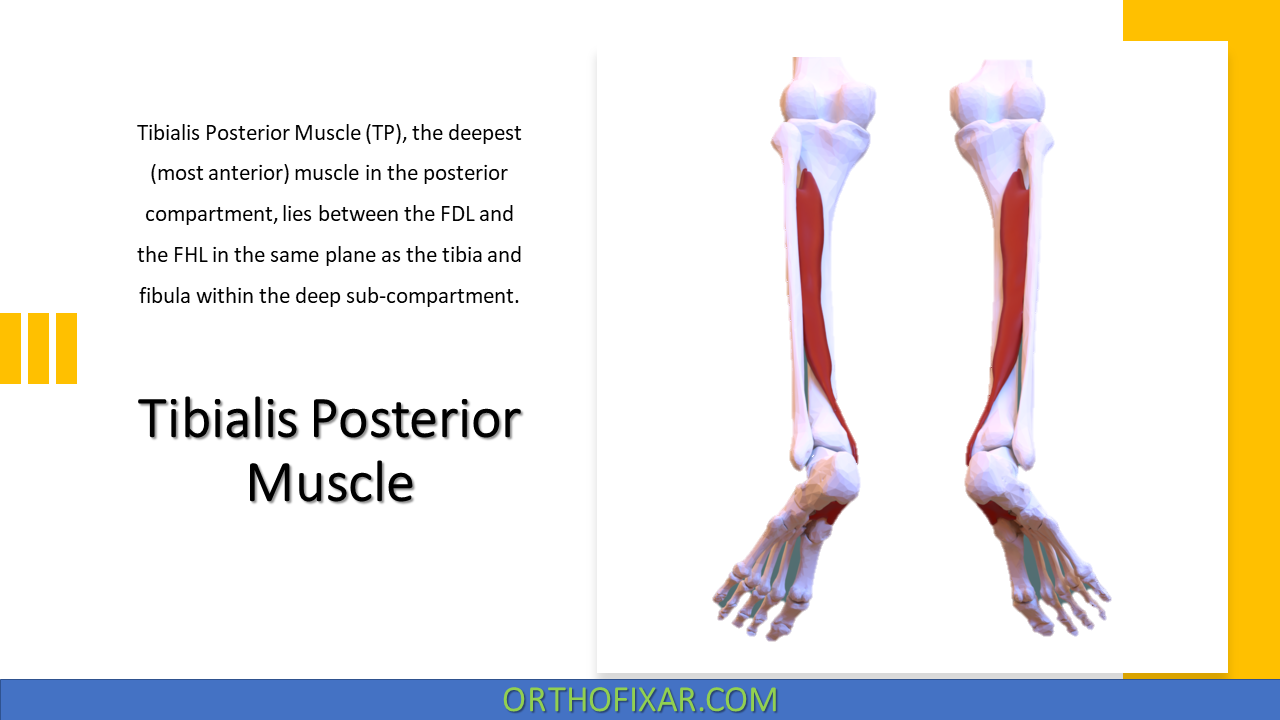
Tibialis Posterior Muscle (TP), the deepest (most anterior) muscle in the posterior compartment, lies between the FDL and the FHL in the same plane as the tibia and fibula within the deep sub-compartment.
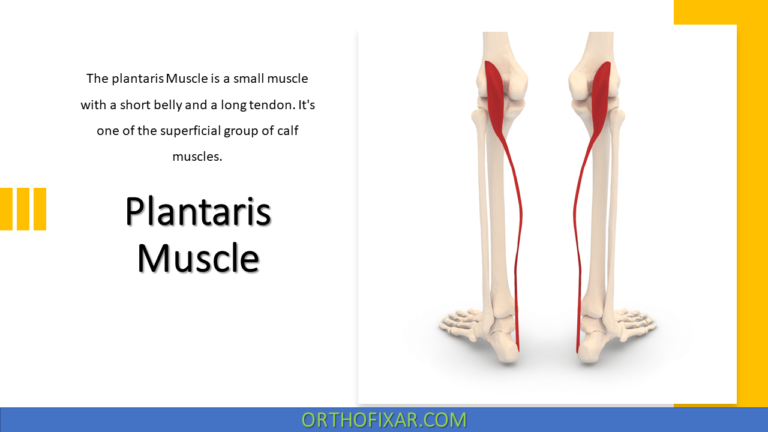
The posterior compartment contains seven muscles: the gastrocnemius, soleus, plantaris, popliteus, flexor digitorum longus, flexor hallucis longus, and the tibialis posterior.
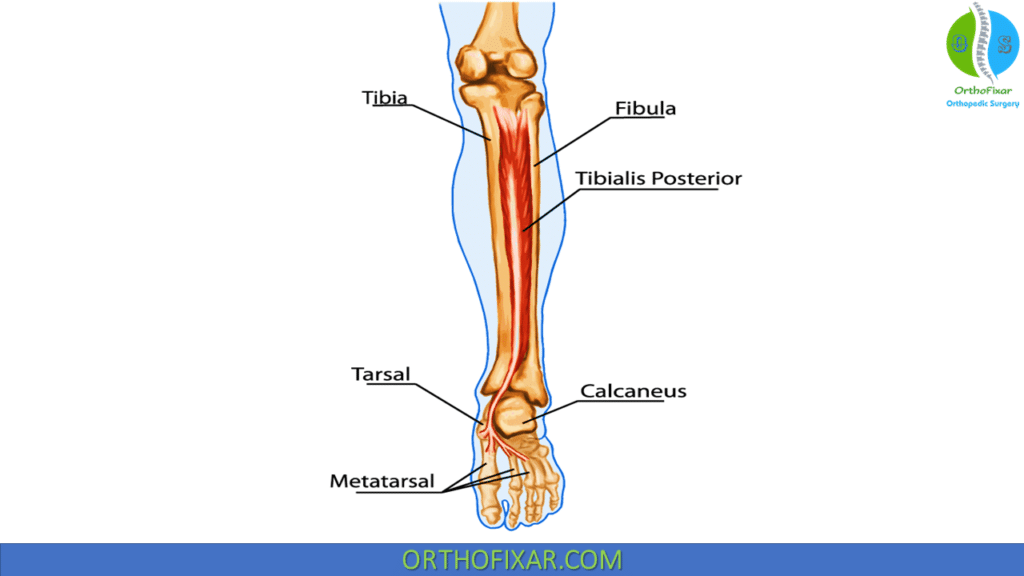
Tibialis Posterior Muscle Anatomy
Distally, the TP attaches primarily to the navicular bone (in close proximity to the high point of the medial longitudinal arch of the foot) but has attachments to other tarsal and metatarsal bones.
See Also: Flexor Digitorum Longus See Also: Flexor Hallucis Longus Muscle
Origin
The tibialis posterior muscle originates from the:
- Posterior aspect of interosseous membrane
- Superior 2/3 of medial posterior surface of fibula,
- Superior aspect of posterior surface of tibia,
- From intermuscular septum between muscles of posterior compartment and deep transverse septum
Insertion
- Splits into two slips after passing inferior to plantar calcaneonavicular ligament;
- superficial slip inserts on the tuberosity of the navicular bone and sometimes medial cuneiform;
- deeper slip divides again into slips inserting on plantar surfaces of metatarsals 2 – 4 and second cuneiform
Innervation
The tibialis posterior is innervated by the tibial nerve (L4, L5) (L4, L5).
Blood Supply
It’s supplied by the muscular branches of sural, peroneal and posterior tibial arteries.
Action
- Principal invertor of foot;
- It also adducts foot
- Plantar flexes ankle,
- Helps to supinate the foot.
The tibialis posterior muscle is traditionally described as an invertor of the foot. Indeed, when the foot is off the ground, it can act synergistically with the tibialis anterior to invert the foot, their otherwise antagonistic functions canceling each other out. However, the primary role of the tibialis posterior is to support or maintain (fix) the medial longitudinal arch during weight bearing; consequently, the muscle contracts statically throughout the stance phase of gait.
In so doing, it acts independently of the tibialis anterior because once the foot is flat on the ground after heel strike, that muscle is relaxed during the stance phase (the dorsiflexion that occurs as the body passes over the planted foot is passive), unless braking requires its eccentric contraction.
While standing (especially on one foot), however, the two muscles may cooperate to depress the lateral side of the foot and pull medially on the leg as needed to counteract lateral leaning for balance.
| Origin | Posterior aspect of interosseous membrane Superior 2/3 of medial posterior surface of fibula, Superior aspect of posterior surface of tibia, From intermuscular septum between muscles of posterior compartment and deep transverse septum |
| Insertion | Splits into two slips after passing inferior to plantar calcaneonavicular ligament; Superficial slip inserts on the tuberosity of the navicular bone and sometimes medial cuneiform; Deeper slip divides again into slips inserting on plantar surfaces of metatarsals 2 – 4 and second cuneiform |
| Innervation | Tibial nerve (L4, L5) (L4, L5) |
| Blood Supply | Muscular branches of sural, peroneal and posterior tibial arteries |
| Action | Principal invertor of foot; Adducts foot Plantar flexes ankle, Helps to supinate the foot |

Clinically
Posterior tibial tendon dysfunction (PTTD) represents an acquired, progressive disease of the foot and ankle that is seen commonly in middle-aged patients. It is the most common cause of adult acquired flatfoot deformity. Treatments involve conservative and surgical options depending on the severity of the disease.
The tibialis posterior tendon (TPT) can also become inflamed and irritated due to an acute injury, such as a fall, or overuse during high-impact sports such as basketball, tennis, or soccer.
To test the tibialis posterior, the foot is inverted against resistance with the foot in slight plantarflexion; if normal, the tendon can be seen and palpated posterior to the medial malleolus.
References & More
- Clinically Oriented Anatomy – 8th Edition
- Knapp PW, Constant D. Posterior Tibial Tendon Dysfunction. [Updated 2023 May 23]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK542160/
- Corcoran NM, Varacallo M. Anatomy, Bony Pelvis and Lower Limb: Tibialis Posterior Muscle. [Updated 2023 Aug 28]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK539913/