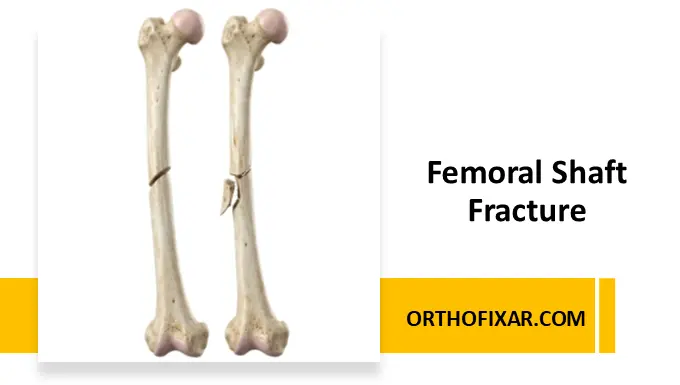
A femoral shaft fracture is a serious orthopedic injury involving the diaphysis of the femur—the longest and strongest bone in the human body. These fractures are typically associated with high-energy trauma and frequently occur alongside multisystem injuries, making them a critical concern in trauma care.
Epidemiological studies indexed in PubMed report an incidence of approximately 10 per 100,000 population annually, with a bimodal distribution:
- Young males (15–24 years): high-energy trauma (e.g., motor vehicle accidents)
- Elderly females (>75 years): low-energy falls due to osteoporosis
Anatomy of the Femoral Shaft
The femoral shaft is a large tubular structure with unique biomechanical and vascular characteristics:
Key Anatomical Features
- Anterior bowing: Important for load distribution
- Medial cortex: Under compression
- Lateral cortex: Under tension
- Isthmus: Narrowest intramedullary canal—critical for implant selection
Muscle Forces Acting on Fractures
Several muscle groups create deforming forces:
- Abductors (gluteus medius/minimus): abduct proximal fragment
- Iliopsoas: flexes and externally rotates proximal fragment
- Adductors: cause varus deformity and shortening
- Gastrocnemius: flexes distal fragment
- Fascia lata: resists medial displacement
Compartments of the Thigh
The thigh is divided into three compartments:
- Anterior: quadriceps, femoral nerve/artery/vein
- Medial: adductors, obturator nerve
- Posterior: hamstrings, sciatic nerve
Unlike the leg, compartment syndrome is rare due to the large volume capacity.
See Also: Muscles of the Lower Limb
Blood Supply and Healing
- Primary supply: Profunda femoris artery
- Endosteal circulation: supplies inner 2/3 of cortex
- Periosteal circulation: supplies outer 1/3
After Femoral Shaft Fracture:
- Endosteal supply is disrupted
- Periosteal vessels dominate early healing
- Revascularization occurs within 3–4 weeks
Mechanism of Injury
Femoral shaft fractures usually result from:
High-Energy Trauma
- Motor vehicle accidents
- Falls from height
- Gunshot wounds
Other Causes
- Pathologic fractures: malignancy or osteoporosis
- Stress fractures: common in athletes and military recruits
- Atypical fractures: associated with prolonged bisphosphonate use
See Also: Femoral Stress Fracture
Clinical Evaluation
Presentation
- Severe thigh pain
- Inability to bear weight
- Deformity, swelling, limb shortening
Important Considerations
- Up to 1 liter of blood loss into the thigh
- Perform full trauma assessment (ATLS protocol)
- Evaluate hip and knee for associated injuries
Associated Injuries
- Occur in 5–15% of cases
- Knee ligament injuries: up to 50%
- Possible spine, pelvis, and acetabular injuries
Radiographic Evaluation
Standard Imaging
- AP and lateral femur X-rays
- Hip and knee views
- Pelvic X-ray
Additional Imaging
- CT scan (if polytrauma suspected)
Radiographic Assessment
- Fracture pattern (spiral, transverse, oblique)
- Comminution and shortening
- Bone quality
- Air in soft tissues (open fracture indicator)
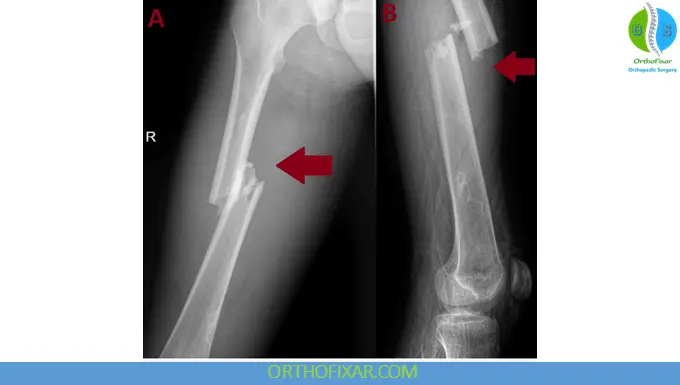
Femoral Shaft Fracture Classification
Descriptive Classification
- Open vs closed
- Location: proximal, middle, distal third
- Pattern: spiral, oblique, transverse
- Degree of comminution
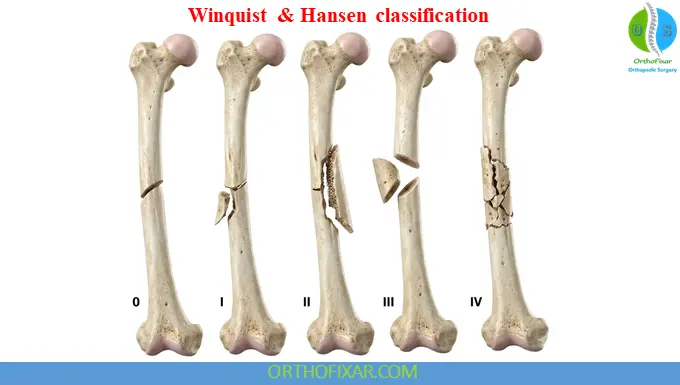
Winquist and Hansen Classification
Based on comminution:
- Type 0: no comminution or a small butterfly fragment <25% of the width of the bone
- Type I: small butterfly fragment <25% of the width of the bone
- Type II: butterfly fragment ≤50% of the width of the bone
- Type III: comminuted with a large butterfly fragment >50% of the width of the bone
- Type IV: severe comminution of an entire segment of bone (segmental comminution)
OTA Classification
Widely used modern system for fracture standardization
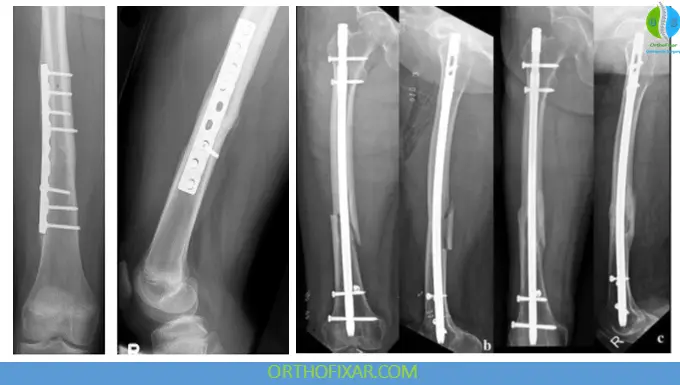
Treatment of Femoral Shaft Fractures
Nonoperative Management
Rarely used except when surgery is contraindicated.
Skeletal Traction
- Temporary stabilization
- Load: 11–15% of body weight (20–40 lbs)
- Goals:
- Maintain length
- Reduce pain
- Prevent deformity
Limitations
- Prolonged immobilization
- Risk of malunion and complications
Operative Management (Standard of Care)
Intramedullary Nailing (IMN)
Gold standard treatment.
Advantages
- 95% union rate
- Minimal soft tissue disruption
- Early mobilization
- Lower infection rates
Types of IM Nailing
1. Antegrade Nailing
- Entry: piriformis fossa or greater trochanter
- Best for midshaft fractures
2. Retrograde Nailing
- Entry via distal femur
- Indications:
- Bilateral fractures
- Obesity
- Pregnancy
- Associated injuries
External Fixation
Used mainly for damage control orthopedics:
- Fast (<30 minutes)
- Temporary stabilization
- Indicated in:
- Polytrauma
- Vascular injury
- Severe soft tissue damage
Plate Fixation
Less common due to IM nailing superiority.
Indications
- Narrow medullary canal
- Complex fracture patterns
- Associated vascular injury
Disadvantages
- Higher infection risk
- More soft tissue damage
- Implant failure risk
Special Clinical Scenarios
Polytrauma Patients
- Early fixation reduces complications
- Damage control approach may be required
Combined Injuries
- Femoral neck fractures (3–5%)
- Distal femur fractures
Rehabilitation
- Early mobilization
- Immediate knee range-of-motion exercises
- Gradual weight-bearing based on:
- Fixation type
- Healing progression
Complications
Early Complications
- Hemorrhage
- Fat embolism syndrome
- Neurovascular injury (rare)
Late Complications
- Nonunion/delayed union (>6 months)
- Malunion (varus, shortening, rotation)
- Infection (<1% in closed fractures)
- Implant failure
- Heterotopic ossification
Prognosis
With modern surgical techniques—particularly intramedullary nailing—the prognosis of Femoral Shaft Fracture is excellent:
- High union rates (>95%)
- Early return to function
- Low complication rates with proper technique
References & More
- Denisiuk M, Afsari A. Femoral Shaft Fractures. [Updated 2023 Jan 2]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: Pubmed
- Denisiuk M, Afsari A. Femoral Shaft Fractures. 2023 Jan 2. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan–. PMID: 32310517. Pubmed
- Egol KA. Handbook of fractures. 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2019.