A hip dislocation is a serious orthopedic emergency in which the femoral head is displaced from the acetabulum (hip socket). Due to the inherent stability of the hip joint, dislocations typically occur only after high-energy trauma such as motor vehicle accidents or falls from height.
Up to 50% of patients with hip dislocations sustain associated injuries, including fractures of the pelvis, femur, or spine.
Epidemiology and Key Facts
- Most cases occur in men aged 16–40 years
- Motor vehicle accidents are the leading cause
- Posterior dislocations account for 85–90% of cases
- Anterior dislocations represent 10–15%
- Sciatic nerve injury: 10–20% (posterior cases)
- Osteonecrosis risk: 2–17%
- Post-traumatic arthritis: ~16%
Unrestrained passengers are at significantly higher risk, emphasizing the protective role of seatbelts.
Anatomy of the Hip Joint
The hip is a ball-and-socket joint composed of:
- Femoral head (ball)
- Acetabulum (socket) formed by:
- Ilium
- Ischium
- Pubis
Key Stabilizing Structures:
- Labrum → deepens the socket
- Capsule and ligaments:
- Iliofemoral ligament
- Pubofemoral ligament
- Ischiofemoral ligament
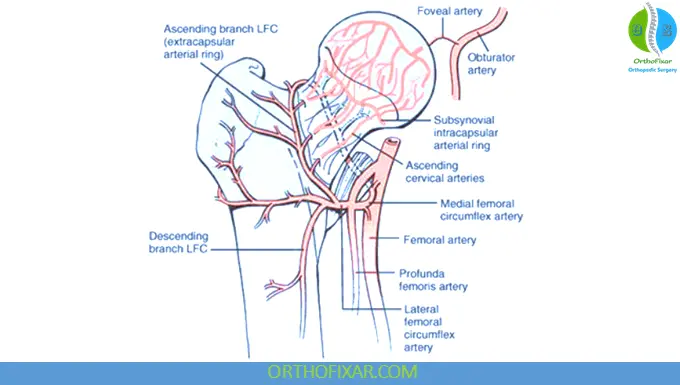
Blood Supply:
- Primarily from:
- Minor contribution:
- Artery of ligamentum teres
Damage to this vascular network can lead to osteonecrosis (avascular necrosis).
See Also: Hip Joint Anatomy
Mechanism of Injury
Hip dislocations usually result from high-energy trauma, including:
- Dashboard injuries (knee striking dashboard)
- Falls from height
- Industrial accidents
Force Transmission Sources:
- Flexed knee impact
- Axial load through the foot
- Direct force on the greater trochanter
Types of Hip Dislocations
1. Posterior Hip Dislocation (Most Common)
- Mechanism: Force on flexed knee (dashboard injury)
- Limb position:
- Flexion
- Adduction
- Internal rotation
Associated Injuries:
- Posterior acetabular fractures
- Sciatic nerve injury
2. Anterior Hip Dislocation
- Mechanism: Abduction + external rotation
Subtypes:
- Inferior (Obturator): flexion + abduction
- Superior (Pubic/Iliac): extension + abduction
- Limb position:
- External rotation
- Abduction
- Mild flexion
Symptoms and Clinical Presentation
Patients typically present with:
- Severe hip pain
- Inability to move the leg
- Visible deformity
Classic Positions:
- Posterior: shortened, internally rotated limb
- Anterior: externally rotated, abducted limb
Clinical Evaluation
Because of high-energy trauma, always perform a full trauma assessment.
Important Assessments:
- Neurovascular exam:
- Sciatic nerve (especially peroneal branch)
- Look for:
- Pelvic fractures
- Femur fractures
- Spine injuries
Imaging and Diagnosis
Initial Imaging:
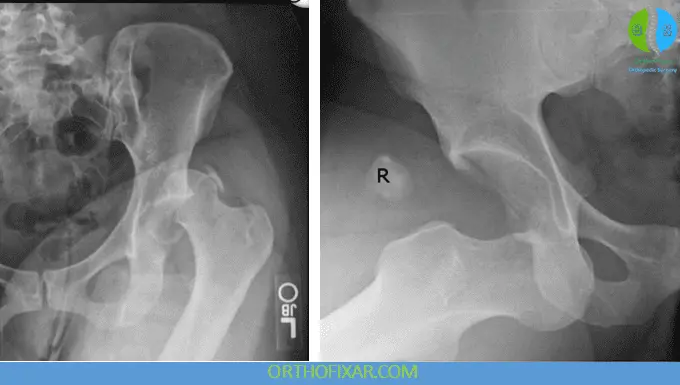
- X-ray pelvis (AP view)
- Cross-table lateral view
Key Findings:
- Posterior dislocation → femoral head appears smaller
- Anterior dislocation → femoral head appears larger
- Disruption of Shenton’s line
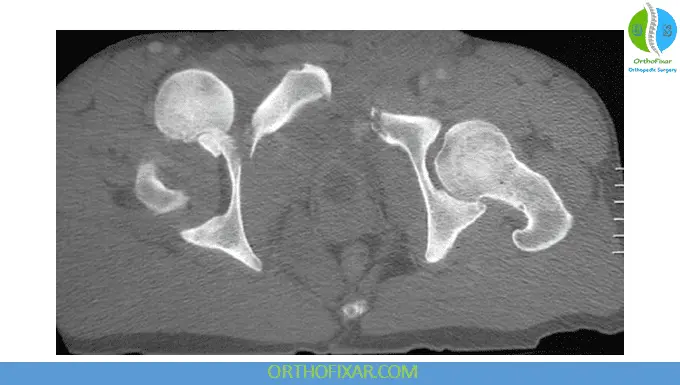
Advanced Imaging:
- CT scan (post-reduction):
- Detect fractures
- Evaluate joint congruency
- MRI (select cases):
- Labral injury
- Vascular status of femoral head
Classification Systems
Posterior Dislocations (Thompson & Epstein)
- Type I → Simple dislocation
- Type II–III → Posterior wall fractures
- Type IV → Acetabular floor fracture
- Type V → Femoral head fracture
Anterior Dislocations (Epstein)
- Type I → Superior
- Type II → Inferior
- Subtypes based on associated fractures
Emergency Treatment
🚨 Hip dislocation is an orthopedic emergency. Reduction should occur ASAP—ideally within 6 hours.
Delayed reduction (>12 hours) significantly increases risk of osteonecrosis.
Closed Reduction Techniques
Usually performed under general anesthesia or sedation.
Common Methods:
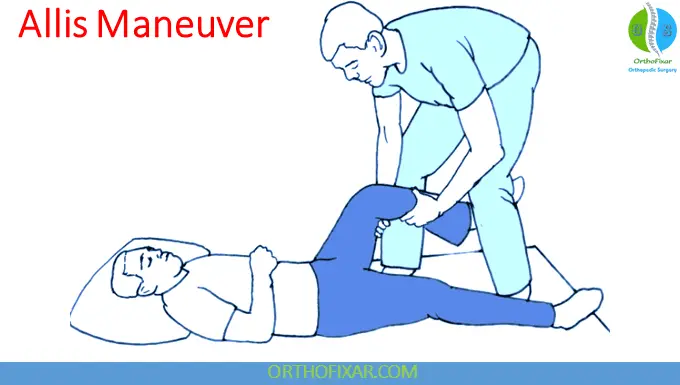
1. Allis Technique (Most Used)
- Patient supine
- Inline traction + gradual hip flexion
- Assistant stabilizes pelvis
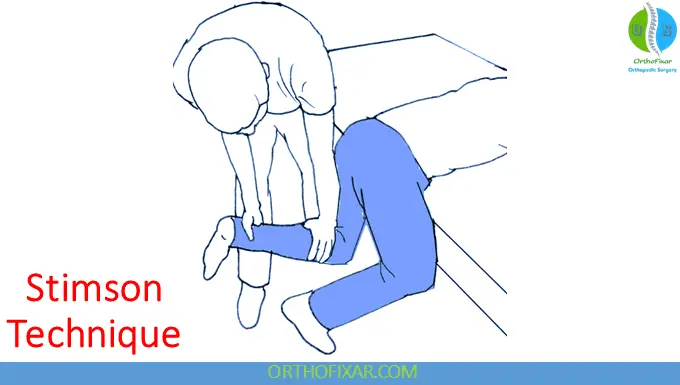
2. Stimson Technique
- Patient prone
- Gravity-assisted reduction
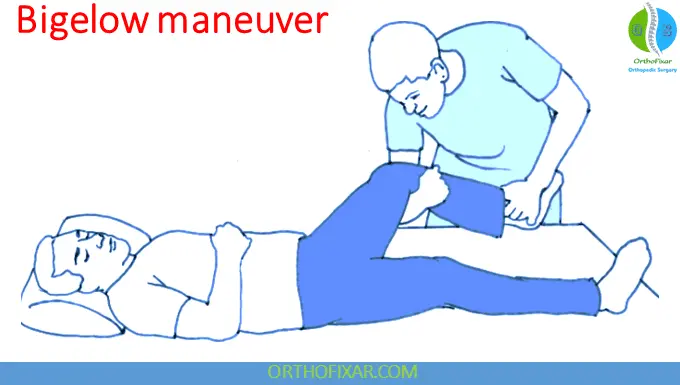
3. Bigelow Maneuver
- Less commonly used (risk of complications)
A successful reduction often produces a “clunk” sound.
Open Reduction (Surgery)
Indicated when:
- Closed reduction fails
- Nonconcentric reduction
- Associated fractures
- Femoral neck fracture
Surgical Approaches:
- Posterior (Kocher-Langenbeck)
- Anterior (Smith-Petersen)
- Anterolateral (Watson-Jones)
Post-Reduction Management
- Confirm with imaging (X-ray + CT)
- Assess joint stability
Rehabilitation:
- Stable hip → partial weight bearing for 4–6 weeks
- Unstable → surgical intervention
Prognosis
- 70–80% good outcomes in simple posterior dislocations
- Worse prognosis with:
- Delayed reduction
- Associated fractures
Complications
1. Osteonecrosis (Avascular Necrosis)
- Occurs in 5–40%
- Risk increases with delayed reduction
2. Post-Traumatic Arthritis
- Most common long-term complication
3. Sciatic Nerve Injury
- Occurs in 10–20%
- Often affects peroneal division
4. Recurrent Dislocation
- Rare (<2%)
5. Heterotopic Ossification
- Occurs in ~2%
6. Thromboembolism
- Requires prophylaxis
Key Takeaways
- Hip dislocation = medical emergency
- Usually caused by high-energy trauma
- Posterior dislocations are most common
- Early reduction is crucial to prevent complications
- Long-term outcomes depend on timing and associated injuries
References & More
- Dawson-Amoah K, Raszewski J, Duplantier N, Waddell BS. Dislocation of the Hip: A Review of Types, Causes, and Treatment. Ochsner J. 2018 Fall;18(3):242-252. doi: 10.31486/toj.17.0079. PMID: 30275789; PMCID: PMC6162140. Pubmed
- Masiewicz S, Mabrouk A, Johnson DE. Posterior Hip Dislocation. [Updated 2023 Jul 31]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: Pubmed
- Graber M, Marino DV, Johnson DE. Anterior Hip Dislocation. [Updated 2023 Jul 25]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: Pubmed
- Egol KA. Handbook of fractures. 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2019.