There are several Shoulder Reduction Techniques for the anterior glenohumeral dislocations. All have relatively high success rates but should be considered based on the availability of analgesia/sedation, the presence of assistants and the ease and time of performing the procedure.
The shoulder is the most commonly dislocated joint in the body accounting for 50 percent of major joint dislocations seen in the acute setting. Anterior dislocations are by far the most common, however posterior, inferior and multidirectional dislocations are possible.
The diagnosis of acute dislocation of the shoulder can be made on the basis of history and physical examination but is often confirmed radiographically, which allows for reliable assessment of direction. Before attempting shoulder reduction, it is important to carefully examine the injured shoulder.
The axillary nerve and vascular bundle may be injured either as a result of the initial trauma, or as a complication of the reduction technique.
It is also important to obtain high quality radiographs before and after shoulder reduction. An anteroposterior (AP), Scapular Y and axillary lateral radiographs are needed to confirm the presence and direction of the glenohumeral joint.
See Also: Shoulder Apprehension Test
Shoulder Reduction in Anterior Dislocation
For primary anterior shoulder dislocation, prompt reduction will provide the patient with a great deal of pain relief. Closed shoulder reduction may be done with or without anesthesia. Reduction without any anesthesia works best for recurrent or very recent dislocations with limited rotator cuff spasm. Intra-articular lidocaine injection has been shown to be as effective as procedural sedation for the shoulder reduction while limiting potential drug complications and time spent before discharge.
The shoulder reduction techniques in anterior dislocation include:
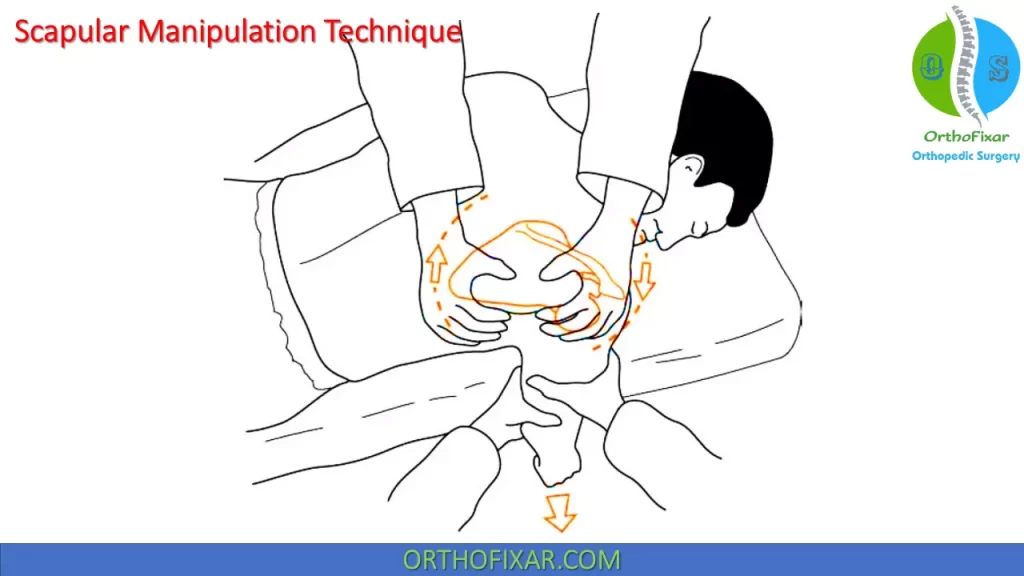
Scapular Manipulation Technique
In a prone position, the patient hangs the affected arm off the table with 5 to 10 pounds of weight suspended from a strap around the wrist.
The physician uses his or her hands to push the inferior tip of the scapula medially while moving the superior aspect laterally.
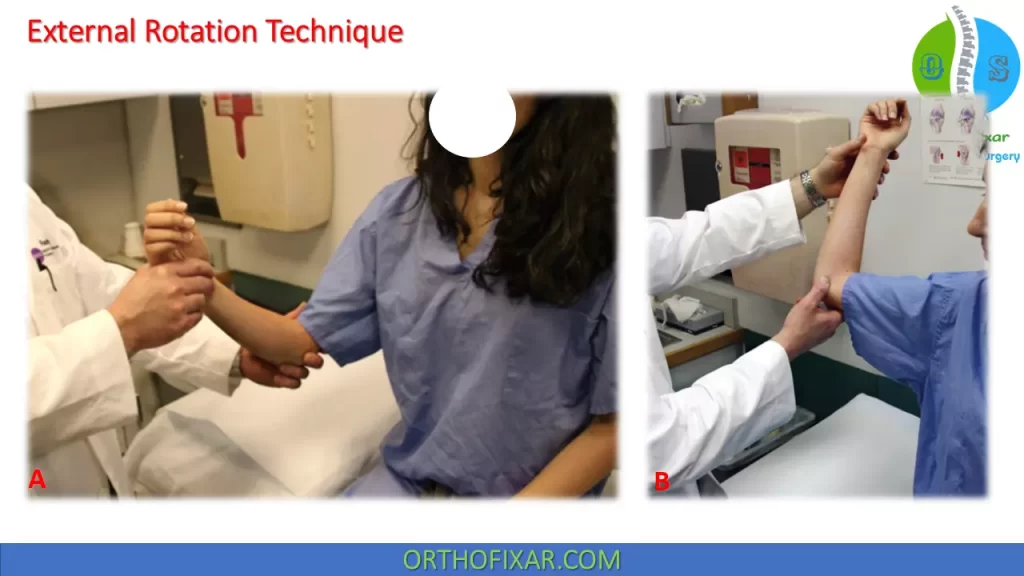
External Rotation Technique
This technique is often favored because it may be used to reduce dislocations successfully with little or no analgesia. The technique can be performed with the patient in supine position or seated upright.
If upright, the patient’s ipsilateral elbow should be supported to eliminate any traction. The elbow should be flexed to 90° and the arm is gently externally rotated. The physician should take care to rotate slowly and pause if the patient experiences pain, in order to allow for muscular relaxation. If the shoulder has not reduced spontaneously by 90° of external rotation, the arm is slowly abducted and the humeral head may be lifted into place.
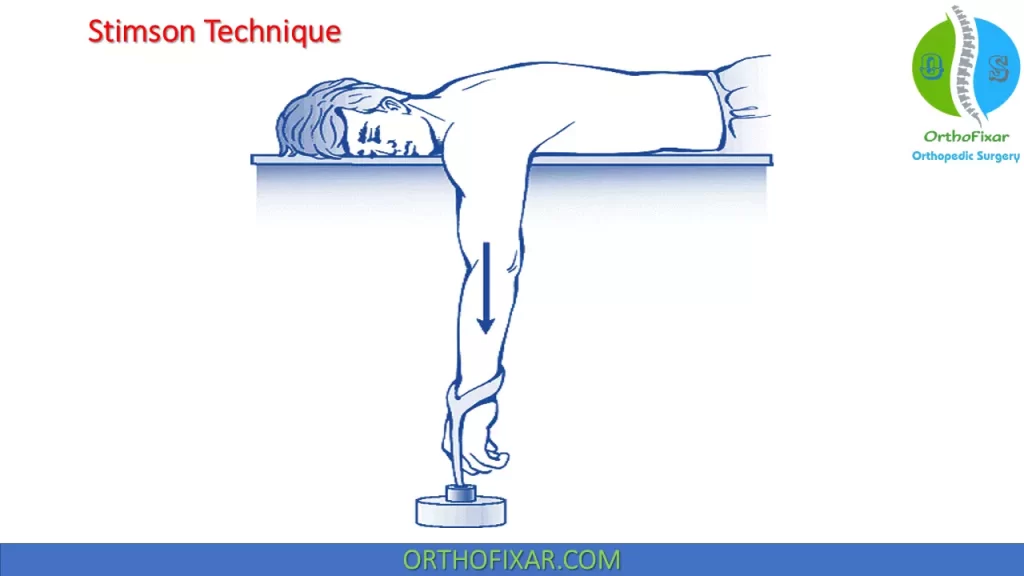
Stimson Technique
This method relies on complete muscle relaxation to be successful. The patient is positioned prone on the gurney or examination table. The injured arm is positioned hanging over the side with 10 to 15 pounds suspended in a similar manner as described above. Shoulder reduction should occur within 20 to 30 minutes.
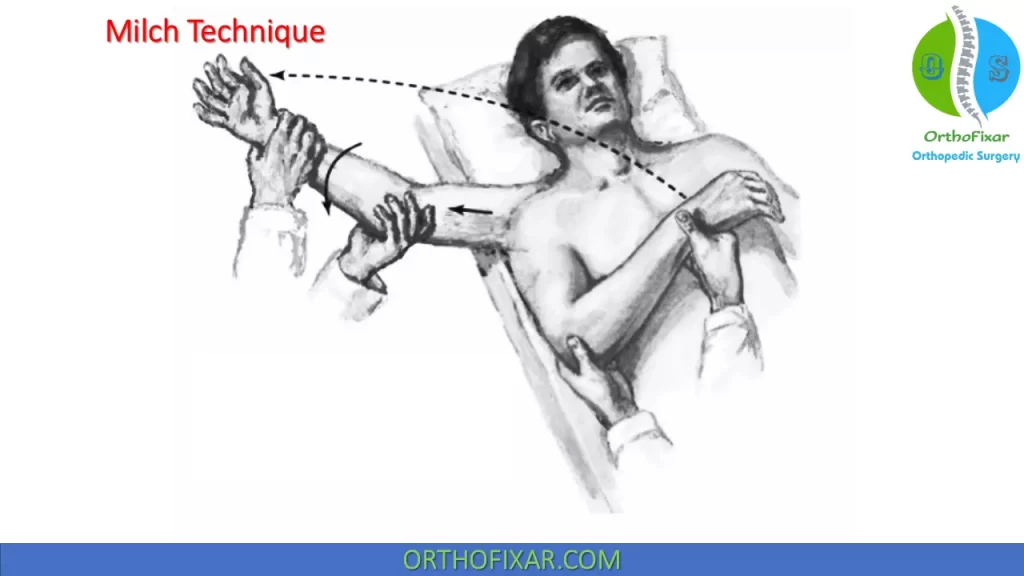
Milch Technique
With the patient supine, the physician externally rotates and abducts the patient’s arm. When the arm reaches the overhead position, the elbow is extended. The physician applies gentle traction. The physician’s free hand may be used to manipulate the humeral head over the glenoid labrum.
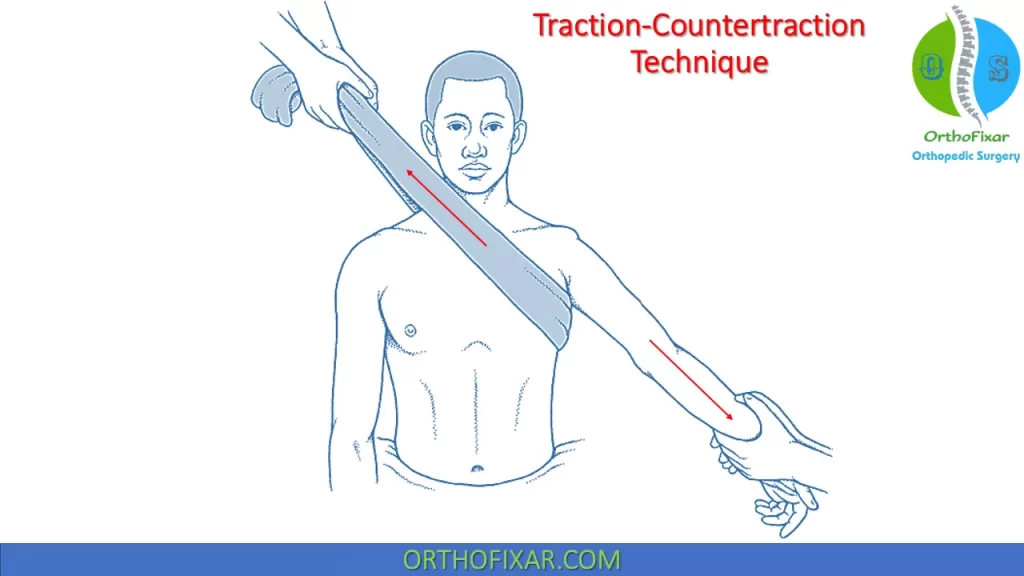
Traction-Countertraction Technique
The patient should be positioned supine, with a sheet tied around the thorax, positioned at the level of the axilla. Using the sheet, an assistant provides countertraction while the physician applies traction to the patient’s forearm at an angle of 30° of abduction and forward flexion of 20 to 30°.
The traction should be gentle and may require a constant application for up to 5 minutes. Sudden forceful movements should be avoided as they may cause additional neurovascular, soft tissue or bony injury to the patient.
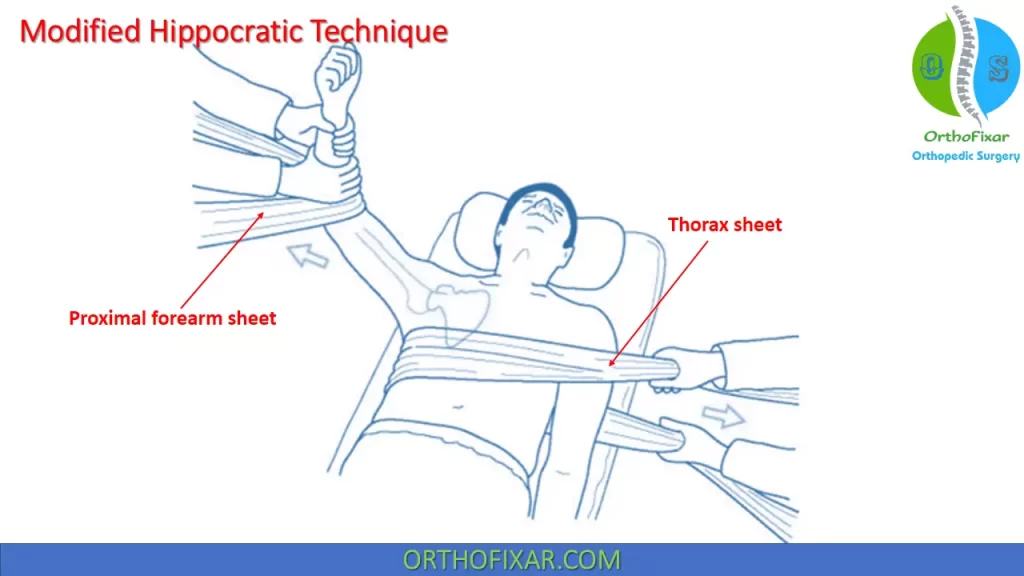
Modified Hippocratic Technique
The patient should be placed in a supine position with the elbow flexed to 90° and the arm abducted. A sheet is tied and placed around the patient’s thorax and an assistant’s waist. A second sheet is placed around the patient’s proximal forearm and the physician’s waist.
The physician applies traction to the patient’s arm, while countertraction is provided by the assistant. Shoulder reduction with modified Hippocratic technique may require gentle internal and external rotation or manipulation of the proximal humerus.
Reduction under Anesthesia
If the above shoulder reduction techniques are not successful, reduction under anesthesia may be necessary. This technique may also be required in the setting of significant fracture. Anesthesia allows for complete muscle relaxation and reduction often occurs easily with little risk of additional injury.
Posterior Shoulder Dislocation
Posterior Shoulder dislocations are much less common, accounting for approximately 1 to 2 percent of all glenohumeral dislocations. They are often associated with a history of direct trauma to the anterior shoulder, the strong muscular contractions of epileptic seizures/electric shock, or falls on an outstretched arm.
They can be more difficult to detect on physical examination than anterior dislocations, making confirmation with a scapular “Y” radiograph very important.
Associated bony lesions include:
- Fractures to the posterior glenoid,
- Reversed hill-Sachs deformity,
- Humeral shaft and lesser tuberosity.
Often, posterior dislocations are accompanied by a high degree of pain and muscular spasm, making analgesia and muscle relaxation extremely important.
Posterior shoulder dislocation reduction technique is applied with the help of an assistant. The patient is positioned supine. The physician applies traction to the humerus with the arm abducted. The assistant gently manipulates the humeral head into the glenoid anteriorly.
Inferior Shoulder Dislocation
Inferior shoulder dislocations, also known as luxatio erecta, are extremely rare. Severe soft tissue trauma and fracture usually accompany inferior dislocation due to the mechanism of injury.
A history will usually reveal that the arm was hyperabducted, where the neck of the humerus is forced against the acromion. The acromion acts as a fulcrum, which forces the humeral head down, tearing the inferior capsule.
Physical examination of luxatio erecta is characteristic, with the arm fully abducted. Usually the patient’s hand will be resting on or behind his or her head. The humeral head will be easily palpable on the lateral chest.
In this type, shoulder reduction is achieved with an assistant through the use of traction and countertraction. The physician applies traction in line with the humerus and the assistant applies countertraction. A noticeable “clunk” demonstrates the reduction.
Two-Step Approach
A two-step technique for Inferior shoulder dislocation reduction may also be used whereby the luxatio erecta dislocation is converted by the physician to an anterior dislocation after which any of the preferred techniques described above may be used to complete the shoulder reduction.
The patient must be placed in a supine position. Sedation may be administered as needed. The physician should stand next to the patient’s head on the ipsilateral side to the injury. Facing towards the patient’s feet, the physician should place the adjacent hand (superior) on the midshaft of the humerus, while the opposite hand (inferior) is positioned over the medial epicondyle.
The inferior hand provides gentle superior force at the distal humerus while the physician uses the superior hand to manipulate the humeral head to the anterior rim of the glenoid from its inferior position. A straight contour of the shoulder and prominence of the posterolateral edge of the acromion demonstrates that the humeral head is now dislocated in an anterior orientation.
The physician should be able to adduct the humerus at this point. At this point, the physician may use whichever anterior dislocation reduction technique that is most comfortable.
Post Reduction Care
Shoulder immobilization should be recommended for a short period of time following subluxations and dislocations as needed for pain.
For primary dislocations, an early range of motion and rotator cuff strengthening program should be recommended; however extreme external rotation or forward flexion should be avoided.
A decrease in apprehension to external rotation and abduction is often a good indicator that the patient may return to normal activities if strength has also improved.
Patients younger than 20 years of age are very likely to develop recurrent dislocations due to soft tissue injuries associated with their first dislocation episode. Incidence of recurrent instability is often seen as indirectly proportional to age.
Early arthroscopic Bankart repair for primary anterior dislocations has been suggested with positive results in the young, active patient population with patients having fewer recurrences of instability.
References
- Paterson WH, Throckmorton TW, Koester M, Azar FM, Kuhn JE. Position and duration of immobilization after primary anterior shoulder dislocation: a systematic review and meta-analysis of the literature. J Bone Joint Surg Am. 2010 Dec 15;92(18):2924-33. doi: 10.2106/JBJS.J.00631. PMID: 21159993.
- Acute Anterior Dislocations: Evaluation and Treatment. Arciero R. Chapter 10. In The Unstable Shoulder. Warren, Craig, Altchek ed. 1999. Lippincott-Raven. Philadelphia, PA.
- Management of acute glenohumeral dislocations. Sileo MJ, Joseph S, Nelson CO, Botts JD, Penna J. Am J Orthop (Belle Mead NJ). 2009 Jun;38(6):282-90.
- Wang SI. Management of the First-time Traumatic Anterior Shoulder Dislocation. Clin Shoulder Elb. 2018 Sep 1;21(3):169-175. doi: 10.5397/cise.2018.21.3.169. PMID: 33330172; PMCID: PMC7726393.
- Riebel GD, McCabe JB. Anterior shoulder dislocation: a review of reduction techniques. Am J Emerg Med. 1991 Mar;9(2):180-8. doi: 10.1016/0735-6757(91)90187-o. PMID: 1994950.
- Posterior shoulder dislocations and fracture-dislocations. Robinson CM, Aderinto J. J Bone Joint Surg Am. 2005 Mar;87(3):639-50.
- The two-step maneuver for closed reduction of inferior glenohumeral dislocation (luxatio erecta to anterior dislocation to reduction). Nho SJ, Dodson CC, Bardzik KF, Brophy Rh, Domb BG, MacGillivray JD. J Orthop Trauma. 2006 May;20(5):354-7.