
The Largest and strongest ligaments is the Lisfranc ligament, traveling from medial cuneiform to base of second metatarsal.
The Midfoot Anatomy can also be divided into three columns:
- Medial column: Includes the first metatarsal, the medial cuneiform, and the navicular.
- Middle column: Includes the second and third metatarsals, the middle cuneiform, and the lateral cuneiform.
- Lateral column: Includes the fourth and fifth metatarsals and the cuboid.
Lateral column has the most sagittal mobility while the middle column has the least.
1. Cuneonavicular joint:
The cuneonavicular joint is classified as a compound, synovial, modified ovoid joint.
The navicular presents a convex surface to the concave surface of the combined cuneiforms.
The wedge-like cuneiform bones articulate with the navicular proximally and with the bases of the first to third metatarsals distally.
The medial cuneiform is the largest and the intermediate, the smallest. In the intermediate and lateral cuneiforms, the posterior (dorsal) surface is the base of the wedge, but in the medial, the wedge is reversed, a prime factor in shaping the transverse arch. The wedge shape of these bones also provides a cavity for the neurovascular and musculotendinous structures of the foot.
The cuneiforms, together with articulations with the metatarsal bones, form Lisfranc’s joint.
The ligament of Lisfranc runs between the medial cuneiform and second metatarsal base. Disruption of this ligament can lead to a dislocation of the medial aspect of the foot, as the first metatarsal and medial cuneiform separate from the second metatarsal and intermediate cuneiform.
The joint cavity and capsule of the cuneonavicular joint is continuous with that of the intercuneiform and cuneocuboid joints, and the synovium is continuous with that of these joints, the second and third cuneometatarsal joints, and the intermetatarsal joints of each base except the fifth.
2. Intercuneiform and Cuneocuboid joints:
These joints are classified as compound, synovial, modified ovoid joints. The joint capsule and synovium is contiguous between all of these joints and with that of the cuneonavicular joint.
Dysfunctions in the cuneocuboid joint result from a collapse of the plantar supporting structures or from direct trauma.
Such dysfunctions may result in the cuboid subluxing in a plantar direction (medial border of cuboid moves inferiorly).
At the intercuneiform joints, the third cuneiform may sublux on the second cuneiform.
3. Cubonavicular Joint:
The cubonavicular joint is classified as a syndesmosis or a plane surfaced joint. If the joint is synovial, the capsule and synovium is continuous with the cuneonavicular joint.
Forefoot Anatomy:
Forefoot Anatomy includes all structures distal to the Tarso-metatarsal joints (TMT) that include:
- Metatarsals bones.
- Phalanges bones.
The joints of the forefoot include:
- the tarsometatarsal joints,
- the intermetatarsal joints,
- the MTP joints,
- the interphalangeal (IP) joints.
Ligaments and tendons of the forefoot include:
- Transverse metatarsal ligament.
- Conjoined tendon of the adductor hallucis muscles.
- Plantar plate.
See Also: Adductor Hallucis Muscle Anatomy & Function
The function of the forefoot is to adapt to the terrain, adjusting to uneven surfaces.
The first metatarsal is the shortest and the strongest, whereas the second is the longest and the least mobile, serving as the anatomic touchstone for abduction and adduction of the foot.
The phalanges of the foot, although similar in number and distribution to those in the hand, are shorter and broader than their counterparts.
1. Cubometatarsal Joint:
Laterally, the cuboid bone articulates with the fourth and fifth metatarsals distally, and with the calcaneus proximally. When considered alone, the cubometatarsal joint is classified as a compound, modified ovoid, synovial joint. When the cubometatarsal joints are considered together, they form a modified sellar joint.
The joint capsule and synovium of the fourth and fifth cubometatarsal joints are separated from the other tarsometatarsal joints by an interosseous ligament.
2. Intermetatarsal Joint:
The first intermetatarsal joint is classified as a simple, synovial, modified ovoid joint, whereas the second, third, and fourth are classified as compound joints.
If the joint is synovial, the capsule and synovium is continuous with the cuneonavicular joint.
Motion at these joints is confined to posterior (dorsal)/anterior (plantar) gliding, producing a fanning and folding motion of the foot.
Proximally, the five metatarsals articulate with the tarsals and with themselves through broad concavities.
3. Metatarsophalangeal Joints:
The MTP joints are classified as simple, synovial, modified ovoid joints.
The capsule and synovium in each of these joints is confined to its own joint and posteriorly (dorsally) is thin, whereas plantarly (anteriorly), it is blended with the plantar and collateral ligaments.
The concave bases of the proximal phalanges articulate with the convex heads of the metatarsals.
The first MTP joint, with its more extensive articular surface on the anterior (plantar) aspect of the metatarsal than on the posterior (dorsal), allows for a greater freedom of motion, and its anterior (plantar) surface forms two grooves for articulation with the hallucal sesamoids.
The fifth metatarsal has a lateral styloid process at its base, which serves as the insertion site for the tendon of the fibularis (peroneus) brevis. The styloid area is often avulsed during acute inversion injuries of the foot.
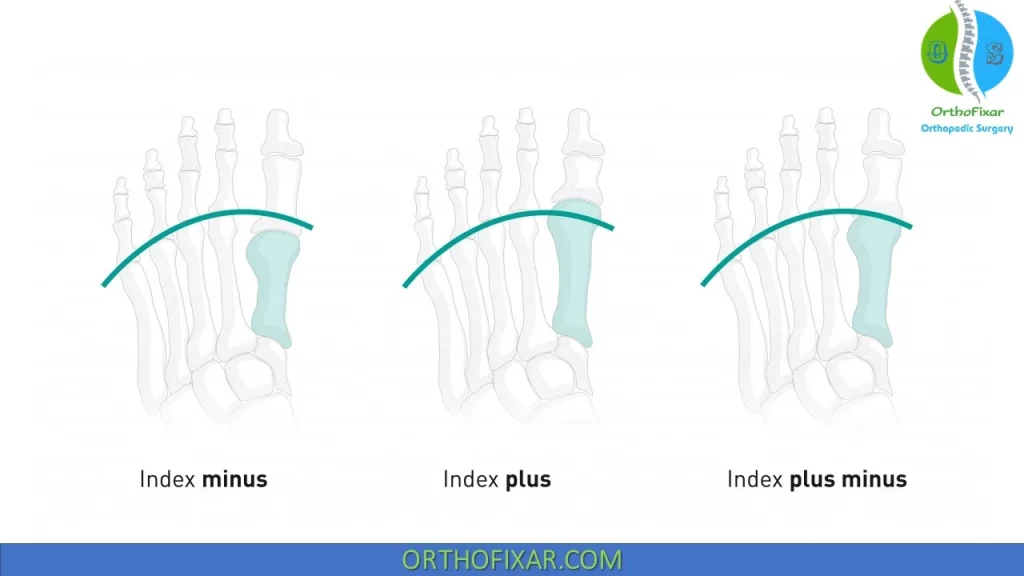
Three types of forefoot are recognized based on the length of the metatarsal bones, although it is unclear whether these various types affect foot function in any way:
- Index plus: This type is characterized by the first metatarsal being longer than the second, with the other three of
progressively decreasing lengths, so that 1 > 2 > 3 > 4 > 5. - Index plus–minus: In this type, the first metatarsal is of the same length as the second, with the others progressively diminishing in length, so that 1 ¼ 2 > 3 > 4 > 5.
- Index minus: With this type, the second metatarsal is longer than the first and third metatarsals. The fourth and fifth metatarsals are progressively shorter than the third, so that 1 < 2 > 3 > 4 > 5.
Stability of the MTP joints is primarily provided by a musculocapsular ligamentous complex anteriorly (plantarly), and medially and laterally by the medial and lateral collateral ligaments, respectively.
First MTP Joint:
The first MTP joint is the articulation between the head of the first metatarsal and the proximal phalanx. Although there is some anatomic variation from patient to patient, the first MTP joint is typically a cam-shaped, condylar-hinged joint.
The MCP joint has little inherent stability because the proximal phalanx has a fairly shallow cavity in which the metatarsal head articulates.
The joint is stabilized posteriorly (dorsally) by the capsule and expansion of the extensor hallucis tendon. Fan-shaped medial and lateral collateral ligaments provide valgus and varus stability, respectively.
The plantar surface of the capsule is reinforced by a fibrocartilaginous plate, called the plantar accessory ligament. In addition, the MTP joints are dynamically stabilized by the short flexor complex (FHB and the two sesamoids embedded in the FHB tendons), the adductor hallucis, and the abductor hallucis tendons.
The sesamoids are connected distally to the base of the proximal phalanx by extensions of the FHB called the plantar plate. Typically, the sesamoids are anterior (plantar) to the medial and lateral condyles of the metatarsal pad. The sesamoids are separated on the anterior (plantar) aspect of the first metatarsal head by a cresta, which helps to stabilize the sesamoids, and are connected to one another by the intersesamoidal ligament.
The abductor hallucis inserts into the medial sesamoid, and the adductor hallucis inserts into the lateral sesamoid.
The FHL pierces the two heads of the FHB muscle to run just anterior (plantar) to the intersesamoidal ligament. In normal gait, the capsuloligamentous complex of the first MTP joint must withstand 40–60% of body weight, but in athletic activity, this can reach as much as eight times body weight.

4. Interphalangeal Joints:
The hallux has two phalanges, whereas each of the remaining toes have three. The IP joints are classified as simple, synovial, modified sellar joints. The saddle-shaped articular fossa of the head of the proximal phalanx articulates with the base of the intermediate phalanx. This in turn receives the smaller and flatter distal phalanx.
Plantar Fascia (Plantar Aponeurosis)
The plantar fascia is the investing fascial layer of the anterior (plantar) aspect of the foot that originates from the os calcis and inserts through a complex network to the anterior (plantar) forefoot. It is a tough, fibrous layer, composed histologically of both collagen and elastic fibers.
The plantar fascia is often regarded as being analogous to the palmar fascia of the hand. However, unlike the fascial layer of the palm, which is generally thin, the plantar fascia is a thick structure, and not only serves a supportive and protective role, but is also intricately involved with the weight-bearing function of the foot.
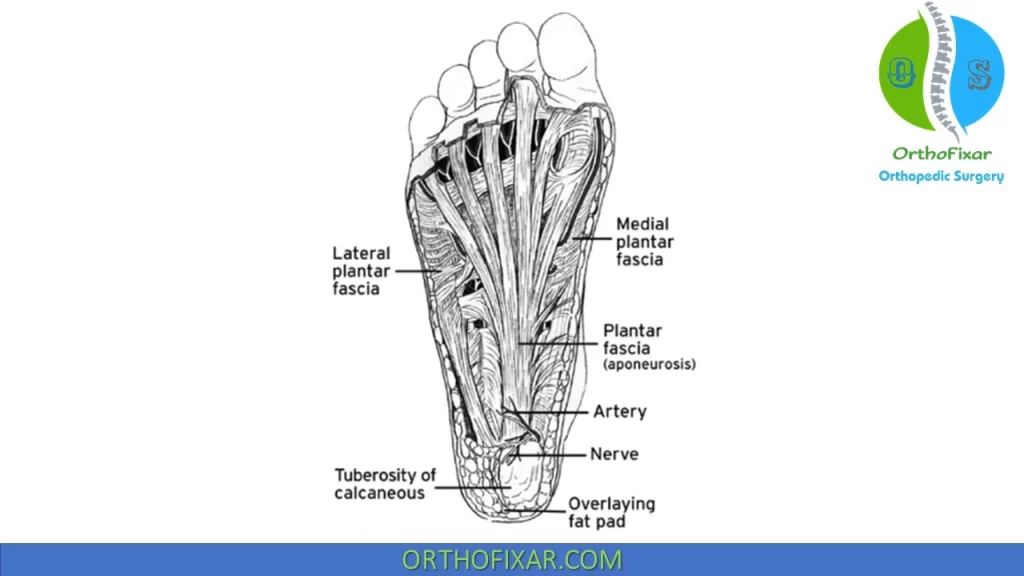
The plantar fascia is divided into three major areas:
- Central portion: The central portion is the major portion of the plantar fascia both anatomically and functionally. This portion is the thickest and the strongest and is narrowest proximally where it attaches to the medial process of the calcaneal tuberosity, proximal to the flexor digitorum brevis (FDB). This attachment site is often involved in a condition called plantar heel pain; however, pain can occur anywhere along the structure. From its insertion, the central portion of the fascia fans out and becomes thinner distally. Its fibers are longitudinally oriented and adhere to the underlying FDB muscle. The central portion of the fascia primarily functions as a dynamic stabilizer of the medial longitudinal arch during weight-bearing activities.
- Lateral and medial portions: The smaller and thinner lateral and medial portions are thin and cover the under surface of the abductor digiti minimi and abductor hallucis muscles, respectively.
With standing and weight-bearing, the plantar fascia plays a major role in the support of the weight of the body, by virtue of its attachments across the longitudinal arch.
During the different phases of gait, the plantar fascia assumes different biomechanical functions. For example:
- During the toe-off portion of the gait cycle, the windlass effect on the plantar fascia helps to reconstitute the arch and generates a more rigid foot for propulsion.
- During heel strike, and during the first half of the stance phase of the gait cycle with the toes in neutral, the plantar fascia relaxes, flattening the arch. This allows the foot to accommodate to irregularities in the walking surface and to absorb shock.
- As the foot proceeds from midstance to terminal stance, the toes dorsiflex and, through its attachments to the toes via the plantar plate, the plantar fascia tightens. The plantar fascia is pulled over the metatarsal heads, causing the metatarsal heads to be depressed and the longitudinal arch to rise.
- During the swing phase of gait, the plantar fascia is under little tension and appears to serve no important functional role.
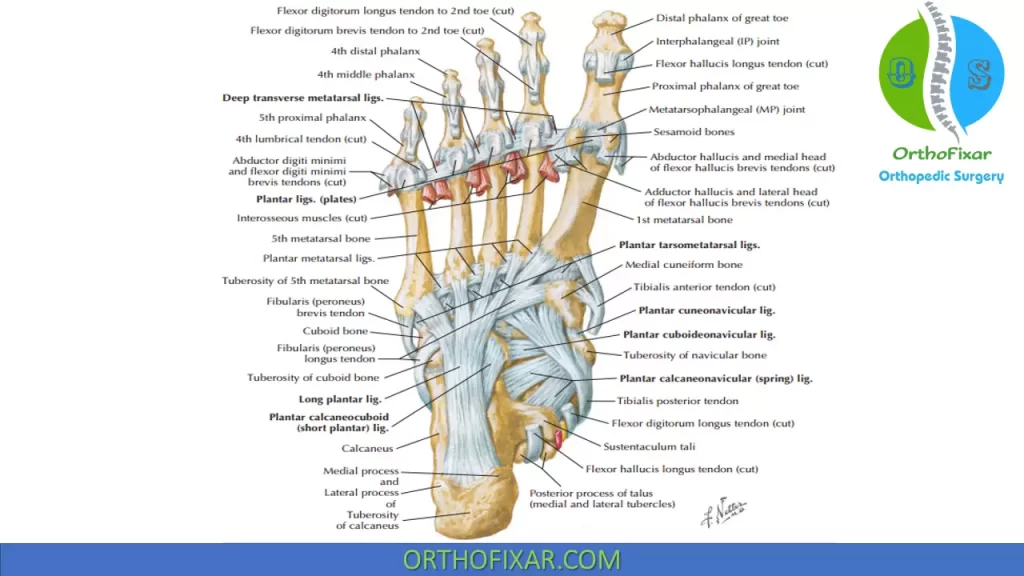
Plantar Foot Ligaments
| Ligaments | Attachments | Function |
|---|---|---|
| Long plantar | Plantar of calcaneus to cuboid | Maintains arches of foot |
| Plantar calcaneocuboid (short plantar) | Anteroinferior aspect of calcaneus to inferior aspect of cuboid | Maintains arches of foot |
| Plantar calcaneonavicular (spring) | Sustentaculum tali to posteroinferior aspect of talus | Maintains longitudinal arch of foot |
| Plantar cubonavicular | Inferior navicular to inferomedial cuboid | Limits separation of cuboid from navicular and supports arch |
| Plantar tarsometatarsal | Connects metatarsals 1 to 5 to corresponding tarsal on plantar aspect | Limits separation of metatarsals from corresponding tarsal bones |
| Collateral | Distal aspect of proximal phalanx to proximal aspect of distal phalanx | Reinforces capsule of IP joints |
| Plantar plate | Thickening of plantar aspect of joint capsule | Reinforces plantar aspect of IP joint |
| Deep transverse metatarsal | MTP joints on plantar aspect | Limits separation of MTP joints |
Motions of the Foot and Ankle
| Plane of Motion | Motion |
|---|---|
| Sagittal (X-axis) | – Dorsiflexion – Plantar flexion |
| Frontal (coronal) (Z-axis) | – Inversion – Eversion |
| Transverse (Y-axis) Forefoot/midfoot | – Adduction – Abduction – Ankle/hindfoot – Internal rotation – External rotation |
| Triplanar motion Supination | – Adduction – Inversion – Plantar flexion – Pronation – Abduction – Eversion – Dorsiflexion |
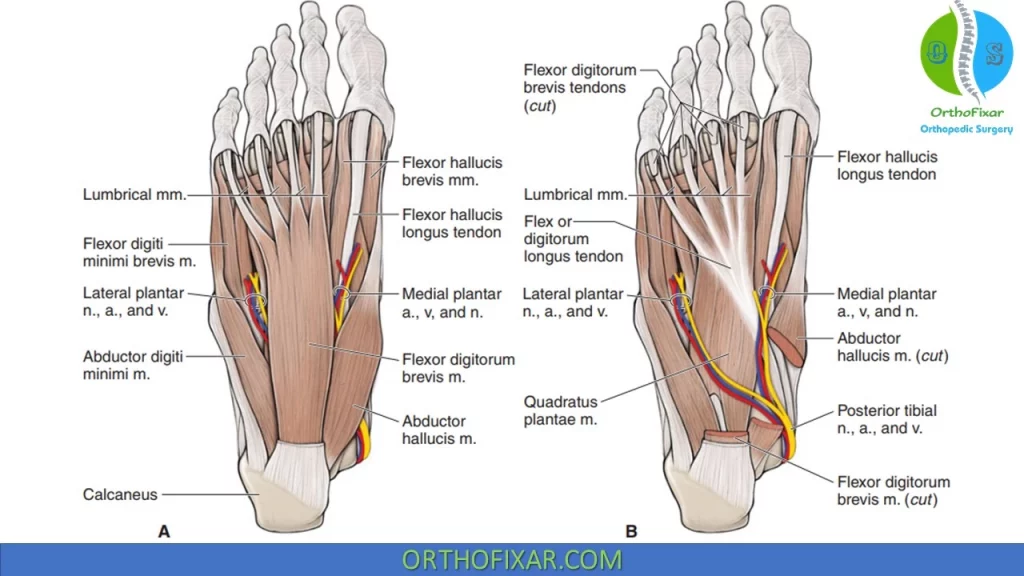
Muscles of the Plantar Foot
| Layer | Muscles | Tendons | Neurovascular |
|---|---|---|---|
| Dorsal Layer | Extensor digitorum brevis | ||
| First Plantar Layer | 1. Abductor hallucis. 2. Flexor digitorum brevis (FDB). 3. Abductor digiti minimi. | ||
| Second Plantar Layer | 1. Quadratus plantae. 2. Lumbrical muscles. | 1. Flexor digitorum longus (FDL). 2. Flexor hallucis longus (FHL). | Medial and lateral plantar arteries |
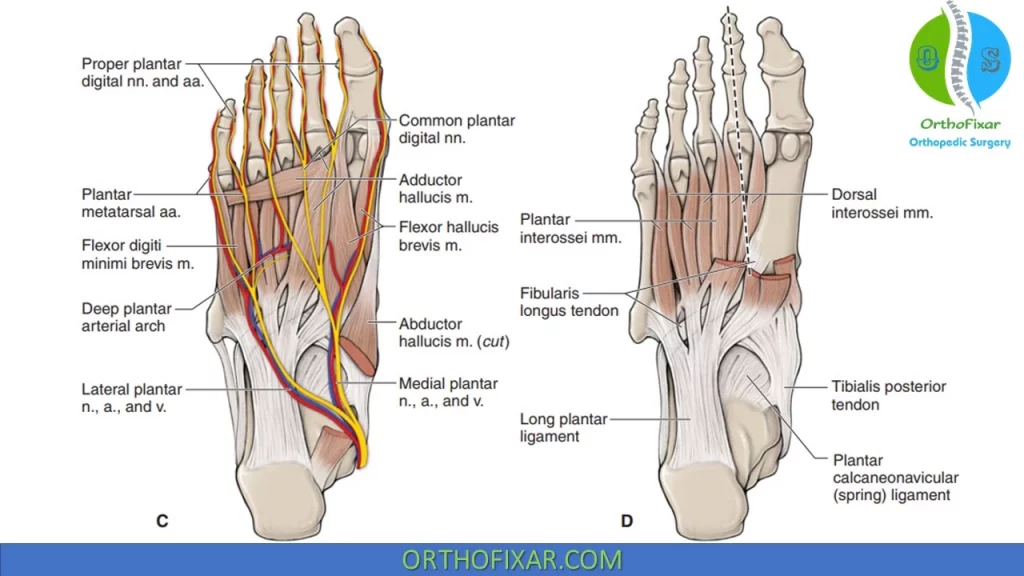
| Third Plantar Layer | 1. Flexor hallucis brevis. 2. Oblique and transverse heads of the adductor hallucis. 3. Flexor digiti minimi brevis. | ||
| Fourth Plantar Layer | 1. Dorsal interosseous.. 2. Plantar interosseus | 1. Peroneus longus 2.Tibialis posterior |
Blood Supply to the Foot
Blood supply to the foot comes from three primary arteries:
| Artery | Branches at ankle | Branches in foot |
|---|---|---|
| Peroneal (fibular) artery | – Posterior lateral malleolar artery. – Communicating branch. | – Lateral calcaneal branch |
| Posterior tibial artery | – Posterior medial malleolar artery. – Communicating branch. – Artery of tarsal canal : dominant blood supply to the talar body | – Lateral plantar arteries – Medial plantar arteries |
| Anterior tibial artery | – Anterior medial malleolar artery -Anterior lateral malleolar artery | – Dorsalis pedis artery |
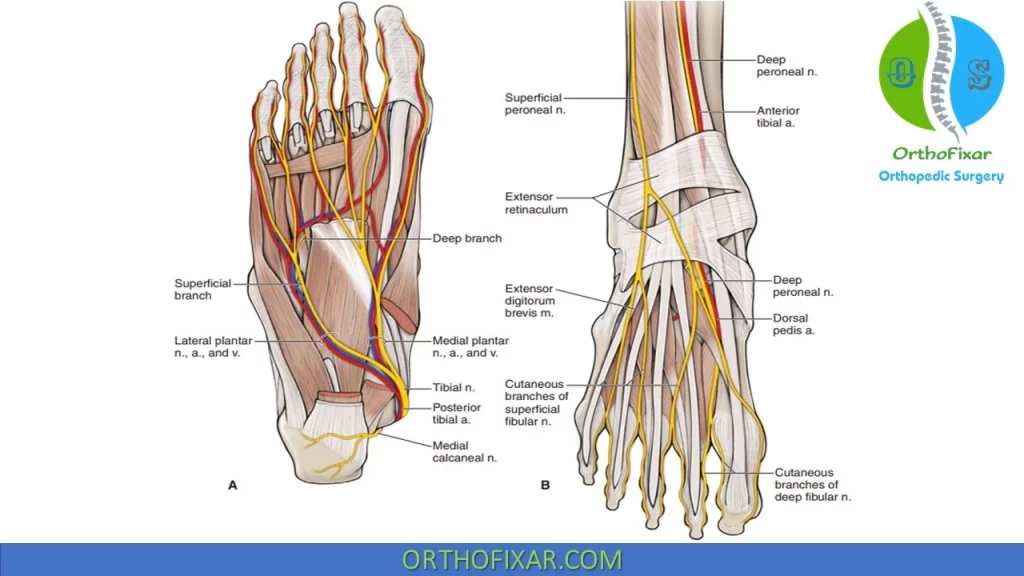
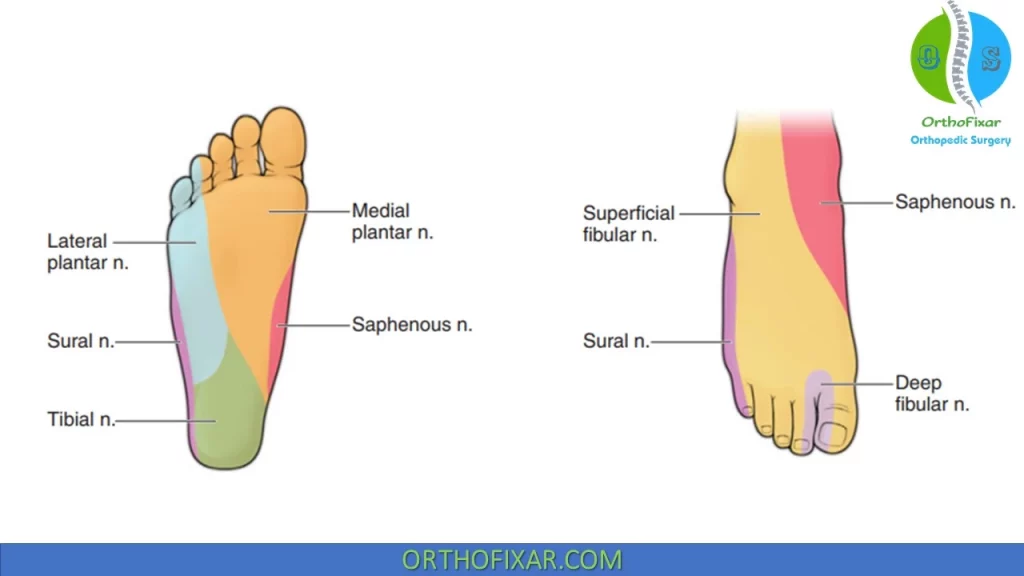
Nerves of the Foot
Branches of the Tibial nerve:
- Medial calcaneal nerve: Innervates plantar medial heel.
- Medial plantar nerve: Innervates Abductor Hallucis, FHB, FDB and lumbircals to 2nd and 3rd toes.
- Lateral plantar nerve: Innervates adductor hallucis, quadratus plantae, all interossei muscles, lateral two lumbricals and abductor digiti minimus. it also provides sensation to plantar lateral foot, lateral fourth toe and fifth toe.
Baxter’s nerve: it’s the first branch of Lateral plantar nerve, courses anterior to the medial tuberosity between the Quadratus plantae and Flexor digitorum brevis.
It gives innervate to the abductor digiti minimus muscle.
- Sural Nerve: Provides dorsal sensory in 4th web space.
- Deep peroneal Nerve: Innervates EDB, and EHB in foot, and provides sensation to the first dorsal webspace.
- Superficial Peroneal Nerve: Medial branch and Lateral cutaneous branch.
- Saphenous Nerve: Supplies sensation to the medial side of foot.
References
- Subotnick SI: Normal anatomy. In: Subotnick SI, ed. Sports Medicine of the Lower Extremity, 2nd ed. Philadelphia, PA: Churchill Livingstone, 1999:75–111
- Pick TP, Howden R: Gray’s Anatomy, 15th ed. New York, NY: Barnes & Noble, 1995.
- Jahss MH: Disorders of the Foot. Philadelphia, PA: WB Saunders, 1982
- Hedrick MR. The plantar aponeurosis. Foot Ankle Int. 1996 Oct;17(10):646-9. doi: 10.1177/107110079601701012. PMID: 8908494.
- Barrett SJ, O’Malley R. Plantar fasciitis and other causes of heel pain. Am Fam Physician. 1999 Apr 15;59(8):2200-6. PMID: 10221305.
- Dutton’s Orthopaedic Examination, Evaluation, And Intervention 3rd Edition.
- Campbel’s Operative Orthopaedics 12th edition Book.
- Millers Review of Orthopaedics -7th Edition Book.