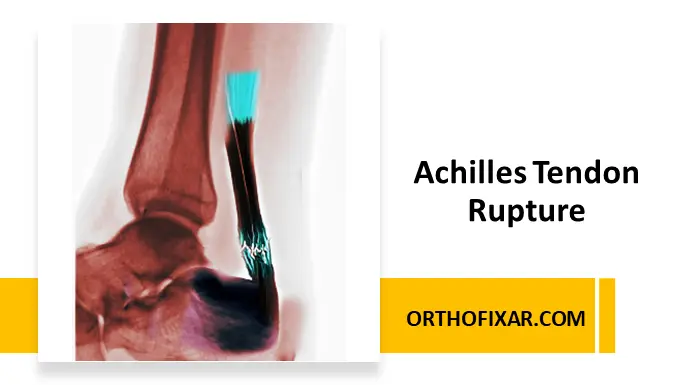
An Achilles tendon rupture is a partial or complete tear of the Achilles tendon, the strongest and largest tendon in the human body. The injury commonly occurs during sudden acceleration, jumping, pivoting, or forceful dorsiflexion of the ankle.
This injury is highly relevant in sports medicine and orthopedic trauma because delayed or missed diagnosis can significantly impair long-term calf strength, gait mechanics, and athletic performance.
Epidemiology of Achilles Tendon Rupture
Most Achilles tendon disorders are related to chronic overuse and repetitive mechanical overload. The pathology exists along a continuum:
- Paratenonitis
- Tendinosis
- Partial tendon tearing
- Acute complete rupture
Acute rupture is the most common severe Achilles injury encountered in trauma settings.
Key Epidemiological Facts
- Achilles tendon rupture incidence is increasing worldwide due to greater sports participation in middle-aged adults.
- Commonly affects patients aged 30–50 years.
- More frequent in males.
- Frequently associated with recreational sports (“weekend warrior” athletes).
- Delayed or missed diagnosis occurs in up to 25% of cases.
- Risk factors include:
- Fluoroquinolone antibiotic use
- Corticosteroid injections
- Obesity
- Diabetes mellitus
- Poor conditioning
- Chronic tendinopathy
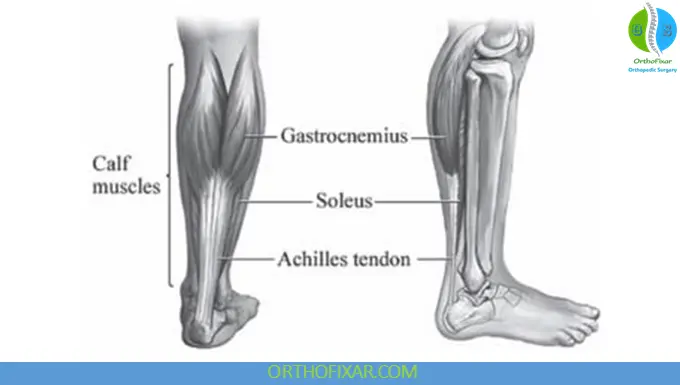
Anatomy of the Achilles Tendon
The Achilles tendon is formed by the confluence of the:
- Gastrocnemius muscle
- Soleus muscle
It inserts onto the posterior calcaneal tuberosity and functions as the primary plantar flexor of the ankle.
Important Anatomical Features
- Largest tendon in the body
- No true synovial sheath
- Surrounded by a paratenon that permits approximately 1.5 cm of tendon glide
- Watershed zone located 2–6 cm proximal to insertion is relatively hypovascular and prone to rupture
Blood Supply
The tendon receives vascular supply from:
- Musculotendinous junction
- Osseous insertion
- Mesotenon vessels along the anterior tendon surface
See Also: Ankle Anatomy
Mechanism of Injury
Achilles tendon rupture typically occurs during:
- Sudden push-off movements
- Explosive jumping
- Forced ankle dorsiflexion
- Unexpected eccentric calf contraction
Common sports include:
- Basketball
- Soccer
- Tennis
- Volleyball
- Sprinting activities
Patients often describe hearing or feeling a “pop.”
Symptoms of Achilles Tendon Rupture
Typical Clinical Presentation
Patients frequently report:
- Sudden sharp posterior ankle pain
- Sensation of being “kicked” in the back of the leg
- Audible snapping sound
- Difficulty walking
- Weak push-off strength
Partial Rupture Symptoms
Partial tears may present with:
- Localized tenderness
- Mild swelling
- Preserved plantar flexion
- Pain during activity
Complete Rupture Symptoms
Complete rupture commonly causes:
- Palpable tendon gap
- Inability to perform single-leg heel raise
- Weak or absent plantar flexion
- Antalgic gait
Physical Examination
Thompson Test
The Thompson test is the most important clinical maneuver for diagnosing Achilles tendon rupture. The patient lies prone while the examiner squeezes the calf muscles. In ruptured tendon there is no plantar flexion occurs.
See Also: Thompson Test
Diagnostic Imaging
Plain Radiographs
X-rays are primarily used to exclude:
- Calcaneal avulsion fractures
- Associated ankle injuries
- Haglund deformity
Soft tissue swelling and obliteration of Kager’s triangle may be visible.
Ultrasound
Ultrasound is highly effective for:
- Dynamic tendon evaluation
- Detecting partial tears
- Identifying tendon gaps
Advantages include low cost and rapid bedside assessment.
MRI
MRI is reserved for:
- Equivocal diagnosis
- Chronic ruptures
- Surgical planning
- Partial tears
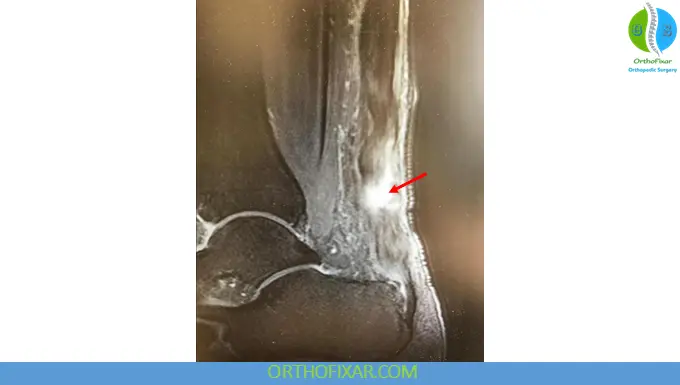
MRI findings include:
- Tendon discontinuity
- Intratendinous edema
- Retraction of tendon ends
Classification of Achilles Tendon Rupture
By Extent
Partial Rupture
- Incomplete tearing
- Some preserved continuity
Complete Rupture
- Full-thickness disruption
By Location
- Midsubstance rupture (most common)
- Insertional rupture
- Musculotendinous junction rupture
Treatment of Achilles Tendon Rupture
The primary treatment goal is restoration of normal musculotendinous length and tension to optimize calf strength and ankle function.
Management remains controversial between operative and nonoperative approaches.
Nonoperative Treatment
Nonoperative management is commonly used for:
- Sedentary patients
- Older adults
- Patients with medical comorbidities
- High surgical-risk individuals
Initial Immobilization
Treatment begins with:
- Posterior splint
- Foot maintained in plantar flexion
- Immobilization for approximately 2 weeks
Casting or Functional Boot
After initial splinting:
- Short- or long-leg cast/boot for 6–8 weeks
- Gradual reduction in plantar flexion
- Progressive weight bearing begins around 2–4 weeks
Rehabilitation Timeline
Weeks 8–10
- Progressive calf strengthening
- Resistance exercises
Months 4–6
- Return to athletic activity
Long-Term Recovery
Patients should understand:
- Maximal plantar flexion power may require 12 months or longer
- Mild residual weakness is common
Surgical Treatment
Operative repair is often preferred for:
- Younger patients
- Competitive athletes
- High-demand individuals
Advantages of Surgery
Potential benefits include:
- Lower rerupture rate
- Improved calf strength
- Faster return to sports
- Better push-off mechanics
Surgical Risks
Potential complications include:
- Wound infection
- Skin necrosis
- Adhesions
- Sural nerve injury
- Deep vein thrombosis
Surgical Techniques
Open Repair
Open repair allows:
- Direct visualization
- Precise tendon reapproximation
- Evaluation of tendon quality
Surgical Approach
- Medial longitudinal incision
- Identification and protection of sural nerve
- Separate paratenon closure
Percutaneous Repair
Advantages:
- Smaller incision
- Less soft tissue dissection
- Lower wound complication rate
Disadvantages:
- Potential sural nerve entrapment
- Incomplete tendon capture risk
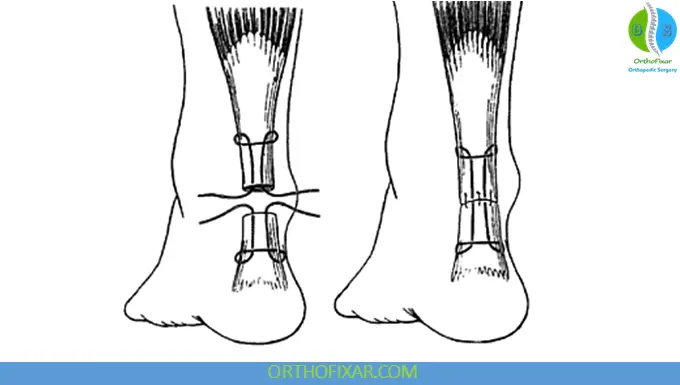
Distal Achilles Rupture and Avulsion
Distal ruptures near the calcaneal insertion typically require:
- Open surgery
- Tendon reattachment to calcaneus
- Transosseous suture fixation
These injuries are technically more challenging than midsubstance ruptures.
Postoperative Rehabilitation
Modern rehabilitation emphasizes early functional recovery.
Typical Protocol
First 6–8 Weeks
- Walking boot or cast
- Partial or tolerated weight bearing
Weeks 8–10
- Strengthening exercises
- Progressive range of motion
Months 4–6
- Return to sports participation
Accelerated rehabilitation protocols using stronger suture constructs are increasingly common.
Complications of Achilles Tendon Rupture
Potential complications include:
- Rerupture
- Tendon elongation
- Calf weakness
- Stiffness
- Infection
- Sural neuritis
- Deep vein thrombosis
- Chronic pain
Prognosis
Most patients achieve satisfactory functional recovery with appropriate management and rehabilitation.
Better Outcomes Are Associated With
- Early diagnosis
- Early functional rehabilitation
- Good patient compliance
- Appropriate patient selection for surgery
Elite athletes may require prolonged rehabilitation before full return to preinjury performance.
Prevention Strategies
Preventive measures include:
- Proper warm-up
- Progressive training loads
- Calf flexibility programs
- Eccentric strengthening
- Avoiding sudden activity spikes
- Managing chronic tendinopathy early
Key Clinical Pearls
- Missed Achilles tendon rupture remains common.
- A positive Thompson test strongly suggests complete rupture.
- Both operative and nonoperative treatment can produce good outcomes.
- Early functional rehabilitation is critical regardless of treatment choice.
- Surgical treatment is generally favored in athletic patients.
Frequently Asked Questions (FAQ)
Can you walk with an Achilles tendon rupture?
Yes. Some patients can still walk due to accessory plantar flexor muscles, which contributes to missed diagnosis.
How long does Achilles tendon rupture recovery take?
Functional recovery typically requires 4–6 months, while maximal strength recovery may take over 12 months.
Is surgery always necessary?
No. Many patients achieve good outcomes with modern nonoperative functional rehabilitation protocols.
What is the rerupture rate?
Historically higher with nonoperative treatment, but modern rehabilitation protocols have significantly reduced the difference between surgical and nonsurgical management.
Conclusion
Achilles Tendon Rupture is a common and potentially disabling injury affecting active individuals and athletes. Accurate early diagnosis, especially through clinical examination and the Thompson test, is essential to avoid chronic dysfunction.
Both operative and nonoperative treatment strategies can yield favorable outcomes when combined with structured rehabilitation. Treatment selection should be individualized according to patient age, activity level, medical comorbidities, and functional goals.
References & More
- Tarantino D, Palermi S, Sirico F, Corrado B. Achilles Tendon Rupture: Mechanisms of Injury, Principles of Rehabilitation and Return to Play. J Funct Morphol Kinesiol. 2020 Dec 17;5(4):95. doi: 10.3390/jfmk5040095. PMID: 33467310; PMCID: PMC7804867. Pubmed
- Shamrock AG, Dreyer MA, Varacallo MA. Achilles Tendon Rupture. [Updated 2023 Aug 17]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: Pubmed
- Wang CC, Chen PY, Yang KC, Wang CL, Chen IH. Current treatment concepts for Achilles tendon rupture. Tzu Chi Med J. 2024 Jan 12;36(1):46-52. doi: 10.4103/tcmj.tcmj_113_23. PMID: 38406567; PMCID: PMC10887342. Pubmed
- Egol KA. Handbook of fractures. 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2019.