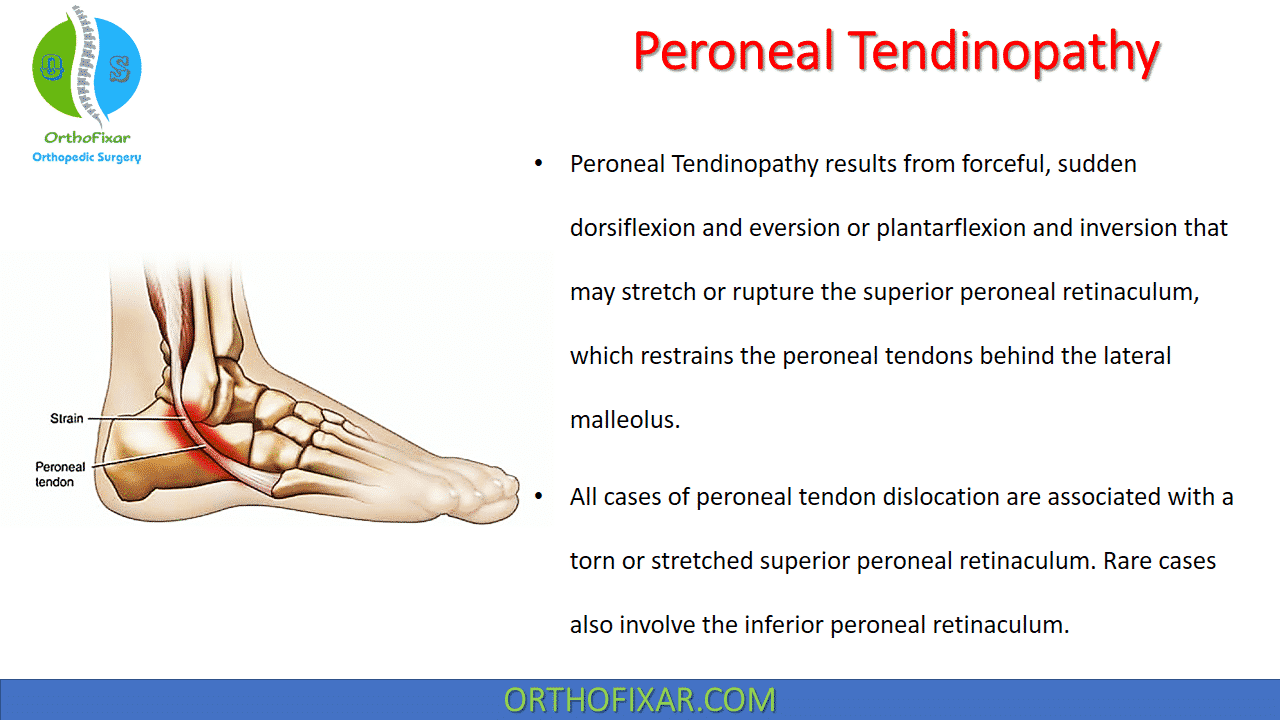
Peroneal Tendinopathy results from forceful, sudden dorsiflexion and eversion or plantarflexion and inversion that may stretch or rupture the superior peroneal retinaculum, which restrains the peroneal tendons behind the lateral malleolus.
All cases of peroneal tendon dislocation are associated with a torn or stretched superior peroneal retinaculum. Rare cases also involve the inferior peroneal retinaculum.
When these tendons lose their alignment from behind the lateral malleolus and slip anteriorly, the peroneals, which are normally plantarflexors, become dorsiflexors . The dislocation process starts proximally and, with time, progresses distally.
See Also: Ankle Anatomy
Pathology
Anatomically, a flattened or convex fibular groove predisposes peroneal subluxations by decreasing the depth of the bony channel through which the tendons pass.
The peroneal tendons may be observed or palpated as they dislocate from the groove behind the lateral malleolus as they snap into and out of position during active plantarflexion and dorsiflexion or active eversion. This change alters the biomechanics of the foot and ankle, resulting in pain and dysfunction.
During an inversion mechanism of an ankle sprain, the peroneus longus tendon pulls the anterior portion of the peroneus brevis tendon over the sharp posterior fibular ridge as it snaps out of the groove. These ruptures contribute to future peroneal tendon subluxation, dislocation, and peroneal tendinopathy.
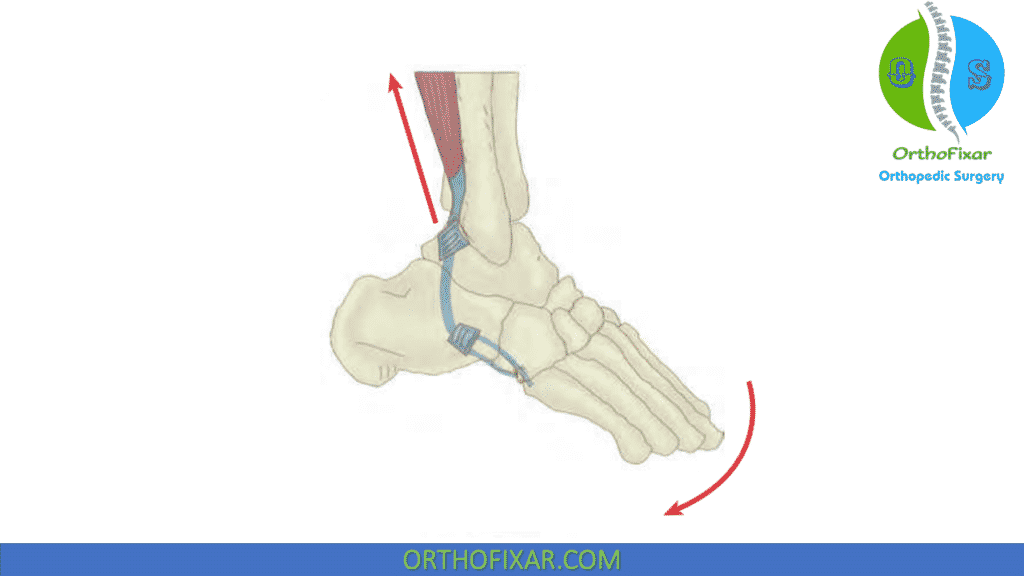
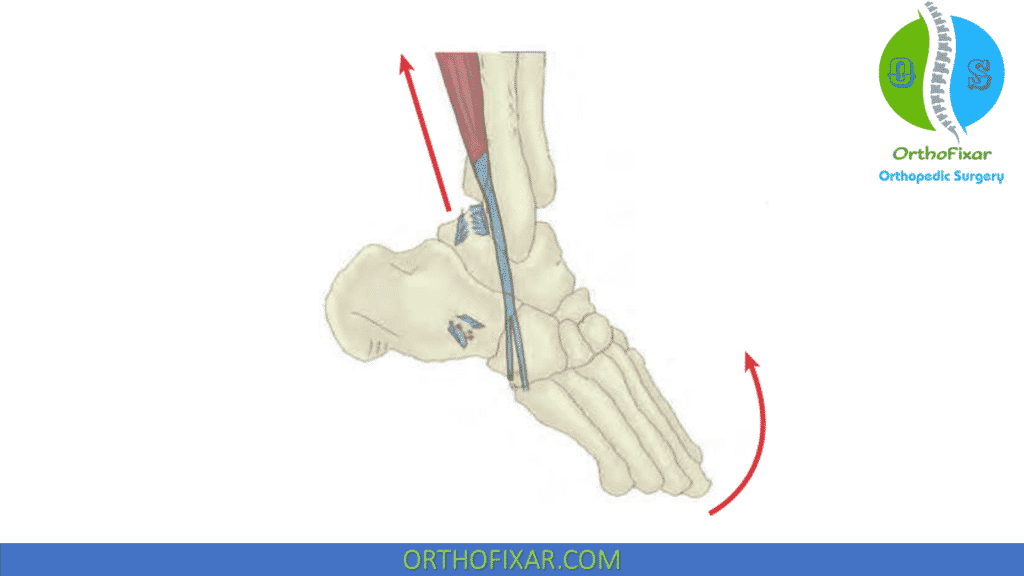
Peroneal Subluxation Risk Factor
- A flattened or convex fibular groove, pes planus, rearfoot valgus.
- Recurrent lateral ankle sprain.
- Laxity of the peroneal retinaculum.
Peroneal Dislocation Classification
There are four peroneal dislocation classifications:
- The superior peroneal retinaculum is torn from its fibular insertion.
- The superior retinaculum and fibrocartilaginous ridge are avulsed from the lateral fibula.
- The superior retinaculum is torn from the lateral fibula, the fibrocartilaginous ridge is avulsed, and flake fractures occur on the lateral malleolus.
- The superior retinaculum is torn from its calcaneal insertion.
Full or partial-thickness longitudinal tears may appear in the tendons. Longitudinal tears of the peroneus brevis tendon are frequently associated with chronic lateral ankle instability.
Clinically
Clinically, peroneus brevis tears and subluxations are differentiated from chronic lateral ankle instability based on the description and location of the symptoms:
- In the presence of peroneus brevis tendon Tendinopathy, the patient will describe lateral instability with associated pain on the posterior portion of the malleolus.
- Patients with chronic ankle instability will complain of the ankle “giving way” and pain in the anterior aspect of the ankle.
Peroneus longus tears tend to afflict older individuals and also result in pain through the foot and lateral ankle.
Swelling and ecchymosis may be isolated behind the lateral malleolus. After 24 hours post dislocation, the swelling becomes diffuse.
Tenderness behind the lateral malleolus, over the peroneal tendons, and perhaps over the site of the inferior peroneal retinaculum.
See Also: Lateral Ankle Sprain
The peroneus longus’ sesamoid, the os peroneum, can be the cause of several painful conditions about the foot and ankle. Generally termed as “painful os peroneum syndrome” (POPS), pain and dysfunction can be associated with an acute or chronic fracture, a multipartite os peroneum (the os peroneum being in two or more pieces), or a tear or rupture of the peroneus longus tendon. In rare instances, POPS can be caused by the os peroneum contacting a large peroneal tubercle. Clinically, POPS is characterized by increased lateral pain during a single stance heel rise, inversion stress test, and resisted plantarflexion of the first ray.
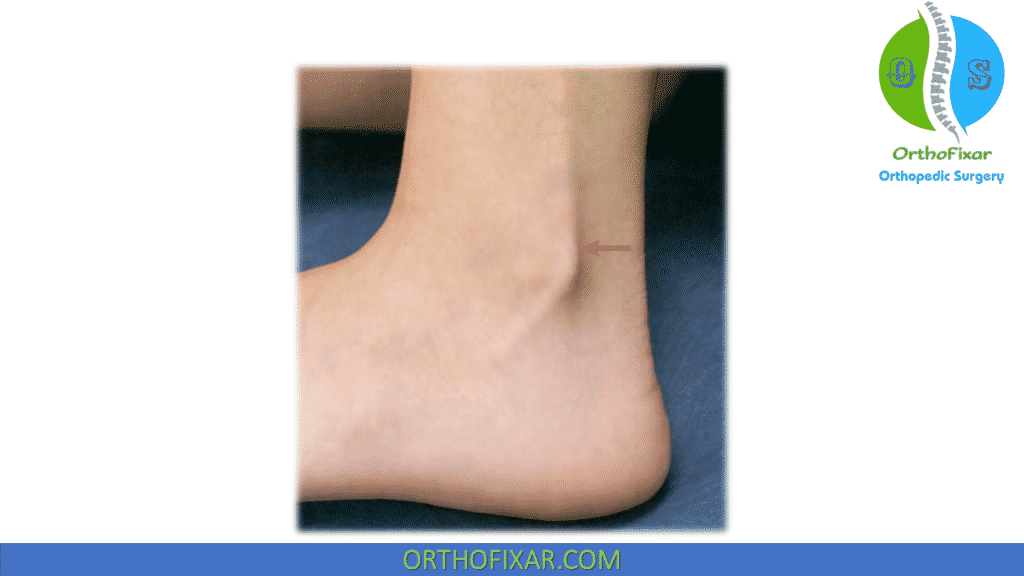
Imaging
An avulsion fracture of the lateral ridge of the distal fibula confirms the diagnosis of a peroneal tendon subluxation or dislocation.
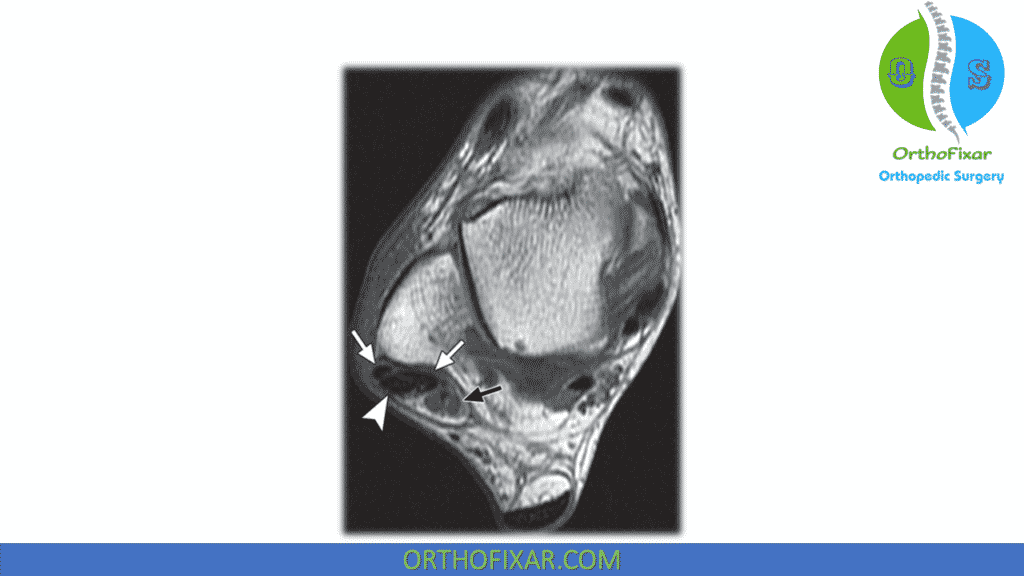
MRI is used to identify tendon lesions. Tears may be identified by a “boomerang” appearance.
Ultrasonic imaging is highly accurate in identifying peroneal tendon lesions.
Treatment
In cases in which the retinaculum is stretched, the degree of subluxation may be controlled by rehabilitation exercises, taping, and using a felt pad over the peroneal groove to help hold the tendons in place. However, after the retinaculum stretches, it does not return to its original length.
When the retinacula have been completely disrupted or pain and dysfunction become great, surgery is required to deepen the fibular groove, repair the involved retinaculum, or both.
Surgery to repair the soft tissue structures is usually necessary for patients with recurrent peroneal tendon dislocations. If the subluxation is not reduced, chronic ankle instability, pain, and decreased strength impair ankle function.
References
- Jones DC. Tendon Disorders of the Foot and Ankle. J Am Acad Orthop Surg. 1993 Nov;1(2):87-94. doi: 10.5435/00124635-199311000-00003. PMID: 10675859.
- Sammarco, GJ, and Mangone, PG: Diagnosis and treatment of peroneal tendon injuries. Foot Ankle Surg, 6:197, 2000.
- Karlsson, J, and Wiger, P: Longitudinal split of the peroneus brevis tendon and lateral ankle instability: treatment of concomitant lesions. J Athl Train, 37:463, 2002.
- Kumai, T, and Benjamin, M: The histological structure of the malleolar groove of the fibula in man: its direct bearing on the displacement of peroneal tendons and their surgical repair. J Anat, 203:257, 2003.
- Schweitzer, ME, et al: Using MR imaging to differentiate peroneal splits from other peroneal disorders. Am J Roentgenol, 168:129, 1997.
- Ferran, NA, Oliva, F, and Maffulli,N: Recurrent subluxation of the peroneal tendons. Sports Med, 36:839, 2006.
- Grant, TH, et al: Ultrasound diagnosis of peroneal tendon tears: a surgical correlation. J Bone Joint Surg, 87:1788, 2005.
- Yao, L: MR Findings in peroneal tendonopathy. J Comput Assist Tomogr, 19:460, 1995.
- Krause, JO, and Brodsky, JW: Peroneus brevis tendon tears: pathophysiology, surgical reconstruction, and clinical results. Foot Ankle Int, 19:271, 1998.
- Steensma, MR, Anderson, JG, and Bohay, DR: Update on diseases and treatment of the peroneal tendon, including peroneal tendon tear, subluxating peroneal tendon, and tendinosis. Curr Opin Orthop, 16:60, 2005.
- Boles, MA, et al: Enlarged peroneal process with peroneus longus tendon entrapment. Skeletal Radiol, 26:313, 1997.
- Magnano, GM, et al: High-resolution US of non-traumatic recurrent dislocation of the peroneal tendons: a case report. Pediatr Radiol, 28:476, 1998.
- Shellock, FG, et al: Peroneal tendons: use of kinematic MR imaging of the ankle to determine subluxation. J Magn Reson Imaging, 7:451, 1997.
- Sobel, M, et al: Painful os peroneum syndrome: a spectrum of conditions responsible for plantar lateral foot pain. Foot Ankle Int, 15:112, 1994.
- Kollias, SL, and Ferkel, RD: Fibular grooving for recurrent peroneal tendon subluxation. Am J Sports Med, 25:329, 1997.
- Karlsson, J, Eriksson, BI, and Sward, L: Recurrent dislocation of the peroneal tendons. Scand J Med Sci Sports, 6:242, 1996.