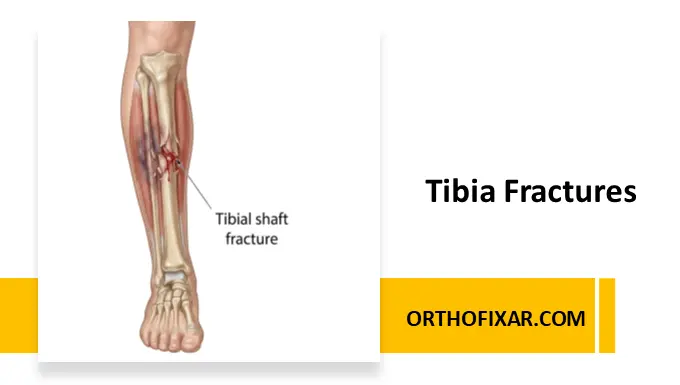
A tibia fracture is the most common long bone fracture, with an incidence of approximately 26 diaphyseal fractures per 100,000 population annually. Due to the subcutaneous location of the tibia (one-third of its surface), there is a high risk of open fractures, making soft-tissue management critical.
Anatomy of the Tibia
The tibia is a long tubular bone with a triangular cross-section responsible for approximately 85% of weight-bearing load, while the fibula transmits the remaining force.
Blood Supply
- Endosteal supply: Nutrient artery (branch of posterior tibial artery)
- Periosteal supply: Primarily from anterior tibial artery
- Distal third: Supplied via periosteal anastomoses around the ankle
⚠️ A watershed zone exists at the junction of the middle and distal thirds, making this region prone to delayed union or nonunion.
Preservation of periosteal attachments during fixation is essential to maintain vascularity.
See Also: Lateral Compartment of Leg
Mechanism of Injury
Mechanism of Injury
Tibia fractures result from direct or indirect trauma:
Direct Trauma (High-Energy)
- Transverse or comminuted fractures
- Significant displacement
- Extensive soft-tissue injury
Indirect Trauma (Low-Energy)
- Spiral fractures (torsion mechanism)
- Minimal displacement
- Less soft-tissue damage
Other Mechanisms
- Bending forces: Short oblique fractures
- Crush injuries: Segmental/comminuted fractures with severe soft-tissue damage
- Associated fibular fractures: Indicate higher energy trauma
See Also: Tibial Plateau Fracture
Symptoms of Tibia Fracture
- Severe leg pain and deformity
- Inability to bear weight
- Swelling and tenderness
- Possible open wound
Important Clinical Considerations
- Always assess neurovascular status
- Soft-tissue injury severity determines treatment strategy
Compartment Syndrome (Critical Complication)
A limb-threatening emergency.
Key signs:
- Pain out of proportion
- Pain on passive stretch
- Tense compartment
- Paresthesia
⚠️ Late signs: Pallor, pulselessness, paralysis
Indication for fasciotomy:
- Compartment pressure >30 mmHg
- Or within 30 mmHg of diastolic pressure
See Also: Anterior Compartment of Leg
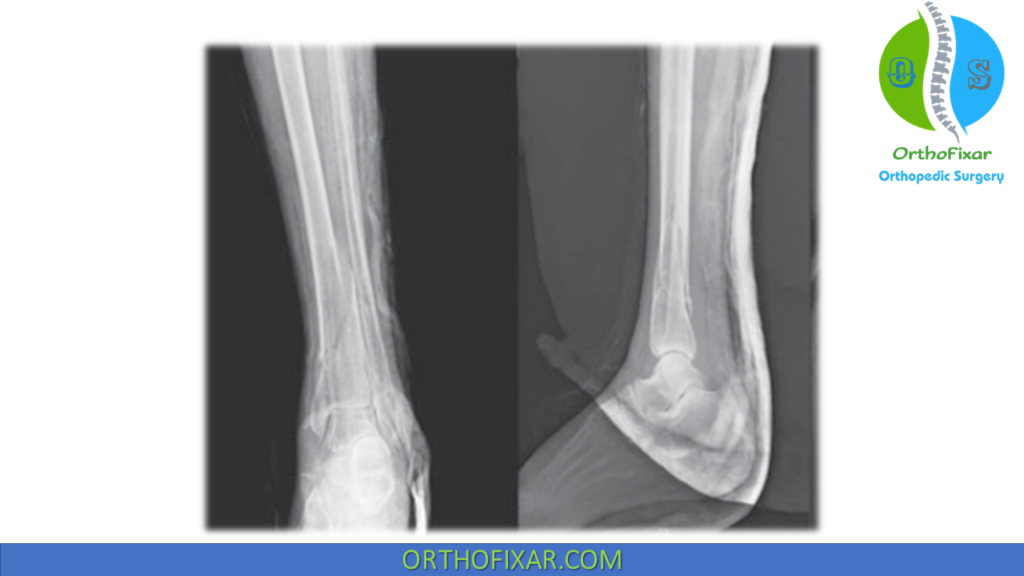
Radiology
- X-rays (AP & lateral views) including knee and ankle
- Assess for:
- Secondary fracture lines
- Bone defects
- Soft-tissue gas
⚠️ Soft-tissue gas may indicate:
- Open fracture
- Gas gangrene
- Necrotizing fasciitis
- CT / MR angiography: If vascular injury suspected
Tibia Fractures Classification
Descriptive Classification
- Location: Proximal, middle, distal third
- Pattern: Spiral, oblique, transverse
- Displacement: Angulation, rotation, shortening
- Comminution: Butterfly, segmental
- Soft tissue: Open vs closed
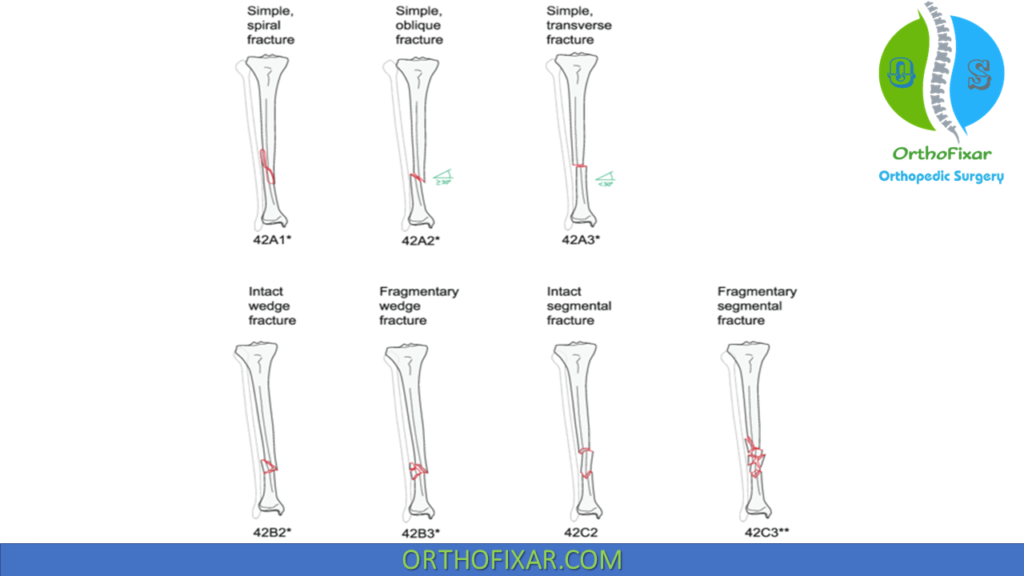
AO Classification
- Type A: Simple fractures
- Type B: Wedge fractures
- Type C: Complex/comminuted fractures
Tibia Fractures Treatment
The fractured tibia treatment options depend on the:
- Morphology of the fracture,
- Status of the soft-tissue envelope,
- The neurovascular status,
- Associated skeletal and other major organ injuries
- The general medical status of the patient.
Most of the tibial fractures may be treated operatively or non-operatively. Tibia fractures surgical treatment is generally the preferred method of treatment as it allows early mobilization and avoids complications of prolonged immobilization.
Non-Operative Treatment
Indicated for:
- Closed, low-energy fractures
- Minimal displacement
Management
- Long leg cast
- Early partial weight-bearing
- Transition to functional brace after 4–6 weeks
Acceptable Alignment
- <5° varus/valgus
- <10° AP angulation
- <10° rotation
- <15 mm shortening
- 50% cortical contact
Healing Time
- Average tibia fracture healing time: ~16 weeks
Operative Treatment
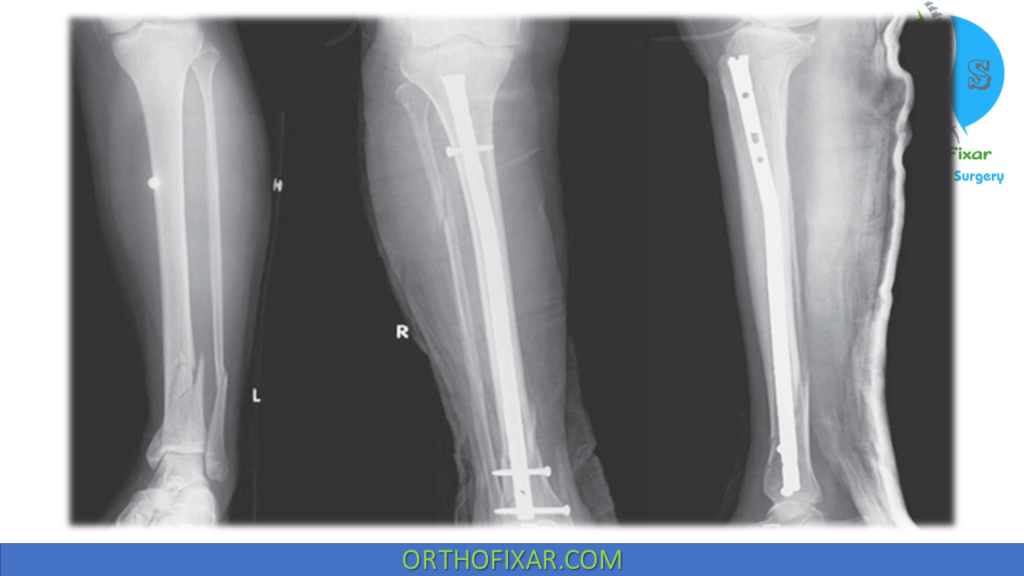
1. Intramedullary (IM) Nailing (Gold Standard)
- Preserves periosteal blood supply
- Allows early mobilization
- Controls alignment and rotation
✔ Reamed nails preferred:
- Stronger fixation
- Better outcomes
✔ Unreamed nails:
- Used in severe open fractures
- Lower mechanical strength
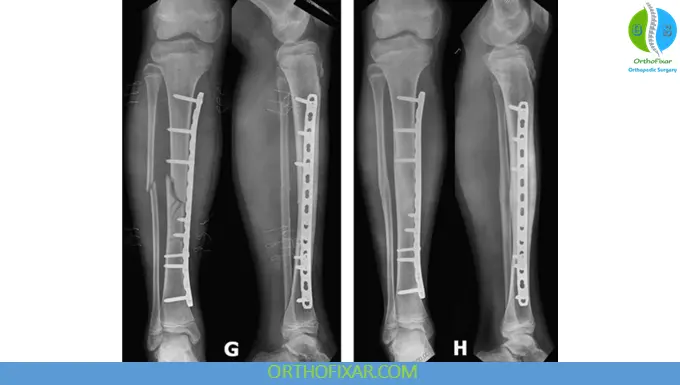
2. Plating
Used in:
- Metaphyseal or intra-articular extension
Limitations:
- Soft-tissue damage
- Infection risk
Modern options:
- Locking plates
- Biological (minimally invasive) plating
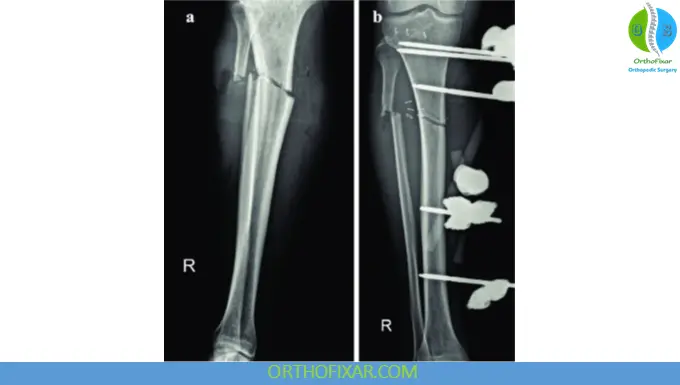
3. External Fixation
Indications:
- Severe open fractures
- Polytrauma
- Compartment syndrome
⚠️ Usually temporary → convert to IM nailing within 2–3 weeks
Complications of Tibia Fracture
- Compartment syndrome
- Infection (especially open fractures)
- Delayed union / nonunion
- Malunion
- Knee ligament injuries
Key Takeaways
- Tibia fractures are the most common long bone fractures
- High risk of open injury and soft-tissue complications
- Intramedullary nailing is the preferred treatment in most cases
- Early recognition of compartment syndrome is critical
- Healing typically occurs within ~16 weeks, depending on severity

References & More
- Mercer’s Textbook of Orthopaedics and Trauma, Tenth edition.
- McQueen MM, Gaston P, Court-Brown CM. Acute compartment syndrome: who is at risk? Journal of Bone and Joint Surgery (British) 2000;82:200–3. Pubmed
- Bhandari M, Tornetta P III, Sprague S, et al. Predictors of reoperation following operative management of fractures of the tibial shaft. Journal of Orthopedic Trauma 2003;17:353–61. Pubmed
- Keating JF, O’Brien PI, Blachut PA, et al. Reamed interlocking intramedullary nailing of open fractures of the tibia. Clinical Orthopaedics and Related Research 1997;338:182–91. Pubmed
- Collinge CA, Sanders RW. Percutaneous plating in the lower extremity. Journal of the American Academy of Orthopaedic Surgeons 2000;8:211–16. Pubmed
- Ricci WM, O’Boyle M, Borrelli J, et al. Fractures of the proximal third of the tibial shaft treated with intramedullary nails and blocking screws. Journal of Orthopedic Trauma 2001;15:264–70. Pubmed
- Henley MB, Chapman JR, Agel J, et al. Treatment of type II, IIIA, and IIIB open fractures of the tibial shaft: A prospective comparison of unreamed interlocking intramedullary nails and half-pin external fixators. Journal of Orthopedic Trauma 1998;12:1–7. Pubmed
- Bhandari M, Guyatt GH, Tong D, et al. Reamed versus nonreamed intramedullary nailing of lower extremity long bone fractures: a systematic overview and meta-analysis. Journal of Orthopedic Trauma 2000;14:2–9. Pubmed