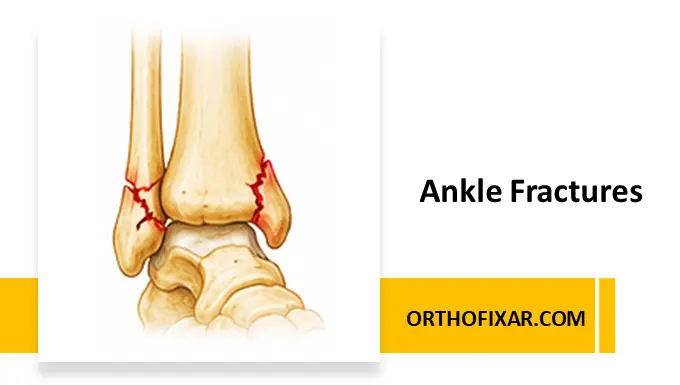
Ankle fractures are among the most common lower-extremity injuries encountered in orthopedic and emergency practice. They range from stable isolated malleolar injuries to highly unstable fracture-dislocations involving syndesmotic disruption and articular incongruity.
The highest incidence of ankle fractures occurs in elderly women, although they are not traditionally categorized as classic fragility fractures. The incidence is approximately 187 fractures per 100,000 individuals annually. Most injuries are isolated malleolar fractures, while bimalleolar fractures account for approximately one-fourth of cases and trimalleolar fractures account for 5%–10%.
Open ankle fractures are relatively uncommon, representing about 2% of all ankle fractures. Increased body mass index (BMI) has also been identified as an independent risk factor.
Epidemiology of Ankle Fractures
Key epidemiologic facts include:
- Incidence: ~187 per 100,000 people annually
- Elderly women are the most commonly affected population
- Isolated malleolar fractures comprise approximately two-thirds of injuries
- Bimalleolar fractures occur in ~25%
- Trimalleolar fractures account for 5%–10%
- Open fractures occur in only ~2%
- Higher BMI increases fracture risk
Common mechanisms include:
- Twisting injuries
- Low-energy falls
- Sports injuries
- Motor vehicle trauma
- Axial loading injuries
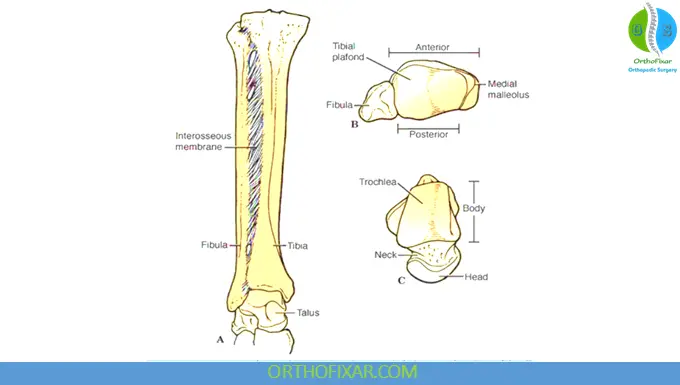
Anatomy of the Ankle Joint
The ankle is a complex hinge joint formed by the:
- Distal tibia
- Distal fibula
- Talus
The distal tibia and fibula create the ankle mortise, which articulates with the talar dome.
Tibial Plafond
The distal tibial articular surface is called the plafond. It:
- Is concave in the AP plane
- Is convex laterally
- Is wider anteriorly
- Provides congruency with the wedge-shaped talus
Talar Dome
The talar dome:
- Is trapezoidal
- Is approximately 2.5 mm wider anteriorly
- Is covered almost entirely by articular cartilage
Medial Malleolus
The medial malleolus consists of:
- Anterior colliculus
- Posterior colliculus
These serve as attachment points for the superficial and deep deltoid ligaments.
Lateral Malleolus
The lateral malleolus is the distal fibula and provides:
- Lateral ankle stability
- Syndesmotic support
- Articular congruency
See Also: Ankle Anatomy
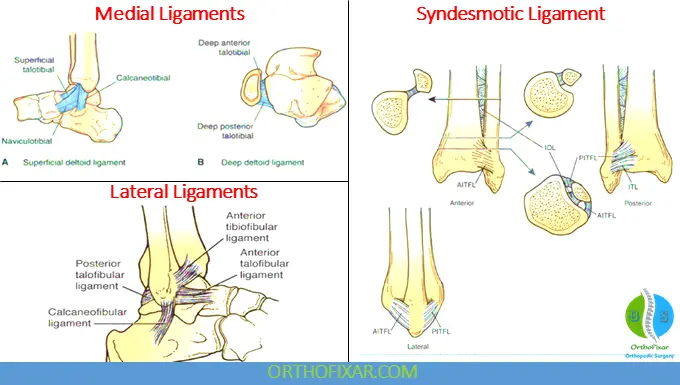
Syndesmotic Ligament Complex
The distal tibiofibular syndesmosis maintains ankle mortise stability.
It consists of:
- Anterior inferior tibiofibular ligament (AITFL)
- Posterior inferior tibiofibular ligament (PITFL)
- Transverse tibiofibular ligament
- Interosseous ligament
The PITFL is stronger than the AITFL and may avulse a posterior malleolar fragment rather than rupture.
Deltoid Ligament Complex
The deltoid ligament stabilizes the medial ankle.
Superficial Deltoid Ligament
Includes:
- Tibionavicular ligament
- Tibiocalcaneal ligament
- Superficial tibiotalar ligament
Functions:
- Resists valgus stress
- Supports the talar head
Deep Deltoid Ligament
The deep tibiotalar ligament is the primary medial stabilizer preventing lateral talar displacement.
Lateral Collateral Ligament Complex
The lateral ligament complex includes:
- Anterior talofibular ligament (ATFL)
- Calcaneofibular ligament (CFL)
- Posterior talofibular ligament (PTFL)
The ATFL is the weakest ligament and is commonly injured during inversion injuries.
Biomechanics of the Ankle
Normal ankle range of motion:
- Dorsiflexion: 30°
- Plantarflexion: 45°
Normal gait requires:
- At least 10° dorsiflexion
- At least 20° plantarflexion
A lateral talar shift dramatically reduces articular contact pressure distribution:
- 1 mm shift → 40% decrease in contact area
- 3 mm shift → >60% decrease
This explains why anatomic reduction is critical.
Mechanism of Injury
Fracture patterns depend on:
- Foot position at injury
- Direction of force
- Rotational versus axial loading
- Bone quality
- Ligamentous integrity
Common mechanisms include:
- Supination-external rotation
- Supination-adduction
- Pronation-external rotation
- Pronation-abduction
See Also: Lateral Ankle Sprain
Clinical Evaluation
Patients may present with:
- Pain
- Swelling
- Ecchymosis
- Deformity
- Inability to bear weight
Physical Examination
Important examination components include:
- Neurovascular assessment
- Skin evaluation
- Open wound assessment
- Palpation of the entire fibula
- Syndesmotic testing
Squeeze Test
Compression of the tibia and fibula proximally may reproduce distal syndesmotic pain.
Ankle Dislocation
A grossly dislocated ankle requires immediate reduction before radiographs if neurovascular compromise or skin tension is present.
Radiographic Evaluation
Standard ankle trauma series includes:
- AP view
- Lateral view
- Mortise view
AP View Findings
Abnormal findings include:
- Tibiofibular overlap <10 mm
- Tibiofibular clear space >5 mm
- Talar tilt >2 mm asymmetry
Mortise View
The mortise view is obtained with 15–20° internal rotation.
Important measurements:
- Medial clear space >4–5 mm suggests deltoid injury
- Talar shift >1 mm is abnormal
- Reduced tibiofibular overlap suggests syndesmotic injury
CT Scan
CT is useful for:
- Posterior malleolar fractures
- Pilon variants
- Articular assessment
- Surgical planning
MRI
MRI may identify:
- Occult fractures
- Cartilage injuries
- Tendon pathology
- Ligamentous injuries
See Also: Ankle X-Ray Imaging
Classification of Ankle Fractures
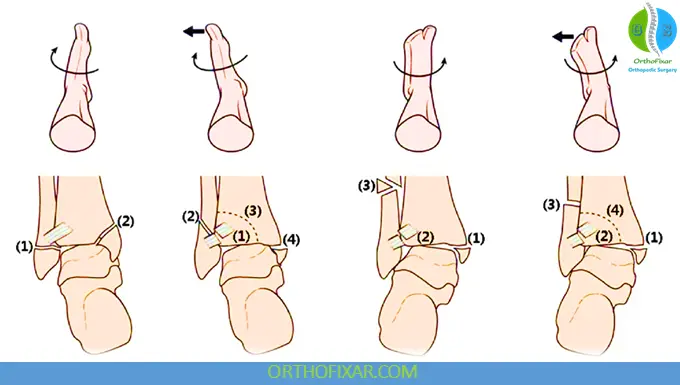
Lauge-Hansen Classification
This classification is based on:
- Foot position
- Direction of deforming force
Supination-External Rotation (SER)
Most common pattern (40%–75%).
Stages include:
- AITFL injury
- Spiral distal fibular fracture
- Posterior malleolar injury
- Medial malleolus fracture or deltoid rupture
Supination-Adduction (SA)
Associated with:
- Vertical medial malleolus fracture
- Distal transverse fibular fracture
Pronation-Abduction (PA)
Produces:
- Medial injury
- Syndesmotic disruption
- Transverse fibular fracture
Pronation-External Rotation (PER)
Typically causes:
- Medial injury
- Syndesmotic injury
- High fibular fracture
- Posterior malleolar injury
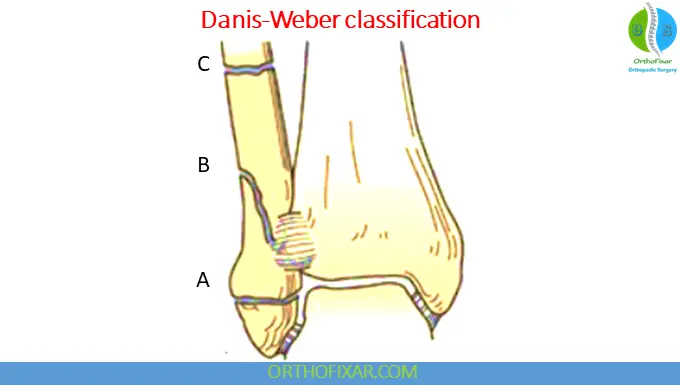
Danis-Weber Classification
The Weber classification is based on fibular fracture level.
Weber A
- Infrasyndesmotic
- Usually stable
Weber B
- At syndesmotic level
- Variable stability
Weber C
- Suprasyndesmotic
- Syndesmotic injury usually present
- Often unstable
Maisonneuve Fracture
A Maisonneuve fracture involves:
- Proximal fibular fracture
- Syndesmotic disruption
- Medial ankle injury
Failure to palpate the proximal fibula may result in missed diagnosis.
Ankle Fractures Treatment
Initial Priorities
- Assess neurovascular status
- Reduce dislocations immediately
- Splint the ankle
- Elevate the limb
- Control swelling
Reduction Principles
Goals include:
- Restoring mortise alignment
- Preventing skin compromise
- Minimizing cartilage injury
- Preserving perfusion
After reduction:
- Obtain repeat radiographs
- Apply posterior splint with stirrup component
Nonoperative Treatment
Indications
Nonoperative management is appropriate for:
- Stable fractures
- Nondisplaced fractures
- Intact syndesmosis
- Medically unfit surgical candidates
Immobilization Options
Treatment may include:
- Short leg cast
- Removable walking boot
- Stirrup brace
Weight bearing depends on fracture stability and healing.
Operative Treatment
Indications for ORIF
Open reduction and internal fixation (ORIF) is indicated for:
- Unstable fractures
- Mortise incongruity
- Syndesmotic instability
- Failure of closed reduction
- Open fractures
- Fracture-dislocations
Lateral Malleolus Fixation
Methods include:
- Lag screws
- Neutralization plates
- Antiglide plates
- Intramedullary fixation
Restoration of fibular length and rotation is essential.
Medial Malleolus Fixation
Fixation methods include:
- Cannulated screws
- Tension band wiring
- Plate fixation
Indications include persistent medial instability or displacement.
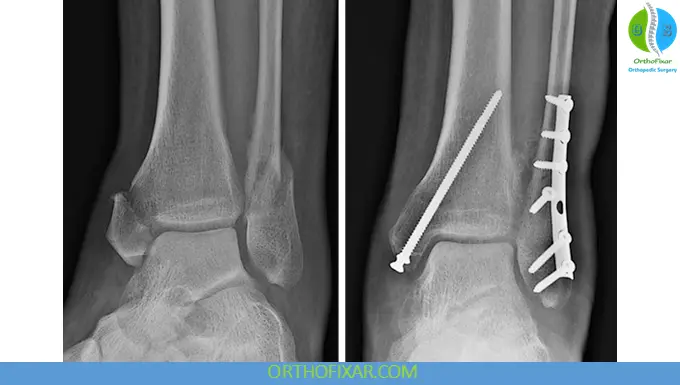
Posterior Malleolus Fixation
Indications for fixation include:
- 25% articular involvement
- 2 mm displacement
- Posterior talar subluxation
Fixation may improve syndesmotic stability because the PITFL remains attached.
Syndesmotic Fixation
Syndesmotic instability may require:
- Trans-syndesmotic screws
- Suture-button fixation
Fixation is usually placed 1.5–2 cm above the plafond.
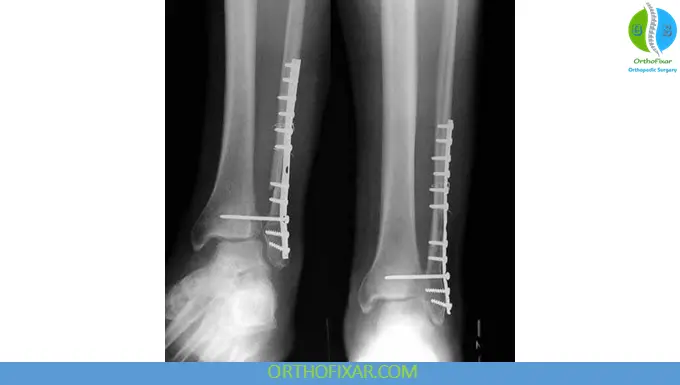
Open Ankle Fractures
Open fractures require:
- Urgent irrigation and debridement
- IV antibiotics
- Fracture stabilization
- Serial wound evaluation
External fixation may be necessary for severe soft tissue injury.
Complications of Ankle Fractures
Malunion
Common deformities include:
- Fibular shortening
- External rotation malalignment
- Persistent talar shift
Nonunion
Rare, most commonly involving the medial malleolus.
Post-Traumatic Arthritis
Risk factors include:
- Articular incongruity
- Residual talar shift
- Cartilage injury
Infection
Occurs in >2% of closed fractures and more frequently in open injuries.
Complex Regional Pain Syndrome (CRPS)
Rare but debilitating complication characterized by:
- Pain
- Edema
- Autonomic dysfunction
- Stiffness
Compartment Syndrome
Rare but limb-threatening.
Rehabilitation After Ankle Fracture
Rehabilitation focuses on:
- Range-of-motion restoration
- Edema control
- Progressive weight bearing
- Strengthening
- Proprioceptive training
Recovery duration varies depending on:
- Fracture severity
- Fixation stability
- Syndesmotic injury
- Patient compliance
Prognosis
Outcomes are best when:
- Mortise congruity is restored
- Fibular length is anatomically corrected
- Syndesmotic reduction is accurate
- Early mobilization is achieved
Persistent talar shift strongly predicts poor functional outcomes and arthritis.
Key Clinical Pearls
- Even 1 mm of talar shift significantly alters ankle biomechanics
- Always examine the entire fibula to exclude Maisonneuve injury
- Syndesmotic injuries are frequently underdiagnosed
- Medial clear space widening suggests deltoid disruption
- Anatomical reduction is the strongest predictor of good outcome
Conclusion
Ankle fractures represent a diverse group of injuries requiring careful assessment of osseous and ligamentous stability. Successful management depends on restoring ankle mortise congruity, fibular length, syndesmotic integrity, and articular alignment. Accurate classification systems, proper imaging interpretation, and timely intervention are essential for optimizing long-term function and minimizing complications such as post-traumatic arthritis.
FAQ
What is the most common type of ankle fracture?
The most common ankle fracture pattern is the supination-external rotation injury, corresponding to Weber B fractures.
When is surgery required for ankle fractures?
Surgery is indicated for unstable fractures, displaced fractures, syndesmotic injuries, open fractures, and fracture-dislocations.
What is the medial clear space in ankle fractures?
The medial clear space is the distance between the medial talus and medial malleolus. A value greater than 4–5 mm suggests deltoid ligament injury or ankle instability.
What is a Maisonneuve fracture?
A Maisonneuve fracture is a proximal fibular fracture associated with syndesmotic disruption and medial ankle injury.
What complication is most associated with poor ankle fracture reduction?
Post-traumatic ankle arthritis is strongly associated with residual talar shift and articular incongruity.
References & More
- Hermena S, Slane VH. Ankle Fracture. [Updated 2025 Feb 15]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: Pubmed
- Kyriacou H, Mostafa AMHAM, Davies BM, Khan WS. Principles and guidelines in the management of ankle fractures in adults. J Perioper Pract. 2021 Nov;31(11):427-434. doi: 10.1177/1750458920969029. Epub 2021 Apr 7. PMID: 33826430; PMCID: PMC8575982. Pubmed
- Koujan K, Saber AY. Bimalleolar Ankle Fractures. [Updated 2023 Feb 11]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: Pubmed
- Egol KA. Handbook of fractures. 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2019.