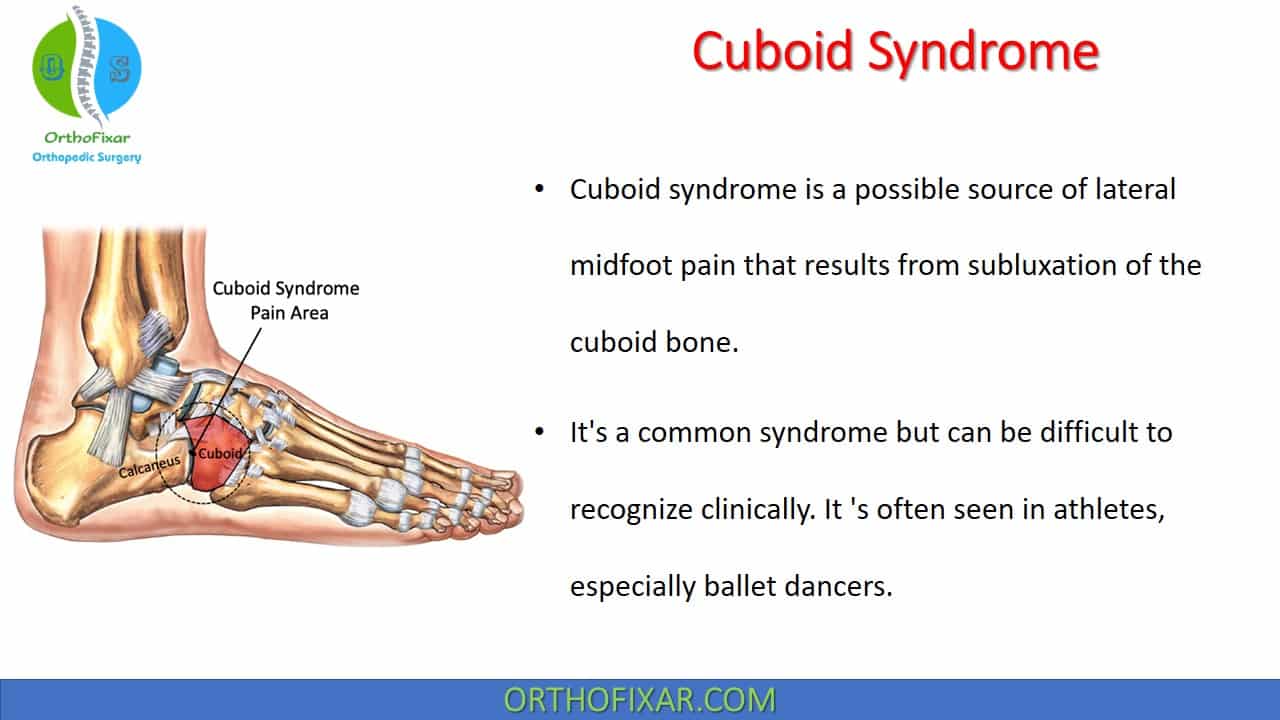
Cuboid syndrome is a possible source of lateral midfoot pain that results from subluxation of the cuboid bone. It’s a common syndrome but can be difficult to recognize clinically. It’s often seen in athletes, especially ballet dancers.
Other names of Cuboid syndrome are:
- Locked cuboid,
- Calcaneal cuboid fault syndrome,
- Cuboid Subluxation.
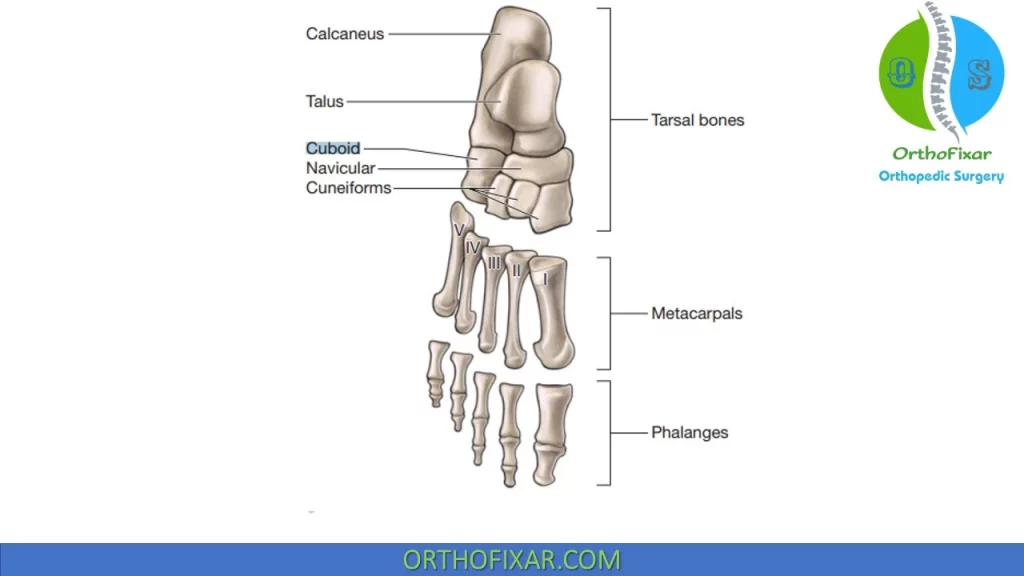
Cuboid Bone Anatomy
Cuboid Bone is the most lateral bone of the tarsus, it’s articulation include:
- Calcaneus bone posteriorly,
- 4th and 5th metatarsals bone anteriorly,
- Lateral cuneiform and talus bone medially.
See Also: Foot anatomy
The calcaneal–cuboid (CC) articulation, the primary joint of interest with cuboid syndrome, has relatively flat lateral joint surfaces, whereas the medial surfaces are somewhat irregular. Maximal congruence of the calcaneus and cuboid articulating surfaces (i.e., the “close-packed” position) is thought to occur during pronation of the forefoot relative to the hind foot. This close packing, which enhances longitudinal arch stability, may be less effective when the CC joint surfaces are more planar.
The fibularis longus tendon uses the cuboid as a pulley, and contraction of the fibularis longus exerts an eversion torque on the cuboid. Eversion of the cuboid approximates the CC joint surfaces and tensions the plantar ligaments, increasing CC rigidity.
The mechanics of the CC joint are highly variable among individuals and thus not fully understood. The planar geometry of the CC joint surfaces allows some abduction/ adduction (frontal plane) and dorsiflexion/plantarflexion (sagittal plane) gliding. The principle movement at the CC joint, however, appears to be rotation with the calcaneal process acting as a pivot.
Calcaneal–cuboid joint function is often considered within the context of composite midtarsal joint mechanics because the navicular and cuboid bones move essentially in tandem during gait. The midtarsal joints (talonavicular (TN) and CC) are thought to play a vital role in the transition of the foot from a mobile adapter during weight acceptance to a rigid lever during push-off and in rearfoot-to-forefoot load transfer during propulsion. To date, the precise manner in which the midtarsal joints influence rearfoot to forefoot load transfer or forefoot flexibility has not been clearly elucidated.
More about Mechanism of gait can be seen in Gait Cycle .

Cuboid Syndrome Causes
Although the precise etiologic mechanism is unclear, cuboid syndrome is thought to result from a sustained disruption or subluxation of calcaneal–cuboid (CC) joint congruity.
Some authors have theorized that CC joint congruity is disrupted when the cuboid is forcefully everted on an inverted calcaneus. The disruption or subluxation, which may be imperceptible by examination, is believed to alter normal midtarsal joint mechanics and induce lateral foot pain.
Factors reported to contribute to or coincide with cuboid syndrome include:
- Midtarsal instability;
- Excessive body weight;
- Excessive foot pronation;
- Ill-fitting or poorly constructed orthoses or shoes;
- Significant increases in exercise intensity, duration, or frequency;
- Inadequate exercise recovery;
- Training on uneven surfaces;
- Sprain of the foot or ankle.
Morphology of the CC joint may be a contributing factor to cuboid syndrome. A flat calcaneal process (of the cuboid) may result in less effective close packing and destabilization of the CC joint during push-off.
Impaired fibularis longus performance may also hinder CC joint close packing.
Folds in the synovial lining between the CC and cubometatarsal joints may be another source of lateral midfoot dysfunction and pain. These synovial folds have the potential to restrict joint motion or become impinged. The audible “pop” that occurs after cuboid manipulation may be the result of mechanical deformation of an obstructive fold.
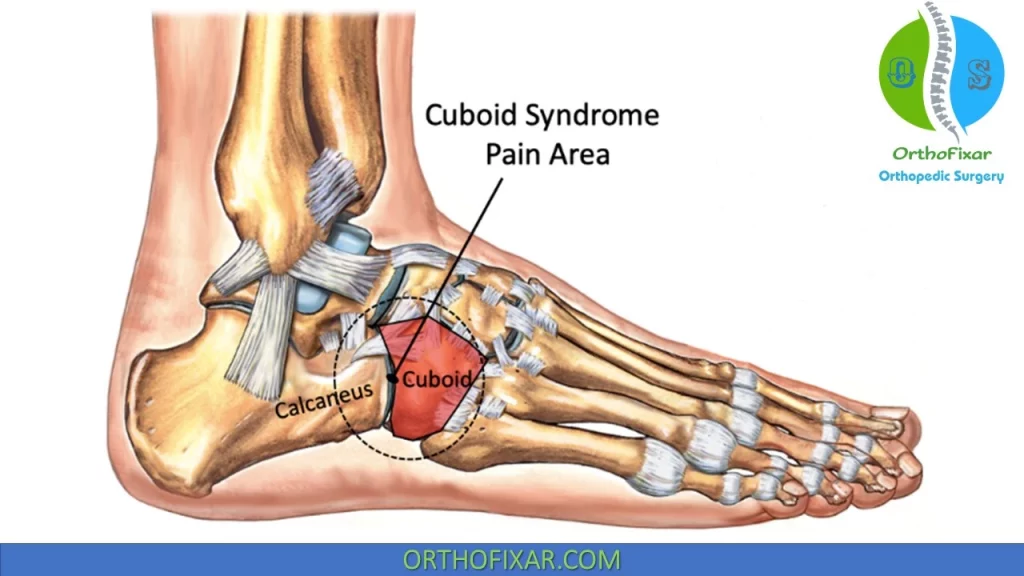
Cuboid Syndrome Symptoms & Signs
Cuboid syndrome usually presents with a gradual onset of lateral midfoot pain: The pain is usually localized near the fourth and fifth metatarsals at the posterior (dorsal) aspect of the cuboid or the calcaneocuboid joint. Often, the patient feels as if he or she is walking with a small stone in their shoe.
Maximum discomfort is elicited by pressure directed over the fibular (peroneal) groove on the plantar surface of the calcaneus.
On occasion, the hook of the bone under the cuboid breaks or the short plantar ligament tears, producing heel pain.
Physical Examination:
Common findings in the physical examination are:
- Subtle forefoot valgus and a pronated foot, the pronated foot produces an unstable midtarsal joint.
- A tight fibularis (peroneus) longus tendon.
- Careful gait analysis will often reveal that the pain is reproduced in terminal stance, at the onset of heel rise.
- Other findings include asymmetrical weakness of the fibularis (peroneus) longus muscle and decreased ROM of the lateral foot.
Two clinical diagnostic maneuvers, the “midtarsal adduction test” and the “midtarsal supination test,” have been described:
Midtarsal Adduction Test:
During the midtarsal adduction test, the midtarsal joint is passively adducted in the transverse plane (about a superior–inferior axis) while the calcaneus is stabilized.
This is thought to provoke pain by compressing the medial CC joint and distracting the lateral CC joint.

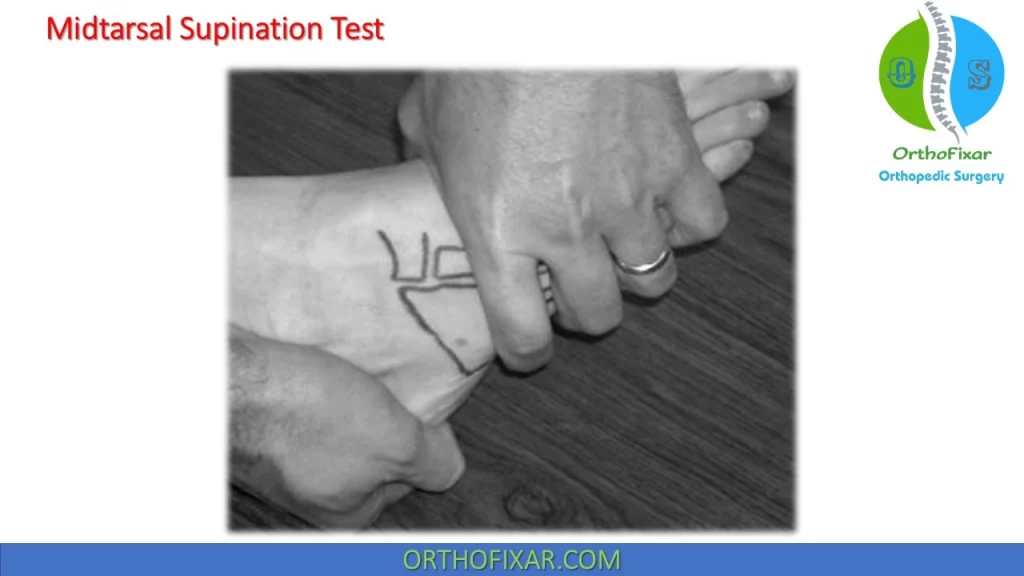
Midtarsal Supination Test:
The midtarsal supination test is similar except that the clinician adds inversion (frontal plane) and plantarflexion (sagittal plane) to the adduction stress, thereby imparting a triplane movement to the midtarsal joint.
Cuboid Shear Test:
For this test the calcaneus is firmly stabilized with one hand while the other hand translates/shears the cuboid plantarward and dorsalward on the fixed calcaneus. As with the midtarsal adduction and supination tests, symptom reproduction is considered a positive test result.

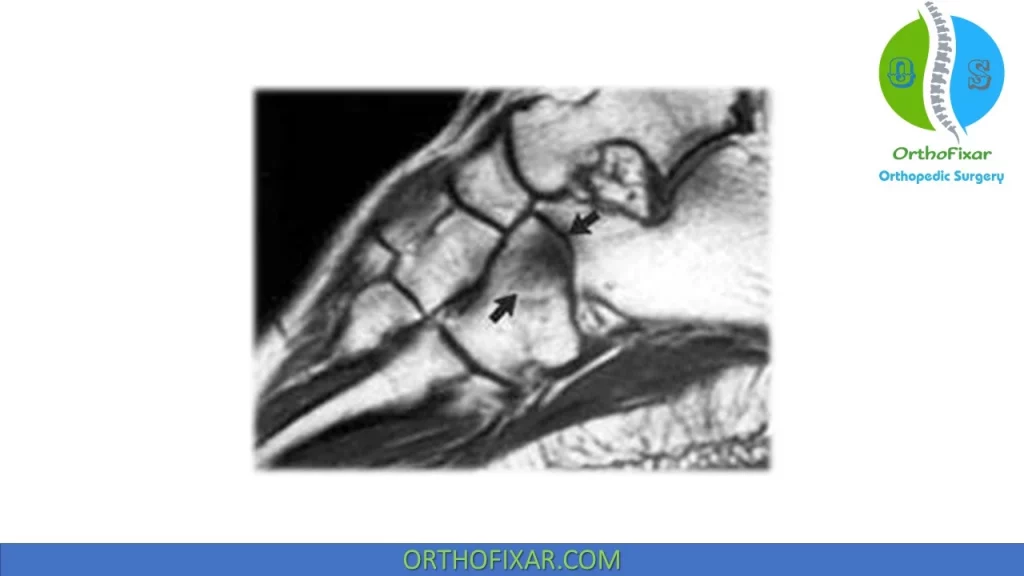
Radiographic Study
Radiography, computerized axial tomography, or magnetic resonance imaging studies have not been shown to aid in the diagnosis of cuboid syndrome.
Calcaneocuboid joint incongruities may be imperceptible with these studies, and non-pathologic variations in lateral foot anatomy are common.
Aberrations in mid-tarsal joint alignment that produce symptoms in weightbearing may also be undetectable with radiography because foot radiographs are typically obtained in non-weightbearing.
Nonetheless, plain radiographs should be obtained to rule out fractures or other significant bony abnormalities and to help establish a differential diagnosis.
Differential Diagnosis of Lateral Foot Pain
Because of the difficulty in accurately diagnosing cuboid syndrome, the differential diagnosis of lateral foot pain should include:
- Fracture or dislocation of the cuboid, calcaneus, or of the fourth or fifth metatarsal bases;
- Calcaneonavicular coalition;
- Fibularis tendinopathy, rupture, or subluxation;
- Plantar fasciitis;
- Extensor digitorum brevis tendonitis;
- Sinus tarsi syndrome;
- Meniscoid of the ankle;
- Gout;
- Tarsitis;
- Lisfranc injury;
- Compression neuropathy of the sural nerve;
- Lateral plantar nerve entrapment.
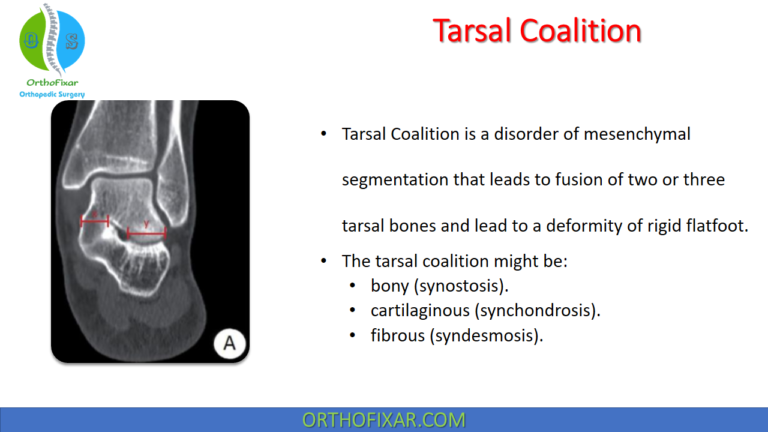
Approximately 90% of tarsal coalitions occur either at the calcaneonavicular joint or the talocalcaneal joint, with the distribution of these two types being equal.
Solitary fractures of the cuboid are rare as are cuboid dislocations, with only 13 reported cases in the literature.
Cuboid syndrome can be easily overlooked when it develops in conjunction with a lateral ankle sprain. Therefore, screening for cuboid syndrome should be considered for all patients with lateral ankle sprains.
Cuboid Syndrome Treatment
The initial treatment often advocated for cuboid syndrome is low-amplitude, high-velocity manipulation of the cuboid.
Thus, unless contraindicated (i.e., bone disease, inflammatory arthritis, gout, neural or vascular compromise, or fracture) a cuboid syndrome manipulation manipulation should be considered when cuboid syndrome is suspected.
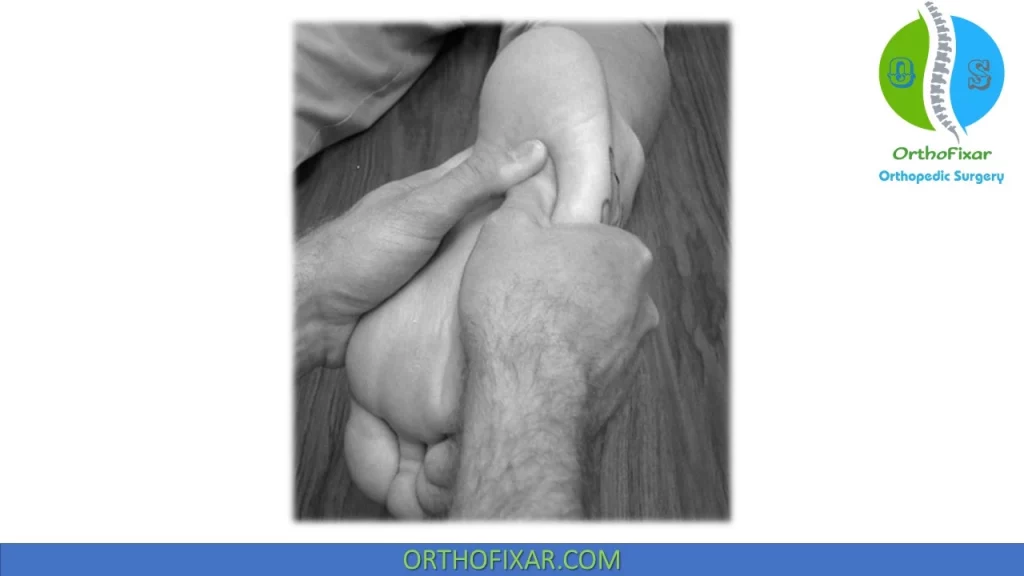
Two manipulative techniques have been described: the “cuboid whip” and the “cuboid squeeze”:
Cuboid Whip
To perform the cuboid whip, the patient is prone and the clinician stands at the patient’s feet.
The clinician interlocks his or her fingers over the dorsum of the forefoot and overlaps his or her thumbs on the plantomedial aspect of the affected cuboid.
The patient’s knee is passively flexed 70 to 90 degrees to slack the superficial peroneal nerve during the manipulation and the ankle is passively placed in 0 degrees of dorsiflexion.
With the patient’s leg relaxed, the clinician abruptly “whips” the foot into inversion and plantarflexion while simultaneously delivering a dorsally directed low-amplitude, high-velocity trust (via the thumbs) to the plantar cuboid.
A “pop” or shift may be heard and/or felt by the clinician and/or patient during the thrust, but these are not requisite for a favorable treatment response.


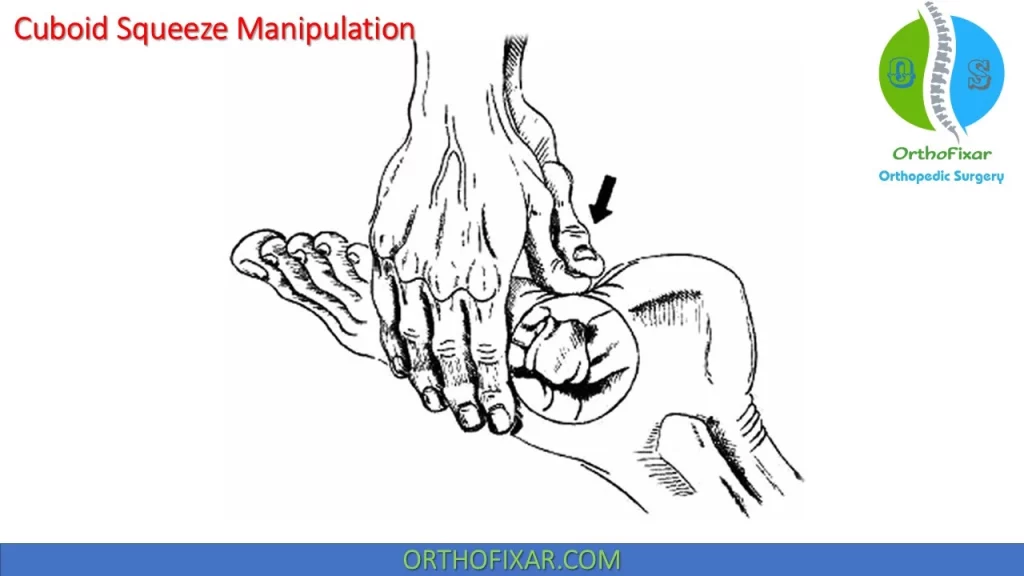
Cuboid squeeze:
Marshall and Hamilton (1992) described a variation of the cuboid whip that they named the cuboid squeeze.
Instead of “whipping” the foot/ankle, the clinician slowly stretches the ankle into maximal plantarflexion and the foot and toes into maximal flexion. When the clinician feels the dorsal soft tissues relax, a low-amplitude, highvelocity thrust is delivered by “squeezing” the cuboid with the thumbs.
The cuboid squeeze requires maximal ankle plantarflexion, which may be inappropriate for patients with a coincident ankle sprain. Immediately after manipulation, clinical tests should be repeated to determine treatment efficacy.
Patients who experience partial or incomplete symptom resolution may benefit from additional manipulations. Patients who experience no relief whatsoever after manipulation should be re-examined and other diagnoses should be considered.
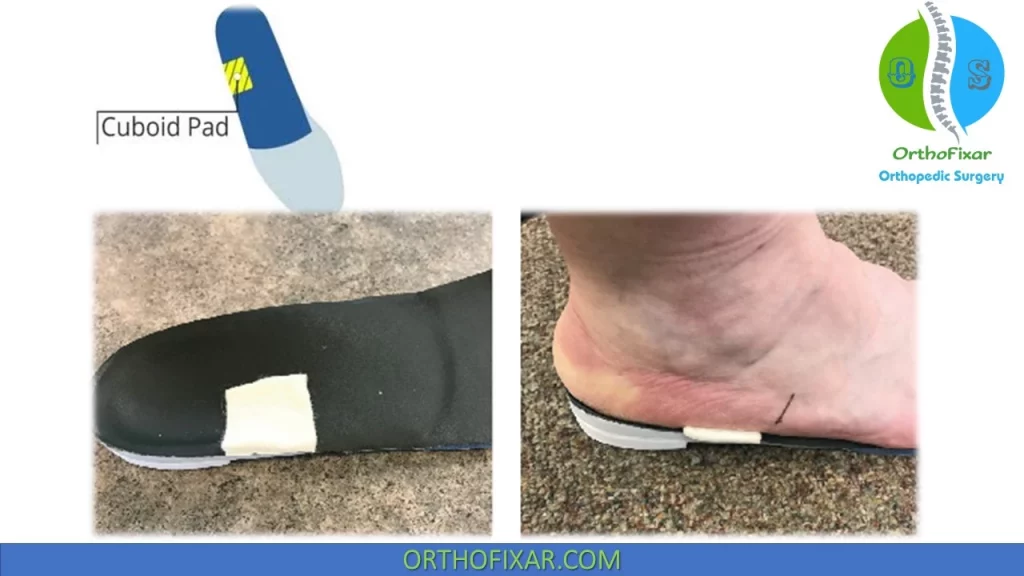
Following the manipulation, low Dye or arch taping, orthotics, and/or cuboid padding may be used to prevent recurrence. Felt padding (~¼ inch) to buttress the plantar cuboid and/or orthotics that reduce excessive pronation may be beneficial in reducing symptoms and preventing recurrence.
Recurrent bouts of cuboid syndrome may be attributable to excessive laxity or insufficiency of the CC joint stabilizers.
Stretching the gastrocnemius, soleus, hamstring, and/ or fibularis longus and strengthening the intrinsic and extrinsic foot muscles have been reported to be helpful in preventing recurrence of cuboid syndrome.
Activities and exercises to improve ankle/foot proprioception are also sensible.
Oral or injectable anti-inflammatory and/ or anesthetic agents may also be beneficial.
References
- Khan K, Brown J, Way S, Vass N, Crichton K, Alexander R, Baxter A, Butler M, Wark J. Overuse injuries in classical ballet. Sports Med. 1995 May;19(5):341-57. doi: 10.2165/00007256-199519050-00004. PMID: 7618011. Pubmed
- Durall CJ. Examination and treatment of cuboid syndrome: a literature review. Sports Health. 2011 Nov;3(6):514-9. doi: 10.1177/1941738111405965. PMID: 23016051; PMCID: PMC3445231. Pubmed
- Omey ML, Micheli LJ. Foot and ankle problems in the young athlete. Med Sci Sports Exerc. 1999 Jul;31(7 Suppl):S470-86. doi: 10.1097/00005768-199907001-00008. PMID: 10416548.
- Newell SG, Woodle A. Cuboid Syndrome. Phys Sportsmed. 1981 Apr;9(4):71-6. doi: 10.1080/00913847.1981.11711057. PMID: 27442099.
- Helfand AE. Nail and hyperkeratotic problems in the elderly foot. Am Fam Physician. 1989 Feb;39(2):101-10. PMID: 2521760.
- Subotnick SI: Foot Injuries. In: Subotnick SI, ed. Sports Medicine of the Lower Extremity. Philadelphia, PA: Churchill Livingstone, 1999:207– 260.
- Dutton’s Orthopaedic Examination, Evaluation, And Intervention 3rd Edition.
- S. Brent Brotzman, Md. Clinical Orthopaedic rehabilitation: an evidence based approach. 3rd Edition.