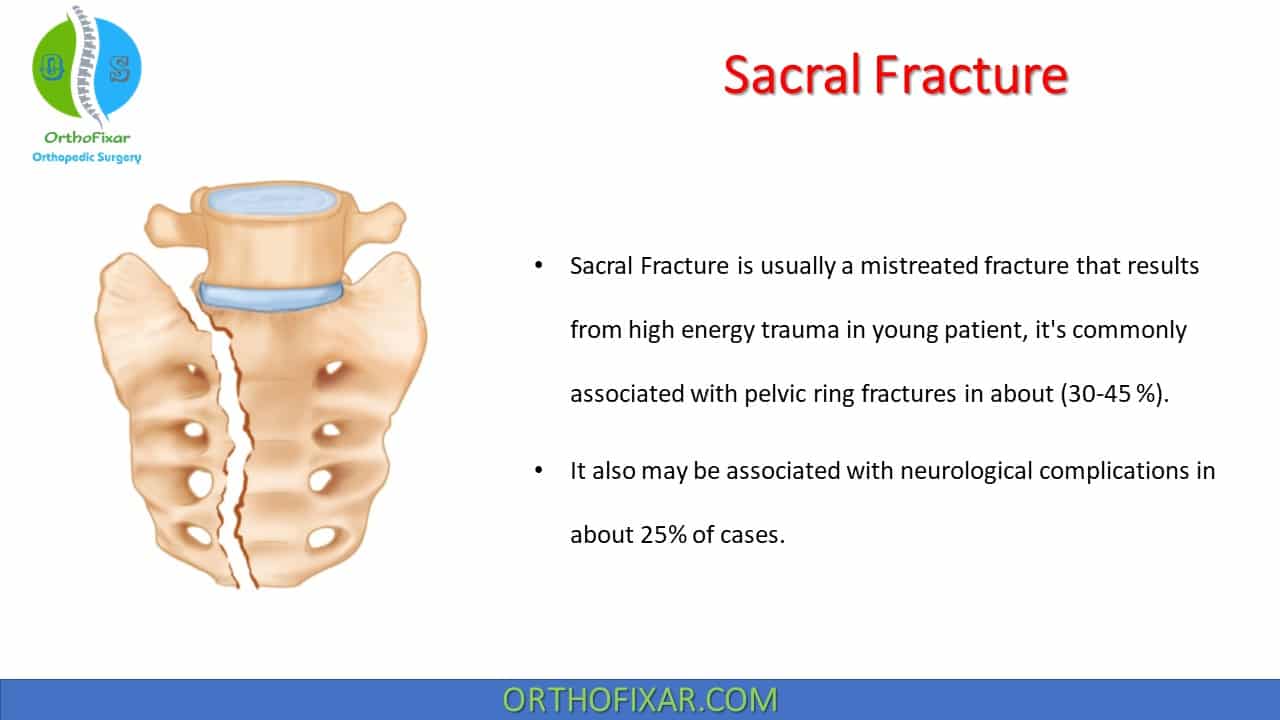
Sacral Fracture is usually a mistreated fracture that results from high energy trauma in young patient, it’s commonly associated with pelvic ring fractures in about (30-45 %).
It also may be associated with neurological complications in about 25% of cases.
See Also: Pelvic Fractures
Sacral Anatomy
The sacrum is formed by fusion of 5 sacral vertebrae.
Proximally it articulates with the 5th lumbar vertebra, while distally it articulates with the coccyx. Laterally, it articulates with the ilium at sacroiliac joints (SI).
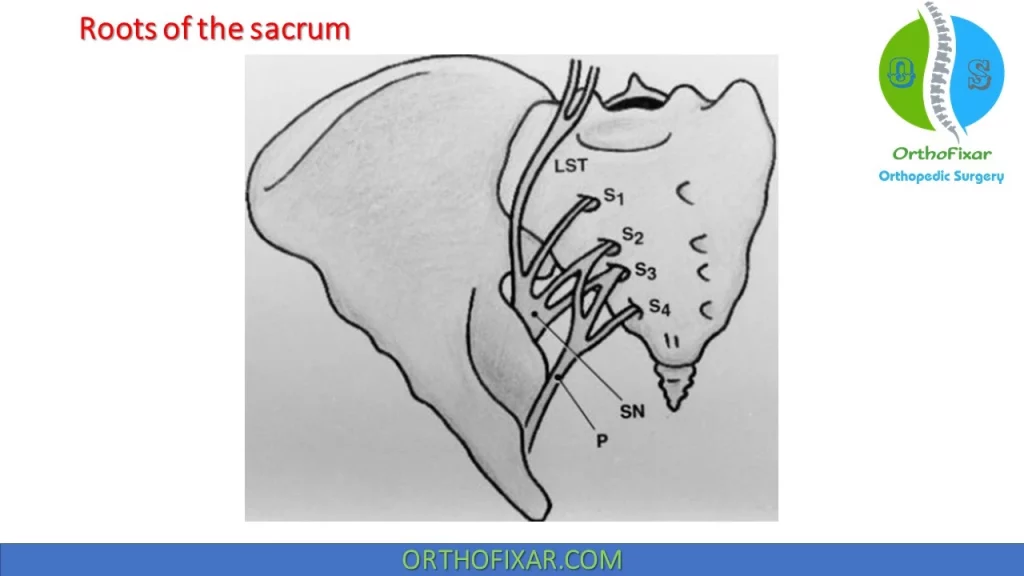
Four pairs of pelvic sacral foramina located both anteriorly and posteriorly transmit respective ventral and dorsal branches of the upper four sacral nerves (S1-S4) , while L5 nerve root runs on top of sacral ala.
The sacrum plays a central role in the stability of both the pelvis and the spinal column. The complex of ligaments that invest the sacrum anteriorly and posteriorly, the ligaments of the pelvic floor, and the osseous structure of the sacrum and pelvis all contribute to lumbopelvic stability and help prevent injury to the neurovascular structures in the region.
Sacral Fracture Classification
Sacral Fracture is classified based on fracture location relative to foramen.
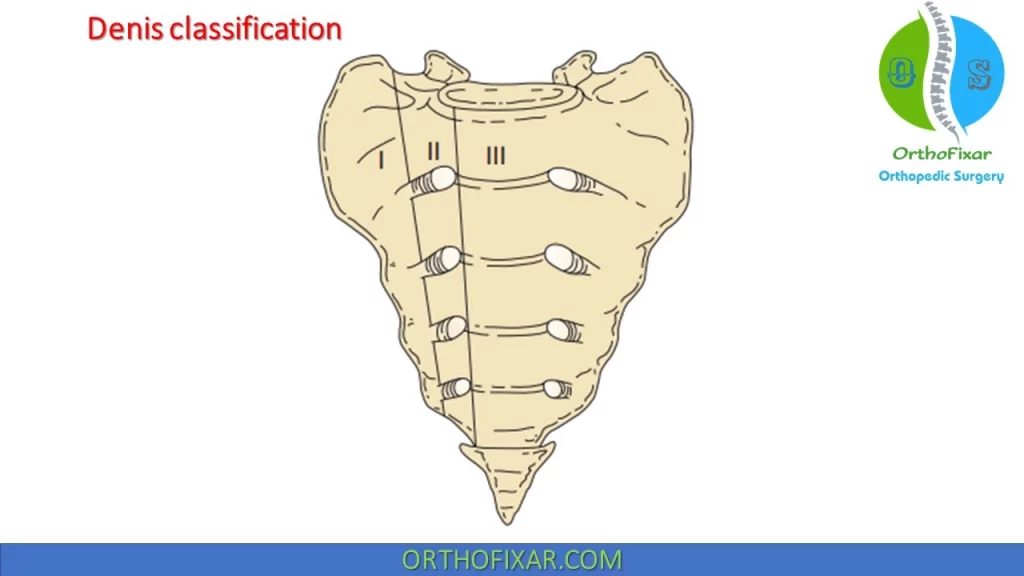
Denis classification of Sacral Fracture:
| Type | Charactaristics | Nerve Injury |
|---|---|---|
| Type I | Fractures occur lateral to the neural foramina through the sacral ala. | Rare (5%) |
| Type II | Fractures are transforaminal, it may be Stable / unstable (increased risk of nonunion). | 28% |
| Type III | Fractures occur medial or central to the neural foramina | High (60%) |
Transverse fractures of the sacrum are classified as type III injuries because they involve the spinal canal and often are H or U shaped (so-called jumper’s fracture because of their association with falls from heights).

Roy-Camille and Strange-Vognsen and Lebech subclassifications of Denis zone 3 fractures:
- Type 1: angulation with no translation;
- Type 2: angulation and translation;
- Type 3: complete displacement of cephalad and caudal sacrum;
- Type 4: segmental comminution.

See Also: Subtrochanteric femur fracture’s most common deformity after antegrade nailing
Sacral Fracture Symptoms
History of high energy trauma, pelvic pain.
The examiner should do a full neurovascular examination and assess for pelvic ring fracture.
The neurological evaluation must include a rectal examination to assess rectal tone and maximal contraction of the anal sphincter.
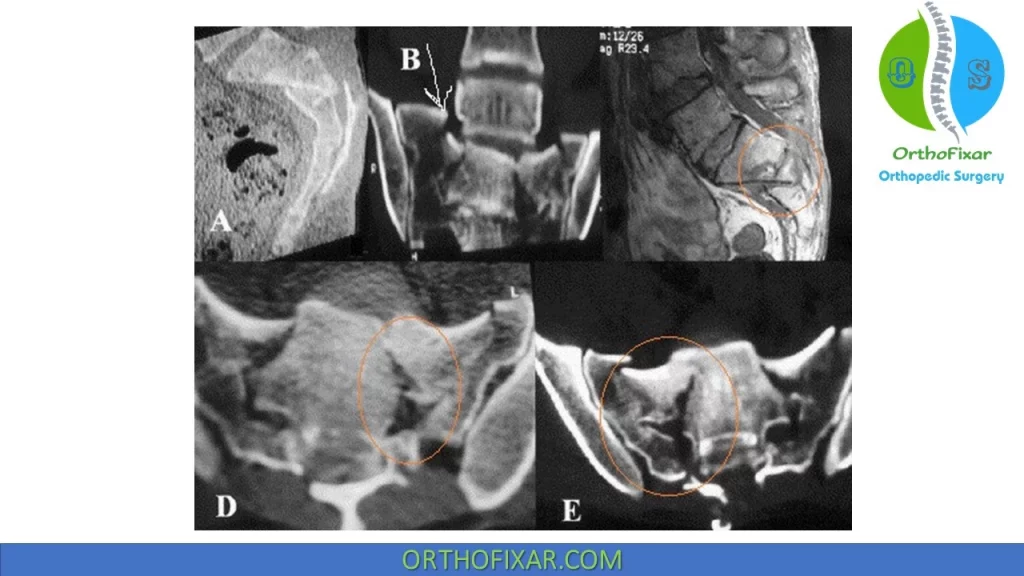
Sacral Fracture Radiology
Recommended Views include AP pelvis view, inlet view, outlet view, and lateral view.
CT scan is usually required.
MRI is required when neurological injury is suspected.
Sacral Fracture Treatment
Nonoperative sacral injury treatment is indicated for stable and minimally displaced fractures, these include:
- Weight bearing as tolerated for incomplete fractures in which the ilium is contiguous with the intact sacrum (e.g., anterior impaction fractures from lateral compression mechanism or isolated sacral ala fractures).
- Touch-toe weight bearing for complete fractures.
Surgical treatment is indicated for displaced fractures (>1 cm), these include:
- Percutaneous iliosacral screws: Before surgery, appropriate fluoroscopic visualization of anatomic landmarks should be made. The pelvic outlet radiograph allows optimal visualization of the S1 neural foramina to avoid injury, while the lateral sacral view identifies the sacral ala slope and minimizes risk to the L5 nerve root. There is high incidence of sacral dysmorphism (20%-44% – Sacralization of L5 or lumbarization of S1). Risk of anterior screw penetration causing neurologic injury is much higher with anterosuperior sacral concavity.
- Posterior plating.
- Transiliac sacral bars.
- Open foraminal decompression considered for neurologic injury associated with zone II fracture.
In low-energy fractures, sacral ala fracture treatment with iliosacral screw fixation, feasible in both the S1 and S2 corridor

Complications
- Neurologic injury: Highest incidence with displaced zone II fractures. The L5 nerve root usually involved with zone II fractures. Cauda equina syndrome can be associated with zone III injuries.
- Chronic low back pain.
- Malunion.
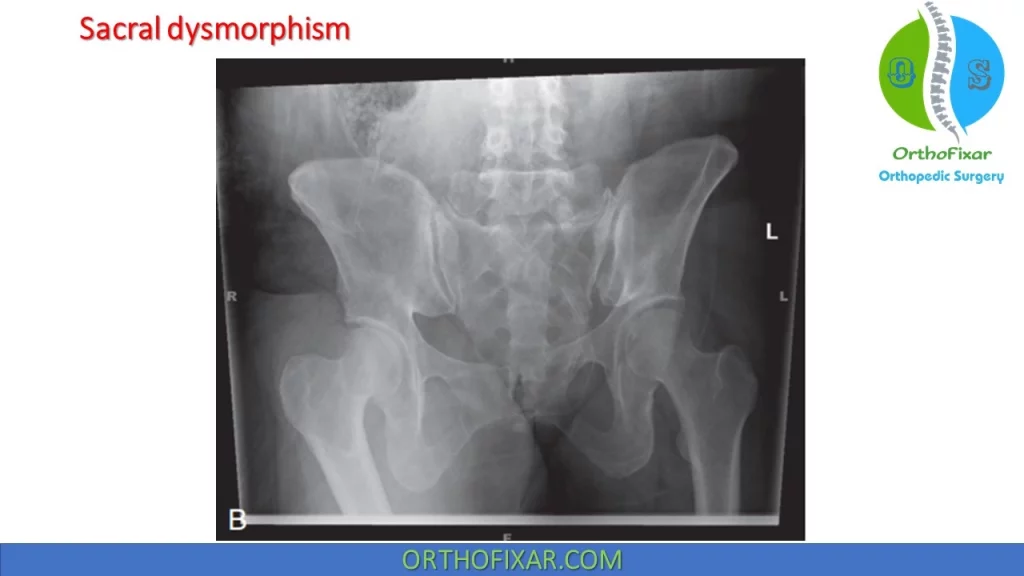
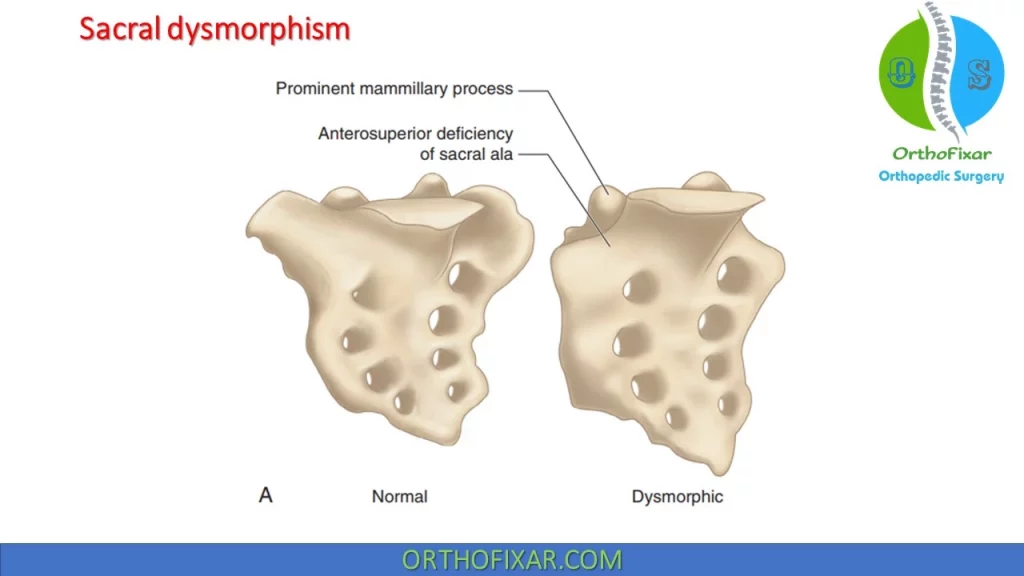
Sacral Dysmorphism:
Sacral dysmorphism is seen as a complication of percutaneous iliosacral screws treatment, where either Sacralization of L5 or lumbarization of S1 is happened.
The incidence is 20%-44%.
Radiographic signs of sacral dysmorphism best seen on outlet view:
- Prominent mammillary processes.
- Laterally downsloping sacral ala.
- Residual vestigial disc space between S1 and S2.
- Top of iliac wing at level of L5/S1 instead of at L4/5.
- Noncircular S1 anterior neural tunnel.
Radiographic signs of sacral dysmorphism best seen on axial CT scan:
- Peaked or prow-shaped sacral promontory.
- Tongue-in-groove sacroiliac articulation.
- Oblique and narrow S1 sacral ala.
- Wider S2 alar channel.
References & More
- Rizkalla JM, Lines T, Nimmons S. Classifications in Brief: The Denis Classification of Sacral Fractures. Clin Orthop Relat Res. 2019 Sep;477(9):2178-2181. doi: 10.1097/CORR.0000000000000861. PMID: 31389896; PMCID: PMC7000068.
- Santolini E, Kanakaris NK, Giannoudis PV. Sacral fractures: issues, challenges, solutions. EFORT Open Rev. 2020 May 5;5(5):299-311. doi: 10.1302/2058-5241.5.190064. PMID: 32509335; PMCID: PMC7265089.
- Byun, Young-Soo & Chang, Se-Ang. (2011). Sacral Fractures. Journal of the Korean Fracture Society. 24. 371. 10.12671/jkfs.2011.24.4.371.
- Campbel’s Operative Orthopaedics 12th edition Book.
- Millers Review of Orthopaedics -7th Edition Book.