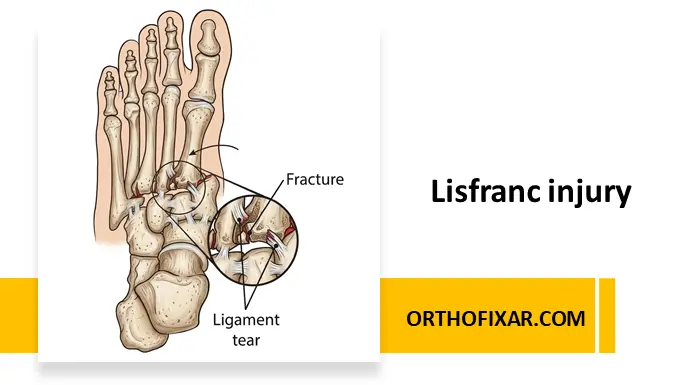
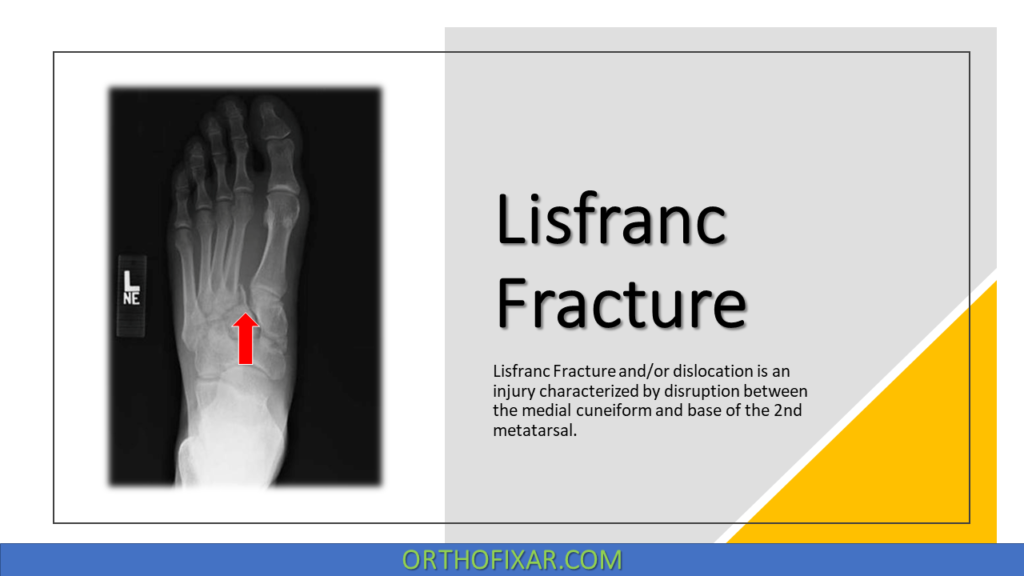
A Lisfranc fracture or injury is a rare but potentially debilitating injury involving the tarsometatarsal (TMT) joint complex. It is characterized by disruption between the medial cuneiform and the base of the second metatarsal. Approximately 20% of Lisfranc injuries are initially overlooked, highlighting the importance of a careful clinical and radiological evaluation.
Lisfranc injuries can be bony, involving fractures, or ligamentous, with Lisfranc ligament tears. The Lisfranc ligament, an interosseous structure running from the medial cuneiform to the base of the second metatarsal on the plantar surface, is critical for stabilizing the second metatarsal and maintaining the midfoot arch.
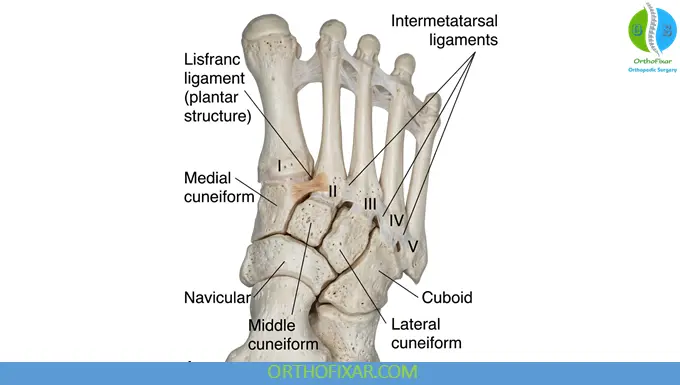
Anatomy of the Lisfranc Joint Complex
The Lisfranc joint complex consists of:
- Tarsometatarsal joints
- Intermetatarsal joints
- Intertarsal joints
Injuries to the tarsometatarsal articulation range from mild sprains to widely displaced, debilitating injuries. Understanding the anatomy is key to diagnosing and treating these injuries effectively.
See Also: Foot Anatomy
Mechanism of Injury
Lisfranc injury occurs through direct or indirect mechanisms:
Direct Injury
A dorsally applied force results in:
- Plantar metatarsal displacement if the force is applied to the metatarsal base.
- Dorsal metatarsal displacement if the force is applied to the cuneiforms.
Direct Lisfranc injury often involves:
- High-energy trauma
- Associated tarsal fractures
- Significant soft-tissue damage
- Risk of compartment syndrome
Indirect Injury
Indirect Lisfranc injury occurs due to axial loading combined with twisting on a plantarflexed foot. Features include:
- Dorsal displacement of metatarsals
- Diastasis between first and second metatarsals
- Greater mobility between the first and second metatarsals due to relatively weaker dorsal ligaments
Lisfranc Fracture Symptoms
Patients with Lisfranc injury typically present with:
- Pain and tenderness on the dorsum of the foot
- Swelling and foot deformity
- Possible neurovascular compromise due to impingement or laceration of the dorsalis pedis artery
- Severe foot swelling in high-energy injuries, requiring serial neurovascular monitoring for compartment syndrome
Radiology
Imaging is essential for diagnosis:
- Plain radiographs: Anteroposterior, internal oblique, and lateral views of the foot to assess TMT articulations
- CT scan: Recommended if plain films are normal but clinical suspicion remains; identifies osseous displacement, intra-articular comminution, and associated fractures (cuneiforms, cuboid, metatarsals)
Lisfranc injury Classification
Classification schemes for Lisfranc injuries guide the clinician in defining the extent and pattern of injury, although they are of little prognostic value.
Download Orthopedic Classification App for Android / iOS devices.
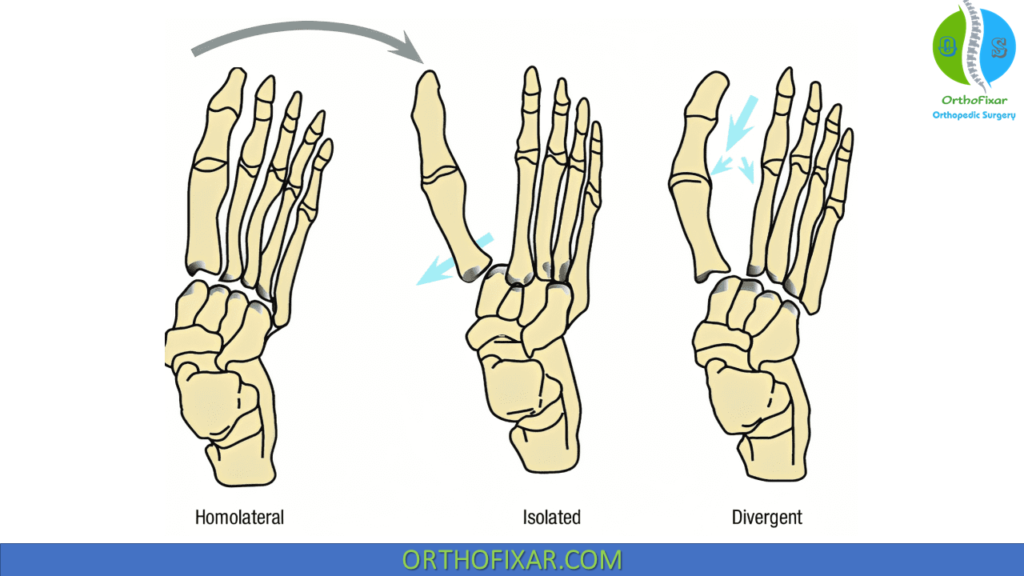
Quenu and Kuss Classification
This classification is based on commonly observed patterns of injury:
| Homolateral | All five metatarsals displaced in the same direction |
| Isolated | One or two metatarsals displaced from the others |
| Divergent | Displacement of the metatarsals in both the sagittal and coronal planes |
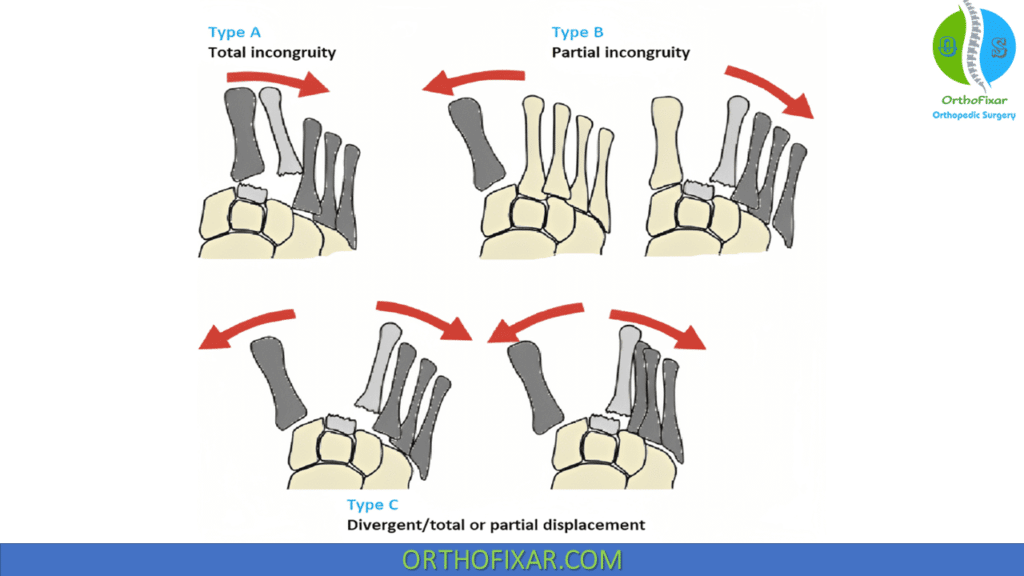
Myerson Classification
This is based on commonly observed patterns of injury with regard to treatment:
| Total incongruity | Lateral and dorsoplantar dislocation |
| Partial incongruity | Medial and lateral dislocation |
| Divergent | Partial and total dislocation |
Lisfranc Fracture Treatment
Non-Surgical Management
Indicated for ligamentous injuries with or without small avulsion fractures and non-displaced fractures:
- Non-weight-bearing short leg cast for 8 weeks
- Gradual weight-bearing with a removable boot
- Repeat radiographs to monitor displacement after swelling resolves
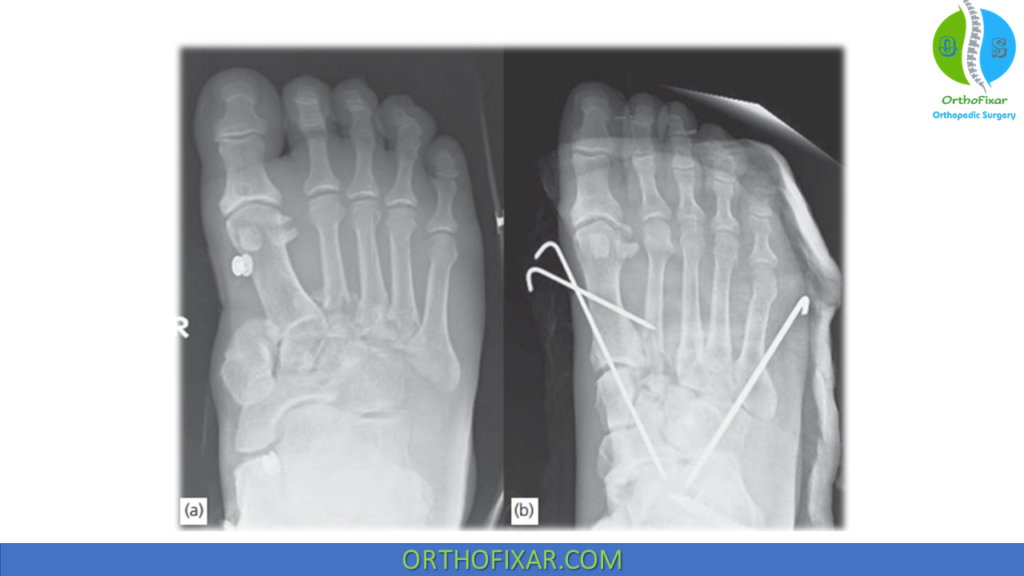
Surgical Management
Indicated for displacement >2 mm in the tarsometatarsal joint:
- Closed reduction & percutaneous fixation: Rarely successful due to interposed Lisfranc ligament
- Open reduction & internal fixation (ORIF): Preferred approach
- Screws: 4.0 mm for medial and middle columns
- Kirschner wires: Lateral column
- Lateral plating and bone grafting may be needed for severe abduction
Postoperative care:
- Non-weight-bearing for 8 weeks
- Gradual weight-bearing in a removable boot
- Implant removal: Lateral column at 6–12 weeks, medial column at 4–6 months
- Partial midfoot arthrodesis may be considered for severe injuries
Prognosis
Early diagnosis and anatomic reduction are critical to prevent:
- Chronic midfoot pain
- Post-traumatic arthritis
- Arch collapse or deformity
Delayed or missed diagnosis increases the risk of long-term disability.
Key Takeaways
- Lisfranc injuries are rare and often overlooked; high suspicion is essential
- Can be bony, ligamentous, or both
- Require careful imaging; CT is recommended for subtle injuries
- ORIF is standard for displaced Lisfranc fractures; non-surgical management is reserved for non-displaced injuries
- Early diagnosis improves outcomes and reduces risk of chronic deformity
References & More
- Peicha G, Labovitz J, Seibert FJ, et al. The anatomy of the joint as a risk factor for Lisfranc dislocation and fracturedislocation: an anatomical and radiological case control study. Journal of Bone and Joint Surgery (British) 2002;84:981–5. Pubmed
- Aitken AP, Poulson D. Dislocations of the tarsometatarsal joint. Journal of Bone and Joint Surgery (American) 1963;45:246. Pubmed
- Quenu E, Kuss G. Etude sur les luxations du metatarse du diastasis entre le 1er et le 2e metatarsien. Revue de Chirurgie 1909;39:281–336.
- Myerson M, Fisher R, Burgess A, et al. Dislocations of the tarsometatarsal joints: end results correlated with pathology and treatment. Foot and Ankle 1986;6:225.
- Teng AL, Pinzur MS, Lomasney L, et al. Functional outcome following anatomic restoration of tarsal-metatarsal fracture-dislocation. Foot and Ankle International 2002;23:922-6.
- Mulier T, Reynders P, Dereymaeker G, Broos P. Severe Lisfrancs injuries: primary arthrodesis or ORIF? Foot and Ankle International 2002;23:902–5.
- Mercer’s Textbook of Orthopaedics and Trauma, Tenth edition.