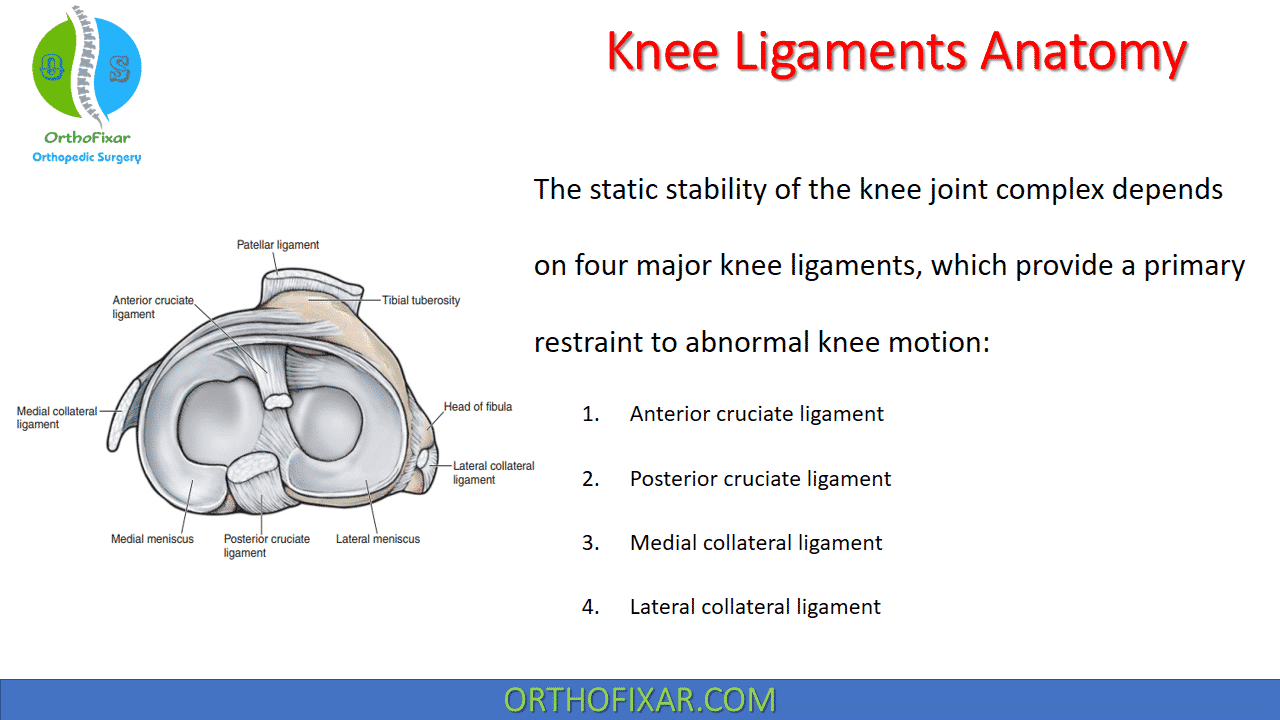
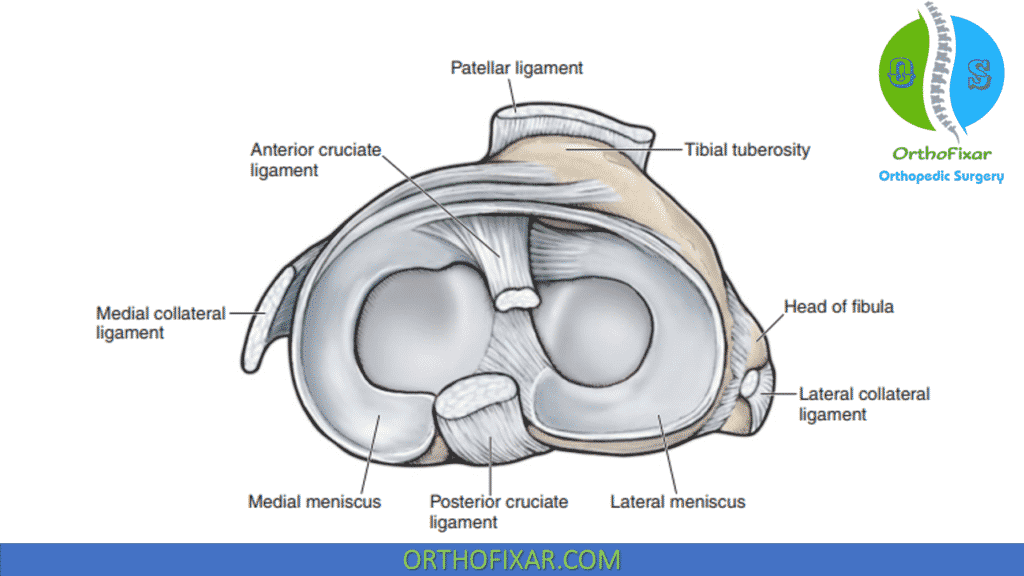
The static stability of the knee joint complex depends on four major knee ligaments, which provide a primary restraint to abnormal knee motion:
- Anterior cruciate ligament: Provides the primary restraint for anterior translation and medial rotation of the tibia on the femur and is a secondary restraint to valgus and varus rotation of the tibia.
- Posterior cruciate ligament: Provides the primary restraint for posterior translation and medial rotation of the tibia on the femur and is a secondary restraint to valgus and varus rotation of the tibia.
- Medial collateral ligament: Provides the primary restraint for valgus and lateral rotation of the tibia, and is a secondary restraint to anterior and posterior translation of the tibia on the femur.
- Lateral collateral ligament: Provides the primary restraint for varus and lateral rotation of the tibia, and is a secondary restraint to anterior and posterior translation of the tibia on the femur.
Knee Ligaments Anatomy
Knee Cruciate Ligaments
The two central intra-articular cruciate ligaments derive their name from the Latin word crucere (cross) because they cross each other. Both the ACL and PCL lie in the center of the joint, and each are named according to their attachment sites on the tibia.
The cruciate ligaments, which differ from those of other joints in that they restrict normal, rather than abnormal, motion, are the main stabilizing ligaments of the knee and restrain against anterior (ACL) and posterior (PCL) translations of the tibia on the femur. They also restrain against excessive internal and external rotation and varus movement of the tibia.
The blood supply to the cruciate ligaments is largely provided from the middle and inferior geniculate branches of the popliteal artery. The cruciate ligaments are innervated by the posterior articular nerve, a branch of the posterior tibial nerve. The function of this nerve supply is questionable although it may serve as proprioceptive in nature. In addition, the cruciate ligaments contain mechanoreceptors, suggesting that disruption of the ligament structure can produce partial deafferentation of the joint.
Anterior Cruciate Ligament
The Anterior Cruciate Ligament is a unique structure and one of the most important ligaments to knee stability, serving as a primary restraint to anterior translation of the tibia relative to the femur, and a secondary restraint to both internal and external rotation in the non–weight-bearing knee.
The Anterior Cruciate Ligament (ACL) originates on the posteromedial aspect of the lateral femoral condyle within the intercondylar notch and inserts onto the anterior intercondylar area of the tibia. It has anteromedial (tight in flexion) and posterolateral (tight in extension) bundles; PL bundle tested with pivot shift test.
See Also:
The ACL is composed of a vast array of individual fascicles. These, in turn, are composed of numerous interlacing networks of collagen fibrils. The fascicles originate on the inner aspect of the lateral femoral condyle in the intercondylar notch and travel obliquely and distally through the knee joint. They enter the anterior intercondylar surface of the tibial plateau, where they partially blend with the lateral meniscus. As the fascicles of the ACL course through the knee joint and attach to their insertion sites, they fan out and give a slight spiral appearance to the ligament, a phenomenon that is more pronounced during knee flexion.
The synovial tissue that enfolds the ACL consists of an intimal layer, facing the joint cavity, and a subsynovial layer. The subsynovial layer is in direct contact with the ACL and contains neurovascular structures.
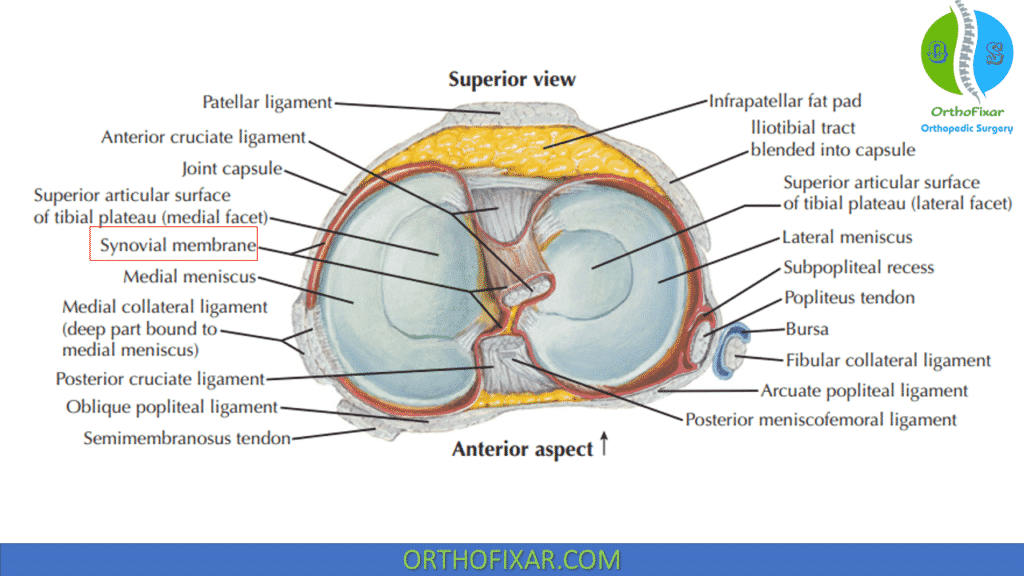
The ACL is considered intra-articular yet extrasynovial because of the posterior invagination of the synovial membrane.
Although the posterior articular nerve is the major nerve for the ACL, afferent fibers have also been demonstrated in the medial and lateral articular nerves. Like all ligaments, the ACL behaves as a viscoelastic structure, allowing it to dissipate energy and to adjust its length and internal load distribution as a function of load history. This means that the normal ACL is capable of microscopic adjustments to internal stresses over time, thus influencing the laxity, stresses, and kinematics of the joint in subtle but potentially important ways.
One anatomic factor that contributes to selective fiber recruitment during tensile loading is the specific location of the insertions of the ACL on the femur and the tibia. These differing insertion sites allow different fibers of the ACL to be recruited with every subtle three-dimensional change in the position of the joint.
The anteromedial bundle of the ACL is taut in flexion, whereas in extension, the posterolateral fibers are stretched.
The amount of strain placed on the ACL is influenced by the type of movement and the subsequent translation of the tibia:
- During passive ROM (PROM), the amount of strain placed on the ACL is minimized when the tibia remains in the neutral position.
- In the final 15 degrees of extension, internally rotating the tibia greatly increases the strain placed on the ACL; externally rotating the tibia decreases the strain relative to internal rotation, but it is still greater than the strain with the tibia in neutral.
- Both valgus and varus stresses increase the strain on the ACL during PROM.
- During active open-chain knee extension when the pull of the quadriceps translates the tibia anteriorly, the amount of strain placed on the ACL is greatest between 0 and 30 degrees of flexion.
- Adding resistance through the arc of knee extension significantly increases the amount of strain as the knee extends from 45 to 0 degrees of flexion.
- During closed kinetic chain exercises, the strain on the ACL does not significantly change throughout the ROM.
See Also: Anterior Cruciate Ligament Injury
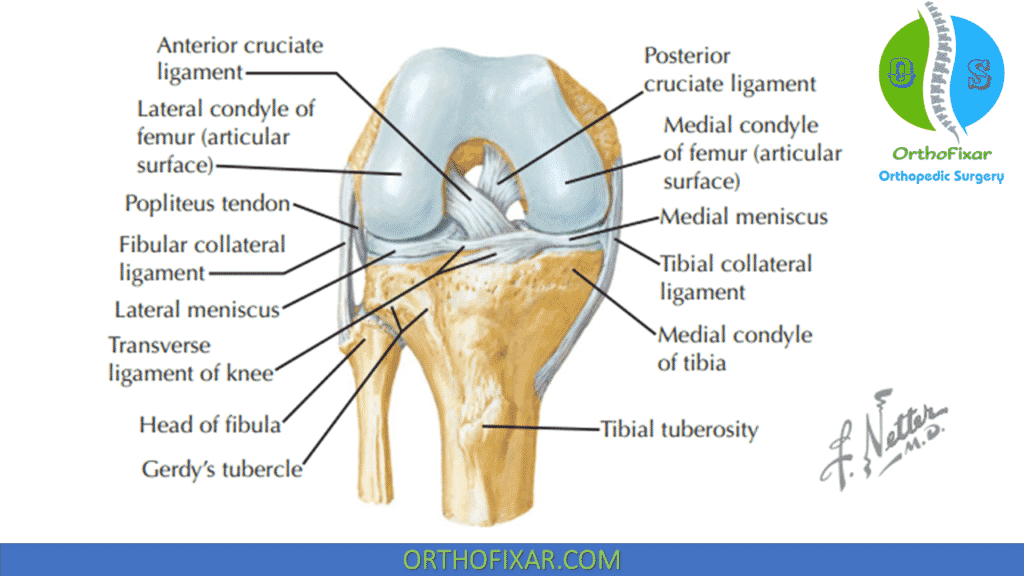
Posterior Cruciate Ligament
The PCL attaches posteriorly to the insertion of the posterior horns of the lateral and medial menisci on the posterior part of the posterior intercondylar fossa of the tibia. From here, the PCL extends obliquely medially, anteriorly, and superiorly to attach to the lateral surface of the medial femoral condyle. Overall, the ligament is wider at its femoral origin and narrowest near the tibial insertion.
The PCL is covered by synovial lining and is therefore considered to be extrasynovial yet intra-articular. Information regarding the biomechanical function of the PCL is scant compared with that of the ACL. It is known that the PCL is 50% thicker and has twice the tensile strength of the ACL.
The PCL is more vertical in extension and horizontal in flexion.
Like the ACL, the PCL consists of two bundles: anterior lateral and posterior medial. Overall, the ligament is most taut with further flexion of the knee. Specifically, the anterior lateral bundle is taut in flexion, while the posterior medial bundle is taut in extension.
The PCL provides 90–95% of the total restraint to posterior translation of the tibia on the femur, with the remainder being provided by the collateral ligaments, posterior portion of the medial and lateral capsules, and the popliteus tendon. The contribution percentage resisting posterior translation decreases as the knee extends.
The PCL is significantly loaded if a posteriorly directed force is applied to the tibia when the knee is flexed to 90 degrees or greater while in neutral rotation. If the same force is applied to the tibia when the knee is in terminal extension, the load on the PCL is not increased. This is contrary to the popular belief that hyperextension of the knee is the mechanism of injury of the PCL.
See Also:
The PCL also restrains internal rotation of the tibia on the femur and helps prevent posterior-medial instability at the knee.
Other functions of the PCL include acting as a secondary restraint to external rotation of the tibia on the femur at 90 degrees of flexion, assisting with a rolling/gliding mechanism of the tibiofemoral joint, and resisting varus/valgus forces at the knee after the collateral ligaments have failed.
A significant force is needed to tear the PCL. Thus, tears of the PCL are usually the result of severe contact injuries that often occur in traumatic situations, such as a dashboard injury during a motor vehicle accident. In concert with the PCL are the anterior and posterior meniscofemoral ligaments, which comprise approximately 22–50% of the cross-sectional area of the PCL. Although these ligaments arise from the common PCL origin they are distinct structures having different insertion sites. Both are named with respect to the orientation to the PCL.
Since the insertion site of the meniscofemoral ligaments are different from that of the PCL, if a midsubstance tear of the PCL occurs, it is possible that one or both of the meniscofemoral ligaments may remain intact.
See Also: Knee Meniscus Anatomy
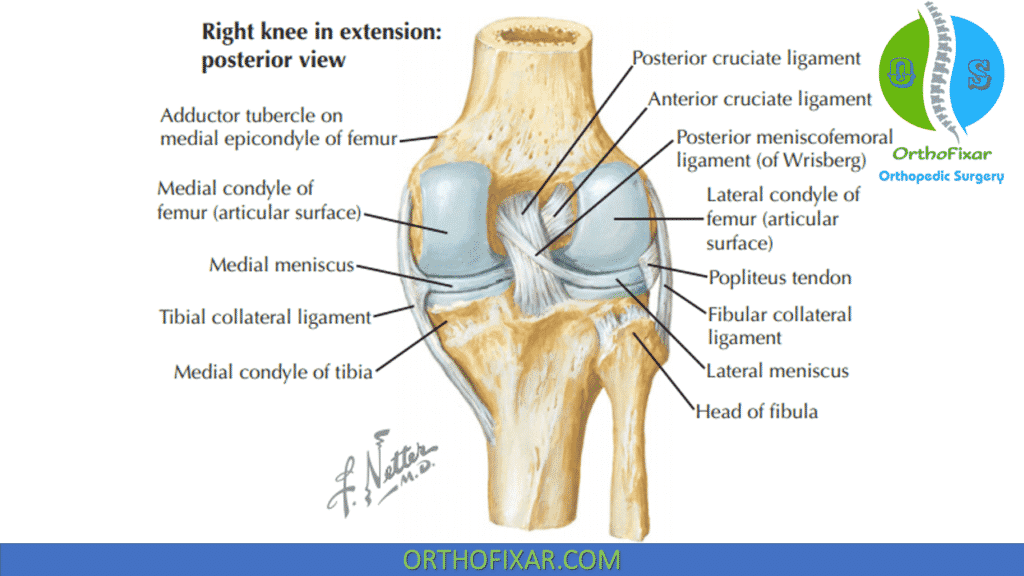
Collateral Ligaments
Both the MCL and the LCL are considered to be extra-articular ligaments.
Medial Collateral Ligament:
The MCL, or tibial collateral ligament, develops as a thickening of the medial joint capsule. It can be subdivided into a superficial band and a deep band:
- The superficial band is a thick, flat band, and has a fan-like attachment proximally on the medial femoral condyle, just distal to the adductor tubercle, from which it extends to the medial surface of the tibia approximately 6 cm below the joint line, covering the medial inferior genicular artery and nerve. The superficial band blends with the posteromedial corner of the capsule and, when combined, is referred to as the posterior oblique ligament. The superficial band is separated from the deep layer of the ligament by a bursa. Since the superficial band is farther from the center of the knee, it is the first ligament injured when a valgus stress is applied.
- The deep band (medial capsular ligament) is a continuation of the capsule. It blends with the medial meniscus and consists of an upper meniscofemoral portion and a lower meniscotibial portion.
The anterior fibers of the MCL are taut in flexion and can be palpated easily in this position. The posterior fibers, which are taut in extension, blend intimately with the capsule and with the medial border of the medial meniscus, making them difficult to palpate.
It would appear that the MCL is the primary stabilizer of the medial side of the knee against valgus forces, and external rotation of the tibia, especially when the knee is flexed.
See Also:
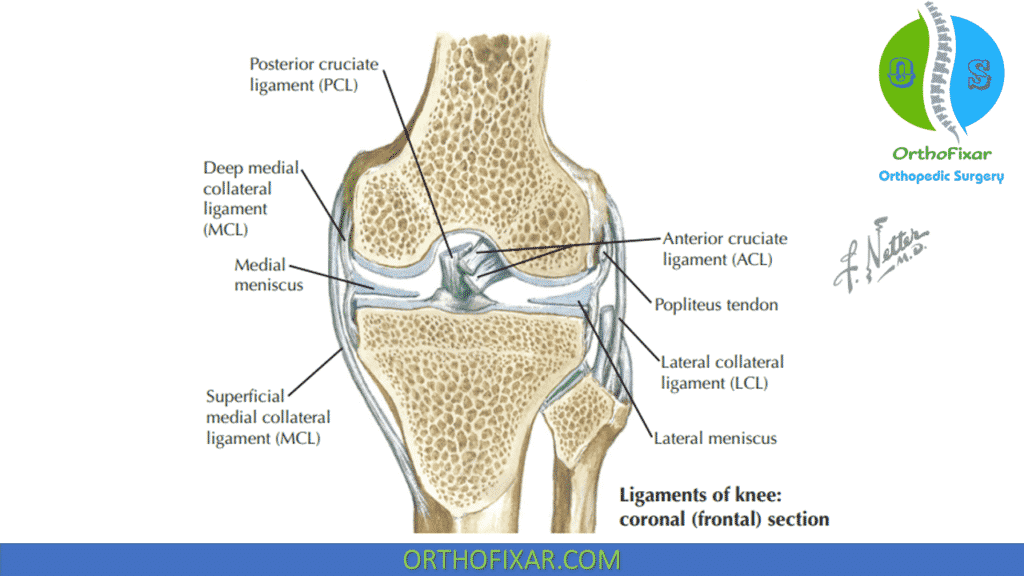
Lateral Collateral Ligament
The LCL, or fibular collateral ligament, arises from the lateral femoral condyle and runs distally and posteriorly to insert into the head of the fibula. The LCL forms part of the so-called arcuate-ligamentous complex. This complex also comprises the biceps femoris tendon, iliotibial tract, and the popliteus.
The cord-like LCL develops independently, and remains completely free from the joint capsule and the lateral meniscus. It is separated from these structures by the popliteus tendon, and straddled by the split tendon of the biceps femoris.
The LCL can be divided into three parts:
- Anterior: This part consists of the joint capsule.
- Middle: This part is considered to be part of the iliotibial band (ITB) and covers the capsular ligament.
- Posterior: This Y-shaped portion of the ligament is part of the arcuate-ligamentous complex, which supports the posterior capsule.
The main function of the LCL is to resist varus forces. It offers the majority of the varus restraint at 25 degrees of knee flexion, and in full extension.
See Also: Varus Test of the knee
Other Ligaments
Some structures in the knee clearly augment the functions of the ACL and the PCL. These structures are known as secondary restraints. The secondary restraints include the structures in the posterolateral and posteromedial corners of the knee, which serve to control anterior tibial translation relative to the femur.
Dynamic stability synergistic to the PCL is provided by unopposed contraction of the quadriceps complex, which increases anterior tibial translation. Conversely, an isolated contraction of the hamstrings results in a posterior translation of the tibia, which is synergistic to the ACL. Cocontraction of the hamstrings and the quadriceps has been theorized to minimize tibial translation in either direction. The popliteus muscle–tendon complex (PMTC) contributes to both static and dynamic posterolateral knee joint stabilization. During concentric activation, the popliteus internally rotates the tibia on the femur. During eccentric activation, it serves as a secondary restraint to tibial external rotation on the femur
The knee joint is also strengthened externally by the many other ligaments:
- The patellar ligament, or patellar tendon, lies in the thickened portion of the quadriceps femoris tendon between the top of the patella and the tibia. The patellar ligament strengthens the anterior portion of the knee joint and prevents the lower leg from being flexed excessively.
- The oblique popliteal ligament, located on the posterior surface of the knee joint, is a dense thickening in the posterior capsule made up of a continuation of the popliteal tendon and part of the insertion of the semimembranosus. It arises posterior to the medial condyle of the tibia and extends superomedially to attach to the posterior fibrous capsule. The oblique popliteal ligament provides reinforcement to the lateral capsule, limits anteromedial rotation of the tibia, and prevents hyperextension of the knee.
- The fabella is located in the posterolateral corner of the knee and may be osseous or cartilaginous in makeup. When the fabella is present, there is a fabellofibular ligament, which courses superiorly and obliquely from the lateral head of the gastrocnemius to the fibular styloid. The fabellofibular ligament helps prevent excessive internal rotation of the tibia and adds further ligamentous support on the lateral and posterolateral aspects of the knee.
- The arcuate ligament provides further support to the posterolateral joint capsule. Arising from the fibular head, the arcuate ligament passes over the popliteus muscle, where it diverges into the intercondylar area of the tibia and the posterior aspect of the femur’s lateral epicondyle. The arcuate ligament assists the cruciate ligaments in controlling posterolateral rotational instability. Injury to this area results in increased external rotation of the tibia on the femur.
- The popliteofibular ligament (also referred to as the short external lateral ligament, the popliteofibular fascicles, fibular origin of the popliteus, and the popliteofibular fibers), is a Y-shaped structure with origins from the tibia and fibula. Inserting on the femur, the popliteofibular ligament is a key stabilizer against posterior translation, varus forces, and external rotation.
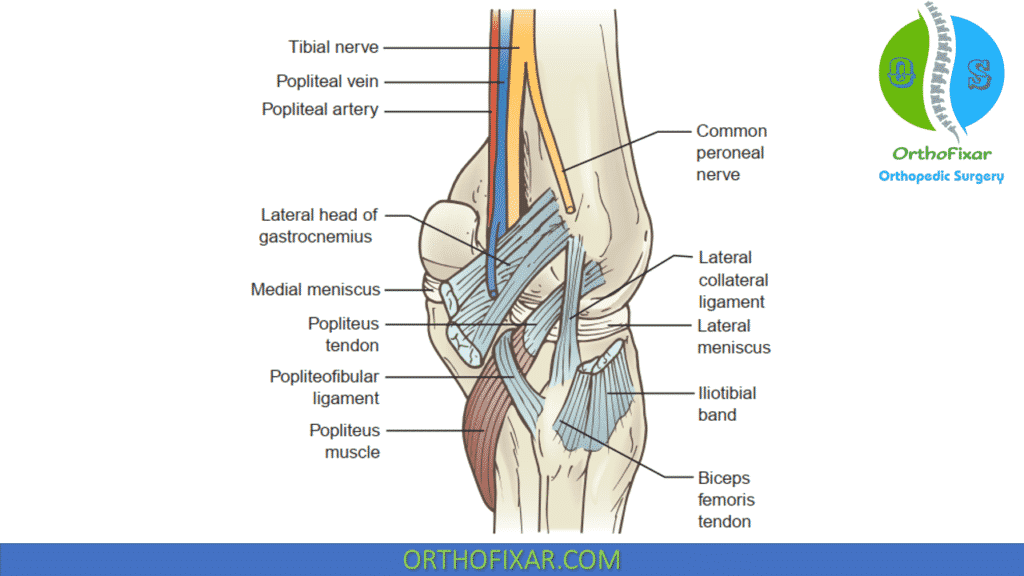
Posterolateral Corner
The knee posterolateral corner (PLC), also known as the lateral complex and posterolateral complex, has been referred to as “the dark side of the knee” for its varied and relatively poorly understood anatomy.
Consisting of both dynamic and static stabilizers, the PLC is integral in providing stability against varus stress, external tibial rotation, and anterior and posterior forces about the knee.
The combined contributions of the anatomical elements of this structure are greater than the sum of the combined parts; the integrity of its individual elements can be disrupted with relatively little joint instability. However, if multiple structures are disrupted, profound instability can result.
References
- Fisher M, Bordoni B. Anatomy, Bony Pelvis and Lower Limb, Pelvic Joints. 2021 Jul 26. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan–. PMID: 30860758.
- Pick TP, Howden R: Gray’s Anatomy, 15th ed. New York, NY: Barnes & Noble Books, 1995.
- Schultz RA, Miller DC, Kerr CS, et al: Mechanoreceptors in human cruciate ligaments. A histological study. J Bone Joint Surg Am 66:1072– 1076, 1984.
- Beynnon BD, Good L, Risberg MA: The effect of bracing on proprioception of knees with anterior cruciate ligament injury. J Orthop Sports Phys Ther 32:11–15, 2002.
- Biedert RM, Stauffer E, Friederich NF: Occurrence of free nerve endings in the soft tissue of the knee joint. A histologic investigation. Am J Sports Med 2:430–433, 1992.
- HausJ,Halata Z,RefiorHJ: Proprioceptionin the human anterior cruciate ligament. Basic morphology. A light microscopic, scanning and transmission electron microscopic study. Zeitschr Orthop 130:484–494, 1992.
- Beynnon B, Howe JG, Pope MH, et al: The measurement of anterior cruciate ligament strain in vivo. Int Orthop 16:1–12, 1992.
- Johnson RJ: Acute knee injuries: An introduction. In: Harries M, Williams C, Stanish WD, et al., eds. Oxford Textbook of Sports Medicine. New York, NY: Oxford University Press, 1994:342–344.
- Arnoczky SP, Matyas JR, Buckwalter JA, et al: Anatomy of the anterior cruciate ligament. In: Jackson DW, Arnoczky SP, Woo SL-Y, et al, eds. The Anterior Cruciate Ligament. Current and Future Concepts. New York, NY: Raven Press, 1993:5–22.
- Samuelson TS, Drez D, Maletis GB: Anterior cruciate ligament graft rotation: Reproduction of normal graft rotation. Am J Sports Med 24:67– 71, 1996.
- Gomez-Barrena E, Munuera L, Martinez-Moreno E: Neural pathways of anterior cruciate ligament traced to the spinal ganglia. Trans Orthop Res Soc 17:503, 1992.
- Haut RC: The mechanical and viscoelastic properties of the anterior cruciate ligament and of ACL fascicles. In: Jackson DW, Arnoczky SP, Woo SL-Y, et al, eds. The Anterior Cruciate Ligament. Current and Future Concepts. New York, NY: Raven Press, 1993:63–73.
- Kwan MK, Lin TH, Woo SL-Y: On the viscoelastic properties of the anteromedial bundle of the anterior cruciate ligament. J Biomech 26:447– 452, 1993.
- Frank CB, Jackson DW: The science of reconstruction of the anterior cruciate ligament. J Bone Joint Surg 79:1556–1576, 1997.
- Takai S, Woo SL-Y, Livesay GA, et al: Determination of the in situ loads on the human anterior cruciate ligament. J Orthop Res 11:686– 695, 1993.
- Butler DL, Guan Y, Kay MD, et al: Location-dependent variations in the material properties of the anterior cruciate ligament. J Biomech 25:511– 518, 1992.
- Butler DL, Noyes FR, Grood ES: Ligamentous restraints to anterior posterior drawer in the human knee: A biomechanical study. J Bone Joint Surg Am 62-A:259–270, 1980.
- Arnoczky SP: Anatomy of the anterior cruciate ligament. In: Urist MR, ed. Clinical Orthopedics and Related Research. Philadelphia, PA: J.B. Lippincott, 1983:19–20.
- Cabaud HE: Biomechanics of the anterior cruciate ligament. In: Urist MR, ed. Clinical Orthopedics and Related Research. Philadelphia, PA: J.B. Lippincott, 1983:26–30.
- Kennedy JC, Hawkins RJ, Willis RB: Strain gauge analysis of knee ligaments. Clin Orthop 129:225–229, 1977.
- Bargar WL, Moreland JR, Markolf KL, et al: In vivo stability testing of post meniscectomy knees. Clin Orthop 150:247–252, 1980.
- Fleming BC, Renstrom PA, Beynnon BD, et al: The effect of weightbearing and external loading on anterior cruciate ligament strain. J Biomech 34:163–170, 1999.
- Fleming BC, Beynnon BD, Renstrom PA, et al: The strain behavior of the anterior cruciate ligament during stair climbing: An in vivo study. J Arthrosc Rel Surg 15:185–191, 1999.
- O’Connor JJ, Zavatsky A: Anterior cruciate ligament function in the normal knee. In: Jackson DW, Arnoczky SP, Woo SL-Y, et al, eds. The Anterior Cruciate Ligament, Current and Future Concepts. New York, NY: Raven Press, 1993:39–52.
- O’Connor JJ, Zavatsky A: Anterior cruciate ligament forces in activity. In: Jackson DW, Arnoczky SP, Woo SL-Y, et al, eds. The Anterior Cruciate Ligament, Current and Future Concepts. New York, NY: Raven Press, 1993:131–140.
- Beynnon BD, Johnson RJ, Fleming BC: The mechanics of anterior cruciate ligament reconstruction. In: Jackson DW, Arnoczky SP, Woo SL-Y, et al, eds. The Anterior Cruciate Ligament Current and Future Concepts. New York, NY: Raven Press, 1993:259–272.
- Noyes FR, Grood ES, Butler DL, et al: Clinical biomechanics of the knee: Ligamentous restraints and functional stability. In: Funk FJJ, ed. American Academy of Orthopedic Surgeon’s Symposium on the Athlete , s Knee. St. Louis, MI: C.V. Mosby, 1980:1–35.
- Harner CD, Xerogeanes JW, Livesay GA, et al: The human posterior cruciate ligament complex: An interdisciplinary study. Ligament morphology and biomechanical evaluation. Am J Sports Med 23:736–745, 1995.
- Kennedy JC, Hawkins RJ, Willis RB, et al: Tension studies of human knee ligaments, yield point, ultimate failure, and disruption of the cruciate and tibial collateral ligaments. J Bone Joint Surg 58-A:350, 1976.
- Van Dommelen BA, Fowler PJ: Anatomy of the posterior cruciate ligament. A review. Am J Sports Med 17:24–29, 1989.
- Grover JS, Bassett LW, Gross ML, et al: Posterior cruciate ligament: MR imaging. Radiology 174:527–530, 1990.
- Markolf KL, Wascher DC, Finerman GAM: Direct in vitro measurement of forces in the cruciate ligaments. Part II: The effect of section of the posterolateral structures. J Bone Joint Surg 75-A:387–394, 1993.
- Hughston JC, Andrews JR, Cross MJ, et al: Classification of knee ligament instabilities. Part 1. J Bone Joint Surg 58A:159–172, 1976.
- Grood ES, Stowers SF, Noyes FR: Limits of movement in the human knee. Effect of sectioning the posterior cruciate ligament and posterolateral structures. J Bone Joint Surg Am 70:88–97, 1988.
- Heller L, Langman J: The Menisco-Femoral Ligaments of the Human Knee. J Bone Joint Surg Br 46:307–313, 1964.
- Amis AA, Gupte CM, Bull AM, et al: Anatomy of the posterior cruciate ligament and the meniscofemoral ligaments. Knee Surg Sports Traumatol Arthrosc 14:257–63, 2006.
- Clancy WG, Jr., Shelbourne KD, Zoellner GB, et al: Treatment of knee joint instability secondary to rupture of the posterior cruciate ligament. Report of a new procedure. J Bone Joint Surg Am 65:310–322, 1983.
- Merida-Velasco JA, Sanchez-Montesionos I, Espin-Ferra J, et al: Development of the human knee joint ligaments. Anat Rec 248:259–268, 1997.
- Hughston JC, Jacobson KE: Chronic posterolateral rotatory instability of the knee. J Bone Joint Surg 67A:351–359, 1985.
- Reinold MM, Berkson EM, Asnis P, et al: Knee: Ligamentous and patella tendon injuries. In: Magee DJ, Zachazewski JE, Quillen WS, eds. Pathology and intervention in musculoskeletal rehabilitation. St. Louis, MI: Saunders, 2009:528–578.
- Tria AJ: Ligaments of the knee. New York, NY: Churchill Livingstone, 1995.
- Grood ES, Noyes FR, Butler DL, et al: Ligamentous and capsular restraints preventing medial and lateral laxity in intact human cadaver knees. J Bone Joint Surg 63A:1257–1269, 1981.
- Greenfield B, Tovin BJ, Bennett JG: Knee. In: Wadsworth C, ed. Current Concepts of Orthopedic Physical Therapy. La Crosse, WI: Orthopaedic Section, APTA, 2001.
- Sudasna S, Harnsiriwattanagit K: The ligamentous structures of the posterolateral aspect of the knee. Bull Hosp Joint Dis Orthop Inst 50:35– 40, 1990.
- Kaplan EB: The fabellofibular and short lateral ligaments of the knee joint. J Bone Joint Surg 43A:169–179, 1961.
- DeLee JC, Riley MD: Acute straight lateral instability of the knee. Am J Sports Med 11:404–411, 1983.
- Nicholas JA: Lateral instability of the knee. Orthop Rev 6:33–44, 1977.
- Terry GC, Norwood LA, Hughston JC, et al: How iliotibial tract injuries of the knee combine with acute anterior cruciate ligament tears to influence abnormal anterior tibial displacement. Am J Sports Med 21:55–60, 1993.
- Wroble RR, Grood ES, Cummings JS, et al: The role of the lateral extraarticular restraints in the anterior cruciate ligament-deficient knee. Am J Sports Med 21:257–262, 1993.
- Last RJ: The popliteus muscle and the lateral meniscus. J Bone Joint Surg 32B:93–99, 1950.
- Pasque C, Noyes FR, Gibbons M, et al: The role of the popliteofibular ligament and the tendon of popliteus in providing stability in the human knee. J Bone Joint Surg Br 85:292–298, 2003.
- Watanabe Y, Moriya H, Takahashi K, et al: Functional anatomy of the posterolateral structures of the knee. J Arthroscopy Rel Surg 9:57–62, 1993.