Femoral neck fractures are a subset of intracapsular hip fractures and represent a major clinical problem, particularly in the elderly population. They are associated with high morbidity, mortality, and healthcare burden, making early diagnosis and appropriate management essential.
Epidemiology
- Over 250,000 hip fractures occur annually in the United States, with approximately 50% involving the femoral neck.
- Incidence is expected to double by 2050, driven by aging populations.
- 80% occur in women, largely due to osteoporosis.
- Bimodal distribution:
- Young patients: High-energy trauma (e.g., motor vehicle accidents)
- Elderly (mean age ~72 years): Low-energy falls
- Incidence rates:
- Women: 63.3 per 100,000 person-years
- Men: 27.7 per 100,000 person-years
Risk Factors
- Advanced age
- Female sex
- Osteoporosis / low estrogen
- Prior fractures
- Smoking and alcohol use
- Poor general health
- History of falls
Anatomy
Understanding femoral neck anatomy is crucial for predicting fracture behavior and healing potential.
- Neck-shaft angle: 130° ± 7°
- Femoral anteversion: 10° ± 7°
- Minimal periosteum → healing relies on endosteal bone formation
- Calcar femorale: Key structural support from posteromedial femoral shaft
Ligamentous Attachments
- Iliofemoral ligament (Y-ligament of Bigelow)
- Pubofemoral ligament
- Ischiofemoral ligament
Biomechanics
- One-legged stance: ~2.5× body weight
- Trabecular alignment reflects stress distribution:
- Vertical → weight-bearing forces
- Horizontal → abductor forces
See Also: Hip Joint Anatomy
Mechanism of Injury
Low-Energy Trauma (Most Common)
- Falls in elderly patients
- Direct impact on greater trochanter
- External rotation forces
High-Energy Trauma
- Motor vehicle accidents
- Falls from height
Stress Fractures
- Athletes, military recruits, dancers
- Due to repetitive loading
Insufficiency Fractures
- Osteoporotic bone failure under normal stress
See Also: Femoral Stress Fracture
Clinical Evaluation
Typical Presentation
- Displaced fractures:
- Shortened limb
- External rotation deformity
- Inability to bear weight
- Nondisplaced/stress fractures:
- Groin pain
- Pain with axial loading
- May still ambulate
Key Clinical Points
- Pain with hip motion and axial compression
- Always assess for associated injuries in trauma cases
- Detailed history is essential (falls, syncope, prior hip pain)
Radiographic Evaluation
Standard Imaging
- AP pelvis
- AP + cross-table lateral hip
Important: Avoid frog-leg lateral (risk of displacement)
Advanced Imaging
- MRI (gold standard): Detects occult fractures
- CT scan: Useful in trauma settings
- Bone scan: Alternative if MRI contraindicated
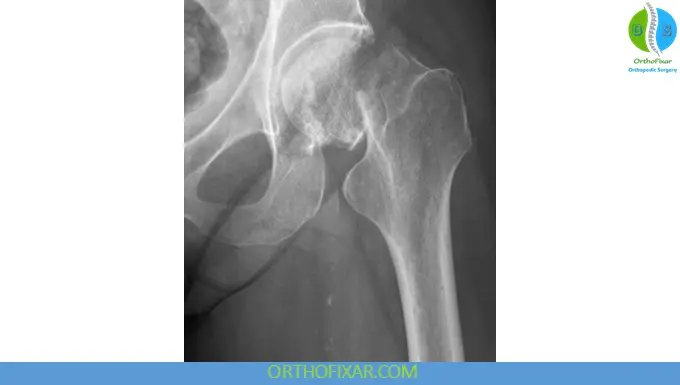
Classification Systems
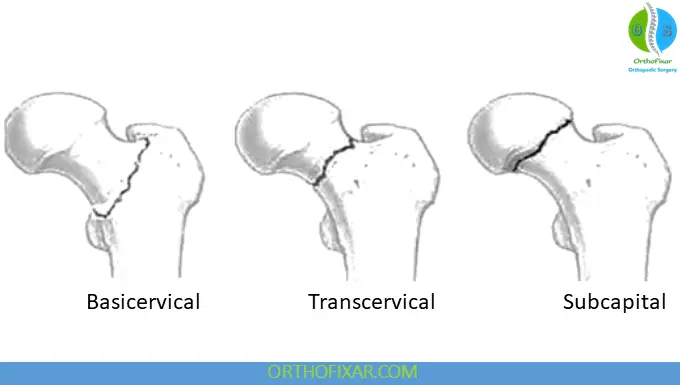
1. Anatomic Classification
- Subcapital (most common)
- Transcervical
- Basicervical
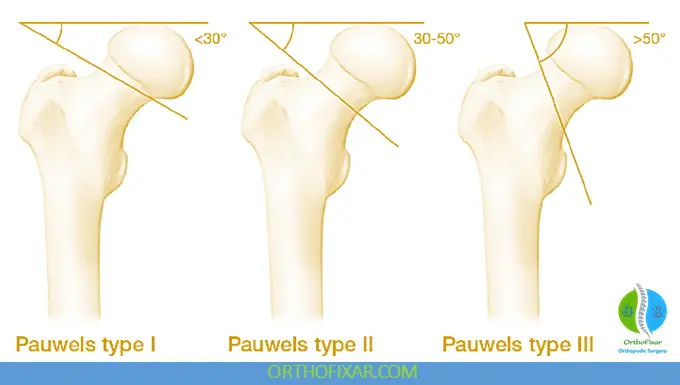
2. Pauwels Classification (Biomechanical)
Based on fracture angle:
- Type I, with fracture line inclination from 0° to 30°;
- Type II, with inclination of 30° to 50°;
- Type III, with inclination of 50° and greater.
Higher angle → increased shear forces → worse healing
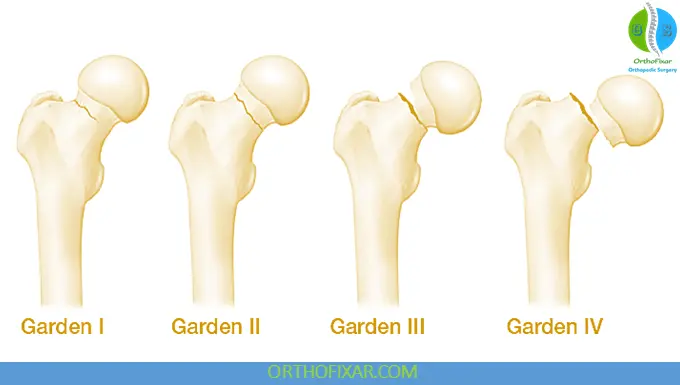
3. Garden Classification (Displacement)
- Type I: Incomplete / valgus impacted
- Type II: Complete, nondisplaced
- Type III: Partially displaced
- Type IV: Completely displaced
Clinical Simplification
- Nondisplaced fractures: Better prognosis
- Displaced fractures: Higher risk of complications
Femoral Neck Fracture Treatment
Goals
- Pain control
- Early mobilization
- Restoration of function
- Prevention of complications
Nonoperative Management
- Reserved for:
- Medically unfit patients
- Nonambulatory individuals
- Requires early mobilization to prevent:
- Atelectasis
- DVT
- Pressure ulcers
Operative Management
1. Stress Fractures of the Femoral Neck
- Tension side: Surgical fixation
- Compression side: Conservative unless symptomatic
2. Nondisplaced Femoral Neck Fractures
- In situ fixation with 2–3 cancellous screws
- Risk of osteonecrosis: 5–15%
3. Displaced Femoral Neck Fractures
Young Patients
- Urgent reduction + internal fixation (ORIF)
- Aim: preserve femoral head
Elderly Patients
- High-demand patients:
- Total hip replacement (THR) preferred
- Low-demand patients:
- Hemiarthroplasty
- Severely ill:
- Consider nonoperative or palliative surgery
Surgical Techniques
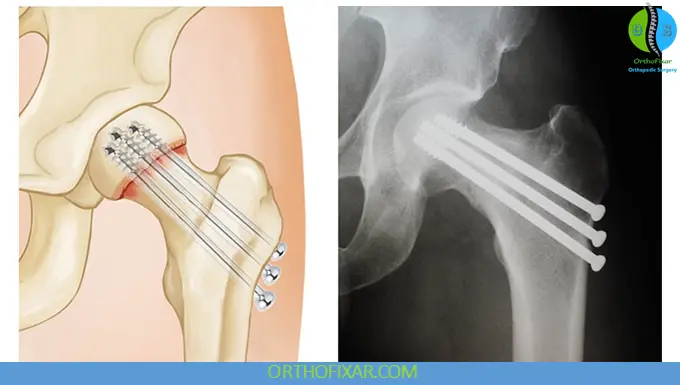
Internal Fixation
- 3 parallel screws (inverted triangle configuration)
- Avoid inferior screw placement below lesser trochanter
Sliding Hip Screw
- Useful for high Pauwels angle fractures
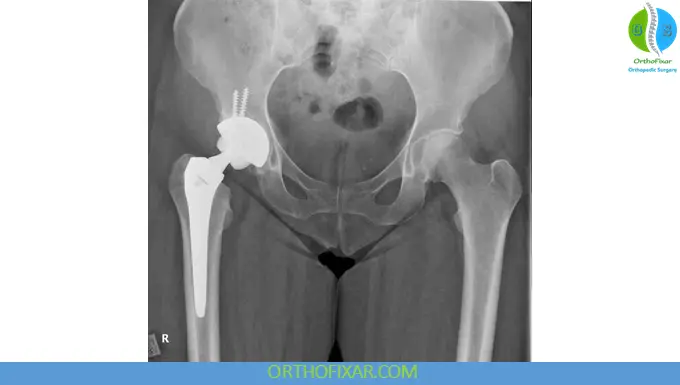
Arthroplasty Options
| Type | Advantages | Disadvantages |
|---|---|---|
| Hemiarthroplasty | Less invasive | Acetabular wear |
| Total Hip Replacement | Better function | Higher dislocation risk |
Complications
1. Nonunion
- Up to 25% in displaced fractures
- Presents with persistent pain
2. Osteonecrosis (Avascular Necrosis)
- Up to 30% in displaced fractures
- Due to disrupted blood supply
3. Fixation Failure
- Common in osteoporotic bone
4. Prosthetic Complications
- Dislocation (1–2%)
- Implant loosening
Prognosis
- Strongly dependent on:
- Age
- Fracture displacement
- Timing of surgery
- Early surgery (<24–48 hours) improves outcomes
Key Clinical Pearls
- Always suspect occult Femoral Neck Fracture in elderly with hip pain
- MRI is the gold standard when X-rays are negative
- Displacement determines prognosis and treatment
- Arthroplasty is increasingly preferred in elderly patients
Final Thoughts
Femoral neck fractures remain a high-impact orthopedic injury, particularly in aging populations. Management decisions must be individualized based on patient age, fracture type, and functional demands. Early intervention and appropriate surgical selection are critical to improving outcomes and reducing complications.
References & More
- Kazley J, Bagchi K. Femoral Neck Fractures. [Updated 2023 May 8]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: Pubmed
- Rogmark C, Viberg B, Wolf O, Mukka S, Costa ML, Gjertsen JE. An Acta Orthopaedica educational article: Femoral neck fractures in adults with emphasis on surgical treatment. Acta Orthop. 2025 Aug 18;96:632-639. doi: 10.2340/17453674.2025.44354. PMID: 40823707; PMCID: PMC12359207. Pubmed
- Hayat Z, Tiwari V, Varacallo MA. Surgical Management of Femoral Neck Fractures. [Updated 2024 May 1]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: Pubmed
- Egol KA. Handbook of fractures. 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2019.