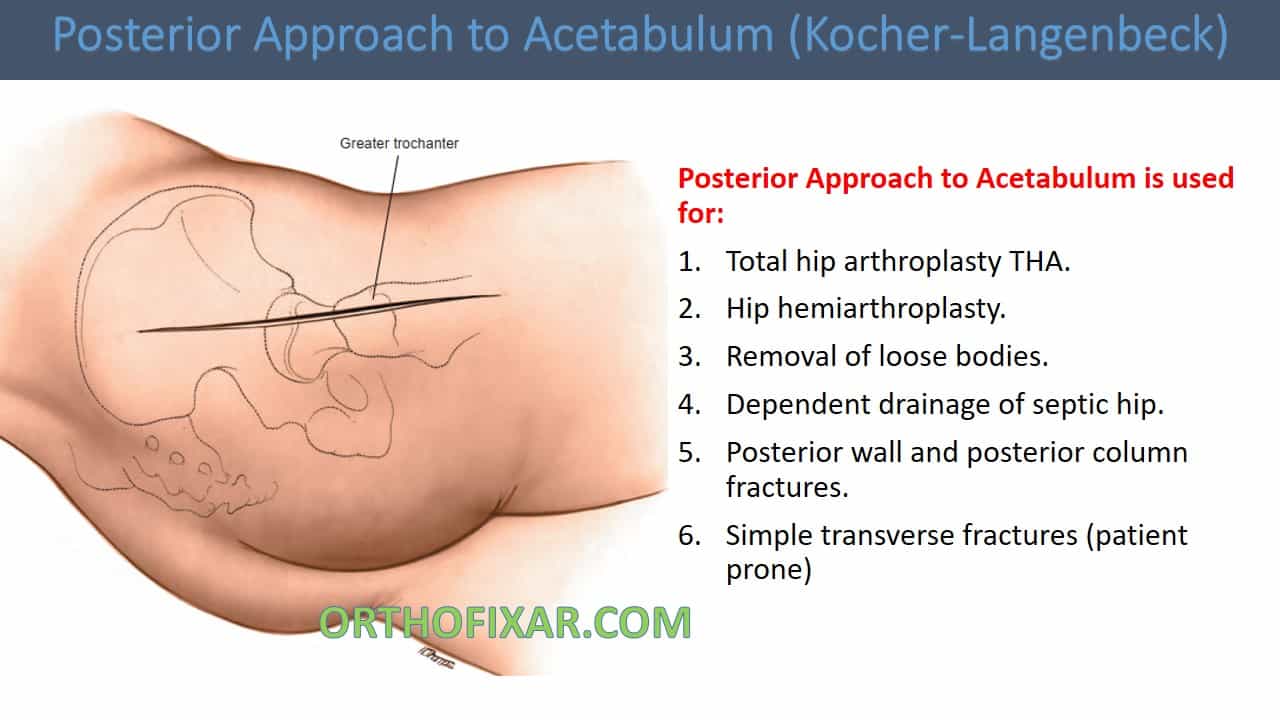
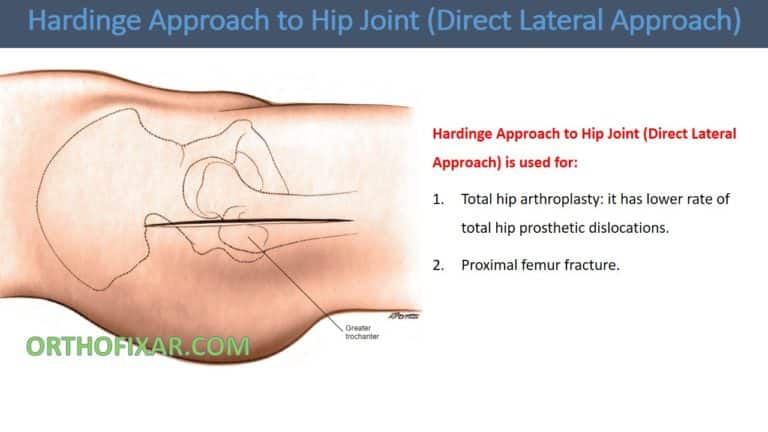
The posterior approach to acetabulum or as called (Kocher-Langenbeck approach) gives access to the posterior wall of the acetabulum and its posterior column.
- It also allows direct visualization of the dorsocranial part of the acetabulum, either through the fracture gap or via a capsulotomy.
Posterior Approach to Acetabulum is used for:
- Total hip arthroplasty THA.
- Hip hemiarthroplasty.
- Removal of loose bodies.
- Dependent drainage of septic hip.
- Posterior wall and posterior column fractures.
- Simple transverse fractures (patient prone):
- Fractures must be less than 15 days old.
- Fractures line located at or below acetabular roof.
- No major anterior displacement.
The Kocher-Langenbeck approach is the easiest of all acetabular approaches, and extensive blood loss is not usually encountered.
Position of the Patient
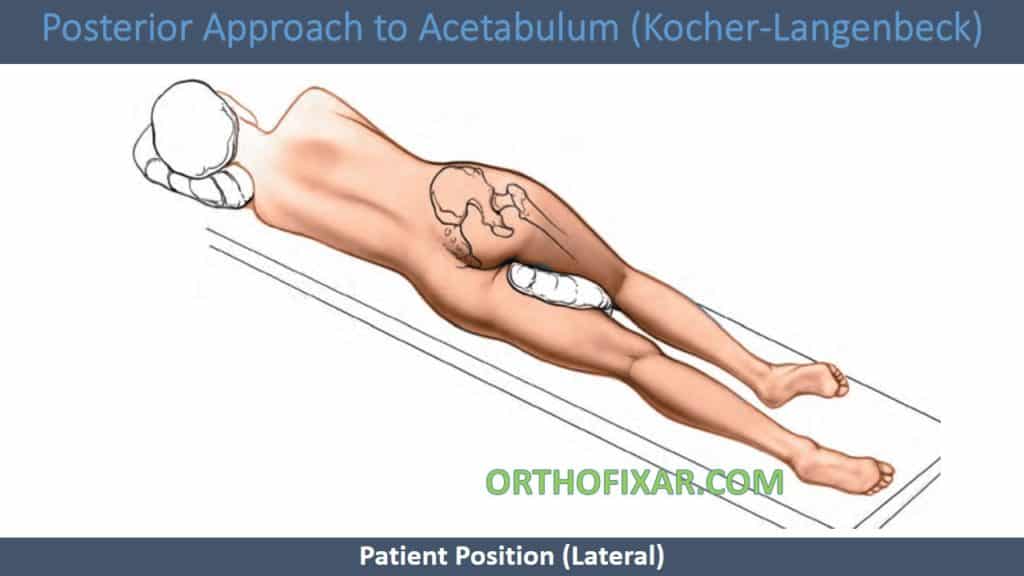
Lateral position:
- Posterior wall and lip fractures (can use skeletal traction when using lateral position).
- Allows for femoral head dislocation.
- Position of choice for joint arthroplasty.
- Allows buttock tissue to “fall away” from the field.
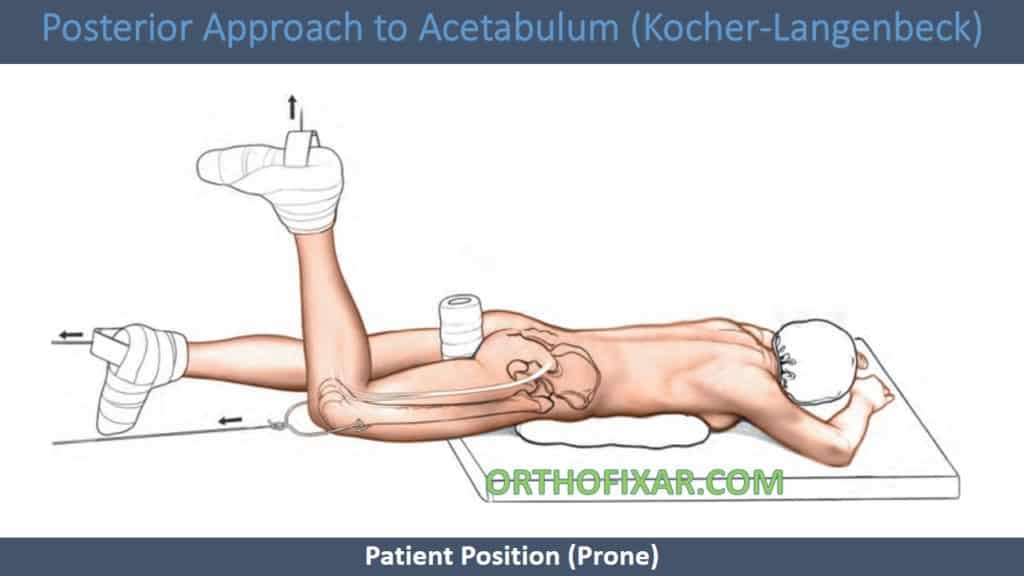
Prone position:
- For transverse fractures (flex the knee to prevent stretching of sciatic nerve).
- Femoral head is maintained in reduced position throughout procedure.
- Improves quadrilateral surface access.
- Improved access to cranial and anterior aspect of posterior wall fractures.
Landmarks and Incision
- Landmarks:
- The greater trochanter.
- Incision:
- Make a longitudinal incision centered on the greater trochanter extending from just below the iliac crest to 10 cm below the tip of the greater trochanter.

Internervous plane
- There is no true internervous plane in the posterior approach to acetabulum.
- The gluteus maximus that is split in the line of its fibers is not significantly denervated because it receives its nerve supply well proximal to the split.
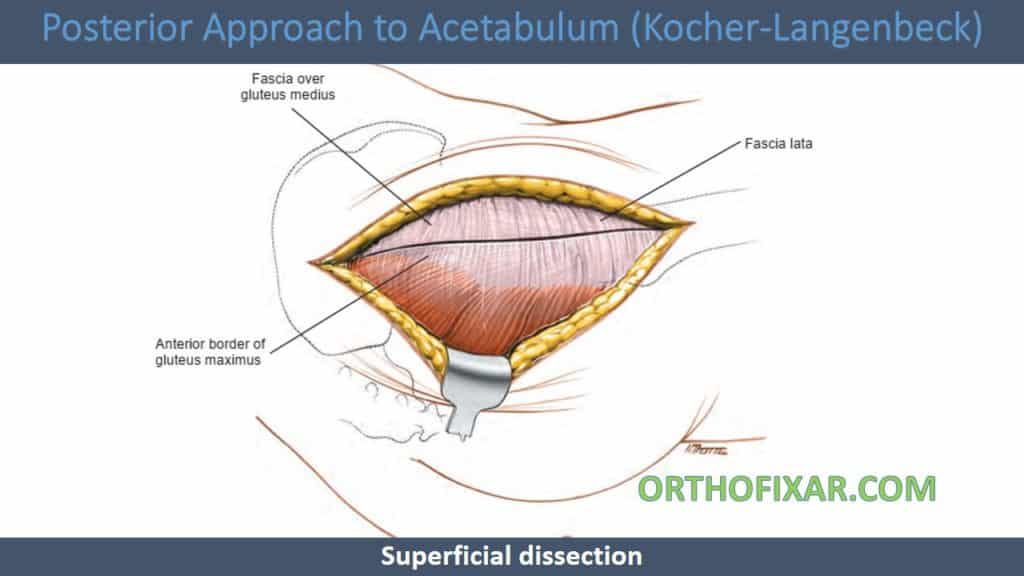
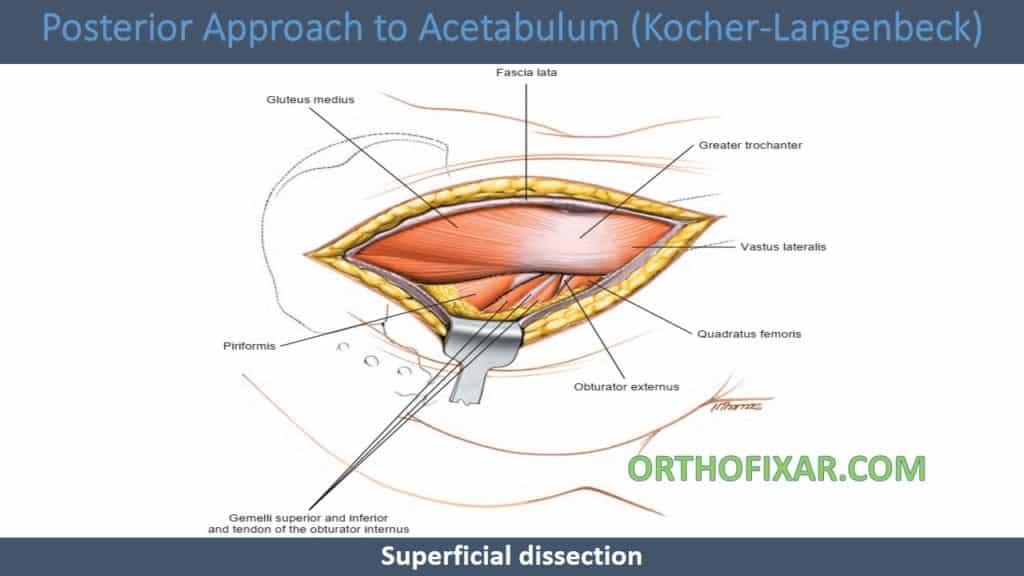
Superficial dissection
- Deepen the incision through subcutaneous fat.
- Incise the fascia lata in the line of the skin incision in the lower half of the wound, and extend this incision superiorly along the anterior border of the gluteus maximus muscles.
- Retract the split edges of the fascia to reveal the piriformis muscle and the short external rotators of the hip.
- Partial detachment of the insertion of gluteus maximus muscle from the femur will facilitate mobilization of this muscle.
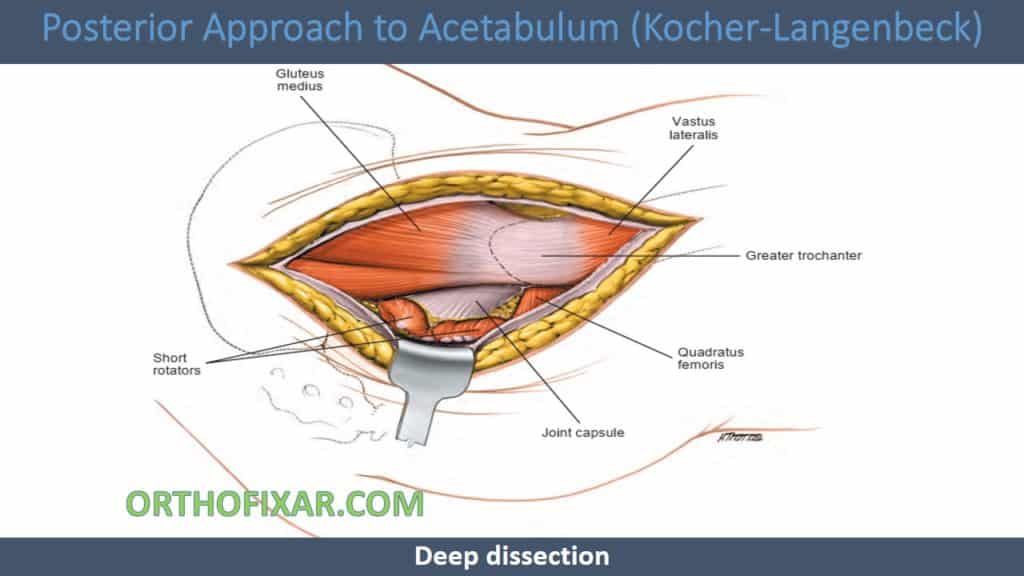
Deep dissection
- Internally rotate the leg to put the short external rotators and the piriformis on the stretch and detach these muscles as they insert into the femur.
- Using the short external rotator muscles as a cushion, carefully insert a retractor into the greater sciatic notch (Do not apply great pressure on this retractor as this will create a sciatic nerve palsy).
- Insert a second retractor into the lesser sciatic notch to expose the posterior column in its whole extent.
- The posterior capsule of the hip is revealed (This is often torn or detached in cases of trauma).
- If the posterior capsule is intact and a direct inspection of the joint is required, make a T-shaped capsulotomy (Ensure that you avoid damage to the limbus when incising the capsule).
- The inner surface of the acetabulum can only be viewed by distracting the femoral head (This can either be achieved by skeletal traction or with the help of a Schanz screw placed in the femoral head).
- Posterior lip fractures of the acetabulum can be adequately visualized and fixed at this stage.
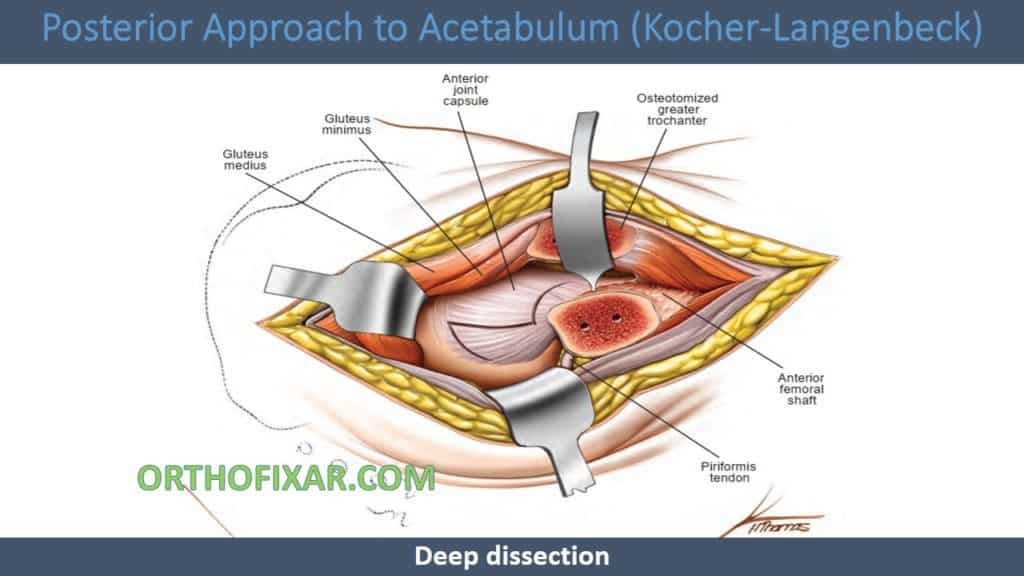
- If you require more extensive exposure of the posterior column, perform an osteotomy of the greater trochanter.
- Divide the greater trochanter from posterior to anterior, removing a piece of bone 5 mm in size. This bone will have the gluteal muscles attached to it superiorly and the vastus lateralis attached to it inferiorly.
- Progressively evert the trochanter with its attached muscles over the anterior surface of the femur using a sharp retractor. The small remaining attachment of gluteus medius to the intertrochanteric ridge will now need to be released.
- If difficulty is encountered mobilizing the fragment, the insertion of piriformis may sometimes need to be partially released.
- If you require access to the anterior surface of the hip joint capsule, flex and externally rotate the hip. Mobilize the insertion of gluteus minimus from the retroacetabular surface along the superior capsule to its femoral insertion along the anterior aspect of the trochanter.
- If further exposure of the anterior capsule is required, mobilize the proximal portion of the vastus intermedius from the femur to allow access to the anterior hip joint capsule.
- This trochanteric fragment can be reattached easily with screws during closure.
- Note that trochanteric osteotomies are associated with heterotopic bone formation in acetabular surgery

Approach Extension
Proximal Extension:
- The posterior approach to acetabulum (Kocher-Langenbeck approach) can be extended distally down to the level of the knee.
- Either split the vastus lateralis or elevate it from the lateral intermuscular septum to allow exposure of the lateral surface of the entire shaft of the femur.
Distal Extension:
- The posterior approach to acetabulum (Kocher-Langenbeck approach) cannot be usefully extended proximally.
Dangers
The structures at risk during posterior approach to acetabulum (Kocher-Langenbeck approach) include:
- Sciatic nerve:
- Extend hip and flex knee to prevent injury.
- Minimize chance of injury by using proper gentle retraction and releasing your short external rotators (obturator internus) posteriorly to protect the sciatic nerve from traction.
- Inferior gluteal artery.
- First perforating branch of profunda femoris.
- Femoral vessels.
- Superior gluteal artery and nerve.
References
- Surgical Exposures in Orthopaedics book – 4th Edition
- Campbel’s Operative Orthopaedics book 12th