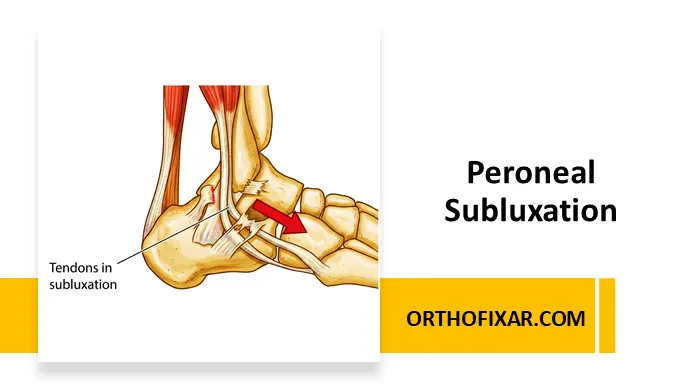
Peroneal tendon subluxation and dislocation are uncommon but important causes of persistent lateral ankle pain, particularly in athletes and highly active individuals. These injuries are frequently misdiagnosed as a simple lateral ankle sprain because they often occur simultaneously with lateral ligament injuries and present with similar symptoms.
Delayed or missed diagnosis may lead to chronic instability, recurrent tendon dislocation, pain, weakness, and long-term ankle dysfunction.
What Is Peroneal Tendon Subluxation?
Peroneal subluxation occurs when the peroneal tendons partially slip out of their normal position behind the fibula. Complete displacement of the tendons is referred to as peroneal tendon dislocation.
The condition most commonly affects:
- Skiers
- Soccer players
- Basketball players
- Rugby players
- Football players
- Ice skaters
- Tennis players
- Gymnasts
Peroneal tendon subluxation injury usually results from sudden forced dorsiflexion or inversion of the ankle during sports activities. Classic cases have been described in skiers when the ski tips abruptly dig into the snow, causing sudden deceleration with the ankle forced into dorsiflexion inside the ski boot.

Epidemiology
Peroneal subluxation and dislocation are relatively uncommon injuries but are increasingly recognized in athletic populations.
Key epidemiologic points include:
- Most commonly seen in young athletic individuals
- Frequently associated with sports involving cutting, jumping, or sudden directional changes
- Often underdiagnosed or mistaken for ankle sprains
- Chronic instability may develop if acute injuries are untreated
- Recurrent dislocation is common after missed diagnosis
Related Anatomy
The stability of the peroneal tendons depends primarily on the:
- Superior peroneal retinaculum (SPR)
- Retrofibular groove
- Fibular morphology
The superior peroneal retinaculum acts as the main restraint preventing tendon displacement at the lateral malleolus.
It:
- Extends approximately 3.5 cm proximally from the tip of the lateral malleolus
- Attaches posterolaterally to the calcaneus
- Blends with the fascia adjacent to the Achilles tendon
Anatomical Risk Factors
Several anatomical abnormalities predispose patients to recurrent instability:
- Incompetent superior peroneal retinaculum
- Shallow fibular groove
- Convex posterior distal fibula
- Low-lying peroneus brevis muscle belly
- Presence of a peroneus quartus muscle
- Congenital vertical talus
- Talipes planovalgus
Mechanism of Injury
Peroneal tendon instability typically occurs during sudden forceful contraction of the peroneal muscles while the foot is dorsiflexed.
Common injury mechanisms include:
- Forced ankle dorsiflexion
- Inversion injuries
- Sudden deceleration injuries
- Violent eccentric contraction of the peroneal muscles
The tendons may:
- Displace within the tendon sheath
- Dislocate outside the sheath and fibular groove
- Move anteriorly over the distal fibula
The superior peroneal retinaculum may:
- Stretch
- Avulse
- Tear completely
leading to tendon instability.
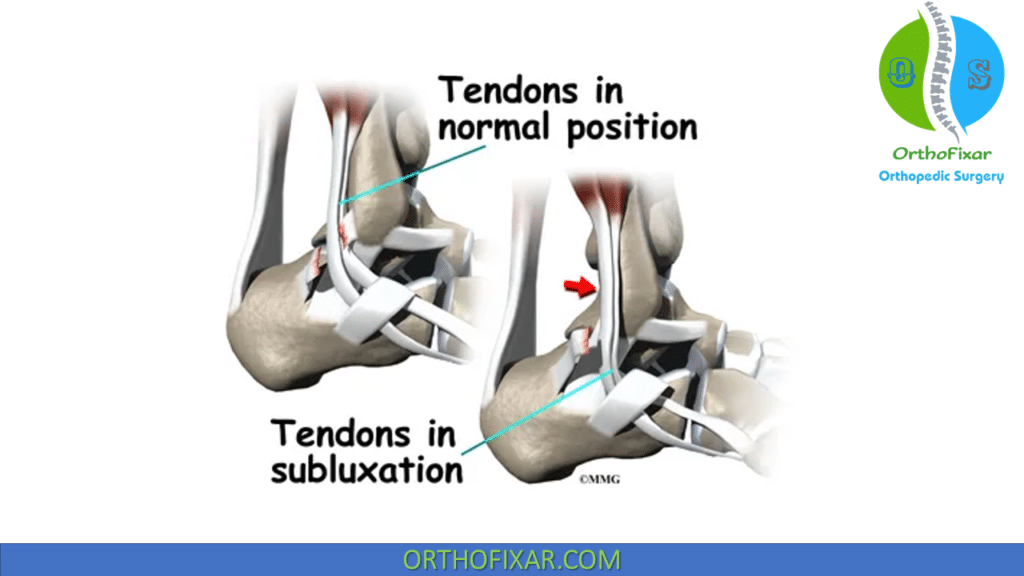
Peroneal Subluxation Classification
Peroneal tendon subluxation injuries have been classified primarily by location.
In one classification system (Shawen and Anderson):
- Zone I injuries involve the fibular groove and usually the peroneus brevis tendon;
- Zone II injuries are located in the cuboid tunnel and primarily involve the peroneus longus tendon.
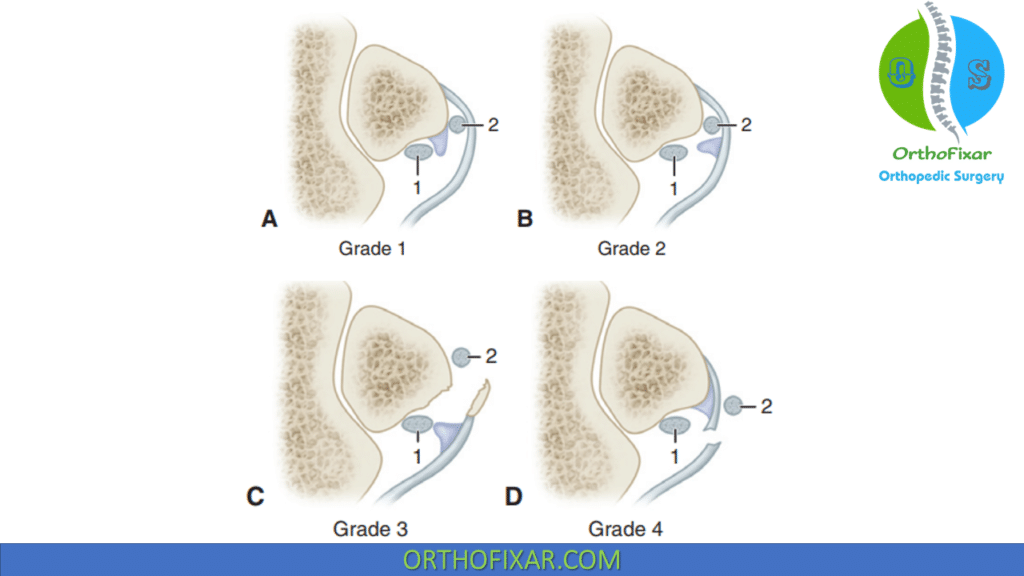
In Oden’s modification of the classification of Eckert and Davis, injuries are divided into four grades:
- In grade 1 lesions, the most common pattern (>50%), the superior peroneal retinaculum is elevated off the fibula with the peroneal tendons coming to lie between the bone and the periosteum.
- In grade 2 lesions the fibrocartilaginous ridge behind the lateral insertion of the superior peroneal retinaculum is avulsed along with the retinaculum and the tendons are displaced beneath the ridge.
- Grade 3 lesions involve an avulsion of a small cortical osseous fragment from the fibular insertion of the superior peroneal retinaculum with the tendons dislocating beneath the fibular fragment.
- Grade 4 lesions, the least common type, involve a complete avulsion or rupture of the superior peroneal retinaculum with the tendons lying external and superficial to the retinaculum.
More recently, Raikin et al. proposed intrasheath peroneal subluxation within the peroneal groove beneath an otherwise intact superior peroneal retinaculum as a subgroup of peroneal subluxation. Two types of these intrasheath subluxations were described:
- Type A, in which there is no peroneal tendon tear and the tendons momentarily switch their relative positions (the peroneus longus tendon lies deep to the peroneus brevis tendon),
- Type B, in which in the peroneus longus subluxes through a longitudinal tear in the peroneus brevis tendon

Peroneal Subluxation Symptoms & Signs
Peroneal tendon subluxation often mimics a lateral ankle sprain.
Common symptoms include:
- Lateral ankle pain
- Swelling
- Ecchymosis
- Snapping sensation around the ankle
- Clicking or popping during movement
- Feeling of instability
- Recurrent ankle pain during sports
Patients frequently report symptoms while:
- Ascending stairs
- Running
- Cutting or pivoting
- Performing ankle circumduction
Physical Examination
Important examination findings include:
- Tenderness posterior to the lateral malleolus
- Pain with resisted eversion
- Apprehension during ankle motion
- Palpable tendon snapping
- Tendon dislocation during circumduction testing
Provocative testing is performed by placing the foot into:
- Dorsiflexion
- Eversion
- External rotation
while resisting inversion and plantarflexion.
Key Clinical Point
Unlike lateral ankle ligament injuries the anterior drawer test is usually negative in isolated peroneal tendon instability.
Differential Diagnosis of Peroneal Subluxation
The differential diagnosis should include degenerative, traumatic, and congenital causes of lateral ankle pain, especially lateral ankle ligament sprain.
- Tendon Subluxation/Dislocation
- Lateral ligament ankle sprain
- Achilles tendon rupture
- Fracture: malleolus, fifth metatarsal, cuboid
- Stress fracture: calcaneus
- Sinus tarsi syndrome
- Calcaneocuboid syndrome
- Peroneal tendinopathy
- Degenerative joint disease
- Tarsal coalition
- Osteochondral lesion of the talus
- Loose bodies in the ankle or subtalar joint
- Sural neuritis
- Radiculopathy
- Malignant or benign neoplasm
- Accessory muscle or bone
Radiology
Radiographs usually are negative; with a grade 3 injury, a “fleck” of bone may be seen off the posterior distal fibula.
MRI can be used to identify injury to the superior peroneal retinaculum, the peroneal tendons, and supporting soft tissues, as well as identify anomalous structures such as the peroneus quartus or a low-lying peroneal brevis muscle belly.
Kinematic MRI of the ankle moving from dorsiflexion to plantar flexion has been suggested to be superior to static imaging because the pathological process is position dependent.
Ultrasonography also has been reported to be effective for dynamically evaluating peroneal tendon subluxation.
Peroneal Subluxation treatment
Treatment depends on:
- Acute versus chronic injury
- Degree of instability
- Associated tendon tears
- Patient age
- Athletic demands
- Bone anatomy
Nonoperative Treatment
Conservative management may be considered in acute stable injuries.
Nonoperative Protocol
Treatment includes:
- Reduction of the tendons
- Immobilization in a well-molded cast
- Slight plantarflexion and inversion positioning
- Non–weight-bearing for approximately 6 weeks
The goal is to:
- Relax the superior peroneal retinaculum
- Maintain tendon reduction
- Allow retinacular healing
Limitations of Conservative Treatment
Nonoperative treatment has relatively high failure rates, especially in:
- Athletes
- Chronic injuries
- Recurrent dislocations
Surgical Treatment
Surgery is generally recommended for:
- Chronic instability
- Recurrent dislocation
- Failed conservative treatment
- Competitive athletes
- Associated tendon tears
Surgical Techniques
Superior Peroneal Retinaculum Repair
Direct reconstruction or repair of the retinaculum.
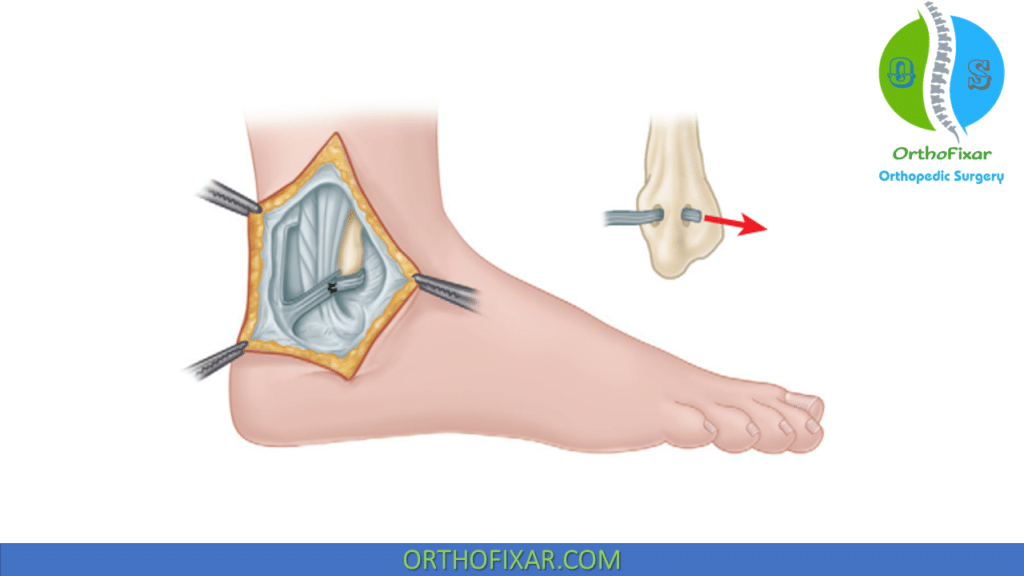
Groove Deepening Procedures
Fibular groove deepening improves tendon containment.
Bone Block Procedures
Bone grafts or osteotomies prevent tendon displacement.
Tendon Rerouting Procedures
Tendons are repositioned beneath stabilizing structures.
Tenoplasty
Used when tendon tears or degeneration are present.
Achilles Tendon Flap Procedures
The Jones procedure uses a flap of the Achilles tendon sheath passed through the lateral malleolus to stabilize the tendons.
Postoperative Rehabilitation
Postoperative care typically includes:
Early Phase
- Splinting for 1–2 weeks
- Slight plantarflexion and inversion positioning
Intermediate Phase
- Passive range-of-motion exercises
- Scar prevention strategies
- Tendon mobilization
Late Phase
- Weight-bearing at approximately 6 weeks
- Progressive strengthening
- Functional rehabilitation
- Return-to-sport training
Prognosis
With accurate diagnosis and appropriate treatment:
- Most patients achieve excellent outcomes
- Athletes often return to sports successfully
- Surgical stabilization has high success rates
- Chronic untreated instability may result in persistent pain and tendon degeneration
Key Clinical Pearls
- Peroneal tendon subluxation is commonly mistaken for a lateral ankle sprain.
- Tenderness posterior to the fibula is an important diagnostic clue.
- The anterior drawer test is usually negative.
- Dynamic ultrasound is highly effective for diagnosis.
- Chronic instability generally requires surgical treatment.
- Early diagnosis improves outcomes and reduces recurrence risk.
References & More
- Campbel’s Operative Orthopaedics 12th edition Book.
- Walt J, Massey P. Peroneal Tendon Syndromes. [Updated 2022 May 29]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: Pubmed
- Roth JA, Taylor WC, Whalen J. Peroneal tendon subluxation: the other lateral ankle injury. Br J Sports Med. 2010 Nov;44(14):1047-53. doi: 10.1136/bjsm.2008.057182. Epub 2009 Nov 27. PMID: 19945971.
- van Dijk PA, Gianakos AL, Kerkhoffs GM, Kennedy JG. Return to sports and clinical outcomes in patients treated for peroneal tendon dislocation: a systematic review. Knee Surg Sports Traumatol Arthrosc. 2016 Apr;24(4):1155-64. doi: 10.1007/s00167-015-3833-z. Epub 2015 Oct 30. PMID: 26519186; PMCID: PMC4823328.
- Raikin SM, Elias I, Nazarian LN: Intrasheath subluxation of the peroneal tendon, J Bone Joint Surg 90A:992, 2008.)