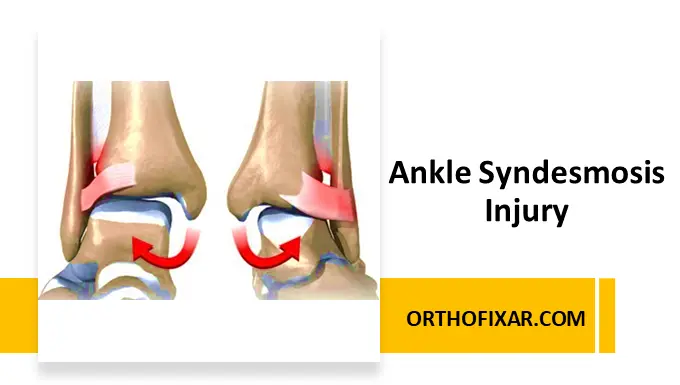
An Ankle Syndesmosis Injury, commonly called a high ankle sprain, involves injury to the distal tibiofibular syndesmotic ligaments that stabilize the ankle mortise. These injuries are clinically important because they often produce prolonged disability compared with routine lateral ankle sprains.
Syndesmotic sprains account for approximately 1% of all ankle sprains, although the true incidence is likely underestimated because many injuries remain undiagnosed. Chronic untreated syndesmotic instability may result in persistent ankle pain, impaired athletic performance, and early degenerative changes.
In athletes, syndesmotic injuries result in substantially greater time lost from sports participation compared with isolated lateral ligament injuries.
Anatomy of the Distal Tibiofibular Syndesmosis
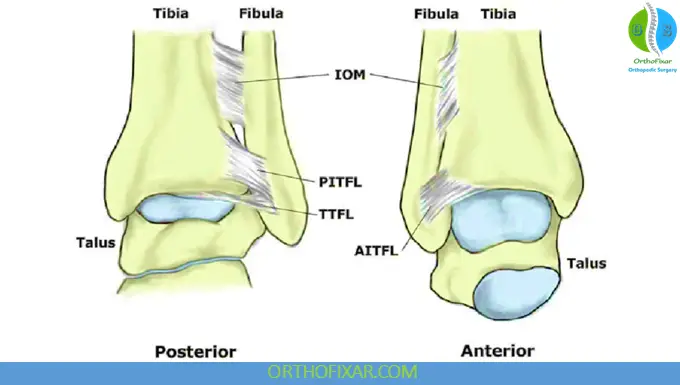
The distal tibiofibular syndesmosis is a fibrous articulation between the distal tibia and fibula that maintains ankle stability.
The primary stabilizing structures include:
- Anterior inferior tibiofibular ligament (AITFL)
- Posterior inferior tibiofibular ligament (PITFL)
- Interosseous ligament
- Interosseous membrane
- Inferior transverse ligament
These structures resist:
- External rotational forces
- Axial loading
- Fibular translation
Disruption of the syndesmosis compromises ankle mortise congruency and may lead to talar instability.
See Also: Ankle Anatomy
Mechanism of Injury
Most syndesmotic injuries occur through:
- Forced external rotation of the foot
- Hyperdorsiflexion
- Axial loading on a planted foot
Common settings include:
- Football
- Rugby
- Soccer
- Skiing
- Wrestling
Syndesmotic sprains may occur:
- Without fracture
- With associated malleolar fractures
- With frank diastasis of the distal tibiofibular joint
See Also: Ankle Fractures: Classification, Diagnosis & Treatment
Classification of Syndesmotic Injuries
Diastases of the distal tibiofibular syndesmosis were classified by Edwards and DeLee into four types:
Type I
- Lateral subluxation without fracture
Type II
- Lateral subluxation with plastic deformation of the fibula
Type III
- Posterior subluxation or dislocation of the fibula
Type IV
- Superior subluxation or dislocation of the talus within the ankle mortise
Clinical Presentation
Patients with acute syndesmotic injuries typically present with:
- Difficulty weight bearing
- Pain above the ankle joint
- Swelling
- Ecchymosis extending proximally up the leg
- Pain during push-off phase of gait
Immediately after injury, tenderness may be localized over the syndesmosis. However, progressive swelling and bruising often obscure the exact injury site.
Chronic or subtle syndesmotic injuries may present with:
- Persistent vague ankle pain
- Pain during athletic activities
- Normal routine radiographs
- Recurrent instability symptoms
Physical Examination
Clinical examination should include careful palpation of:
- Anterior inferior tibiofibular ligament
- Posterior syndesmotic region
- Fibular shaft
- Proximal tibiofibular joint
- Medial ankle structures
The fibula should be palpated from proximal to distal to exclude associated proximal fibular injuries such as a Maisonneuve fracture.
Special Tests for Syndesmotic Injury
Squeeze Test
The squeeze test is performed by compressing the tibia and fibula together at the mid-calf. Pain reproduced at the distal tibiofibular syndesmosis suggests syndesmotic ligament injury.
External Rotation Stress Test
The patient sits with the knee flexed to 90 degrees while the examiner externally rotates the foot relative to the stabilized leg. Pain over the syndesmosis during external rotation indicates probable syndesmotic injury.
Radiographic Evaluation
Initial imaging should include:
- Weight-bearing AP ankle radiograph
- Mortise view
- Lateral ankle radiograph
Normal Mortise View Findings
A normal ankle mortise demonstrates:
- No widening of the medial clear space
- Tibiofibular clear space ≤6 mm
Radiographic Signs of Syndesmotic Injury
Possible findings include:
- Widened medial clear space
- Increased tibiofibular clear space
- Fibular displacement
- Small avulsion fragments
- Syndesmotic calcification in chronic cases
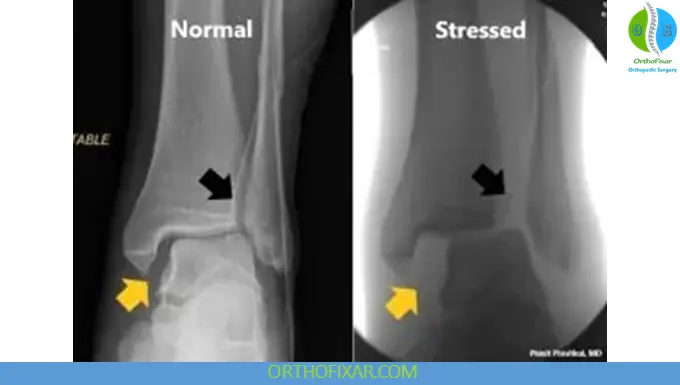
Stress radiographs may reveal:
- Dynamic widening of the mortise
- Posterior fibular displacement
MRI Evaluation
When plain radiographs are inconclusive but suspicion remains high, MRI is the preferred imaging modality.
MRI may identify:
- Partial ligament tears
- Complete syndesmotic disruption
- Associated bone edema
- Deltoid ligament injury
- Occult fractures
MRI is particularly valuable in:
- Latent instability
- Chronic ankle pain
- Athletes with persistent symptoms
Differential Diagnosis
Conditions that may mimic syndesmotic injury include:
- Lateral ankle sprain
- Deltoid ligament injury
- Osteochondral lesion of the talus
- Peroneal tendon injury
- Maisonneuve fracture
- Posterior ankle impingement
- Stress fracture
Treatment of Ankle Syndesmosis Injury
Treatment depends on:
- Stability of the syndesmosis
- Presence of diastasis
- Associated fractures
- Functional demands of the patient
Nonoperative Management
Stable syndesmotic sprains without diastasis are usually treated conservatively.
Initial Treatment
Conservative management includes:
- Immobilization in a non–weight-bearing cast or boot
- Ice and elevation
- Anti-inflammatory medications
- Protected weight bearing
Patients are commonly maintained non–weight bearing for 2–3 weeks.
Rehabilitation
After immobilization:
- Progressive range-of-motion exercises begin
- Strengthening exercises are introduced
- Proprioceptive rehabilitation is emphasized
A protective articulated ankle-foot orthosis may help prevent external rotation stress during recovery.
Recovery is often slower than routine lateral ankle sprains.
Operative Management
Surgical treatment is indicated for:
- Syndesmotic diastasis
- Unstable injuries
- Irreducible syndesmotic disruption
- Associated fractures with instability
Surgical Fixation
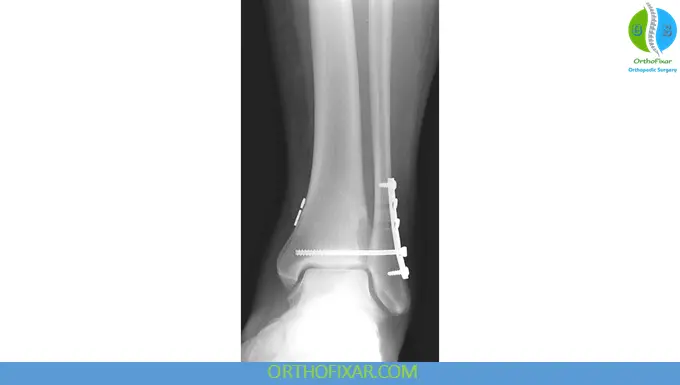
Operative stabilization commonly uses:
- One or two trans-syndesmotic screws
- Suture-button fixation systems
Traditional fixation typically involves screws placed from the fibula into the tibia proximal to the syndesmosis.
Postoperative Care
Typical postoperative protocol includes:
- Non–weight bearing for approximately 6 weeks
- Gradual rehabilitation thereafter
- Screw removal at 12–16 weeks in selected cases
Return to sports may require several months depending on injury severity.
Complications
Potential complications include:
- Chronic syndesmotic instability
- Persistent ankle pain
- Heterotopic ossification
- Post-traumatic ankle arthritis
- Malreduction of the syndesmosis
- Loss of athletic performance
Delayed diagnosis significantly increases the risk of chronic morbidity.
Prognosis
Stable injuries treated early generally have favorable outcomes. However, syndesmotic injuries often require substantially longer recovery than lateral ankle sprains.
Athletes may require:
- Extended rehabilitation
- Functional bracing
- Sport-specific conditioning before return to play
Persistent instability may lead to chronic pain and degenerative ankle disease.
Key Clinical Pearls
- Syndesmotic sprains are frequently underdiagnosed.
- Pain above the ankle joint should raise suspicion for syndesmotic injury.
- Positive squeeze and external rotation stress tests are valuable clinical tools.
- MRI is highly useful when radiographs are normal but suspicion remains high.
- Recovery is usually slower than standard lateral ankle sprains.
- Untreated instability may lead to chronic ankle dysfunction and arthritis.
Conclusion
Ankle Syndesmosis Injury is an important cause of prolonged ankle disability and chronic pain, particularly in athletes. Accurate diagnosis requires careful clinical examination combined with appropriate imaging. Early recognition and appropriate management are essential to restore ankle stability, prevent chronic instability, and optimize long-term outcomes.
References & More
- Bergman R, Li D, Shuman VL. Acute Ankle Sprain. [Updated 2025 Aug 2]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: Pubmed
- Liu J, Valentine D, Ebraheim NA. Management of Syndesmosis Injury: A Narrative Review. Orthop Res Rev. 2022 Dec 10;14:471-475. doi: 10.2147/ORR.S340533. PMID: 36530364; PMCID: PMC9749496. Pubmed
- Norkus SA, Floyd RT. The anatomy and mechanisms of syndesmotic ankle sprains. J Athl Train. 2001 Jan-Mar;36(1):68-73. PMID: 16404437; PMCID: PMC155405. Pubmed
- Egol KA. Handbook of fractures. 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2019.