What Is Turf Toe?
Turf toe is a common sports injury involving a sprain of the first metatarsophalangeal (MTP) joint, also known as the big toe joint. The injury usually occurs when the toe is forcefully bent upward into hyperextension, resulting in damage to the plantar plate, joint capsule, and sesamoid complex.
Turf toe is frequently seen in athletes participating in football, soccer, baseball, basketball, and other sports requiring explosive running, cutting, or jumping motions.
See Also: Foot Anatomy
Hallux (Big Toe) Anatomy
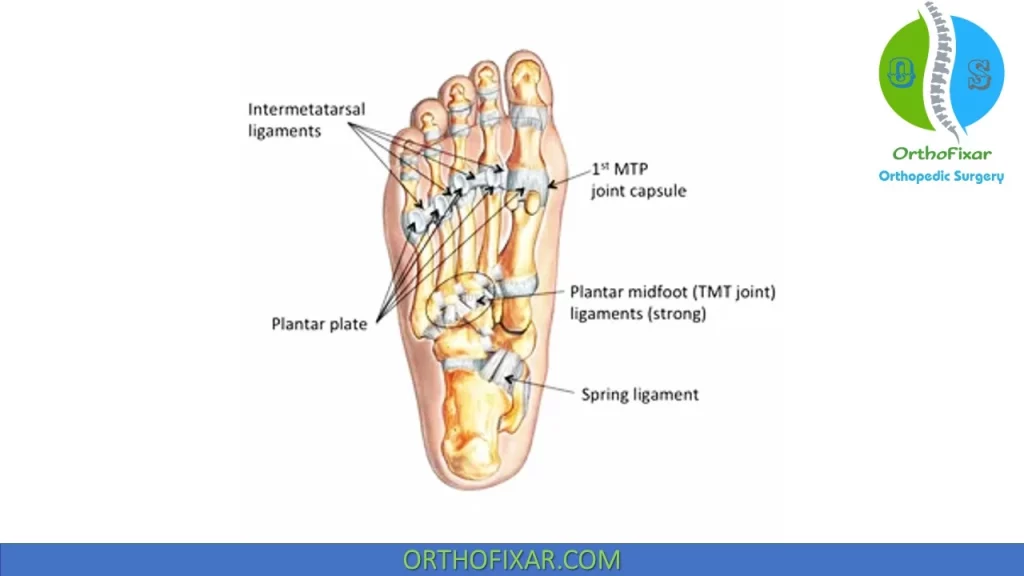
The first MTP joint plays a critical role during gait and push-off activities. Important stabilizing structures include:
- Plantar plate
- Joint capsule
- Collateral ligaments
- Flexor hallucis brevis tendon
- Sesamoid bones
These structures absorb load and stabilize the toe during propulsion. Injury to this complex can significantly impair athletic performance.
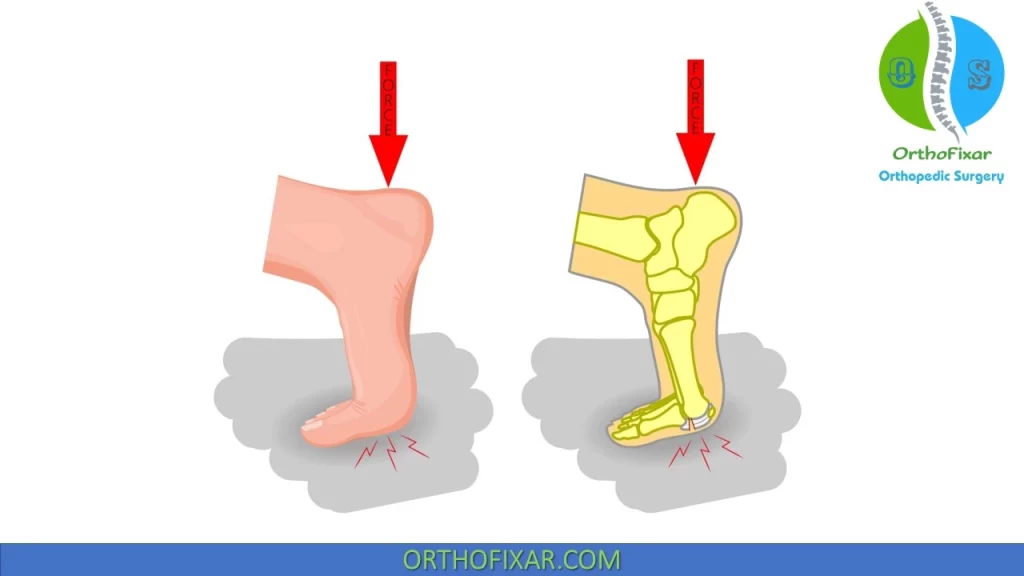
Mechanism of Injury
Most common mechanism of Turf Toe injury is Forced hyperextension of the big toe.
Other causes include:
- Hyperflexion of the toe
- Varus or valgus stress
- Direct trauma
Severe cases may cause:
- Dorsal dislocation of the big toe joint
- Tearing of the capsule and ligaments
- Sesamoid fracture
Turf Toe Injury Classification
Clanton and Ford have classified the severity of turf toe injury into 3 grades:
- Grade I: a minor stretch injury to the soft tissue restraints with little pain, swelling, or disability.
- Grade II: a partial tear of the capsuloligamentous structures with moderate pain, swelling, ecchymosis, and disability.
- Grade III: a complete tear of the plantar plate with severe swelling, pain, ecchymosis, and inability to bear weight normally.
| Grade | Description | Clinical Features | Treatment |
|---|---|---|---|
| Grade I | Minor stretch injury | Mild pain and swelling | Taping, stiff insole, immediate return to play |
| Grade II | Partial tear of plantar structures | Moderate pain, swelling, ecchymosis | Rest 2 weeks, stiff insole, rehab |
| Grade III | Complete plantar plate tear | Severe pain, swelling, inability to bear weight | Immobilization or surgical repair |
Clinical Findings
Patients commonly present with:
- Pain at the first MTP joint
- Swelling around the big toe
- Joint stiffness
- Redness
- Tenderness on plantar and dorsal surfaces
- Limping gait
- Difficulty running or jumping
- Weak push-off strength
Athletes may report either:
- A single traumatic dorsiflexion event
- Repetitive stress injuries over time
Clinical Examination
Important examination findings include:
- Pain with passive dorsiflexion
- Reduced range of motion
- Swelling/ecchymosis
- Antalgic gait
- Weak toe flexion strength
- Tender sesamoids
In chronic cases, athletes may develop:
- Decreased first MTP motion
- Impaired push-off
- Hallux rigidus
Studies suggest that approximately 50% of athletes continue to experience symptoms 5 years after injury.
Radiographic Imaging
Radiographic views include:
- weightbearing AP,
- Lateral view,
- oblique view.
- sesamoid axial views.
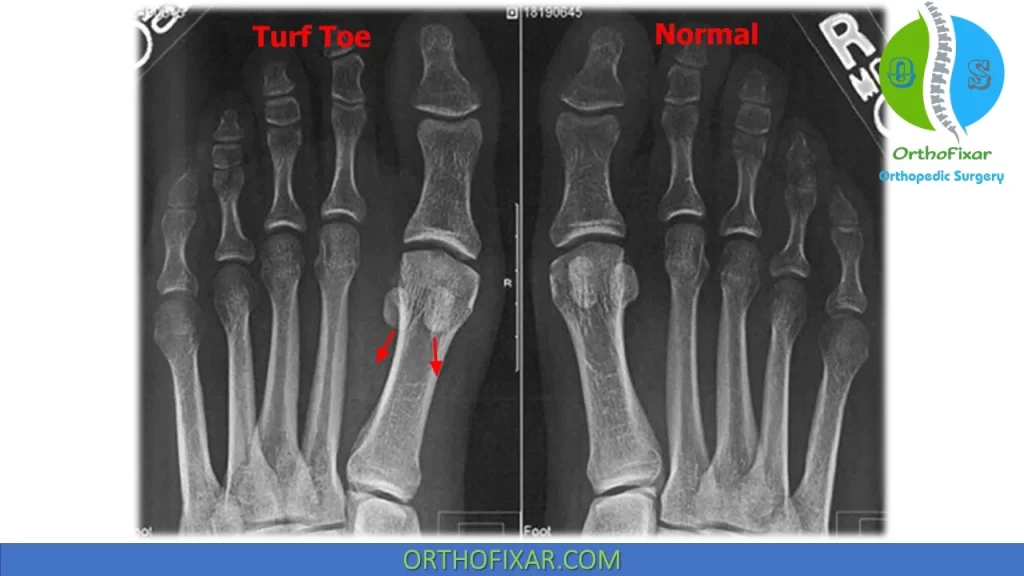
Radiographic findings may include:
- Increased the sesamoid-to-joint distance.
- Medial sesamoid may be displaced proximally.
- A sesamoid fracture
Bone scan is indicated if persistent pain, swelling, weak toe push-off with negative x-ray findings. It may show increased signal at 1st MTP joint.

MRI will show disruption of volar plate.

Turf Toe Treatment
Initial treatment follows the RICE protocol:
- Rest
- Ice
- Compression
- Elevation
Additional treatments include:
- Stiff-soled shoes or carbon-fiber plates
- NSAIDs for pain relief
- Activity modification
- Protective footwear
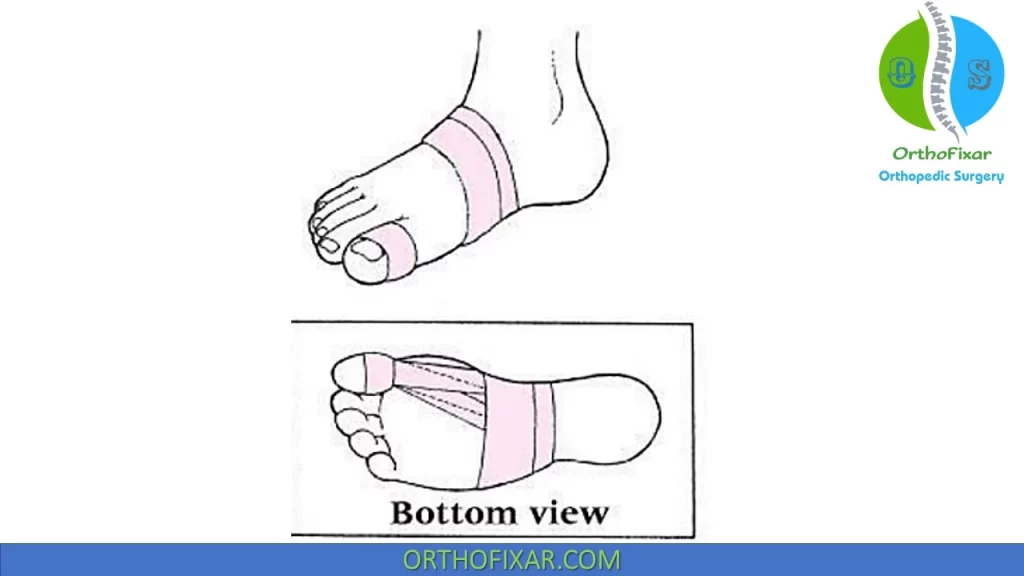
Turf Toe Taping Technique
Turf toe taping helps restrict dorsiflexion of the first MTP joint.
The technique involves:
- Multiple loops of tape over the dorsal proximal phalanx
- Crisscrossing under the plantar forefoot
- Limiting hyperextension during activity
See Also: Turf Toe Taping Technique
Turf Toe Physical Therapy
Grade I Turf Toe Rehabilitation
Treatment includes:
- Taping in slight plantarflexion
- Compression and motion restriction
- Early rehabilitation after 3–5 days
Exercises may include:
- Gentle plantarflexion stretching
- Progressive strengthening
- Joint mobilization
- Cycling
- Pool therapy
- Elliptical training
Stiff-soled shoes are recommended.
Grade II Turf Toe Rehabilitation
Goals include:
- Reducing pain and inflammation
- Restoring range of motion
- Improving strength
Rehabilitation methods:
- Passive joint mobilization
- Toe protectors/orthotics
- Toe crunches
- Towel curls
- Sand bucket exercises
- Short-foot exercises
- Pulsed ultrasound
- Iontophoresis
Return to sports usually requires at least 2 weeks.
Grade III Turf Toe Rehabilitation
Grade III injuries often require:
- Immobilization in plantarflexion for 8 weeks
- Extended rehabilitation
- Gradual return to sport over several months
Before returning to sports, the athlete should achieve:
- Pain-free dorsiflexion of 50–60°
- Functional strength restoration
- Normal push-off mechanics
Some severe injuries require surgery.
Surgical Treatment for Turf Toe
Operative treatment may be indicated for:
- Complete plantar plate rupture
- Sesamoid fractures
- Joint instability
- Failed conservative treatment
- Persistent pain
- Chronic instability
Surgical repair may include:
- Plantar plate repair
- Sesamoid fixation
- Capsular reconstruction
Studies have demonstrated favorable outcomes with operative repair in severe Grade III injuries.
Return to Sport After Turf Toe
Return-to-play timelines depend on injury severity.
| Injury Grade | Expected Return |
|---|---|
| Grade I | Immediate or symptom-guided |
| Grade II | 3–14 days |
| Grade III | Up to 6 weeks or longer |
Return to play is generally allowed when:
- Pain is minimal
- Strength is restored
- Push-off is painless
- The toe achieves approximately 90° dorsiflexion
Premature return may lead to chronic disability.
Turf Toe Complications
Potential long-term complications include:
Hallux Rigidus
A chronic degenerative condition causing:
- Pain
- Stiffness
- Limited motion
Treatment options include:
- Cheilectomy
- Arthrodesis
Stress Fractures
Proximal phalanx stress fractures may occur and are sometimes overlooked.
Prevention of Turf Toe
Preventive measures include:
- Wearing stiff-soled athletic shoes
- Using orthotics or toe protectors
- Proper warm-up before sports
- Avoiding repetitive overload
- Strengthening intrinsic foot muscles
Athletes competing on artificial turf surfaces may benefit from footwear modifications.
Prognosis
Most Grade I and II injuries recover well with conservative treatment. However, severe injuries may result in chronic pain, stiffness, and long-term functional impairment if not properly managed.
Early diagnosis and structured rehabilitation are essential for optimal outcomes.
Key Points
- Turf toe is a sprain of the first MTP joint.
- Forced hyperextension is the most common mechanism.
- MRI is useful for diagnosing plantar plate injuries.
- Treatment depends on injury severity.
- Early rehabilitation improves outcomes.
- Severe injuries may require surgery.
- Chronic complications include hallux rigidus and persistent pain.
Q&A for Patients
What is turf toe?
Turf toe is a sprain of the first metatarsophalangeal (MTP) joint in the foot, which is the joint that connects the big toe to the rest of the foot. It is often caused by hyperextension of the joint, and is common in sports like football, baseball, and soccer.
What are the symptoms of turf toe?
Symptoms of turf toe include pain, swelling, stiffness, and redness in the first MTP joint. The joint may be tender to the touch, and patients may have difficulty running or jumping due to pain. In more severe cases, patients may experience difficulty bearing weight on the foot.
How is turf toe diagnosed?
Diagnosis of turf toe is typically based on a physical examination, where the doctor will assess the patient’s range of motion and check for tenderness in the affected joint. X-rays may also be taken to rule out any other injuries, such as fractures or dislocations.
What is the treatment for turf toe?
Treatment for turf toe depends on the severity of the injury. In general, rest, ice, compression, and elevation (RICE) are recommended in the acute phase of injury, along with nonsteroidal anti-inflammatory drugs (NSAIDs) for pain relief. Turf toe tapping may also be used to limit dorsiflexion of the joint. Physical therapy is often recommended to help restore range of motion and strength, and in some cases, surgical intervention may be necessary.
How long does it take to recover from turf toe?
Recovery time for turf toe varies depending on the severity of the injury. Grade I injuries may allow for a quick return to sports activities, while Grade III injuries may require up to 6 months of immobilization and rehabilitation before returning to normal activity.
What are the long-term complications of turf toe?
Long-term complications of turf toe may include decreased range of motion in the affected joint, impaired push-off, and the development of hallux rigidus, which is a condition that causes stiffness and pain in the big toe. In some cases, a stress fracture of the proximal phalanx may also occur. Treatment for these complications may involve cheilectomy or arthrodesis, depending on severity.
How can I prevent turf toe?
To help prevent turf toe, it is important to wear appropriate footwear for your sport, with stiff-soled shoes that limit the motion of the big toe. Toe protectors or orthotics may also be recommended to provide additional support. It is also important to warm up properly before engaging in sports activities, and to avoid overuse or repetitive stress on the joint.
References
- Wedmore IS, Charette J: Emergency department evaluation and treatment of ankle and foot injuries. Emerg Med Clin North Am 18:86–114, 2000. PubMed
- Hockenbury RT. Forefoot problems in athletes. Med Sci Sports Exerc. 1999 Jul;31(7 Suppl):S448-58. doi: 10.1097/00005768-199907001-00006. PMID: 10416546. PubMed
- Sammarco GJ: Turf toe. Instr Course Lect 42:207–212, 1993.
- Omey ML, Micheli LJ. Foot and ankle problems in the young athlete. Med Sci Sports Exerc. 1999 Jul;31(7 Suppl):S470-86. doi: 10.1097/00005768-199907001-00008. PMID: 10416548. PubMed
- Glasoe WM, Yack HJ, Saltzman CL: Anatomy and biomechanics of the first ray. Phys Ther 79:854–859, 1999. PubMed
- Garrick JG. Characterization of the Patient Population in a Sports Medicine Facility. Phys Sportsmed. 1985 Oct;13(10):73-6. doi: 10.1080/00913847.1985.11708901. PMID: 27409750. PubMed
- Dutton’s Orthopaedic Examination, Evaluation, And Intervention 3rd Edition.
- Millers Review of Orthopaedics -7th Edition Book.