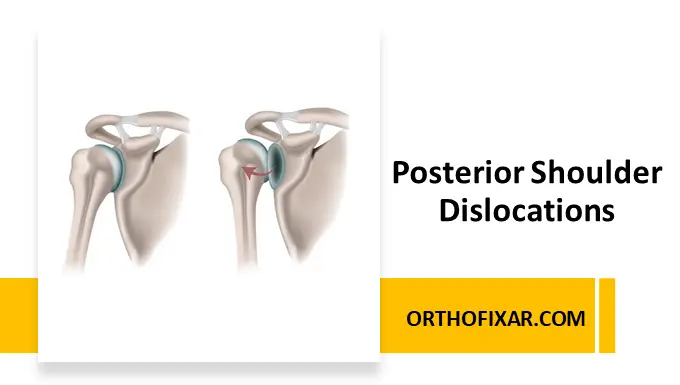
Posterior Shoulder Dislocations is an uncommon but clinically important shoulder injury. Despite its rarity, it carries a high risk of missed diagnosis, particularly in acute care settings. This condition demands a high index of suspicion and careful radiographic evaluation to avoid missed diagnosis and long-term morbidity.
Incidence
Posterior Shoulder Dislocations:
- Account for 2%–4% of all shoulder dislocations
- Represent about 2% of shoulder injuries overall
- Are missed in 60%–80% of initial evaluations, making them one of the most frequently overlooked joint dislocations
Mechanism of Injury
Indirect Trauma (Most Common)
- Posterior Shoulder Dislocation Occurs when the shoulder is positioned in:
- Adduction
- Flexion
- Internal rotation
- Common scenarios:
- Seizures
- Electrical shock
- Pathophysiology:
- Powerful contraction of internal rotators (latissimus dorsi, pectoralis major, subscapularis)
- These overpower weaker external rotators (infraspinatus, teres minor), forcing the humeral head posteriorly
Direct Trauma
- Force applied to the anterior shoulder
- Results in posterior translation of the humeral head
See Also: Anterior Glenohumeral Dislocation
Clinical Evaluation
Posterior shoulder dislocations are often subtle in presentation:
Typical Findings
- Arm held in:
- Adduction
- Internal rotation
- Limited external rotation (often < 0°)
- Limited forward elevation (often < 90°)
Physical Examination Signs
- Flattened anterior shoulder contour
- Prominent coracoid process
- Palpable posterior mass (displaced humeral head)
Neurovascular Assessment
- Essential to evaluate:
- Axillary nerve function
- Neurovascular injuries are less common than in anterior dislocations but still possible
Radiographic Evaluation
A complete trauma series is mandatory:
- AP view
- Scapular-Y view
- Axillary view (most diagnostic)
If standard axillary view is not feasible:
- Use Velpeau axillary view
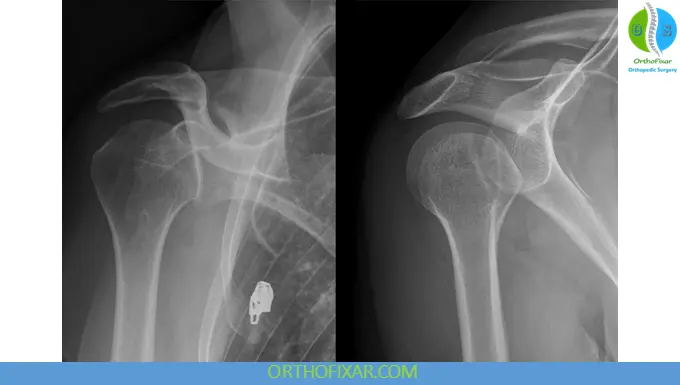
Key Radiographic Signs (AP View)
- Loss of normal humeral head–glenoid overlap
- Vacant glenoid sign (>6 mm space)
- Trough sign (reverse Hill-Sachs lesion; seen in ~75%)
- Internal rotation appearance (“light bulb sign”)
- Loss of humeral neck profile
Advanced Imaging
- CT scan:
- Essential for evaluating humeral head impaction defects
- Determines percentage of articular surface involvement
See Also: Shoulder X-ray Views
Classification
Etiologic Classification
- Traumatic: sprain, subluxation, dislocation (acute or recurrent)
- Atraumatic:
- Voluntary
- Congenital
- Acquired (microtrauma)
Anatomic Classification
- Subacromial (98%):
- Humeral head displaced posteriorly without gross displacement
- Often associated with reverse Hill-Sachs lesion
- Subglenoid (rare):
- Humeral head posterior and inferior to glenoid
- Subspinous (rare):
- Humeral head medial to acromion and below scapular spine
Posterior Shoulder Dislocation Treatment
Nonoperative Management
Closed Reduction
- Requires:
- Adequate sedation and analgesia
- Often general anesthesia
- Technique:
- Traction applied to adducted arm
- Gentle anterior repositioning of humeral head
⚠️ Important Precaution
- Avoid forced external rotation → risk of fracture if humeral head is locked
Special Consideration
- If impaction fracture is locked:
- Combine axial traction + lateral traction
Post-reduction Care
- Immobilization:
- Sling and swathe
- External rotation positioning for large defects
- Early rehab:
- Deltoid isometrics
- Gradual strengthening of rotator cuff
See Also: Shoulder Reduction Techniques
Operative Management
Indications
- Irreducible posterior shoulder dislocation
- Large humeral head defect (reverse Hill-Sachs lesion)
- Significant fractures:
- Lesser tuberosity
- Posterior glenoid rim
- Recurrent instability
- Open dislocation
Surgical Options
- Modified McLaughlin procedure (20%–40% defect)
- Hemiarthroplasty (>40% defect)
- Open reduction and stabilization
- Tendon transfers:
- Subscapularis
- Biceps (Boyd-Sisk procedure)
- Capsulorrhaphy or osteotomies
Special Case
- Voluntary dislocators:
- Managed nonoperatively with rehabilitation and counseling
Complications
Fractures
- Posterior glenoid rim
- Humeral head
- Tuberosities
- Humeral shaft
Recurrent Instability
- More common in:
- Atraumatic cases
- Large humeral head defects
- Glenoid fractures
Neurovascular Injury
- Less frequent than anterior dislocation
- Possible injuries:
Iatrogenic Anterior Subluxation
- Caused by overtightening posterior structures
- Leads to:
- Limited flexion
- Restricted internal rotation
Key Clinical Pearls
- Always suspect posterior shoulder dislocation in:
- Seizure patients
- Electrical injuries
- Do not rely on AP X-ray alone
- Loss of external rotation is a critical clinical clue
- Early diagnosis prevents chronic instability and joint damage
References & More
- Kammel KR, El Bitar Y, Leber EH. Posterior Shoulder Dislocations. [Updated 2022 Sep 12]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: Pubmed
- Egol KA. Handbook of fractures. 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2019.