Pediatric hip fractures are rare but potentially devastating injuries in children. They account for less than 1% of all fractures in the pediatric population and occur far less frequently than hip fractures in adults. Despite their rarity, these injuries are associated with serious complications, particularly osteonecrosis of the femoral head, premature physeal closure, coxa vara, and nonunion.
Most pediatric hip fractures result from high-energy trauma such as motor vehicle accidents or falls from significant heights. Prompt diagnosis and early anatomic reduction are critical to preserving blood supply to the femoral head and minimizing long-term disability.
Epidemiology
- Pediatric hip fractures represent less than 1% of childhood fractures
- Approximately 75%–80% are caused by severe trauma
- More common in:
- Motor vehicle collisions
- Falls from height
- Sports trauma
- Pathologic fractures may occur through:
- Bone cysts
- Fibrous dysplasia
- Bone tumors
- Stress fractures are uncommon in children
Anatomy of the Pediatric Hip
Understanding proximal femoral anatomy is essential because growth plate injury and vascular disruption strongly influence prognosis.
Ossification Centers
- Proximal femur begins ossification at approximately 7 weeks in utero
- Proximal femoral epiphysis appears between 4–8 months of age
- Greater trochanter ossifies around 4 years
- Proximal femoral epiphysis fuses at approximately 18 years
- Trochanteric apophysis fuses between 16–18 years
Blood Supply of the Femoral Head
The blood supply is primarily derived from:
By age 3–4 years, the posterosuperior retinacular vessels become the dominant blood supply to the femoral head.
The artery of the ligamentum teres contributes minimally before age 8 years.
Disruption of these vessels significantly increases the risk of avascular necrosis (AVN).
Mechanism of Injury
Pediatric hip fractures may result from:
- Axial loading
- Torsional forces
- Hyperabduction injuries
- Direct trauma
Common mechanisms include:
- Motor vehicle accidents
- Pedestrian trauma
- Falls from height
- Sports injuries
Pathologic fractures should raise suspicion for underlying bone disease.
Clinical Presentation
Children with hip fractures commonly present with:
- Severe hip or groin pain
- Inability to bear weight
- Shortened lower extremity
- External rotation deformity
- Painful hip motion
- Swelling and ecchymosis
- Tenderness around the proximal femur
A complete neurovascular examination is mandatory.
Diagnostic Evaluation
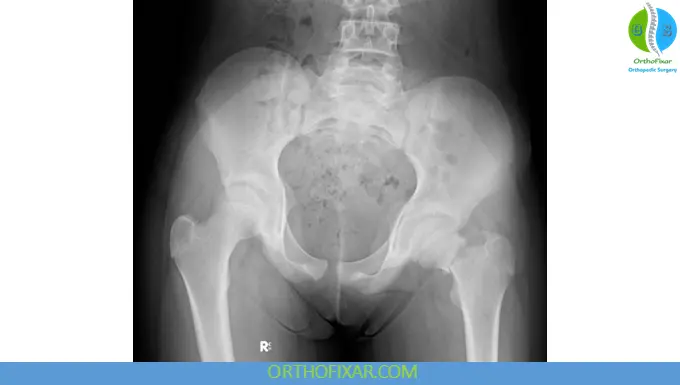
Plain Radiographs
Initial imaging includes:
- Anteroposterior (AP) pelvis radiograph
- Cross-table lateral hip radiograph
Internal rotation views may improve visualization if tolerated.
Computed Tomography (CT)
Useful for:
- Nondisplaced fractures
- Stress fractures
- Preoperative planning
Magnetic Resonance Imaging (MRI)
MRI can detect occult fractures within 24 hours and evaluate associated soft tissue injury.
Bone Scan
Radioisotope bone scans may demonstrate increased uptake approximately 48 hours after injury.
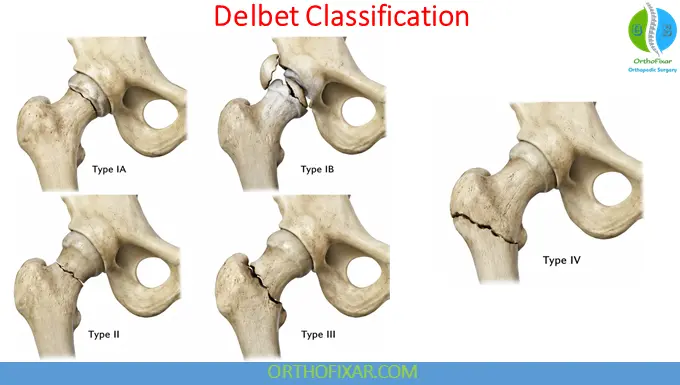
Delbet Classification of Pediatric Hip Fractures
The Delbet classification is the most widely used system and correlates strongly with the risk of osteonecrosis.
Type I: Transepiphyseal Fracture
- Approximately 8% of pediatric hip fractures
- Highest risk of osteonecrosis
- Often associated with hip dislocation
Subtypes
- Type IA: Without dislocation
- Type IB: With dislocation
Key Features
- AVN risk approaches 100%
- May represent the traumatic end of slipped capital femoral epiphysis spectrum
Type II: Transcervical Fracture
- Most common type
- Represents approximately 45% of pediatric hip fractures
- Frequently displaced
Complications
- Osteonecrosis in up to 50% of cases
Type III: Cervicotrochanteric Fracture
- About 30% of pediatric hip fractures
- More common in children than adults
Complications
- AVN rate approximately 20%–30%
Type IV: Intertrochanteric Fracture
- Represents 10%–15% of cases
- Lowest risk of AVN due to better blood supply
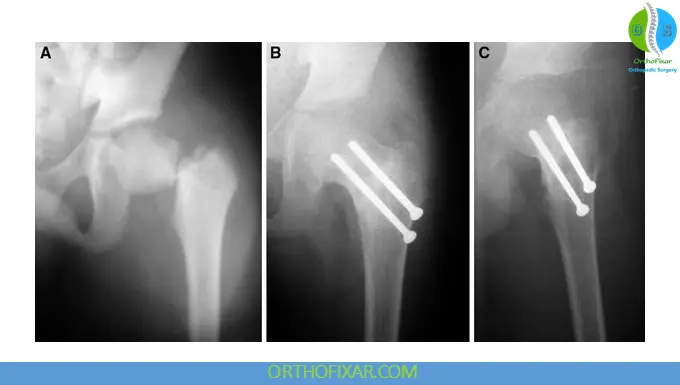
Treatment of Pediatric Hip Fractures
Management depends on fracture type, displacement, age, and skeletal maturity.
General Principles
- Urgent reduction and fixation
- Restoration of anatomy
- Preservation of femoral head blood supply
- Stable fixation
- Avoidance of physeal injury when possible
Type I Fracture Treatment
Recommended Management
- Closed reduction and pin fixation
- Smooth pins in younger children
- Partially threaded pins in older children
Open reduction is indicated if closed reduction fails.
Type II Fracture Treatment
Nondisplaced Fractures
Options include:
- Abduction spica cast
- In situ pinning
Displaced Fractures
- Closed reduction and internal fixation
- Open reduction if necessary
Avoid transphyseal pin placement whenever possible.
Type III Fracture Treatment
Nondisplaced
- Traction followed by spica casting
- Immediate spica casting
- In situ fixation
Displaced
- Open reduction and internal fixation (ORIF)
Type IV Fracture Treatment
Nondisplaced
- Traction for 2–3 weeks
- Abduction spica cast for 6–12 weeks
Displaced or Unstable
- Open reduction and internal fixation
Complications of Pediatric Hip Fractures
Osteonecrosis (Avascular Necrosis)
AVN is the most serious complication.
- Overall incidence approximately 40%
- Risk increases with:
- Proximal fracture location
- Fracture displacement
- Delay in treatment
Ratliff Classification of AVN
Type I
- Complete femoral head involvement
- Femoral head collapse
- Poor prognosis
Type II
- Partial head involvement
- Minimal collapse
Type III
- Femoral neck involvement only
- Femoral head spared
Premature Physeal Closure
Occurs in up to 60% of cases.
Potential consequences include:
- Femoral shortening
- Coxa vara
- Short femoral neck
- Limb length discrepancy
Risk increases with transphyseal fixation.
Coxa Vara
Occurs in approximately 20% of patients.
Usually caused by:
- Inadequate reduction
- Loss of fixation
- Malunion
Anatomic reduction and stable fixation reduce incidence.
Nonunion
Occurs in approximately 10% of cases.
Risk factors include:
- Poor reduction
- Inadequate fixation
- Delayed diagnosis
Treatment may require:
- Valgus osteotomy
- Bone grafting
- Revision fixation
Prognosis
Outcomes depend on:
- Fracture type
- Degree of displacement
- Time to treatment
- Presence of osteonecrosis
Type I fractures have the worst prognosis because of the extremely high risk of femoral head ischemia.
Early diagnosis and stable fixation significantly improve long-term outcomes.
Key Points
- Pediatric hip fractures are rare but serious injuries
- Most result from high-energy trauma
- Delbet classification predicts AVN risk
- Type I fractures have the highest complication rate
- Urgent reduction and fixation are critical
- Osteonecrosis remains the most feared complication
- Long-term follow-up is essential to monitor growth disturbance and deformity
Frequently Asked Questions (FAQs)
What is the most common pediatric hip fracture?
Delbet Type II transcervical fractures are the most common pediatric hip fractures.
What is the most serious complication?
Avascular necrosis (osteonecrosis) of the femoral head is the most serious complication.
Why are pediatric hip fractures dangerous?
These fractures may disrupt blood supply to the femoral head, causing permanent deformity and arthritis.
Can children recover fully from hip fractures?
Many children recover well with prompt treatment, but complications such as AVN or growth disturbance can affect long-term outcomes.
Conclusion
Pediatric hip fractures are uncommon orthopedic emergencies associated with substantial morbidity. Accurate diagnosis, understanding of proximal femoral vascular anatomy, and prompt surgical management are essential to reduce complications and optimize outcomes. The Delbet classification remains the cornerstone for prognostication and treatment planning. Long-term surveillance is critical because growth disturbance and osteonecrosis may develop months or years after injury.
References & More
- Boardman MJ, Herman MJ, Buck B, Pizzutillo PD. Hip fractures in children. J Am Acad Orthop Surg. 2009 Mar;17(3):162-73. doi: 10.5435/00124635-200903000-00005. PMID: 19264709. Pubmed
- Theunissen WWES, Veldman HD, Witlox MA. Een heupfractuur bij een kind [Management of pediatric hip fractures]. Ned Tijdschr Geneeskd. 2025 Aug 11;169:D8458. Dutch. PMID: 40831414. Pubmed
- Papalia R, Torre G, Maffulli N, Denaro V. Hip fractures in children and adolescents. Br Med Bull. 2019 Mar 1;129(1):117-128. doi: 10.1093/bmb/ldz004. PMID: 30753305. Pubmed
- Lark RK, Dial BL, Alman BA. Complications After Pediatric Hip Fractures: Evaluation and Management. J Am Acad Orthop Surg. 2020 Jan 1;28(1):10-19. doi: 10.5435/JAAOS-D-17-00689. PMID: 31633660. Pubmed
- Egol KA. Handbook of fractures. 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2019.