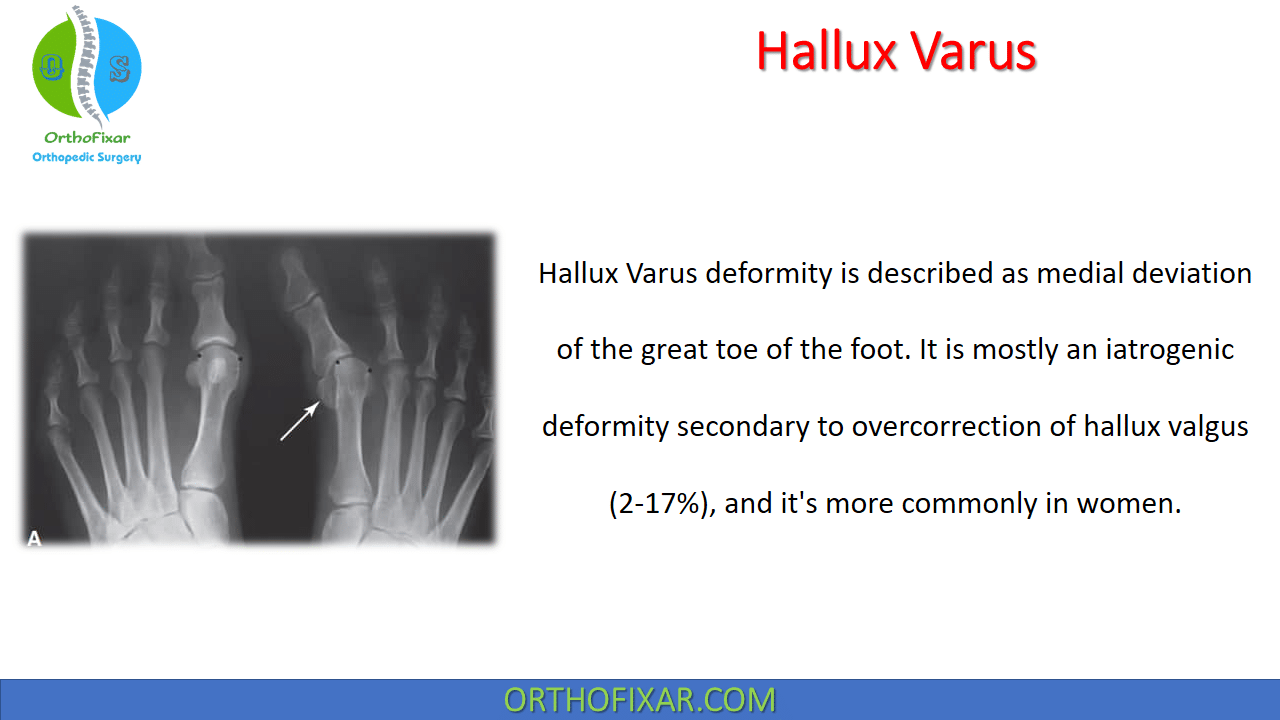
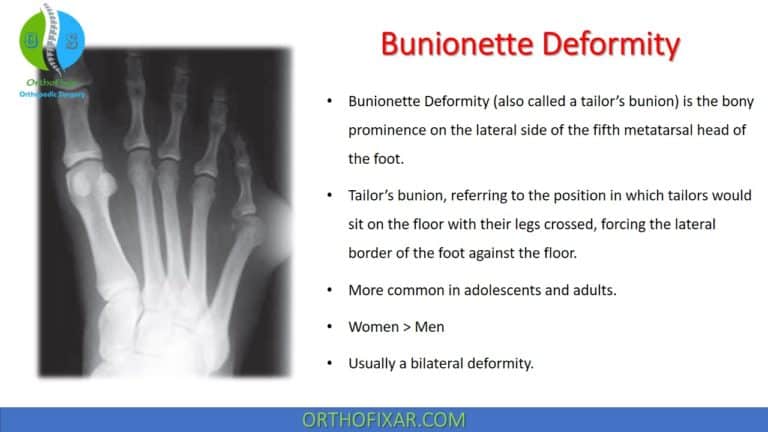
Hallux Varus deformity is a medial deviation of the great toe of the foot. It is mostly an iatrogenic deformity secondary to overcorrection of hallux valgus (2-17%), and it’s more commonly in women.
Hallux Varus Causes
Hallux Varus causes may be:
- Congenital.
- Acquired.
Acquired hallux varus may be due to:
- Iatrogenic (after hallux valgus surgery).
- trauma.
- Inflammatory (rheumatoid arthritis, ankylosis spondylitis).
- Neurological (Charcot-Marie-Tooth).
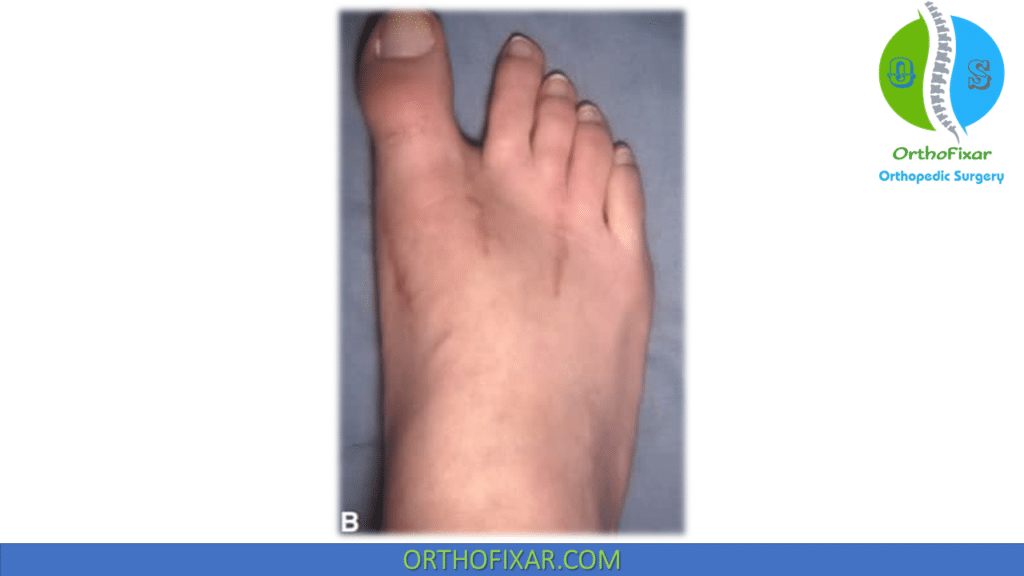
The main causes for hallux varus after hallux valgus surgery are:
- Complete release of the lateral structures of the metatarsophalangeal joint combined with excessive plication of the medial capsule.
- Excessive resection of the medial eminence, leading to loss of medial bony buttress for the proximal phalanx.
- Excision of the fibular sesamoid.
- Release of the lateral head of the flexor hallucis brevis muscle at its insertion on the fibular sesamoid.
- Closure of the intermetatarsal angle IMA to neutral or a negative value.
See Also: Anatomical Deformities in Hallux Valgus
Hallux Varus Types
Hallux varus can be classified into two types:
Static Hallux Varus:
The deformity is described as:
- Supple.
- Uniplanar.
- Passively correctable.
- It’s usually asymptomatic and mainly is a cosmetic complication.
When the foot is viewed in a weight-bearing position, the hallux rests in varus, the metatarsophalangeal joint rests in a normal position in the sagittal plane (10 degrees to the plantar surface of the foot or 20 to 25 degrees to the first metatarsal), and the interphalangeal joint is in a normal position.
Most often, the hallux is not rotated abnormally in an axial plane and does not assume a “snake-in-the-grass” appearance in the frontal plane. All the deformity occurs at the metatarsophalangeal joint, but only in the transverse or frontal plane.
Dynamic Hallux Varus
It’s also called “intrinsic minus deformity of the hallux with a varus component”. This is a true intrinsic-extrinsic muscle imbalance.
The deformity is described as:
- Multiplanar deformity.
- It’s often is fixed.
- Symptomatic.
- Difficult to correct surgically.
- In dynamic hallux varus, the first metatarsophalangeal joint is hyperextended, and the interphalangeal joint is acutely flexed.
- The hallux is rotated, and its varus and extended posture makes shoe wear difficult.
- The most common complaint is that the toe box of the shoe rubs on the dorsomedial surface of the interphalangeal joint.
The intrinsic muscles balance the hallux on the first metatarsal head, whereas the extrinsic muscles add gross balance and greatly increase the mobility of the hallux.
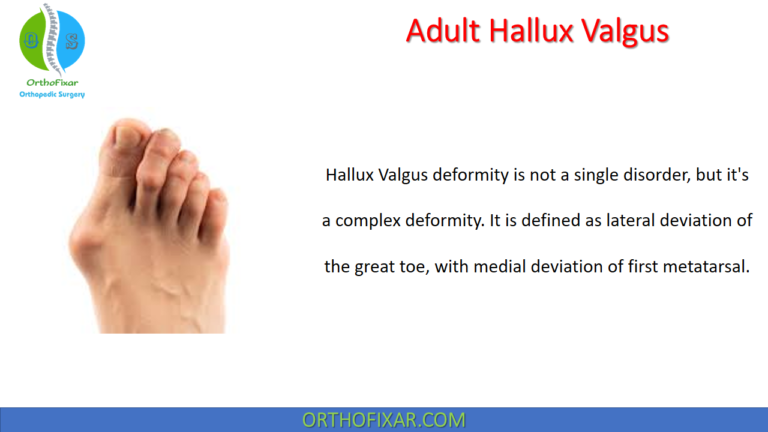
See Also: Adult Hallux Valgus
Clinical Evaluation
The deformity is often asymptomatic. The presence of pain indicates underlying joint arthritis or trauma. The patient may also complain of decreased ROM, instability, weakness with push-off during gait cycle.
Imaging Evaluation
Recommended views include weight-bearing anterior-posterior and lateral views of the foot.
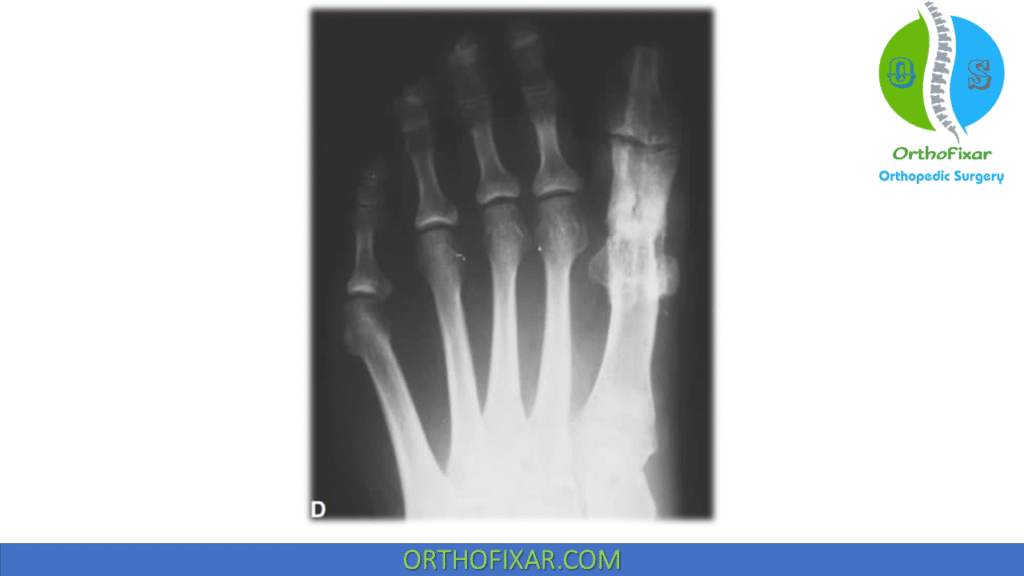
Radiographic Findings of hallux varus include:
- Hallux valgus angle HVA < 0 degrees.
- medial eminence is excessively resected.
- Reduced IMA between first and second metatarsals
- Medial subluxation of tibial seasmoid.
- Lateral seasmoid is absent.
- Degenerative changes at MTP or IP joint.
CT scan or MRI are not usually required.
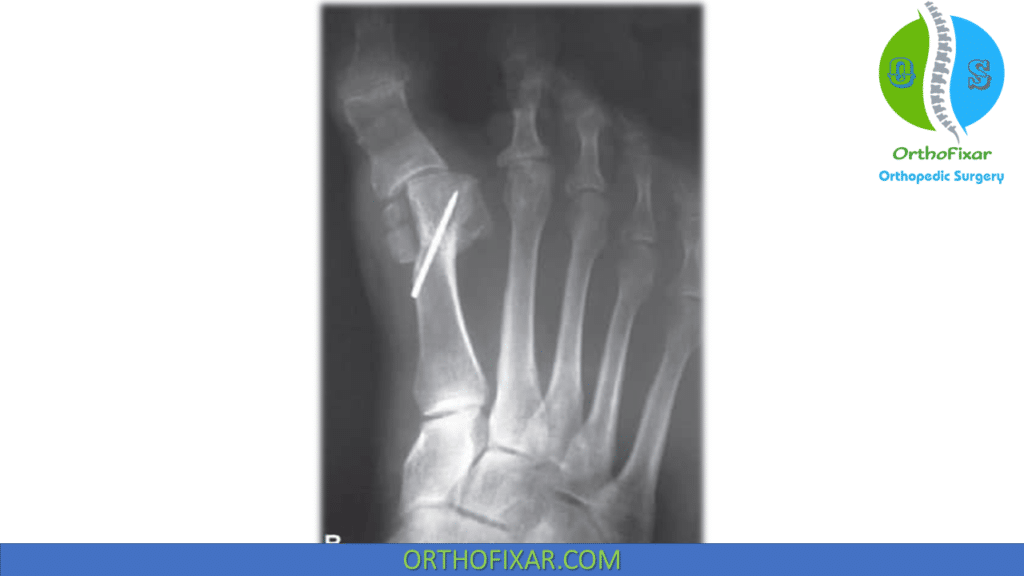
Hallux Varus Treatment
Nonoperative treatment
Nonoperative treatment of hallux varus is indicated in flexible and asymptomatic deformities. Limited to accommodation of the deformity with shoe modifications and shoe stretching.
Operative treatment
The operative treatment is based on whether the deformity is is flexible (reducible) or rigid (irreducible).
Flexible deformity:
The deformity can be corrected with a soft tissue procedure as following:
Release of abductor hallucis muscle and fascia. Transfer of a portion of extensor hallucis longus (EHL) or brevis (EHB) tendon under the transverse intermetatarsal (IM) ligament to the distal metatarsal neck (taken from lateral to medial). The distal portion of the tendon is left intact, creating a static stabilizer to correct the deformity.
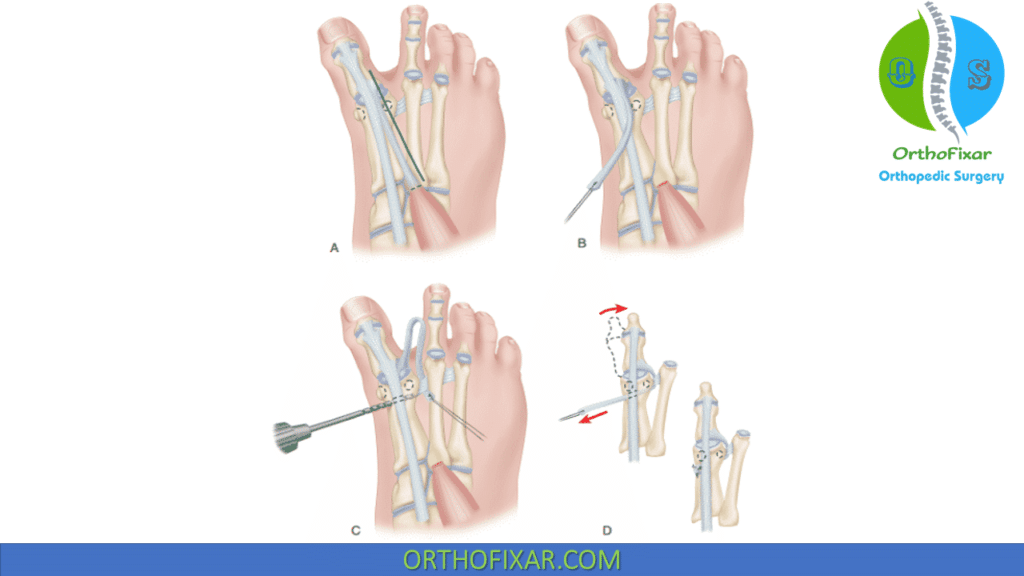
Fixed deformity:
First metatarsophalangeal joints MTP arthrodesis:
- Deformity with limited first metatarsophalangeal joints (MTP) motion.
- The presence of first MTP Degenerative joint disease (DJD).
References & More
- Campbel’s Operative Orthopaedics 12th ed Book
- Munir U, Mabrouk A, Morgan S. Hallux Varus. [Updated 2022 Sep 25]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK470261/