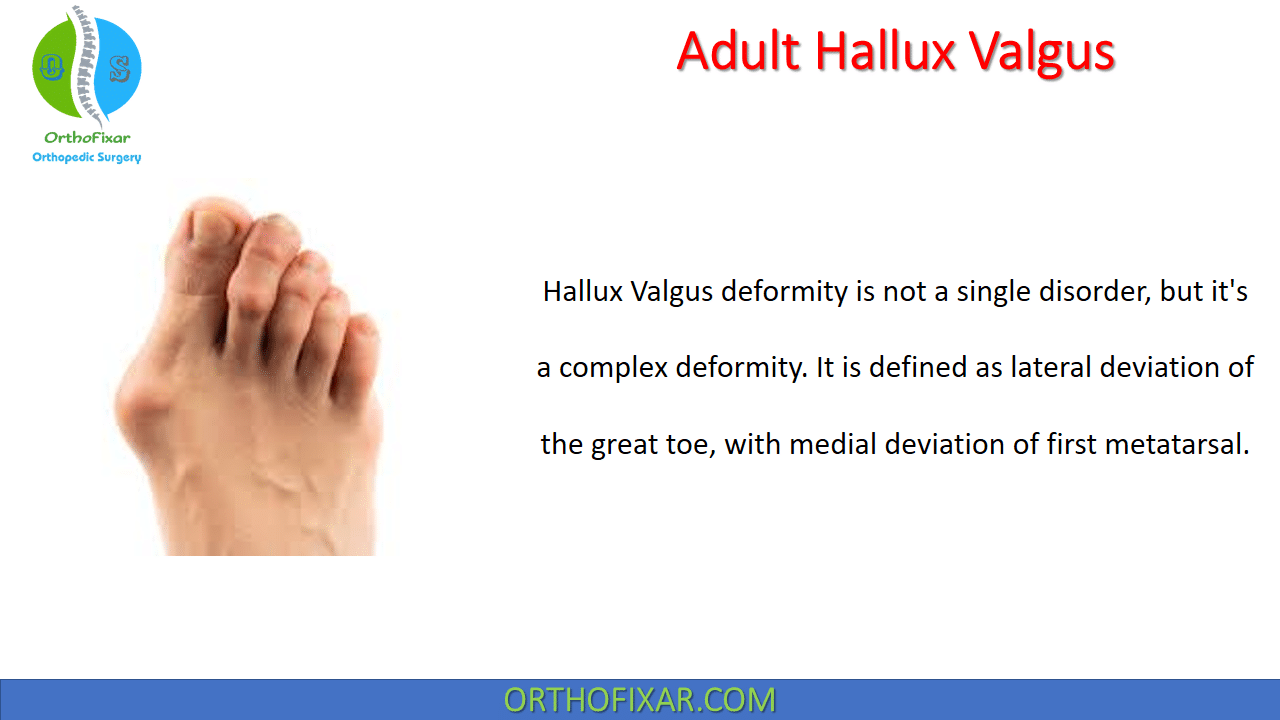
Hallux Valgus deformity is not a single disorder, but it’s a complex deformity. It is defined as lateral deviation of the great toe, with medial deviation of first metatarsal.
Hallux valgus deformity is more common in women. There’s a family history in 70 % of patients.
Risk factors
Risk factors for developing Hallux Valgus deformity include intrinsic and extrinsic factors.
Intrinsic factors include:
- Genetic predisposition,
- Ligamentous laxity,
- Predisposing anatomy (convex metatarsal head, pes planus).
- Rheumatoid arthritis.
- Cerebral palsy..
Extrinsic factors include:
- Certain types of shoe wear (narrow toe box, high heels) also play a role.
Deformities in hallux valgus
Many deformities are found in hallux valgus, these include:
- Medial capsular becomes attenuated and stretched.
- Proximal phalanx drifts laterally, leading to the following conditions:
- Plantar-lateral migration of abductor hallucis; change in position causes the muscle to plantar flex and pronate the hallux.
- Stretching of the extensor hood of the extensor hallucis longus.
- Lateral deviation of the extensor hallucis longus and flexor hallucis longus (FHL), causing a muscular imbalance and deforming force for valgus progression and pronation of the great toe.
- First metatarsal head moves medially off the sesamoids because of the unopposed pull of the adductor hallucis.
- Secondary contracture of the lateral capsule, adductor hallucis, lateral metatarsal-sesamoid ligament and intermetatarsal ligament.
- Flattens of the sesamoid ridge on the plantar surface of the first metatarsal head (the crista) because of pressure (abutment) from the tibial sesamoid.
- The valgus posture of the great toe frequently causes hammer toe–like deformity of the second toe.
The entire spectrum of hallux valgus is: varus deformity of the first metatarsal, valgus of the great toe, bunion formation, arthritis of the first metatarsophalangeal joint, hammer toe of one or more toes, corns, calluses, and metatarsalgia.
Anatomy
See Foot anatomy.
Clinical Evaluation:
Symptoms include difficulty with shoe wear due to medial eminence, pain over prominence at MTP joint. Compression of digital nerve may cause numbness and anesthesia.
Examine the entire foot and first ray of the foot and look for associated deformities: pes planus, lesser toe deformities and midfoot and hindfoot conditions.
Imaging Evaluation:
Recommended X-ray views for the foot include:
- AP view.
- Lateral view.
- Oblique view.
- Sesamoid view.
Radiographic measurements
| Angle | Discription | Normal Value |
|---|---|---|
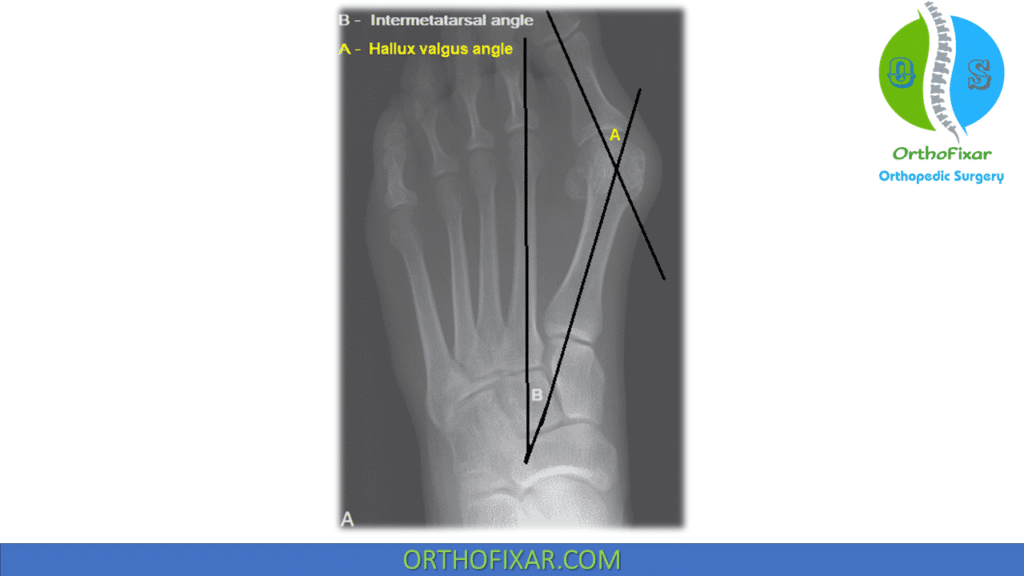
| Hallux valgus angle (HVA) | Angle is formed by line along first metatarsal shaft and line along shaft of proximal phalanx. | < 15 |
| First-second intermetatarsal angle (IMA) | Angle is formed by line along first metatarsal shaft and line along second metatarsal shaft. | < 9 |
| Hallux valgus interphalangeus (HVI) | Angle is formed by line along shaft of proximal phalanx and line along shaft of distal phalanx. | < 10 |
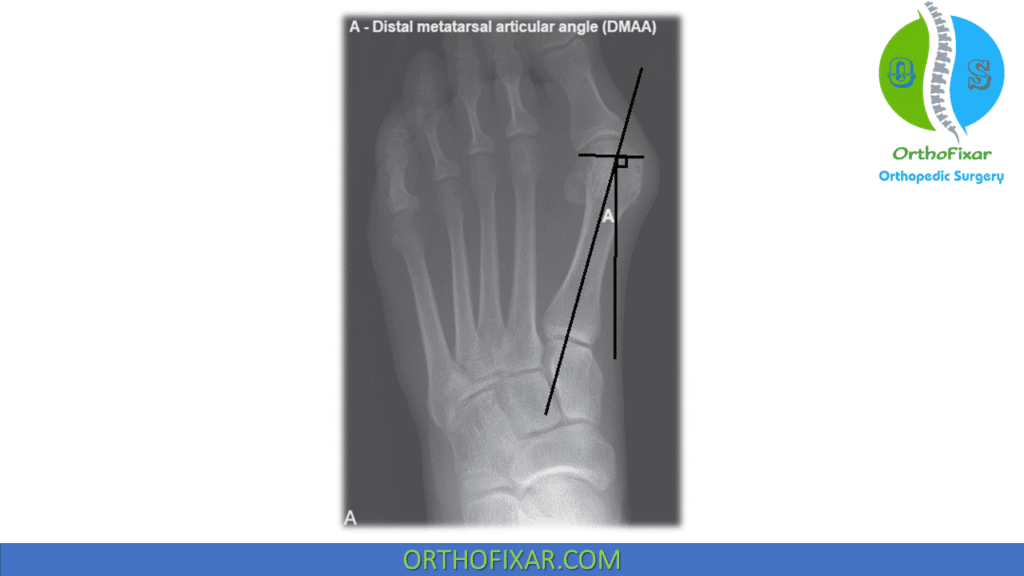
| Distal metatarsal articular angle (DMAA) | Angle is formed by line along articular surface of first metatarsal and line perpendicular to axis of first metatarsal. | < 10 |
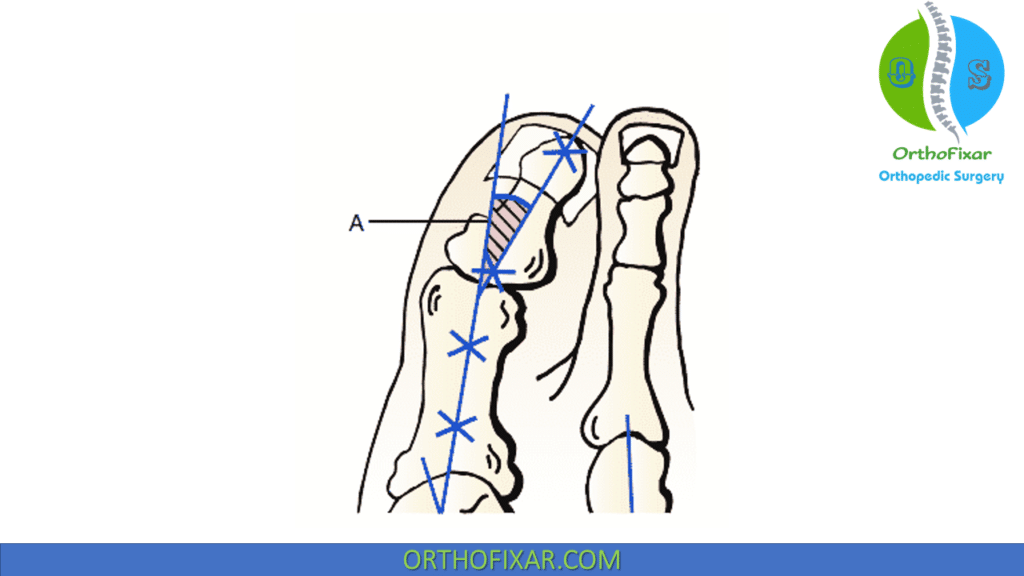
Treatment
Non-Operative is the first line of treatment in mild deformities.
Non-operative hallux valgus treatment include adjusting shoe wear and increasing the size of the toe box may limit pain with pressure along the prominent dorsomedial eminence.
There is no role for “corrective” braces or splints.
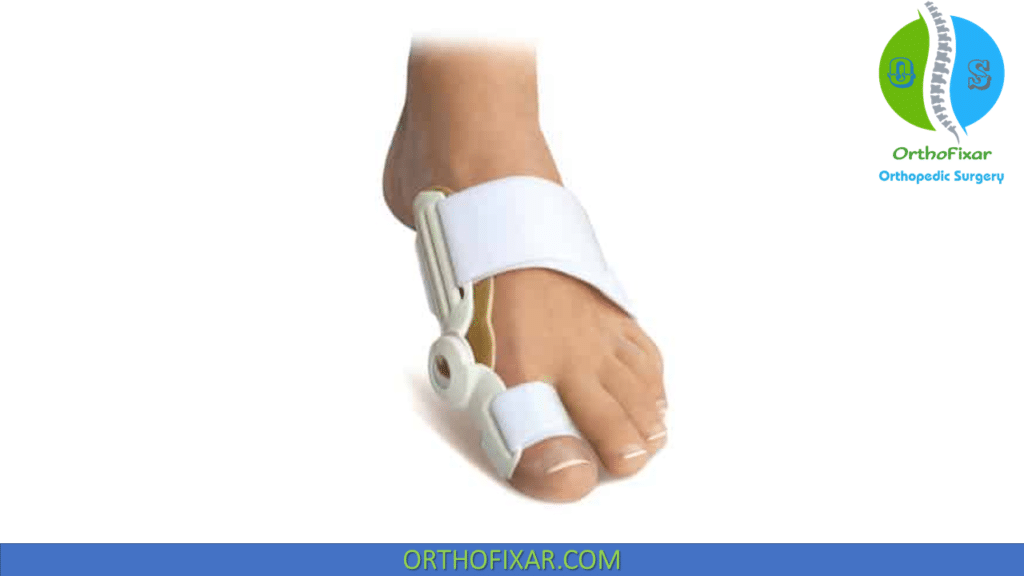
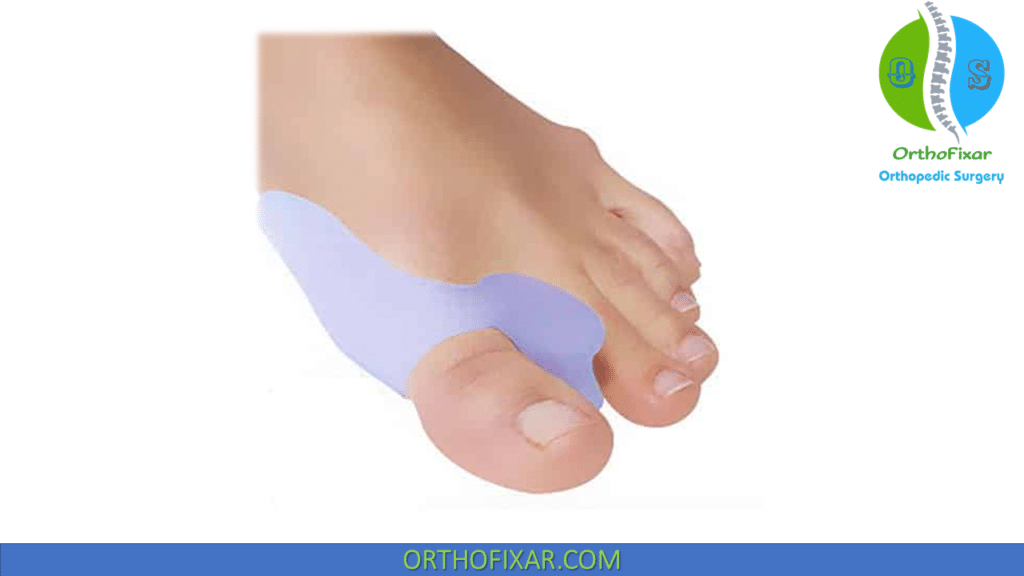
Operative
The best indication for hallux valgus surgery is pain that has not responded to adjusting shoe wear or activity.
Surgical correction of a hallux valgus deformity is NOT a cosmetic procedure.
All patients should undergo a soft tissue release and medial eminence resection and capsular repair with all associated osteotomies and first TMT arthrodesis (Lapidus).
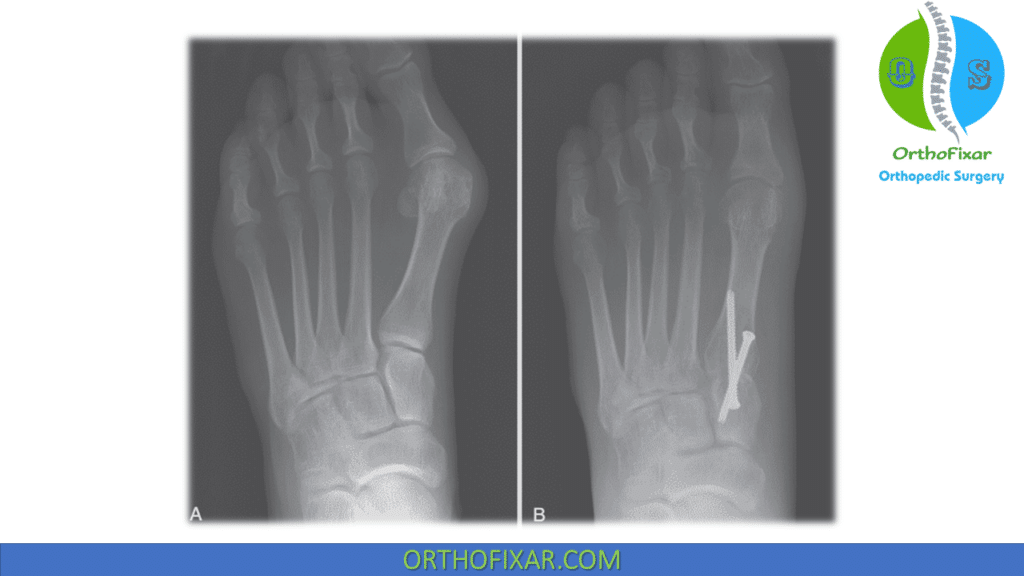
These procedures are not appropriate in isolation (high recurrence rate):
- Distal soft tissue release (modified McBride).
- Medial eminence resection.
- Medial capsular imbrication.
- Isolated osteotomy without associated soft tissue correction.
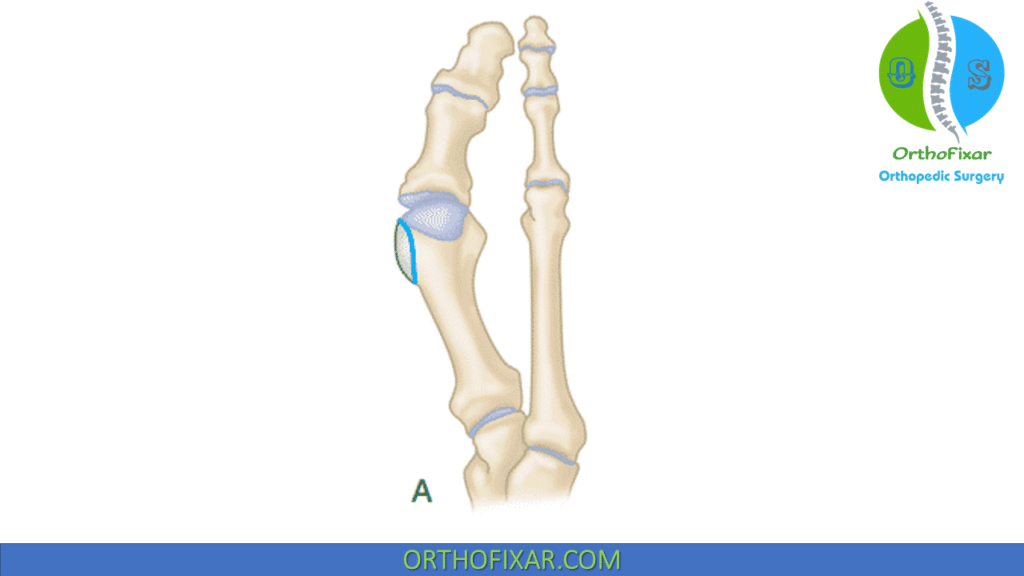
| Measurment | Procedures |
|---|---|
| IMA ≤ 13 degrees AND HVA ≤ 40 degrees | • Distal metatarsal osteotomy (chevron). |
| IMA > 13 degrees OR HVA > 40 degrees | • Proximal metatarsal osteotomy / scarf. |
| Instability of the first TMT/joint laxity | • Lapidus (fusion of first TMT joint). |
| Arthritis or spasticity | First MTP fusion |
| Increased DMMA | Distal metatarsal redirectional osteotomy in addition to metatarsal translational osteotomy |
| HVI | Akin osteotomy |
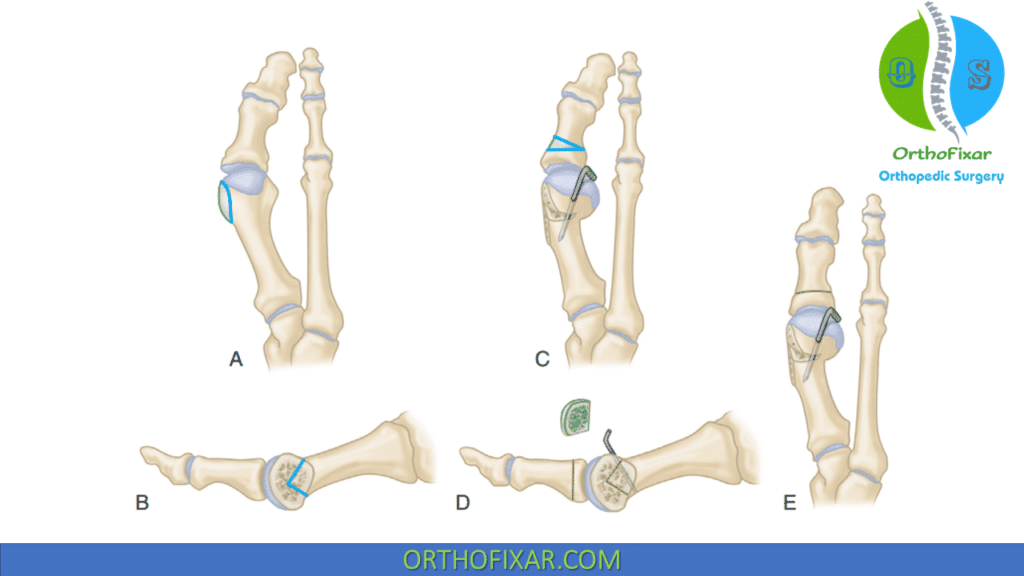
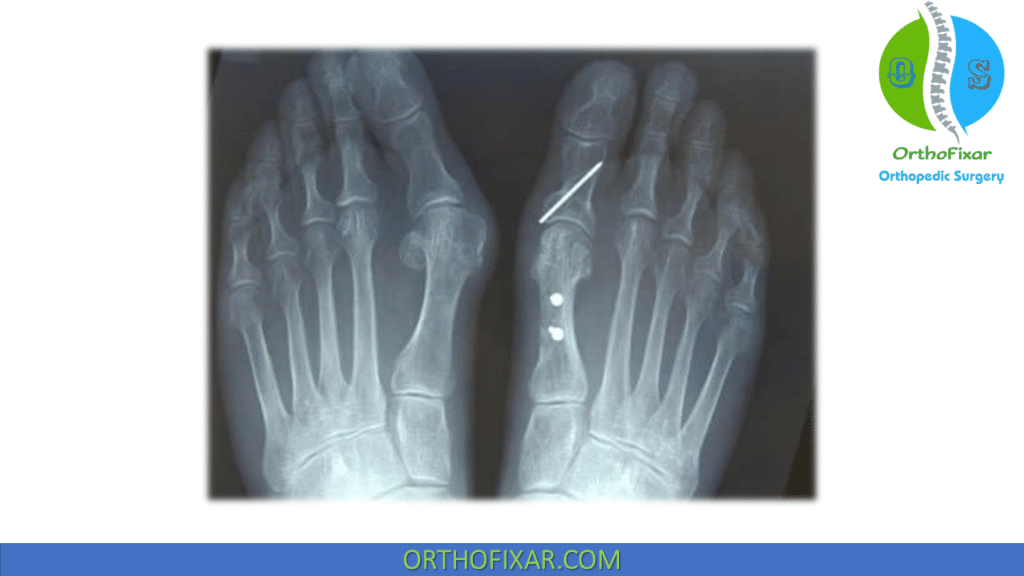
Operative Complications
- Avascular necrosis (AVN) of the metatarsal head.
- Recurrence: highly associated with undercorrection of IMA, isolated soft tissue reconstruction (modified McBride) and isolated resection of the medial eminence.
- Dorsal malunion.
- Hallux varus.
- Nonunion.
References & More
- Campbel’s Operative Orthopaedics 12th edition Book.
- Millers Review of Orthopaedics -7th Edition Book.
- Kuhn J, Alvi F. Hallux Valgus. [Updated 2022 Sep 29]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK553092/
- Wülker N, Mittag F. The treatment of hallux valgus. Dtsch Arztebl Int. 2012 Dec;109(49):857-67; quiz 868. doi: 10.3238/arztebl.2012.0857. Epub 2012 Dec 7. PMID: 23267411; PMCID: PMC3528062.