Achilles tendinitis is the most common overuse syndrome of the lower leg, accounting for 5–18% of the total number of running injuries.
The Achilles tendon is placed under extreme and rapid eccentric loading forces during such activities as running, standing up while cycling, ballet, gymnastics, soccer, and basketball.
Achilles Tendinitis Causes
The underlying mechanism of Achilles tendinitis is not well understood, but a number of mechanisms have been proposed of which the biomechanical hypothesis is the most popular.
Pronation & supination of the foot:
Immediately after the foot makes contact with the ground in a supinated position, it pronates and then supinates again as the propulsion phase approaches. The pronated foot imparts an internal rotation force through the tibia, whereas knee extension imparts an external rotation force through the tibia. The overpronated foot places the medial aspect of the Achilles tendon under tension, generating an obligatory internal tibial rotation, which tends to draw the Achilles tendon medially.
The rapid and repeated transitions from pronation to supination cause the Achilles tendon to undergo a “bow-string” or “whipping” action. Moreover, if the foot remains in a pronated position after knee extension has begun, the external tibial rotation at the knee and the internal tibial rotation at the foot result in a “wringing” or twisting action of the tendon.

See Also: Ankle Anatomy
Eccentric contraction of the triceps surae during support:
Another proposed mechanism involves the eccentric contraction of the triceps surae during support. Maximal triceps sural contraction is associated with adduction and supination of the foot. At heel strike, the calf muscles undergo a rapid shortening before lengthening, as the tibia rotates forward over the foot. The calf muscles then shorten again during the forward propulsion phase. These abrupt alternations in muscle action may cause microtears in the tendon.
Number of other factors appear to have some influence on the development of Achilles tendinitis:
Stretching: the injured runners were less likely to incorporate stretching into their regular training routines. However, whether stretching habits can be related to the incidence of overuse injuries remains uncertain.
Training variables: Overuse injuries of the tendons have been strongly associated with a number of training variables
including training at a faster pace, and hill training.
Fatigue: Overtraining has been found to correlate with muscle fatigue and microtears of a tendon.
Exercise variable: Muscular insufficiency has been proposed as a significant factor in the inability to eccentrically control dorsiflexion during the beginning of the initial contact phase of running.
Anthropometric variables: One study determined that 20% of the injured runners with Achilles tendinitis had cavus feet. A potential cause was compensatory overpronation resulting from the inflexibility of the cavus foot. A high-arched foot has also been found to be related to the incidence of various overuse syndromes by a number of other studies.
Age: Some studies have found a correlation between age and the pathogenesis of running injuries, whereas others have found no associations.
Shoe type: Spiked running shoes, which provide minimal shock absorption and which lock the feet on the surface during the single support phase during running have been correlated with Achilles tendinitis. Theoretically, this type of shoe transfers the lateral and vertical torque shear forces directly to the foot and ankle and through the Achilles tendon, thereby increasing the overloading of the tendon, and causing microtrauma and inflammation of the tendon.
Sacroiliac joint dysfunction: The primary function of the pelvis appears to be as a shock absorber, transmitting the weight of the trunk and upper extremities to the lower limbs and distributing the ground reaction forces. The ground forces, which tend to rotate the innominate posteriorly, and the trunk forces combine to provide a mechanism of stability. Posterior dysfunction is reported to be the most common lesion of the sacroiliac articulation by several authors.
This results in a functional shortening and external rotation of the involved leg, both of which may influence the kinematic chain of the lower extremity in the following manner:
- The ankle and foot position will be in external rotation, instead of neutral, at heel strike.
- Due to the transfer of body weight over the involved leg during the rest of the stance phase, the loading of the lateral aspect of the heel will be short, the following pronation prolonged, and the inversion delayed. This may decrease the amount of dorsiflexion in the ankle, thus minimizing the tension in the plantar soft tissues. This, in turn, decreases the leverage of the Achilles tendon and the truss mechanism may not be activated due to insufficient hyperextension of the big toe.
- Because of the relative ineffectiveness of the foot’s truss mechanism at terminal stance, together with the decrease in leverage of the Achilles tendon, the triceps surae will have to activate more motor units to ensure continued performance, thus putting additional loading on the Achilles tendon.
Types of Achilles Tendinitis
Achilles tendinitis typically occurs as one of two types of tendinitis:
- Insertional Achilles Tendonitis: involves the tendon–bone interface.
- Non-Insertional Achilles Tendonitis: occurs just proximal to the tendon insertion on the calcaneus in or around the tendon substance.
Non-Insertional Achilles Tendonitis can be referred to as peritendinitis, peritendinitis with tendinosis, or tendinosis:
- Peritendinitis: The inflammation in peritendinitis is limited to the peritendon, and thickening can result.
- Peritendinitis with tendinosis: This condition describes a second stage of inflammation, in which a portion of the Achilles tendon itself is involved in the disease process.
- Pure tendinosis: This condition, which typically affects the weekend warrior, is characterized by microscopic and macroscopic mucoid degeneration of the tendon.
Symptoms & Signs
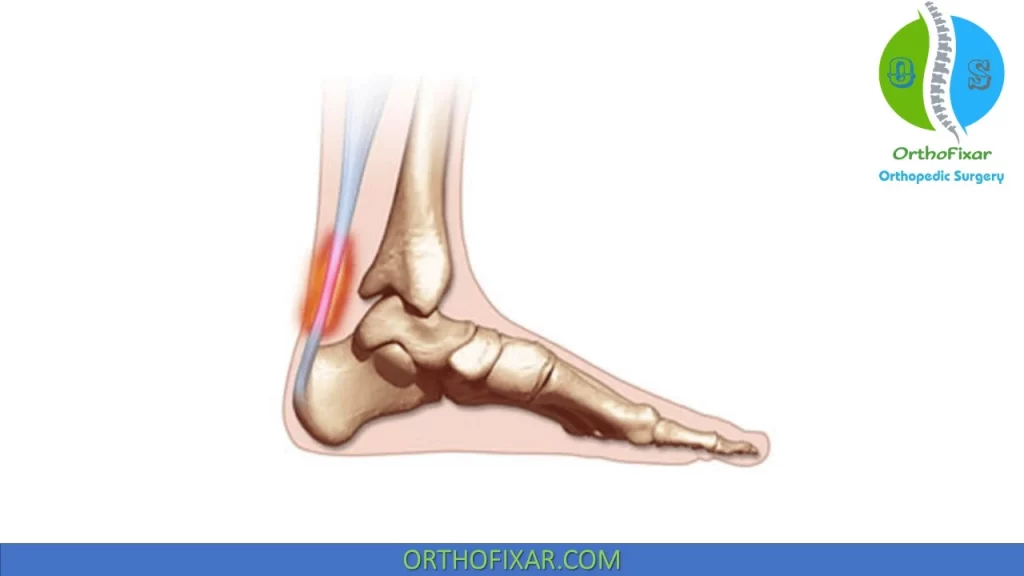
Clinical symptoms associated with Achilles tendinitis consist of a gradual onset of Achilles Tendon Pain and swelling 2–3 cm proximal to its insertion, which is exacerbated by activity. The Achilles Tendon Pain typically worsens over time, until it inhibits the individual from running, at which point they usually seek medical attention.
Some patients will present with pain and stiffness along the Achilles tendon when rising in the morning or complain of pain at the start of activity, which improves as the activity progresses. In fact, in the early stages of the condition, morning stiffness may be the only symptom, whereas pain is felt even at rest in the advanced stages.
The vast majority of symptomatic patients are runners who complain of pain in the posterior aspect of the heel, approximately 2 cm proximal to the superior margin of the calcaneus, which increases during running activities.
The Achilles tendon and heel may be examined with the patient in sitting or prone. Upon observation, the patient will often be found to have pronated feet, and the presence of swelling around the tendon is common.
Systematic palpation is performed along the tendon, over the heel, along the posterior border of the calcaneus, and down to the heel pad.
Localization of the tenderness is extremely important:
- Tenderness located 2–6 cm proximal to the insertion is indicative of noninsertional tendinitis,
- whereas pain at the bone–tendon junction is more indicative of insertional tendinitis.
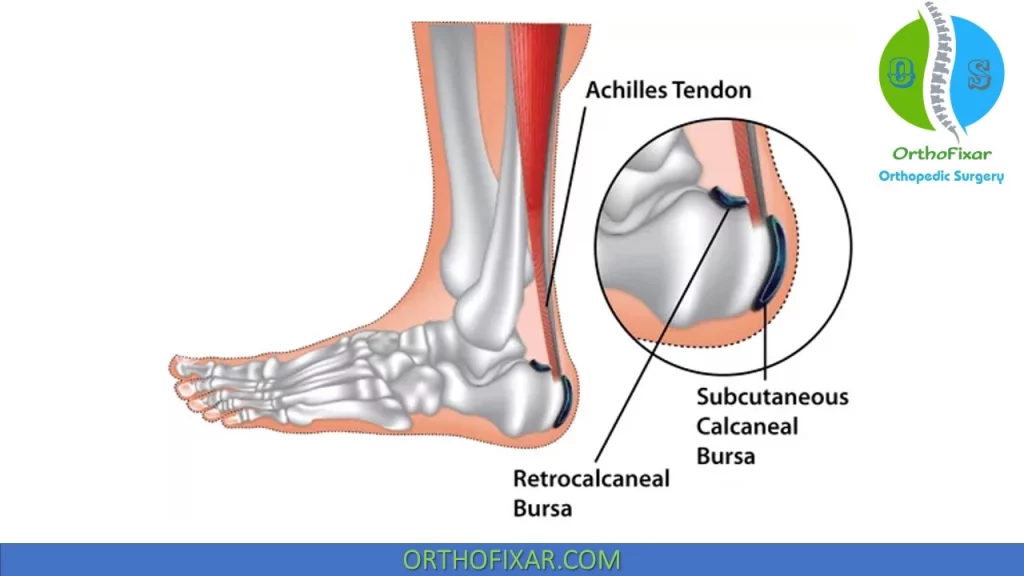
If there is an area in the tendon itself, which is discrete and painful with side-to-side pressure of the fingers, this often indicates an area of mucoid degeneration or a small partial rupture of the tendon. If the tenderness is in the area of the retrocalcaneal bursa, which is noted by side-to-side pressure in that area, this is the primary area of involvement.
A lack of 20 degrees of dorsiflexion in knee extension signifies adaptive shortening of the gastrocnemius, and an inability to dorsiflex 30 degrees in knee flexion implicates the soleus as well.
Analysis of gait may reveal an antalgic gait, with the involved leg held in external rotation during both the stance and swing phases. There is often pain with resisted testing of the gastrocnemius/soleus complex
See Also: Gait Cylce
Differential Diagnosis
The differential diagnosis for posterior heel pain includes:
- retrocalcaneal bursitis,
- metabolic diseases,
- arthritis and chondropathic diseases of the ankle joint,
- tibia vara,
- os trigonum,
- a calcaneal contusion,
- plantar heel pain,
- calcaneal stress fracture,
- stress fractures of the fibula or tibia.
Radiology
Lateral X-ray of the foot may show a spur and intratendinous calcification at the isertion of Achilles Tendon. It should be differentiated from Hugland Deformity.
MRI can demonstrate amount of degeneration or a thickened tendon.

Achilles Tendinitis Treatment
The Achilles Tendinitis Treatment in relation to exercise intensity varies according to the severity of the symptoms:
- Type I: Characterized by pain that is only experienced after activity. These patients should reduce their exercise by 25%.
- Type II: Characterized by pain that occurs both during and after activity but does not affect performance. These patients should reduce their training by 50%.
- Type III: Characterized by pain during and after activity that does affect performance. These patients should temporarily discontinue running.
The conservative Treatment of Achilles Tendinitis include:
- modification of extrinsic factors: training errors including a sudden increase in mileage, excessive hill running, and improper shoes),
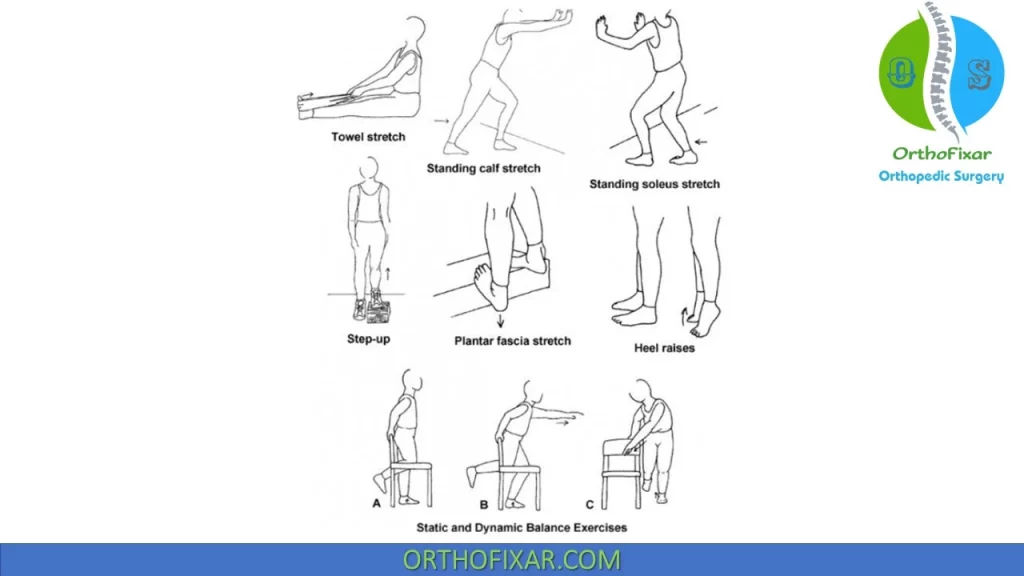
- Achilles stretching,
- eccentric strengthening of the calf muscles,
- the correction of any lower chain asymmetries (low-back, pelvic, and hip flexor asymmetries; knee flexion contracture; femoral anteversion; and foot pronation),
- electrotherapeutic modalities as appropriate,
- correct shoe wear,
- orthotics: appropriately designed orthoses made from a mold of the foot held in subtalar neutral,
- non–weight-bearing can be of significant benefit.
A literature review that investigated the best intervention for a patient with recurrent Achilles tendinitis, based on its validity and strength, recommended the 12-week eccentric program as outlined by Alfredson et al:
- The program consists of two types of eccentric exercises: eccentrically loading the calf muscles with the knee bent and the knee straight and three sets of 15 repetitions using just body weight to start, with the patient instructed to continue unless the pain becomes disabling.
- The exercises are performed two times per day, each day of the week, for 12 weeks. If only minor pain or discomfort is experienced, the patient is instructed to increase the load by using a backpack loaded with weight. The 37-year old patient in this study was compliant with the program and was able to successfully progress to marathon training within 3 weeks of beginning the program.
Operative Treatment
Operative Treatment for Achilles Tendinitis is indicated if conservative treatment has failed.
Operative Treatment includes:
- retrocalcaneal bursa excision,
- debridement of diseased tendon,
- calcaneal bony prominence resection.
When > 50% of Achilles tendon insertion is removed during debridement, tendon augmentation or transfer (FDL, FHL, or PB) or suture anchor repair should be considered.
Retrocalcaneal Bursitis
Retrocalcaneal bursitis is a distinct entity denoted by pain that is anterior to the Achilles tendon, just superior to its insertion on the os calcis. This type of bursitis appears to be more common in older individuals and low-level recreational athletes.
The bursa becomes inflamed, hypertrophied, and adherent to the underlying tendon, resulting in deep pain and visible swelling. Characteristic findings include pain with a two finger squeeze just superior and anterior to the Achilles insertion and pain with passive dorsiflexion.
Retrocalcaneal bursitis is treated conservatively with shoe modifications (open backed if necessary) and a heel lift.
In rare cases, a bursectomy with associated resection of the posterior superior margin of the os calcis is necessary. A small percentage of the population has an adventitious subcalcaneal bursa, which may become inflamed and cause heel pain.
References
- Clement DB, Taunton JE, Smart GW. Achilles tendinitis and peritendinitis: etiology and treatment. Am J Sports Med. 1984 May-Jun;12(3):179-84. doi: 10.1177/036354658401200301. PMID: 6742297.
- Scioli MW: Achilles tendinitis. Orthop Clin North Am 25:177–182, 1994.
- Nichols AW: Achilles tendinitis in running athletes. J Am Bd Fam Pract 2:196–203, 1989.
- Clain MR, Baxter DE: Achilles tendinitis. Foot Ankle 13:482–487, 1992.
- Voorn R: Case report: Can sacroiliac joint dysfunction cause chronic Achilles tendinitis? J Orthop Sports Phys Ther 27:436–443, 1998.
- McCrory JL, Martin DF, Lowery RB, et al: Etiologic factors associated with Achilles tendinitis in runners. Med Sci Sports Exerc 31:1374–1381, 1999.
- Smart GW, Taunton JE, Clement DB: Achilles tendon disorders in runners: A review. Med Sci Sport Exerc 12:231–243, 1980.
- Jacobs SJ, Berson BJ: Injuries to runners: A study of entrants to a 10,000 meter race. Am J Sports Med 14:151–155, 1986.
- Pinshaw R, Atlas V, Noakes TD: The nature and response to therapy of 196 consecutive injuries seen at a runners’ clinic. S Afr Med J 65:291–298, 1984.
- Brunet ME, Cook SD, Brinker MR, et al: A survey of running injuries in 1505 competitive and recreational runners. J Sports Med Phys Fitness 30:307–315, 1990.
- van Mechelen W, Hlobil H, Kemper HCG, et al: Prevention of running injuries by warm-up, cool-down and stretching exercises. Am J Sports Med 21:711–719, 1993.
- Hess GP, Cappiello WL, Poole RM, et al: Prevention and treatment of overuse tendon injuries. Sports Med 8:371–384, 1989.
- Clement DB, Taunton JE, Smart GW, et al: A survey of overuse running injuries. Physician Sportsmed 9:47–58, 1981.
- DickinsonPH, CouttsMB,Woodward EP, et al: Tendo achillis bursitis: A report of twenty-one cases. J Bone Joint Surg 48:77–81, 1966.
- Myerson MS, McGarvey W: Disorders of the Achilles tendon insertion and Achilles tendinitis. AAOS Instr Course Lect 48:211–218, 1999.
- Frey CC, Rosenburg Z, Shereff M, et al: The retrocalcaneal bursa: Anatomy and bursography. Foot Ankle 13:203–207, 1982.
- Leach RE, Schepsis AA: Achilles Tendinitis. Bulgaria: Forum Medicus, 1986.
- Reynolds NL, Worrell TW: Chronic Achilles peritendinitis: Etiology,pathophysiology, and treatment. J Orthop Sports Phys Ther 13:171–176, 1991.
- Goodnite EA: The practical use of evidence-based practice in determining the best treatment for a patient with recurrent Achilles tendinitis. Orthop Pract 17:12–14, 2005.