Metatarsus Adductus is a postural deformity in which the children are born with inward deviation of the forefoot relative to the hindfoot.
The Metatarsus Adductus deformity may be very mild and resolve spontaneously, it may be slightly fixed and persist to walking age, or it may be rigid and associated with valgus of the hindfoot.
Other terms of metatarsus adductus include:
- A third of a clubfoot,
- hook-foot,
- bean-shaped foot,
- serpentine foot,
- congenital metatarsus adductus,
Skewfoot has been used to describe feet with fixed hindfoot valgus and subluxation of the midfoot.
Wynne-Davies found an incidence of metatarsus varus of 1 in 1000 births and reported that if 1 child were affected, the risk of deformity in a second child in the same family was 1 in 20.
Widhe and associates noted foot abnormalities in 4% of the infants, with 1% having metatarsus adductus.
See Also: Foot Anatomy
Metatarsus Adductus Causes
It has long been presumed, but never proved, that intrauterine compression produces metatarsus adductus. Metatarsus Adductus is associated with torticollis and developmental dislocation of the hip to some degree; but unlike DDH, it is not related to birth order.
The incidence of ultrasonographic or clinical hip instability in children with metatarsus adductus has been reported to be as high at 1 in 25.
Pathology
The shape of the medial cuneiform is altered, with medial deviation of the articular surface. There was also adduction of the metaphyses of the second through the fifth metatarsals. No joint subluxations or tendon abnormalities were noted.
Based on findings after dissection of stillborn infant feet, Reimann and Werner concluded that the primary abnormality was medial subluxation of the tarsometatarsal joints in utero when the foot was in a dorsiflexed position.
Clinically
The deformity is usually noted at birth, but it may initially be recognized at any age.
The clinical hallmark of the condition is medial deviation of the forefoot relative to the hindfoot:
- When the foot is viewed from the dorsal surface: the entire foot often appears to be turned inward.
- When the foot is viewed from the plantar surface: the sole of the foot has the shape of a bean.
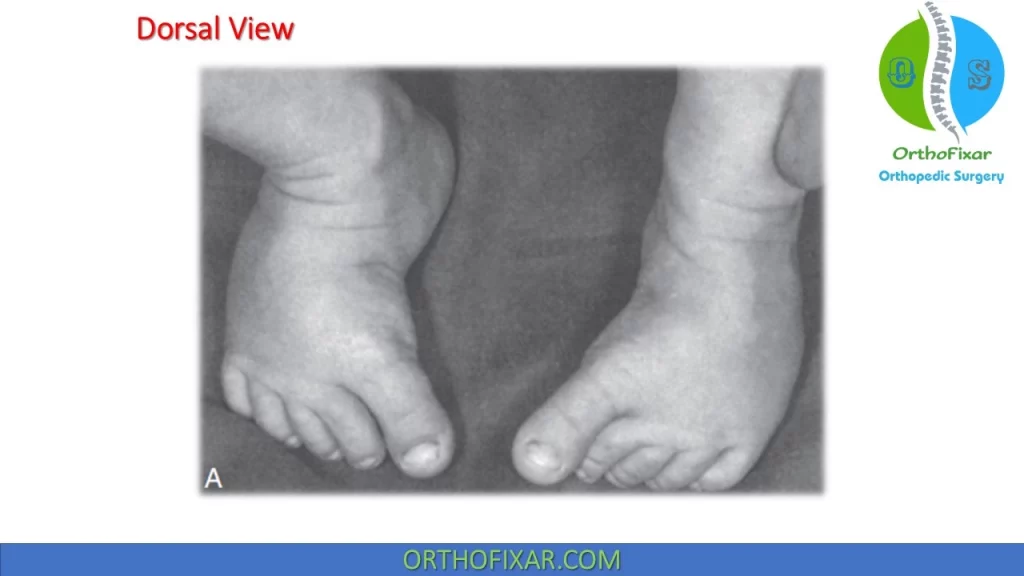
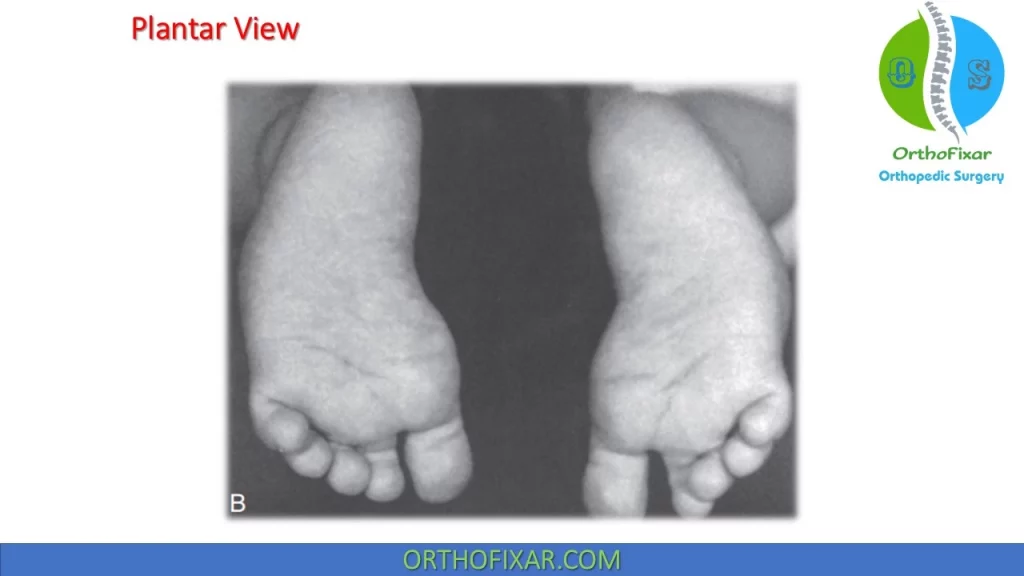
The base of the fifth metatarsal is usually prominent and the arch frequently appears higher than normal. In addition, the space between the first and second toes is wider than normal, and the first toe seems to be reaching medially.
The full extent of the deformity can be best appreciated when the examiner grasps the heel and compares the alignment of the heel with that of the forefoot. Although it is not seen on a casual examination, careful evaluation of the hindfoot reveals slight valgus of the heel.
It is important to establish the degree of flexibility of the metatarsus adductus deformity:
- In mild cases the foot will correct actively when the lateral border of the foot is stimulated.
- In less flexible cases the foot will not correct actively but can easily be corrected passively. The examiner should maintain the hindfoot in neutral during this maneuver, grasp the heel with one hand, and with the web space of the hand placed against the head of the first metatarsal, push the foot laterally. A gentle push will align the metatarsals in most children.
- A rigid deformity has a medial soft tissue crease at the tarsometatarsal level and a medial soft tissue contracture that prevents passive correction of the foot. As the forefoot is abducted, a tight abductor hallucis can be palpated medially.
Many of these children will also have internal tibial torsion, which will contribute to an intoed appearance. This is the most common parental complaint, and this component of the deformity should be noted separately.
Characteristic Features of Metatarsus Adductus
Kite listed six characteristic features of the disorder:
- Spontaneous active medial deviation of the foot by the child.
- High arch.
- Concave medial border of the foot.
- Separation of the first and second toes.
- Fixed adductus of the forefoot when the hindfoot is held in neutral.
- Bean-shaped sole of the foot.
Metatarsus Adductus Grading
Bleck Classification for Metatarsus Adductus:
Bleck method is based on the heel bisector line, normally, the heel bisector should align with the web space between the second and third toes.
- Normal: heel bisector line through 2nd and 3rd toe webspace.
- Mild: heel bisector line through 3rd toe.
- Moderate: heel bisector through 3rd and 4th toe webspace.
- Severe: heel bisector through 4th and 5th toe webspace.

Berg Classification:
| Simple Metatarsus Adductus | Metatarsus Adductus alone |
| Complex Metatarsus Adductus | Metatarsus Adductus + lateral shift of midfoot |
| Skew foot | Metatarsus Adductus + valgus hindfoot |
| Complex skew foot (serpentine foot) | Metatarsus Adductus + lateral shift + valgus hindfoot |
Radiographic Imaging
Radiographs show medial deviation of the metatarsals at the tarsometatarsal level, with some degree of valgus of the hindfoot.
Older children with more severe forms of metatarsus adductus may have medial deformation of the metatarsal shafts.

Metatarsus Adductus Treatment
Stretching Treatment:
If the metatarsus adductus is flexible and actively corrects as the foot is stimulated, the condition does not need to be treated. These mild deformities will resolve gradually. Parents should be reassured and shown how to gently stretch the foot and how to stimulate it to actively correct.
Stretching Technique: Parents are taught to hold the heel in a neutral position with one hand and abduct the forefoot with the web space of the other hand. Some physicians also recommend that the child wear straight last shoes.
There is controversy as to whether or not the metatarsus adductus treatment is required for intermediate severity, in which the deformity does not actively correct but is easily corrected passively. Many physicians believe that these deformities will self-correct over time without intervention.
Rushforth found asymptomatic moderate deformity in 10% of children with untreated metatarsus adductus, and residual deformity and stiffness in 4% at 7-year follow-up.

Serial casting Treatment:
For a child younger than 6 months, a short series of short-leg plaster casts will easily correct the foot position, and this treatment approach may be warranted for patients with obvious deformity.
Some authors prefer long-leg bent-knee casts but reports indicate that only 10% of patients require such treatment.
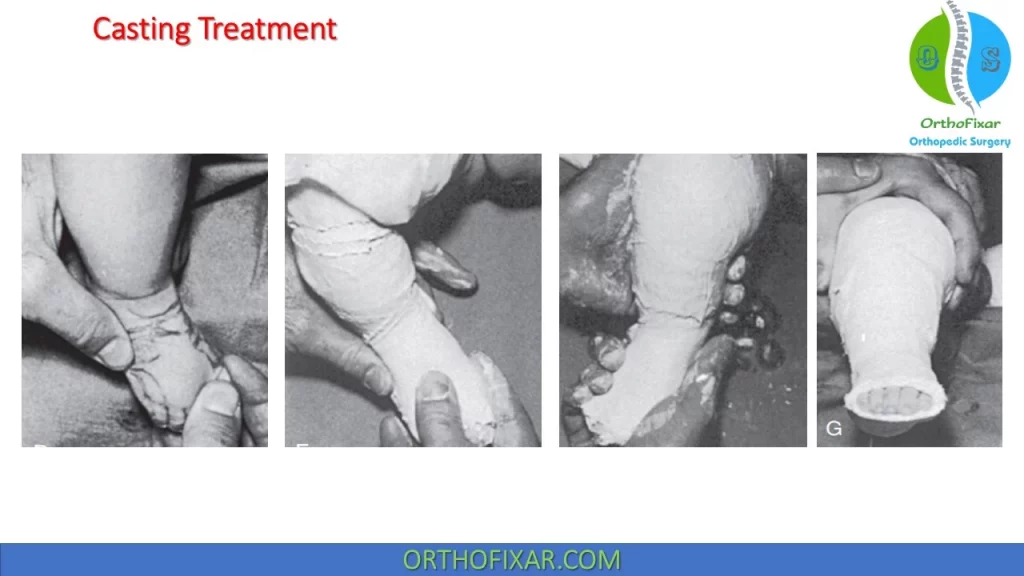
The technique of cast correction is similar to the stretching procedure taught to the parent:
- The child’s heel is grasped and held in a neutral position while the forefoot is abducted.
- The thumb of the hand holding the heel should reach the cuboid so that the fulcrum for abducting the forefoot is at the level of the cuboid metatarsal joint.
- Eversion of the foot should be avoided.
Non-rigid casts that are easily removed are preferable to rigid casting material.
Before discontinuing cast treatment, several things should be reached:
- the convexity of the lateral border of the foot should be straightened or reversed,
- the prominence of the base of the fifth metatarsal should no longer be noticeable,
- active adduction should no longer occur when the child moves the foot.
Metatarsus adductus that cannot be passively corrected should be more vigorously treated. These feet usually have significant rigidity and a medial crease with an overactive abductor hallucis. Most such feet can be corrected with serial stretching and cast application, which should be started as soon as possible.
Surgical Treatment:
If the foot is resistant to cast correction, surgical release of the abductor hallucis and capsulotomy of the first tarsometatarsal joint may be indicated, followed by further cast correction. Good results have been reported in children (3.5 years old) at an average follow-up of 3.5 years.
This procedure is recommended for treating severe adductus in children that are too young to undergo osteotomies.
Children with significant deformity who are older than 3 years may benefit from metatarsal osteotomies to realign the foot. Care must be taken, though, to avoid forcing the hindfoot into valgus and creating a skewfoot deformity.
Napiontek and others reported good results with the use of an opening wedge osteotomy of the medial cuneiform in children younger than 4 years old.
Two other surgical procedures that have been recommended for metatarsus adductus treatment are:
- Anteromedial release with capsulotomy of the medial metatarso-cuneiform and naviculo-cuneiform joints
- Transfer of the posterior tibial tendon with capsulotomy of the naviculo-cuneiform joint.
References & More
- Asirvatham R, Stevens PM. Idiopathic forefoot-adduction deformity: medial capsulotomy and abductor hallucis lengthening for resistant and severe deformities. J Pediatr Orthop. 1997 Jul-Aug;17(4):496-500. PMID: 9364391.
- Bleck EE, Minaire P: Persistent medial deviation of the neck of the talus: a common cause of in-toeing in children, J Pediatr Orthop 3:149, 1983.
- 3. Browne RS, Paton DF: Anomalous insertion of the tibialis posterior tendon in congenital metatarsus varus, J Bone Joint Surg Br 61:74, 1979.
- Giannestras NJ: Recognition and treatment of flatfeet in infancy, Clin Orthop Relat Res 70:10, 1970.
- Heyman CH, Herndon CH, Strong JM: Mobilization of the tarsometatarsal and intermetatarsal joints for the correction of resistant adduction of the fore part of the foot in congenital club-foot or congenital metatarsus varus, J Bone Joint Surg Am 40:299, 1958.
- Kite JH: Congenital metatarsus varus, J Bone Joint Surg 16:203, 1964.
- Kite JH: Congenital metatarsus varus, J Bone Joint Surg Am 49:388, 1967.
- Lincoln TL, Suen PW: Common rotational variations in children, J Am Acad Orthop Surg 11:312, 2003.
- Morcuende JA, Ponseti IV: Congenital metatarsus adductus in early human fetal development: a histologic study, Clin Orthop Relat Res 333:261, 1996.
- Napiontek M, Kotwicki T, Tomaszewski M: Opening wedge osteotomy of the medial cuneiform before age 4 years in the treatment of forefoot adduction, J Pediatr Orthop 23:65, 2003.
- Paton RW, Choudry Q: Neonatal foot deformities and their relationship to developmental dysplasia of the hip: an 11-year prospective, longitudinal observational study, J Bone Joint Surg Br 91:655, 2009.
- Ponseti IV, Becker JR: Congenital metatarsus adductus: the results of treatment, J Bone Joint Surg Am 48:702, 1966.
- Reimann I, Werner HH: Congenital metatarsus varus. A suggestion for a possible mechanism and relation to other foot deformities, Clin Orthop Relat Res 110:223, 1975.
- Rushforth GF: The natural history of hooked forefoot, J Bone Joint Surg Br 60:530, 1978.
- Stark JG, Johanson JE, Winter RB: The Heyman-Herndon tarsometatarsal capsulotomy for metatarsus adductus: results in 48 feet, J Pediatr Orthop 7:305, 1987.
- Thomson SA: Hallux varus and metatarsus varus: a five-year study (1954-1958), Clin Orthop 16:109, 1960.
- Widhe T, Aaro S, Elmstedt E: Foot deformities in the newborn– incidence and prognosis, Acta Orthop Scand 59:176, 1988.
- Wynne-Davies R: Family studies and the cause of congenital clubfoot, talipes equinovarus, talipes calcaneo-valgus and metatarsus varus, J Bone Joint Surg Br 46:445, 1964.