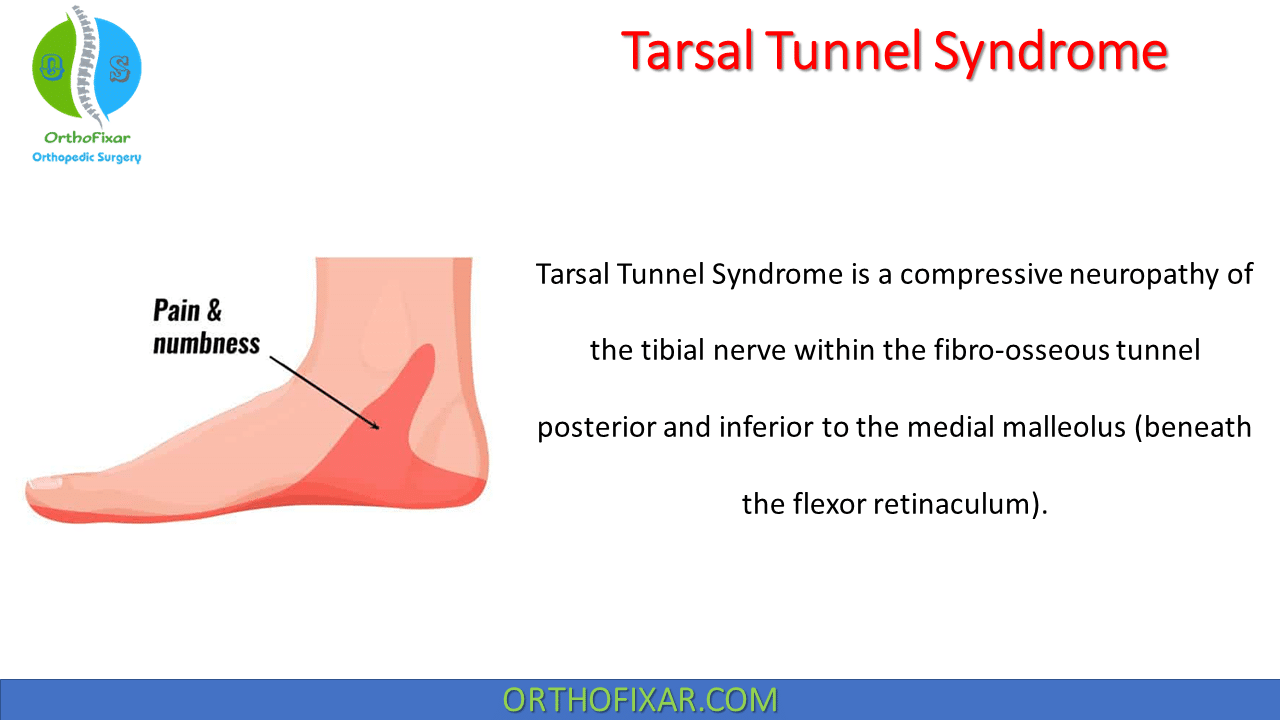
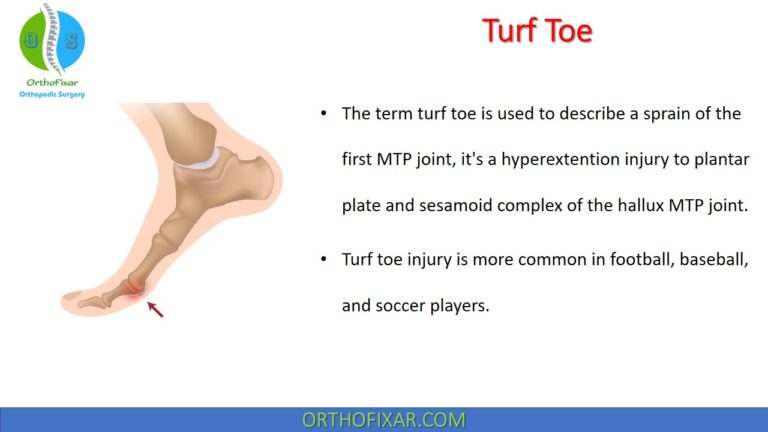
Tarsal Tunnel Syndrome is a compressive neuropathy of the tibial nerve within the fibro-osseous tunnel posterior and inferior to the medial malleolus (beneath the flexor retinaculum).
The incidence of tarsal tunnel syndrome is unknown. It is a relatively rare and often underdiagnosed disease. It is higher in females than in males and can be seen at any age.
Tarsal Tunnel Anatomy
Tarsal tunnel borders are as following:
- The roof of tunnel is formed by Flexor retinaculum (laciniate ligament).
- The ground of the tunnel is formed by talus and calcaneus bone.
- Inferiorly: abductor hallucis tendon.
- anteriorly: the medial malleolus.
Tarsal tunnel includes the following:
- tibialis posterior tendon.
- Flexor hallucis longus tendon.
- Flexor digitorum longus tendon.
- Posterior tibial artery, the venae comitantes.
Flexor retinaculum (laciniate ligament) is an unyielding fibrous roof extends from the medial malleolus posteriorly and inferiorly to the medial side of the tuberosity of the calcaneus and is 2.5 to 3.0 cm wide with indistinct borders. Its proximal border is continuous with the investing deep fascia of the calf, and distally its anterior margin is continuous with the deep fascia of the medial part of the sole.
Causes
The causes of Tarsal Tunnel Syndrome may include the following:
- Tenosynovitis.
- Engorged or varicose vessels.
- synovial or ganglion cysts.
- Pigmented villo-nodular synovitis.
- Nerve sheath tumors.
- Lipomas.
- Fracture of the sustentaculum tali or medial tubercle of the posterior process of the talus.
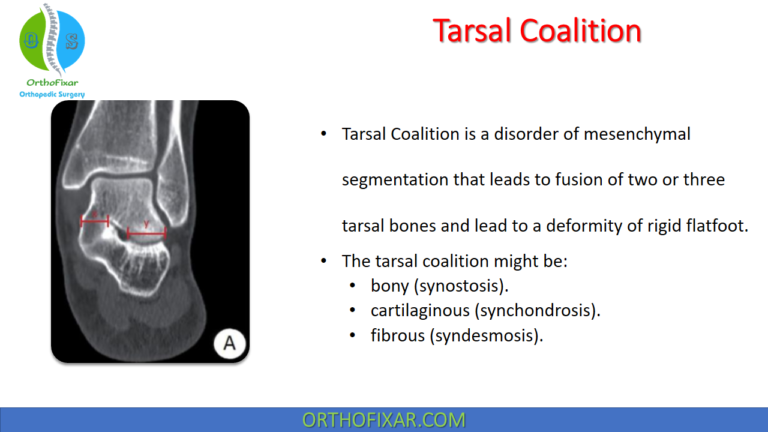
- Middle facet tarsal coalition.
- Accessory muscles.
- Inflammatory edema: as in systemic diseases such as diabetes mellitus, RA, and ankylosing spondylitis may have an indirect effect by causing inflammatory edema.
- A fixed valgus hindfoot can predispose to chronic traction neuropathy of the posterior tibial nerve or one of its branches, resemble tarsal tunnel syndrome.
Clinical Evaluation
Symptoms of tarsal tunnel syndrome may be vague and misleading. These include a burning sensation on the plantar surface of the foot and medial ankle and occasional sharp pains or paresthesia.
Prolonged standing, walking, or running can exacerbate the symptoms.
Symptoms may increased at night, by exercise or rest, or by elevating or lowering the extremity.
Clinical examination include the Tinel’s sign which is positive over tibial nerve. Other clinical signs and examination include:
- The dorsiflexion-eversion is a provocative maneuver that produces the symptoms.
- Sensory examination is usually unpredictable: Sensory abnormalities or differences in temperature, sweating pattern, and skin abnormalities compared to the opposite foot. Dryness and scaliness of the skin may be present over only the medial or only the lateral plantar nerve distribution.
- Assess hindfoot alignment: pes planus may cause increased tension on the nerve.
- Atrophy of the abductor hallucis or abductor digiti minimi or both (often a difficult finding to detect).
Diagnostic Tests
- Electrodiagnostic studies.
- Electromyography (EMG) abnormalities are less sensitive.
- MRI may identify the presence of a mass occupying lesion.
Treatment
Nonoperative treatment is indicated as the first line of treatment which include 6 to 12 weeks of ankle immobilization in a night splint, and medications such as NSAIDs, vitamin B6, and tricyclic antidepressants.
Physical therapy for tarsal tunnel syndrome may include stretching, massage, desensitization, and iontophoresis.
Tarsal tunnel syndrome orthotics is used to correct hindfoot valgus, they play an important role as well.
Operative treatment
Tarsal tunnel release surgery is indicated in these cases:
- Failed of nonoperative treatment (for 3 to 6 months)
- Space-occupying lesion.
- positive EMG.
- Reproducible physical findings.
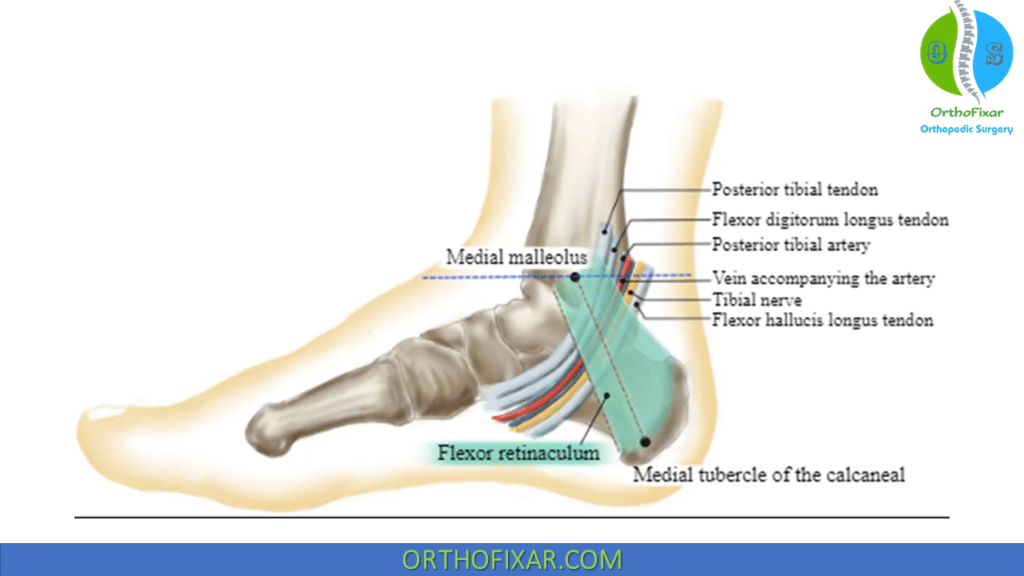
Tarsal tunnel release surgery is performed as following:
- Longitudinal incision made over the course of the tibial nerve; curves distally behind medial malleolus to the abductor musculature.
- The nerve is identified proximally, and the proximal investing fascia and flexor retinaculum are released.
- Care must be taken to release the superficial and deep fascia of the abductor hallucis muscle.
Endoscopic tarsal tunnel release is not recommended.
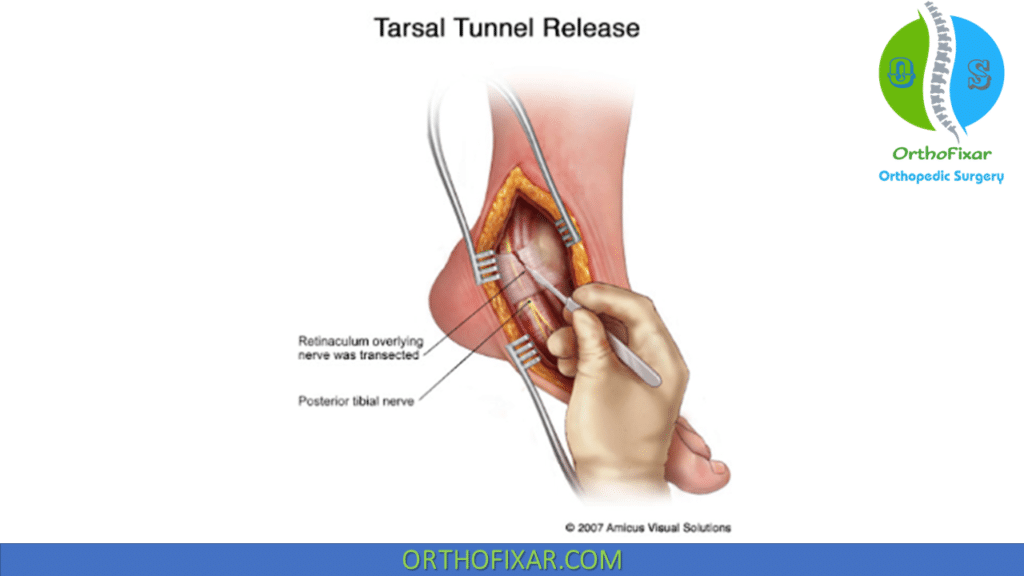
Anterior Tarsal Tunnel Syndrome
Anterior Tarsal Tunnel Syndrome is a compressive neuropathy of the deep peroneal nerve in the fibro-osseous tunnel formed by the inferior extensor retinaculum.
Causes of Compression Anterior Tarsal Tunnel Syndrome
- Tightly laced shoes.
- Anterior osteophytes at the tibiotalar and talo navicular articulations
- A bony prominence associated with pes cavus deformity or fracture.
- Ganglion cysts.
- Tendinitis of the extensor digitorum longus, extensor hallux longus, or tibialis anterior.
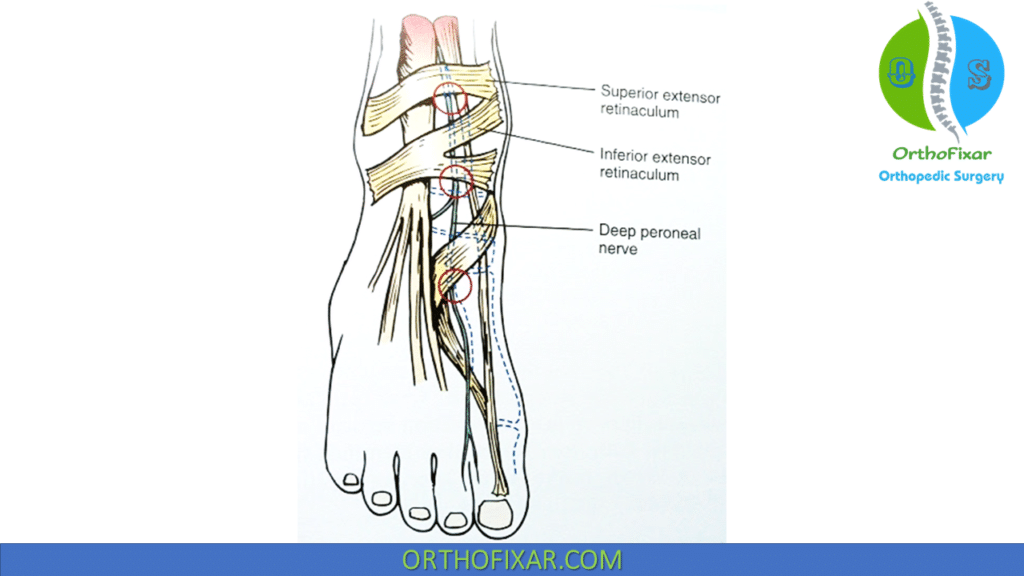
Clinical Evaluation
Burning pain and paresthesias along the medial second toe, lateral hallux, and first web space, or even vague dorsal foot pain.
Symptoms are often worse at night as the ankle assumes a plantar-flexed posture, and with shallow, laced shoes.
Physical examination
- Decreased two-point discrimination.
- Positive Tinel sign along course of the deep peroneal nerve.
- Pain may be worse with plantar flexion of ankle as the nerve is stretched.
Treatment
Nonoperative treatment is the first line of treatment.
Treatments include:
- Night splints.
- Non-steroidal anti-inflammatory drugs (NSAIDs) .
- Corticosteroid injections.
- Shoe tongue padding, and footwear with loose lacing or alternative lacing techniques are the conservative approaches.
Operative treatment
Anterior Tarsal tunnel surgery:
- Incising the inferior extensor retinaculum,
- Excising bone spurs,
- Carefully repairing the bony capsule to avoid exposing the nerve to bleeding bone while protecting the dorsalis pedis artery.
References & More
- Campbel’s Operative Orthopaedics 12th edition Book.
- Millers Review of Orthopaedics -7th Edition Book.
- Rodríguez-Merchán EC, Moracia-Ochagavía I. Tarsal tunnel syndrome: current rationale, indications and results. EFORT Open Rev. 2021 Dec 10;6(12):1140-1147. doi: 10.1302/2058-5241.6.210031. PMID: 35839088; PMCID: PMC8693231.
- Kiel J, Kaiser K. Tarsal Tunnel Syndrome. 2022 Aug 8. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan–. PMID: 30020645.
- Kiel J, Kaiser K. Tarsal Tunnel Syndrome. [Updated 2022 Aug 8]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK513273/