What is Mallet Finger?
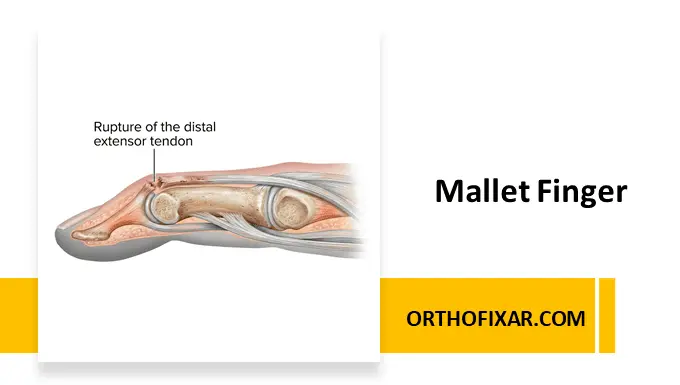
Mallet finger is a common hand injury characterized by the inability to actively extend the distal interphalangeal (DIP) joint, resulting in a flexed fingertip deformity. It occurs due to disruption of the terminal extensor tendon at its insertion on the distal phalanx, either from tendon rupture or bony avulsion.
This injury is also known as:
- Baseball finger
- Drop finger
Anatomy and Pathophysiology
The extensor mechanism of the finger inserts into the distal phalanx via the terminal tendon. When this structure is disrupted, the balance between flexor and extensor forces is lost, leading to unopposed flexion at the DIP joint.
Two main types exist:
- Soft tissue mallet finger: rupture of the extensor tendon
- Bony mallet finger: avulsion fracture of the distal phalanx
If untreated, the deformity may progress to a swan neck deformity (PIP hyperextension + DIP flexion).
See Also: Hand Anatomy: Bones & Muscles
Causes and Mechanism of Injury
Mallet finger typically results from:
- Sudden forced flexion of an extended fingertip
- Direct trauma (e.g., ball striking the finger)
- Crush injuries or lacerations
- Hyperextension injuries (less common)
This mechanism leads to failure of the terminal extensor tendon.
Common scenarios:
- Sports (baseball, basketball, volleyball)
- Occupational injuries
- Simple daily activities (e.g., pulling socks)
See Also: Extensor Tendon Injury of the Hand
Epidemiology
- Frequently affects young to middle-aged individuals
- More common in men due to higher exposure to trauma
- Commonly involves:
- Middle finger
- Ring finger
- Small finger
Clinical Presentation
Key Symptoms
- Inability to actively extend the fingertip
- Pain and swelling over the DIP joint
- Visible drooping of the distal phalanx
Physical Examination Findings
- DIP joint rests in flexion
- Passive extension is possible but cannot be maintained
- Tenderness over dorsal distal phalanx
Diagnosis
Clinical Diagnosis
Mallet finger is primarily diagnosed clinically based on deformity and loss of extension.
Imaging
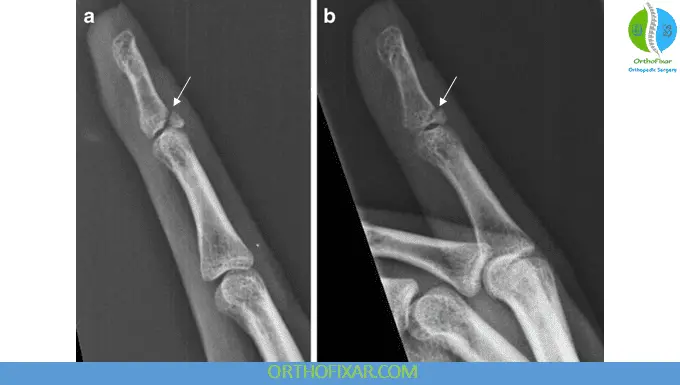
- X-rays are essential to:
- Identify avulsion fractures
- Assess joint alignment
- Detect subluxation of the DIP joint
Classification
Common classification systems include:
- Soft tissue vs. bony mallet
- Acute vs. chronic
- Acute: < 4 weeks
- Chronic: > 4 weeks
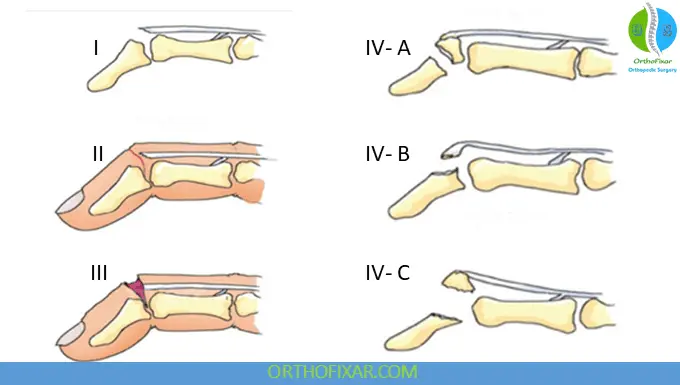
Doyle’s Classification of Mallet Finger Injuries
| Type I | Closed injury with or without small dorsal avulsion fracture |
| Type II | Open injury (laceration) |
| Type III | Open injury (deep soft tissue abrasion involving loss of skin and tendon substance) |
| Type IV | Mallet fracture: A = distal phalanx physeal injury (pediatrics) B = fracture fragment involving 20% to 50% of articular surface (adult) C = fracture fragment >50% of articular surface (adult) |
Treatment of Mallet Finger
1. Non-Surgical Treatment (First-Line)
The majority of cases are treated conservatively.
Splinting
- Continuous DIP joint extension splinting
- Duration:
- Typically 6–8 weeks, sometimes up to 12 weeks
- Only the DIP joint is immobilized
Key Principles
- Strict compliance is critical
- Any flexion during treatment may delay healing
Evidence Insight:
Splinting is effective in most uncomplicated cases, with comparable outcomes across different splint types.
2. Surgical Treatment
Surgery is reserved for specific indications:
Indications
- Open injuries
- Large bony fragment (>30–50% joint surface)
- DIP joint subluxation
- Failed conservative treatment
- Chronic deformity with functional deficit
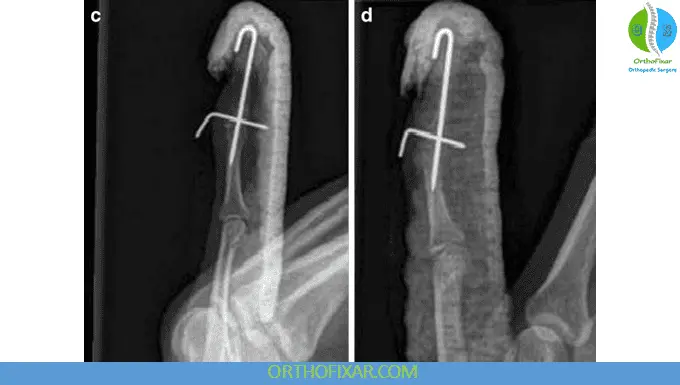
Surgical Options
- Kirschner wire fixation
- Extension block pinning
- Screw fixation
- Tendon reconstruction
Complications
Potential complications include:
- Residual extensor lag
- Skin breakdown from splints
- Joint stiffness
- Swan neck deformity (if untreated)
Prognosis
- Most patients achieve good functional outcomes with proper treatment
- Mild residual extension lag is common but usually not functionally limiting
- Early treatment improves outcomes
Key Takeaways
- Mallet finger is a terminal extensor tendon injury at the DIP joint
- Usually caused by forced flexion trauma
- Splinting is the gold standard for most cases
- Surgery is reserved for complicated injuries
- Early diagnosis and compliance are critical for optimal outcomes
References & More
- Khera B, Chang C, Bhat W. An overview of mallet finger injuries. Acta Biomed. 2021 Nov 3;92(5):e2021246. doi: 10.23750/abm.v92i5.11731. PMID: 34738569; PMCID: PMC8689306. Pubmed
- Beutel BG, Waseem M. Mallet Finger Injuries. [Updated 2025 Jul 6]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: Pubmed
- Smit JM, Beets MR, Zeebregts CJ, Rood A, Welters CFM. Treatment options for mallet finger: a review. Plast Reconstr Surg. 2010 Nov;126(5):1624-1629. doi: 10.1097/PRS.0b013e3181ef8ec8. PMID: 21042117. Pubmed
- Alla SR, Deal ND, Dempsey IJ. Current concepts: mallet finger. Hand (N Y). 2014 Jun;9(2):138-44. doi: 10.1007/s11552-014-9609-y. PMID: 24839413; PMCID: PMC4022957. Pubmed
- Egol KA. Handbook of fractures. 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2019.