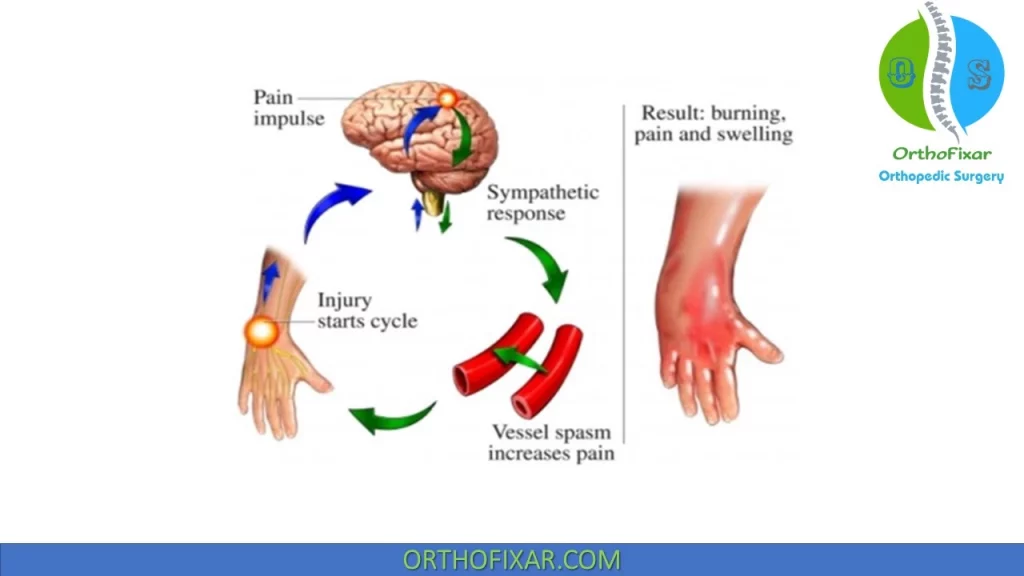
Complex regional pain syndrome (CRPS) is a chronic pain condition involving hyperalgesia and allodynia of the extremities. It’s divided into CRPS-I and CRPS-II. The pain experienced is disproportionate to the amount of tissue injury and persists beyond the expected healing time for normal tissue.
In the past, it was called Reflex sympathetic dystrophy causalgia, Sudeck atrophy, or Leriche posttraumatic syndrome. In 1994, complex regional pain syndromes term was established by the International Association for the Study of Pain.
The incidence of CRPS is:
- 1–2 % after various fractures
- 2–5 % after peripheral nerve injury,
- 7–35 % in Colles fracture.
Complex regional pain syndrome occurs most commonly in elderly patients and those with psychological or psychiatric conditions and has been reported in 8% to 35% of patients with distal radial fractures.
CRPS Etiology
There is no well-defined or complete system for explaining the etiology for causalgia. Many theories have been introduced:
- Mitchell, Morehouse, and Keen in 1867 after median neural injury occurring during the Civil War aided in defining certain characteristics, such as burning, dysesthesia, and vasomotor instability after injury.
- Sudeck delineated other features of osseous and vascular changes.
- Evans described the sympathetic instability.
More clearly explanation was that there is a local injury consequences to sensory nerves, resulting in altered vasomotor responses and aberrant afferent neural transmission, and internuncial transmission dysregulation. This alteration results in sympathetic hyperactivity.
CRPS Disease frequently does not limit itself exclusively to well-delineated dermatomes, myotomes, or sclerotomes.
Adults can present with causalgia after a fracture or trauma with immobilization. With children, it occurs most often in athletic girls (1:6, boys to girls) with an average age of 12 years.
CRPS Types
There are two types of Complex Regional Pain Syndrome that are recognized by the International Association for the Study of Pain:
CRPS Type 1:
CRPS Type 1 refers to the pain syndrome, previously termed Reflex sympathetic dystrophy RSD, which involves a pain syndrome triggered by a noxious event that is not limited to a single peripheral nerve.
CRPS Type 2:
CRPS Type 2 refers to the pain syndrome, previously termed causalgia, which involves a pain syndrome that involves direct partial or complete injury to a nerve or one of its major branches.
More recently, it has been suggested that a third type may exist. This type is characterized by irreversible changes in the skin and bones, marked muscle atrophy, unyielding pain, and severely limited mobility of the affected area.
CRPS Stages
| Stage 1 | – Burning, aching, tenderness, joint stiffness – Swelling, temperature changes – ↑ nail growth & ↑ hair on foot/feet |
| Stage 2 | – ↑ Pain, swelling, joint stiffness – Pain becomes less localized – Change in skin color & texture |
| Stage 3 | – Pain radiates all the way up the leg – ↓ Nerve conduction velocity – Muscle atrophy |
CRPS Symptoms
The signs and symptoms for both causalgia types include:
The pain of type I CRPS is classified as sympathetically maintained pain or sympathetically independent pain, where sympathetically maintained pain is characterized by an abnormal reaction of the sympathetic nervous system.
Pain is not necessarily located in an area corresponding to the cutaneous distribution of the nerve. Another characteristic of the pain, particularly in major causalgia, is accentuation by stimuli to such emotions as surprise and anger and by other disturbances in the patients’ environment.
The edema, which can be pitting or nonpitting, is often present throughout all stages of CRPS and may be the result of vasomotor instability coupled with a lack of motion.
The stiffness is one of the components of type 1 that increases with time and is due to increased fibrosis in the ligamentous structures and adhesion formation around the tendons.
The diagnosis of CRPS is made from the physical examination and the patient’s medical history, which may include past events of trauma, persistent pain, hyperalgesia, allodynia (perception of a nonpainful stimulus as painful), edema, and diminished function of the area.
The type of pain and its duration are perhaps the most important diagnostic signs. The pain is typically burning in nature and is of a much longer duration than would be expected from the injury.
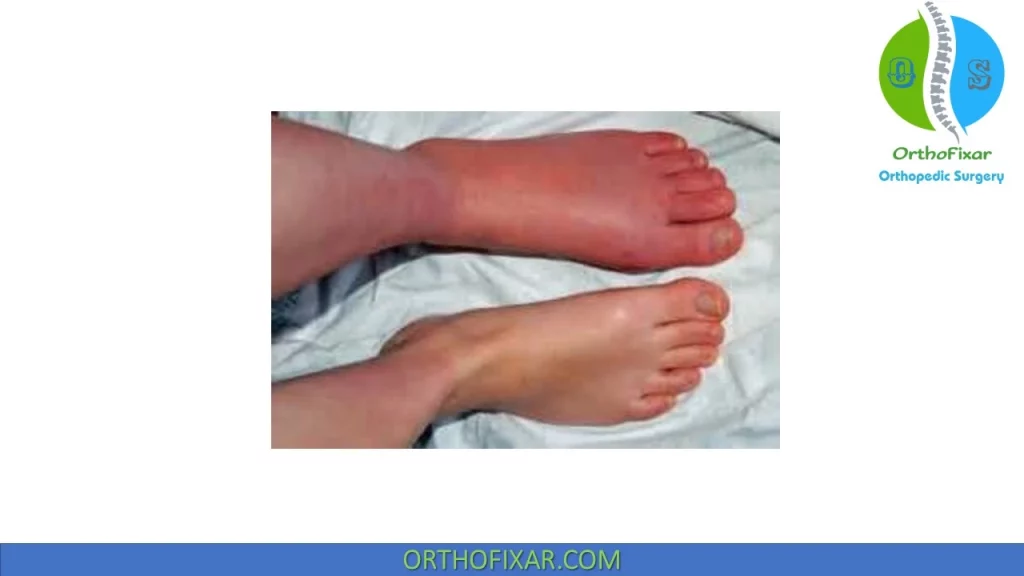
CRPS Clinical Phases
CRPS 1 has been subdivided into three clinical phases:
1. Acute inflammatory phase:
An acute inflammatory phase that can last from 10 days to 2–3 months. The acute stage of CRPS lasts from 1 to 3 months. This stage is reversible if the patient is treated. The affected limb becomes flushed, warm, and dry because regional blood vessels are relaxed, and stimulation of the sweat glands is reduced. The pain is diffuse, severe, and constant with a burning, throbbing, or aching quality. Edema and increased hair and nail growth can also occur. By the end of this stage, the limb turns cold, sweaty, and cyanotic from vasoconstriction caused by paradoxical
sympathetic stimulation.
2. Vasomotor Instability phase:
A phase of vasomotor instability that can last for several months. This is the dystrophic stage, which lasts another 3–6 months. Constricted blood vessels can cool limb temperature by nearly 10 degrees. The area will be pale, mottled, edematous, and sweaty. Pain remains continuous, burning, or throbbing but is more severe. Nails may crack or become brittle and heavily grooved. Limb movement is limited by muscle wasting and joint stiffness. Osteoporosis and contractures can develop.
3. Cold End Phase:
The atrophic stage is characterized by irreversible damage to muscles and joints. Over the next 2–3 months the bones atrophy and the joints become weak, stiff, or even ankylosed. The pain lessens and may become spasmodic or breakthrough but is no longer mediated by the sympathetic nervous system. The skin is cool and looks glossy and pale or cyanotic.
A prospective study of 829 patients indicated that the following:
- In its early phase, CRPS is characterized by regional inflammation and not of a disturbance of the sympathetic nervous system. The regional inflammation increases after muscular exercise.
- Tremor was found in 49 percent and muscular incoordination in 54 percent of patients.
- Sympathetic signs such as hyperhidrosis are infrequent. These data support the concept of an exaggerated regional inflammatory response to injury or operation in CRPS.
Laboratory & Imaging Study
There are no laboratory studies that are diagnostic for causalgia.
The use of quantitative sensory and autonomic testing, quantitative sudomotor axonal reflex testing, thermography, and bone scans has been described.
Mackinnon and Holder showed that a three-phase radionuclide bone scan can aid in the early diagnosis of reflex sympathetic dystrophy. A diffusely increased uptake in the delayed images was found to be diagnostic of reflex sympathetic dystrophy with a sensitivity of 96% and a specificity of 98%. A bone scan may be helpful if positive in a nontraumatic patient.
MRI changes have been described in early CRPS phases, with muscle edema, interstitial edema, and hyperpermeability, but again this modality is not considered consistently a definitive resource.
Thus, the diagnosis remains clinical.
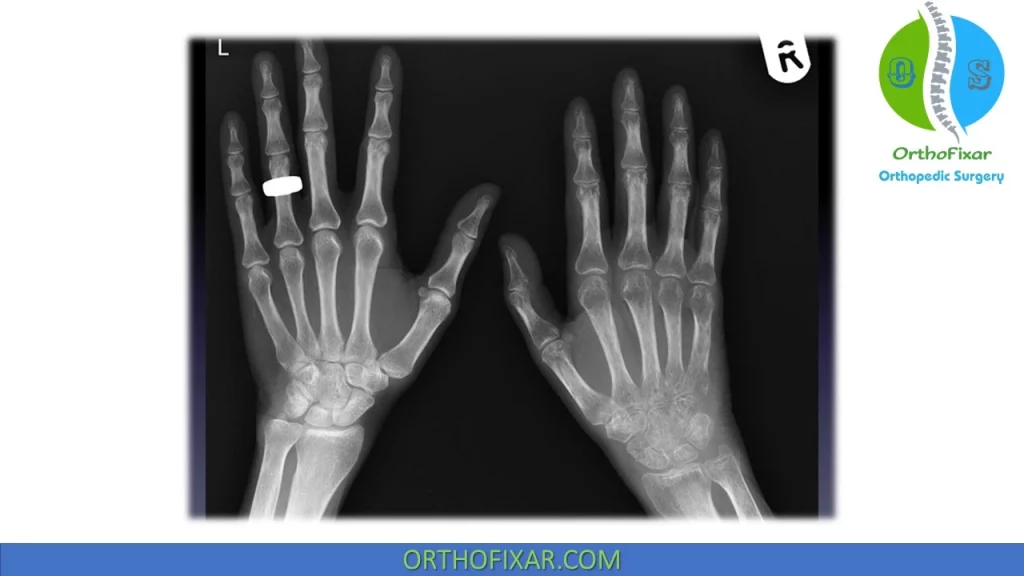
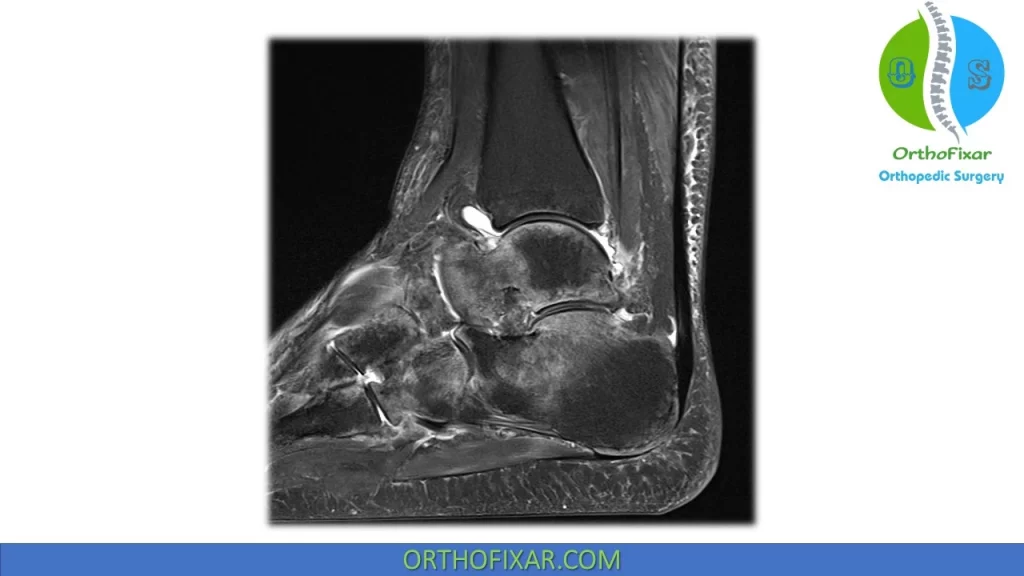
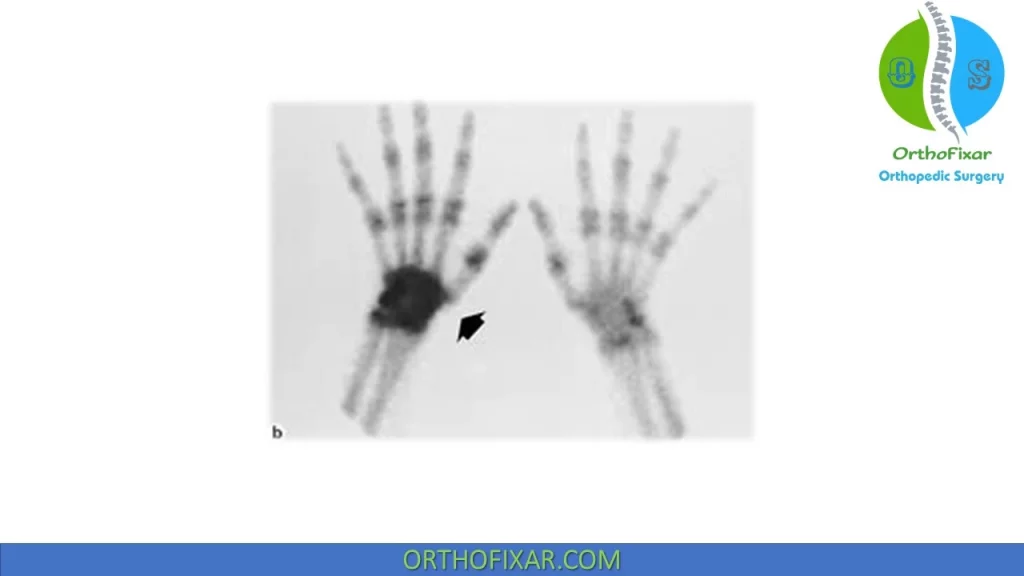
CRPS Differential Diagnosis
A number of other conditions need to be ruled out before establishing a diagnosis of CRPS type 1, and these include, but are not limited to the following:
- Rheumatoid and septic arthritis
- Gout
- Disk herniation
- Peripheral neuropathy
- Peripheral nerve entrapment
- Peripheral vascular disease.
CRPS Treatment
No regimen has been completely satisfactory in treating Complex Regional Pain Syndrome.
Comprehensive multidisciplinary approach is optimal with help from specialists in neurology, physical or occupational therapy, physical medicine, pain management, and psychology as required.
Medications used in CRPS Treatment include:
- anti-inflammatory medication,
- analgesics (oral or topical),
- tricyclic antidepressants,
- selective serotonin reuptake inhibitors,
- anticonvulsants,
- antidepressants.
Interventional options used in CRPS treatment include:
- selective peripheral neural blocks,
- trigger point injections,
- sympathetic blocks (single or indwelling),
- dorsal column stimulators,
- and rarely sympathectomies (chemical or surgical).
A randomized, controlled, multicenter study involving 416 patients with 427 distal radial fractures determined that vitamin C (500 mg daily) can reduce the prevalence of CRPS, and this was listed as having “adequate evidence to support a moderately strong endorsement” in the recent AAOS clinical practice guidelines for distal radial fractures.
Complex Regional Pain Syndrome Physical Therapy
Physical therapy is the first line of intervention, whether it be the sole intervention or performed immediately following a nerve block.
The most important rule is to minimize pain while employing physical therapy. When excessive pain is created, sympathetically mediated pain may worsen.339 It is vital to not reinjure the region or aggravate the problem with aggressive physical rehabilitation.
Therapy should be directed not only to all the joints of the involved extremity but also include more generalized movement patterns.
The patient’s involved limb must be elevated as often as possible to counteract the vascular stasis and actively mobilized several times per day.
Recovery from muscle dysfunction, swelling, and joint stiffness requires appropriate physical activity and exercise, and pressure and motion are necessary to maintain joint movement and prevent stiffening. The progression should occur slowly and gently with strengthening, active assisted range-of-motion, and AROM exercises.
Weight-bearing exercises and active stress loading exercises should also be incorporated. Active stress loading exercises include scrubbing and carrying. Scrubbing is a form of closed kinetic chain exercise for the upper or lower extremity in which the patient in a variety of positions performs a scrubbing action on a firm surface. As its name suggests, carrying exercises for the upper extremity involve having the patient carry small objects in the hand on the affected side and gradually increasing the weight of the object. For the lower extremity stress loading can be achieved through weight bearing.
Sensory threshold techniques can be used. These include fluidotherapy, vibration desensitization, transcutaneous electrical nerve stimulation, contrast baths, and desensitization using light and heavy pressure of various textures over the sensitive area.
Case Study
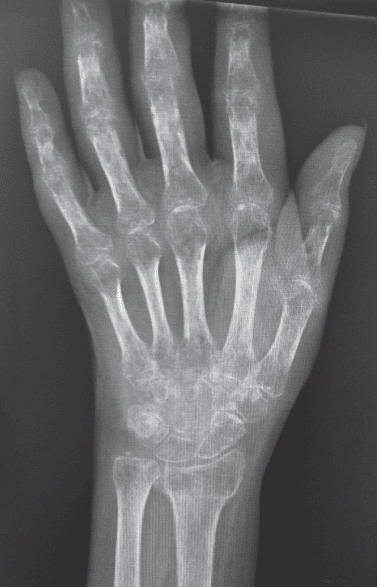
38-year-old woman presents with a 4-month history of pain, stiffness, decreased strength, and an inability to return to work after experiencing a minor work-related injury in which her hand and wrist were caught between a sliding glass steel door and its frame. She has no abrasions or external signs of trauma, and plain radiographs are negative. At the time of injury, a physical examination revealed diffuse tenderness on palpation of the dorsal carpus. A physical examination on presentation to the office reveals a bright glassy complexion to the skin, passive and active digital stiffness in attempted flexion, diffuse tenderness on palpation of the dorsal and volar carpus, and decreased objective two-point discrimination in the median nerve distribution.
Description of the Problem
Subacute, nonspecific signs and symptoms consisting of pain, tenderness, digital stiffness, and skin discoloration and tightness are highly suggestive of complex regional pain syndrome type 1 (CRSP type1). The diagnosis is one of exclusion—bony, ligamentous, and tendon injuries should be ruled out by clinical examination and appropriate imaging; peripheral nerve injury and compression syndromes should be ruled out by clinical examination and electrophysiologic assessment; and vascular injury should be ruled out by clinical examination and either noninvasive or invasive studies, as indicated.
Once a correctable cause has been ruled out, CRPS1 can be diagnosed. A three-phase bone scan has been used historically for diagnosis, but presently its usefulness is open to debate.
A differential diagnosis includes:
- carpal tunnel compression of the median nerve,
- radial sensory nerve neuritis,
- lateral antebrachial sensory nerve neuritis,
- Guyon canal compression of the ulnar nerve ,
- ulnar or radial artery injury,
- injury to the metacarpus, the carpus, or the distal radius and ulna.
- Tendinosis or tendinitis of the first dorsal compartment, the sixth dorsal compartment, and the flexor carpi radialis should be considered.
A diagnosis is based on a clinical examination and the observation of diffuse osteopenia on plain radiographs, with normal vascular and electrophysiologic assessments. An MRI of the affected area can be useful to rule out structural lesions.
Imaging studies include plain radiographs of the hand and wrist, electrophysiologic assessment, MRI (optional), three-phase bone scan (optional), and vascular studies (optional).
Treatment
The initial treatment should focus on evaluation and treatment of any structural lesion causing the pain syndrome to persist. Most frequently, this consists of relieving compression of the median nerve in the carpal tunnel (thus a diagnosis of CRPS2 is appropriate) by a carpal tunnel release. Other modalities such as sympathetic ganglion (stellate ganglion) blocks, oral medications (gabapentin and antidepressants) can be attempted. The stiff digits and thumb can be mobilized while the patient is anesthetized.
Q&A for Patients
What causes complex regional pain syndrome?
Trauma is the major cause of the CRPS disease, other causes include surgery and prolonged immobilization.
What is the first line of treatment for CRPS?
The first line of treatment for CRPS is physical therapy.
Does CRPS show up on MRI?
MRI can’t confirm the diagnosis of CRPS, but it can rule out other causes of the symptoms.
What vitamin prevents CRPS?
Vitamin C can prevent the prevalence of CRPS as a daily dose of 500mg for 50 days after the injury.
References
- Zollinger PE, Tuinebreijer WE, Breederveld RS, Kreis RW: Can vitamin C prevent complex regional pain syndrome in patients with wrist fractures? A randomized, controlled, multicenter dose-response study, J Bone Joint Surg 89A:1424, 2007. PMID: 17606778
- Veldman PHJM, Reynen HM, Arntz IE, et al: Signs and symptoms of reflex sympathetic dystrophy: Prospective study of 829 patients. Lancet 342:1012–1016, 1993.
- Metules TJ: When a simple fall turns into years of pain. RN 63:65–66, 2000.
- Bohm E: Das Sudecksche Syndrom. Hefte Unfallheilkd 174:241–250, 1985.
- Omer GC, Thomas MS: Treatment of causalgia. Tex Med 67:93–96, 1971.
- Atkins RM, Duckworth T, Kanis JA. Features of algodystrophy after Colles’ fracture. J Bone Joint Surg Br. 1990 Jan;72(1):105-10. doi: 10.1302/0301-620X.72B1.2298766. PMID: 2298766.
- Acquaviva P, Schiano A, Harnden P, et al: Les algodystrophies: terrain et facteurs pathogeniques. Resultats dune enquete multicentrique portant
- sur 765 observations (Rapport). Rev Rhum Mal Osteoartic 49:761–766, 1982.
- Dunn D. Chronic regional pain syndrome, type 1: Part I. AORN J. 2000 Sep;72(3):422-32, 435-49; quiz 452-8. PMID: 11004961.
- Maurer G: Umbau, Dystrophie und Atrophie an den Gliedmassen (Sogenannte Sudecksche Knochenatrophie). Erg Chir 33:476–531, 1940.
- STEINBROCKER O. The shoulder-hand syndrome; associated painful homolateral disability of the shoulder and hand with swelling and atrophy of the hand. Am J Med. 1947 Oct;3(4):402-7. doi: 10.1016/0002-9343(47)90170-8. PMID: 20264705.
- Sudeck P: Ueber die acute entzundliche Knochenatrophie. Arch Klin Chir 62:147–156, 1900.
- Walker SM, Cousins MJ. Complex regional pain syndromes: including “reflex sympathetic dystrophy” and “causalgia”. Anaesth Intensive Care. 1997 Apr;25(2):113-25. doi: 10.1177/0310057X9702500202. PMID: 9127652.
- Kingery WS: A critical review of controlled clinical trials for peripheral neuropathic pain and complex regional pain syndromes. Pain 73:123– 139, 1997.
- Wilson PR: Post-traumatic upper extremity reflex sympathetic dystrophy: Clinical course, staging, and classification of clinical forms. Hand Clin 13:367–372, 1997.
- Gordon N: Review article: Reflex sympathetic dystrophy. Brain Dev 18:257–262, 1996
- Dutton’s Orthopaedic Examination, Evaluation, And Intervention 3rd Edition.
- Campbel’s Operative Orthopaedics 12th edition Book.
- Millers Review of Orthopaedics -7th Edition Book.