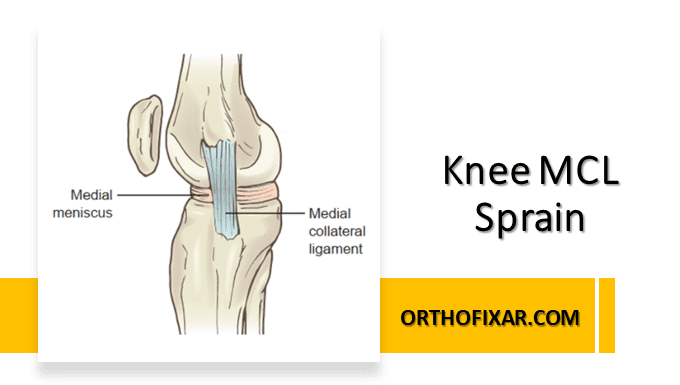
The Knee MCL sprain (Medial Collateral Ligament Sprain) is a result of tensile forces, most commonly a valgus stress caused by a blow to the lateral aspect of the knee. Injuries most commonly occur at the femoral origin of the MCL ligament.
MCL Function
- When the knee is fully extended, the valgus force is dissipated by the superficial and deep layers of the MCL, the anteromedial and posteromedial joint capsule, and the tendons of the pes anserine group.
- When the knee is flexed beyond 20 degrees, the superficial layer of the MCL becomes more responsible for resisting valgus forces.
MCL Sprain Mechanism of Injury
Noncontact valgus loading or a rotational force being placed on the knee can injure the MCL.
Ruptures of the deep layer of the MCL are almost always associated with a rupture of the superficial layer. Medial collateral ligament sprains may occur in isolation, but, because of the deep layer’s communication with the medial joint capsule and medial meniscus, concurrent injury to these structures must always be suspected.
See Also: Knee Ligaments Anatomy
Extreme valgus forces or rotational forces placed on the knee at the time of injury may also lead to the involvement of the ACL or the posteromedial corner.
Fractures of the distal femoral physis can mimic a third degree MCL sprain in growing patients. Patellar dislocations can occur secondary to a valgus force placed on the knee. Therefore, all MCL sprains must include an evaluation of the patella for lateral instability before stress testing.

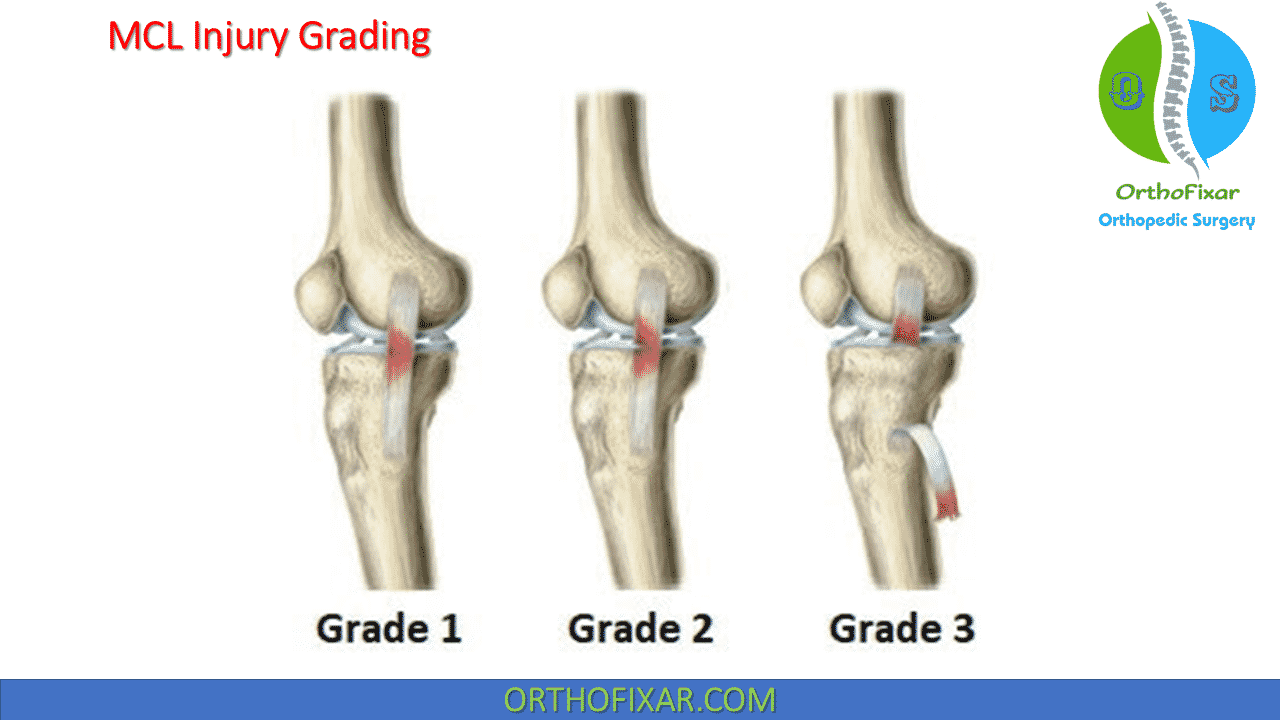
MCL Injury Grading
| Grade | Description |
|---|---|
| Grade I | – mild severity – no loss of ligamentous integrity (stretch injury) – minimal torn fibers |
| Grade II | – moderate severity – incomplete tearing of MCL (partial tear) – increased joint laxity – end point found at 30 degrees of flexion with valgus stress – fibers remain apposed |
| Grade III | – severe – complete disruption of ligament (complete tear) – gross laxity – no end point with valgus stress at 30 degrees of knee flexion |
MCL Sprain Symptoms
MCL Sprain represents with acute pain on the medial aspect of the knee, on, above, or below the joint line, depending on the location of the damage. Swelling may be present along the medial aspect of the knee.
Tenderness along the length of the MCL from its origin below the adductor tubercle to the insertion on the medial tibial flare.
Fluid escaping from the knee joint to the area around the MCL is an indirect sign of a complete rupture of the deep layer of the MCL.
The valgus stress test performed in complete extension and 25 degrees of flexion is used to manually determine the integrity of the MCL.
A complete MCL tear, marked by the medial joint line opening 8mm to 15mm and marked by an empty end-feel strongly suggests that the ACL and/or PCL have also been ruptured. Complete ruptures of the MCL are associated with ACL sprain in about 80% of cases.
See Also: Valgus Test of the Knee
Imaging
Plain film radiographs may be ordered to rule out epiphyseal fractures in children or avulsion fractures in adults.
MRI is the diagnostic modality of the MCL injury.
In chronic injuries, calcification may be present at the medial femoral condyle insertion (Pellegrini-Stieda sign).

Medial Collateral Ligament Sprain Treatment
Most MCL injuries are treated nonoperatively, even when surgical repair of other structures, including the ACL, is warranted, because the MCL ligament lies within the soft tissue matrix of the medial aspect of the knee and enjoys an adequate blood supply for healing.
An aggressive functional rehabilitation program provides long-term stability against valgus forces. Successful nonoperative rehabilitation of the MCL includes protecting the joint from valgus stress while healing, providing an optimal healing environment within the MCL through a controlled restoration of ROM, and adequate strengthening and proprioceptive training of the lower extremity.
Use of a knee brace with the ability to limit ROM may be indicated in grade II and III injuries to control further injurious stress and provide the restoration of motion without compromising healing within the ligament.
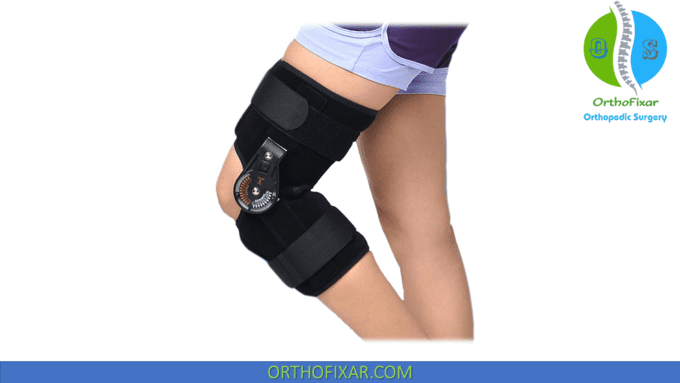
Clinical work has shown the advantage of nonoperative treatment (bracing) of an associated MCL injury in patients receiving an ACL reconstruction.
If a period of conservative treatment does not restore valgus stability, the physician may opt to reconstruct the MCL with a third-degree sprain when an associated ACL injury is present.
MCL ligament repair is indicated in acute or sub-acute grade III MCL injuries, while MCL reconstruction is used in chronic injury or in case of insufficient tissue for repair where semitendinosus autograft or hamstring, tibialis anterior or Achilles tendon allograft can be used.
Pellegrini-Stieda syndrome, which can occur with chronic MCL injury, usually responds to a brief period of immobilization followed by progressive motion.
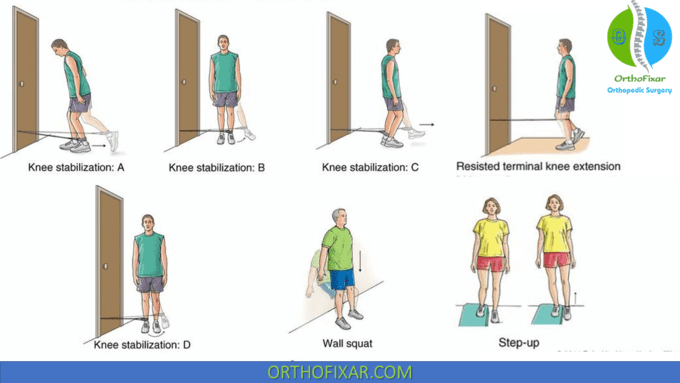
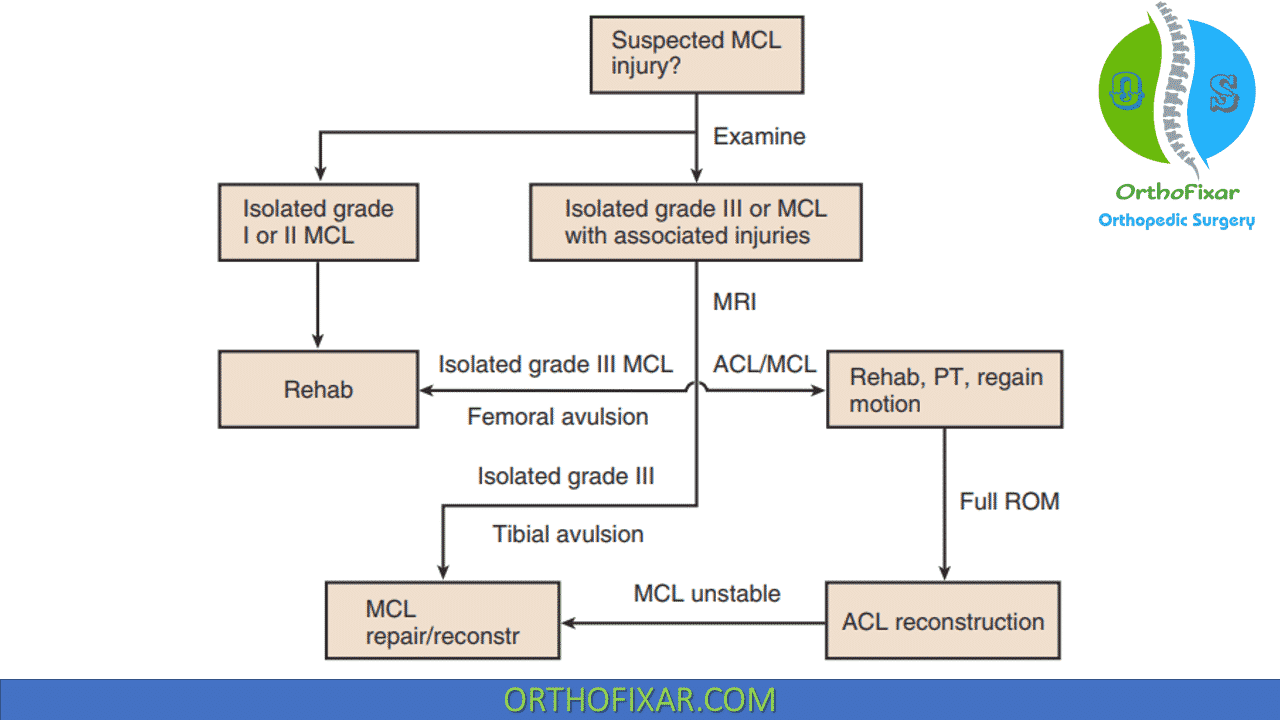
References
- Rasenberg EI, Lemmens JA, van Kampen A, Schoots F, Bloo HJ, Wagemakers HP, Blankevoort L. Grading medial collateral ligament injury: comparison of MR imaging and instrumented valgus-varus laxity test-device. A prospective double-blind patient study. Eur J Radiol. 1995 Nov;21(1):18-24. doi: 10.1016/0720-048x(95)00660-i. PMID: 8654454.
- Sawant, M, Murty, AN, and Ireland, J: Valgus knee injuries: evaluation and documentation using a simple technique of stress radiography. Knee, 11:25, 2004.
- Indelicato, PA: Isolated medial collateral ligament injuries of the knee. J Am Acad Ortho Surg, 3:9, 1995.
- Stannard, JP: Medial and posteromedial instability of the knee: evaluation, treatment, and results. Sports Med Arthrosc Rev, 18:1263, 2010.
- Robbins, AJ, Newman, AP, and Burks, RT: Postoperative return of motion in anterior cruciate ligament and medial collateral ligament injuries: the effects of medial collateral ligament rupture location. Am J Sports Med, 21:20, 1993.
- Veenema, KR: Valgus knee instability in an adolescent: ligament sprain or physeal fracture? Phys Sportsmed, 27:62, 1999.
- Kastelein, M, et al: Assessing medial collateral ligament knee lesions in general practice. Am J Med, 121:982, 2008.
- Laprade, RF, and Wijdicks, CA: The management of injuries to the medial side of the knee. J Orthop Sports Phys Ther, 42:221, 2012.
- Reider, B, et al: Treatment of isolated medial collateral ligament injuries with early functional rehabilitation: a five-year follow-up study. Am J Sports Med, 22:470, 1993.