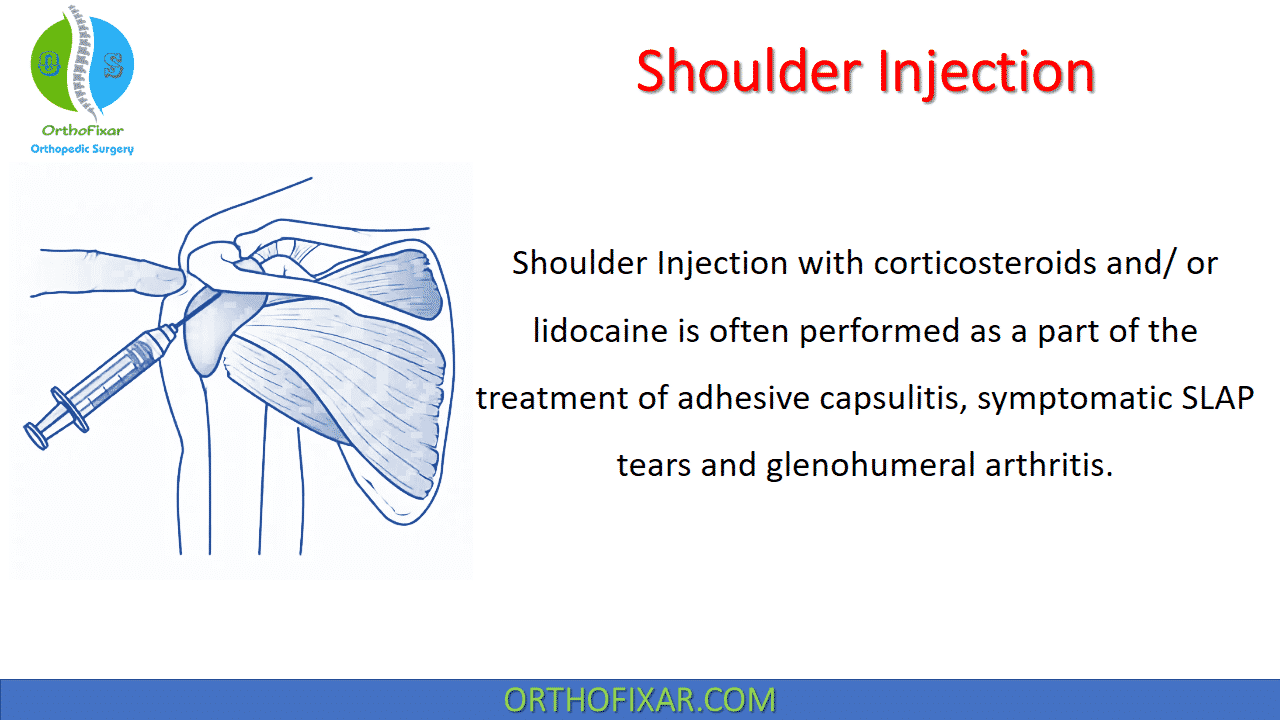
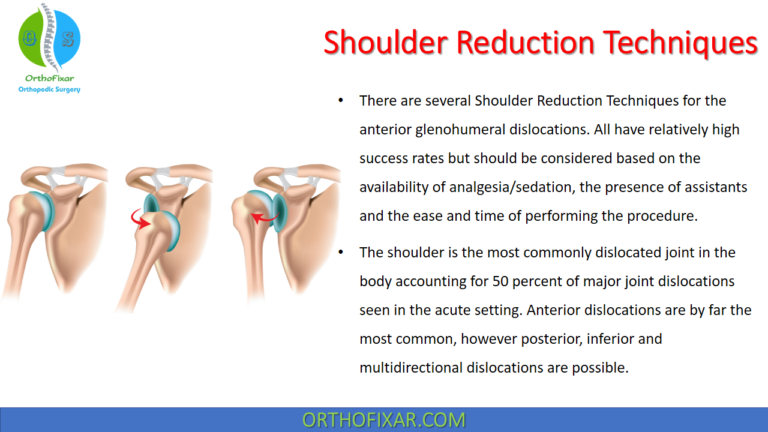
Shoulder Injection with corticosteroids and/or lidocaine is often performed as a part of the treatment of adhesive capsulitis, symptomatic SLAP tears and glenohumeral arthritis.
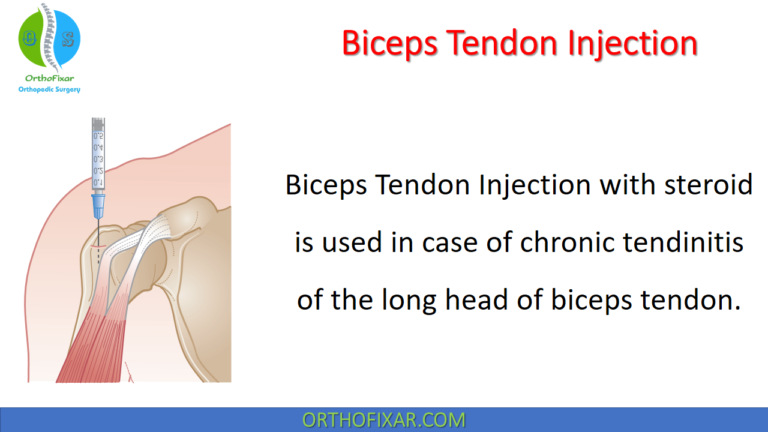
Patients with symptoms and functional limitations secondary to rotator cuff tendinopathy, long head of the biceps tendonitis and subdeltoid bursitis unresponsive to oral anti-inflammatory medications and physical therapy are often indicated for subacromial injections.
A number of approaches to the aspiration and injection of the shoulder have been described, with the anterior and posterior approaches most commonly used.
See Also: Shoulder Range of Motion
Absolute and Relative Contraindications to Joint Injection
Absolute Contraindications:
- Local cellulitis.
- Septic arthritis (shoulder aspiration for diagnosis is indicated).
- Acute fracture.
- Bacteremia.
- Joint prosthesis.
- History of allergy or anaphylaxis to injectable pharmaceuticals or constituents.
Relative Contraindications
- Minimal relief after two previous corticosteroid injections.
- Underlying coagulopathy.
- Anticoagulation therapy.
- Evidence of surrounding joint osteoporosis.
- Anatomically inaccessible joints.
- Uncontrolled diabetes mellitus.
See Also: Shoulder SLAP Lesion
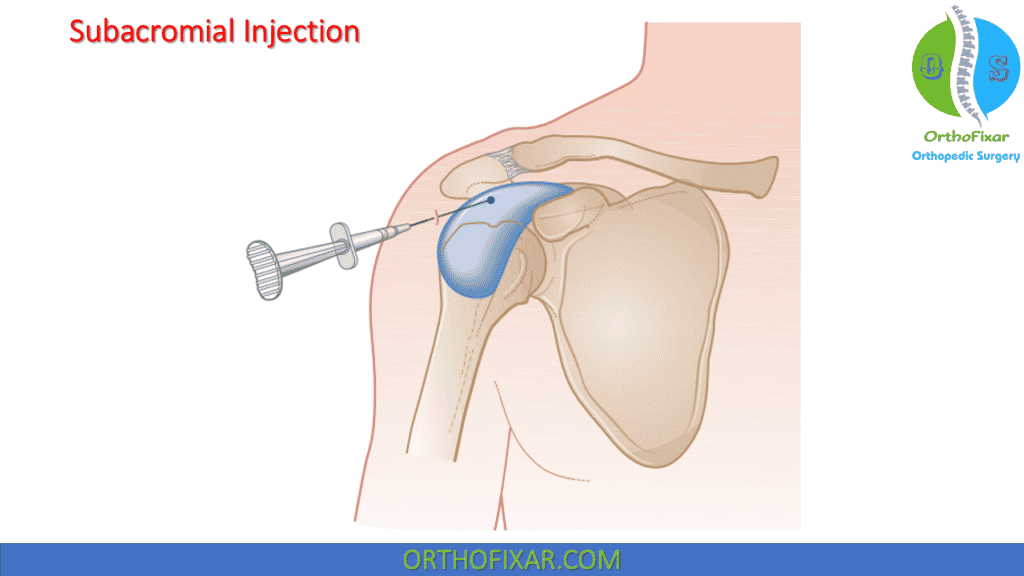
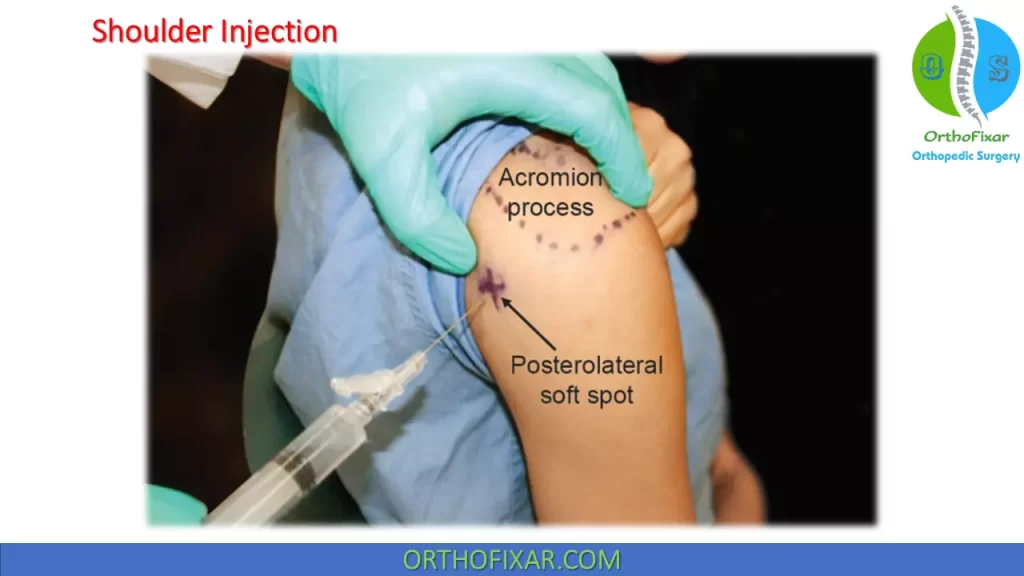
Posterior Approach
Patient is placed in the seated position with their affected upper extremity resting comfortably at their side on the chair’s arm rest with the shoulder in an internally rotated position.
Examine the posterolateral aspect of the shoulder looking for evidence of overlying cellulitis (avoid placing the needle through any area of potential infection).
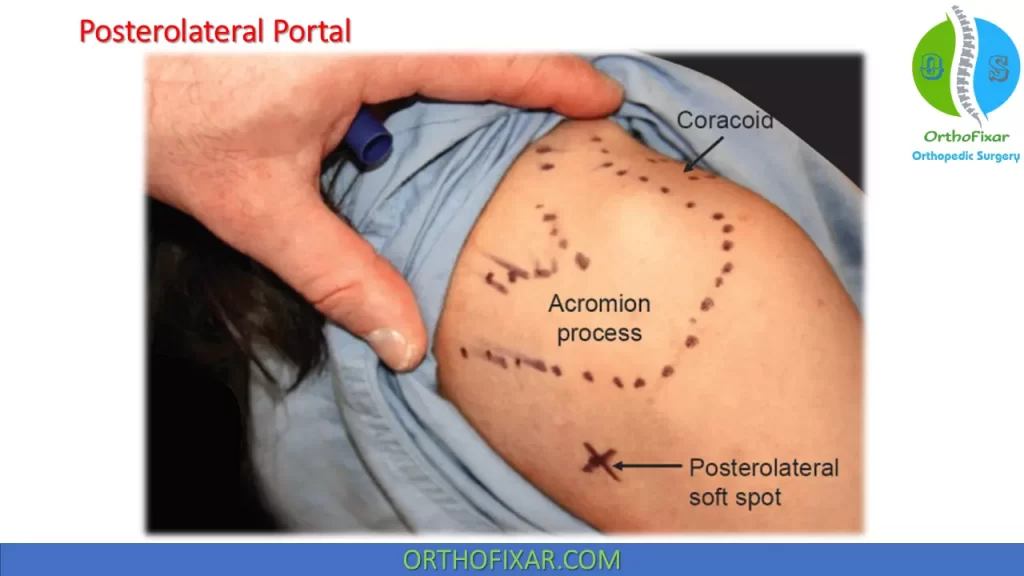
Palpate the posterior and lateral borders of the acromion process localizing its most posterolateral aspect and palpate the coracoid process anteriorly.
Localize the posterolateral soft spot between the humeral head and the glenoid approximately two fingerbreadths distal and one fingerbreadth medial to the posterolateral corner of the acromion (The location of the humeral head relative to the glenoid can be appreciated with rotation of the upper arm). Mark this site as the starting point for the aspiration/injection. The same starting point has been used for both glenohumeral injection and subacromial injection.
Prep the skin in this region using alcohol and povidone-iodine.
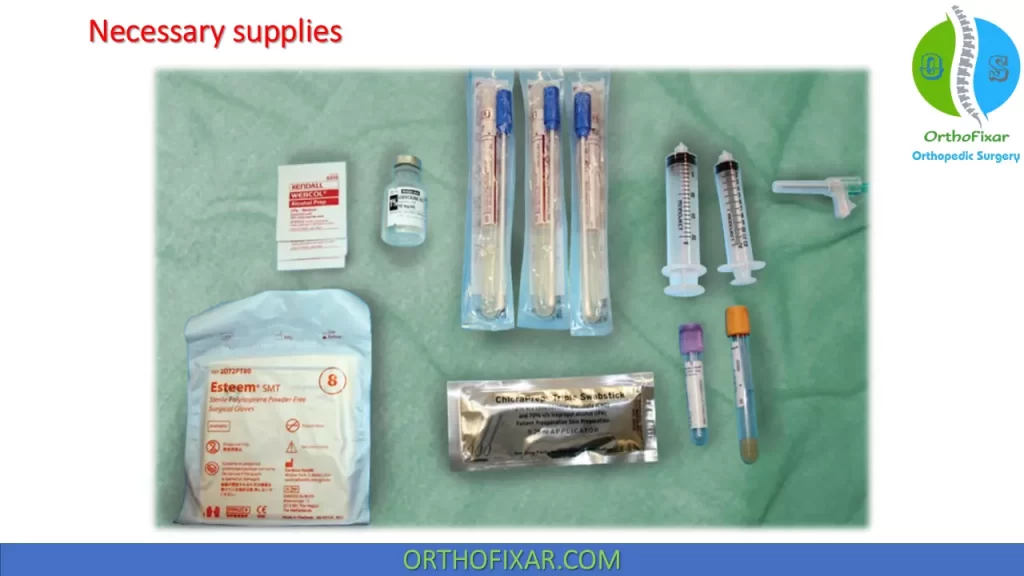
For shoulder aspiration:
- use a 18-20-gauge needle attached to the appropriately sized syringe (typically a 10–20 cc syringe will be used).
- If available, an assistant can spray the area with ethyl chloride spray to provide superficial analgesia just prior to needle insertion.
- The needle should be directed anteriorly toward the coracoid process advancing slowly aiming slightly medial. Any contact with underlying bone of the humeral head should prompt a careful retraction and redirection of the needle more medially and slightly more superiorly.
- Once the needle is injected in the intra-articular space, start aspirating.
- If necessary, additional syringes can be used for aspiration by disconnecting the luer lock from the needle. One can use a hemostat to stabilize the needle taking care to avoid changing its intra-articular position.
- Once the aspiration is complete, a new sterile needle can be attached to the syringe allowing for distribution of the obtained fluid into culture tubes and blood tubes for later analysis (assistant can be helpful during this step to ensure maintenance of sterility).
For shoulder / subacromial injection:
- The same approach can be used injecting the prepared medication once the needle is within the intra-articular space.
- When injecting medication into the subacromial space, the same starting point is used with the needle aimed superiorly at a 10 to 15° angle to end up just distal to the undersurface of the acromion process.
- Once in the subacromial space, aspirate first to ensure that the tip of the needle is not intravascular followed by the prepared lidocaine/ steroid injection shoulder.
- Following the aspiration and/or injection the needle is removed from the shoulder. The prepped skin is cleaned with an alcohol swab, dried with a gauze pad and a band-aid is applied.
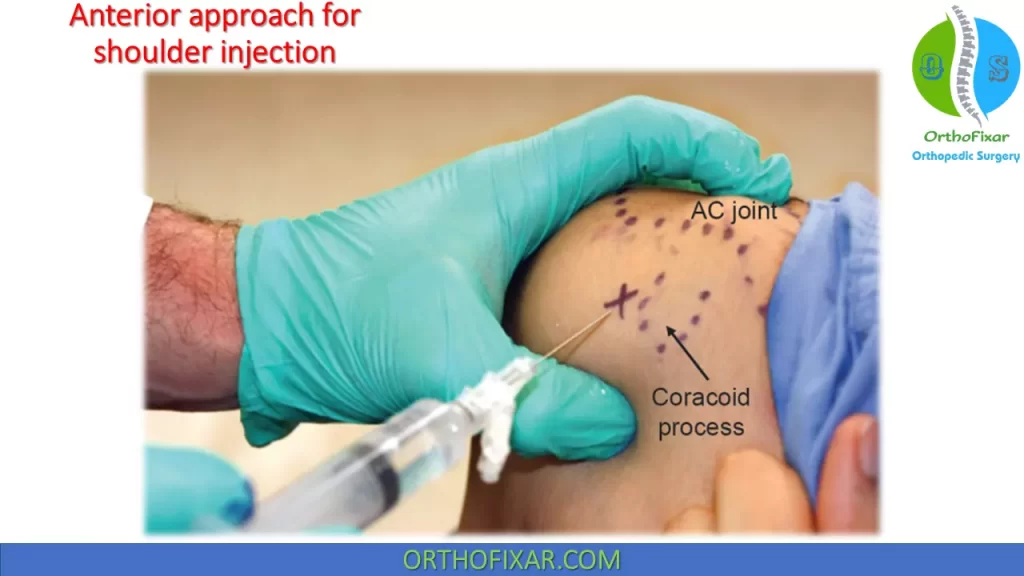
Anterior Approach
Patient is placed in the seated position with their affected upper extremity resting comfortably at their side on the chair’s arm rest with the shoulder in a neutral or slightly externally rotated (approximately 15 to 20°) position.
Examine the anterior aspect of the shoulder looking for evidence of overlying cellulitis (avoid placing the needle through any area of potential infection).
Palpate the coracoid process and the humeral head (rotation of the upper extremity can help localize the humeral head relative to the glenoid).
Mark the starting point for the aspiration/injection just medial to the humeral head, 5 to 10 mm lateral to the tip of the coracoid process.
Prepare the skin in this region using alcohol and povidone-iodine.
For shoulder aspiration:
- use a 20- or 21-gauge needle attached to the appropriately sized syringe (typically a 10–20 cc syringe will be used).
- If available, an assistant can spray the area with ethyl chloride spray to provide superficial analgesia just prior to needle insertion.
- The needle should be directed posteriorly aiming slightly lateral and slightly superior in an effort to penetrate the joint in the region of the rotator interval. Any contact with underlying bone of the humeral head should prompt a careful retraction and redirection of the needle more medially and slightly more superiorly, contact with the bone of the glenoid should prompt redirection further laterally.
- Once in the intra-articular space, start aspirating.
- If necessary, additional syringes can be used for aspiration by disconnecting the luer lock from the needle. One can use a hemostat to stabilize the needle taking care to avoid changing its intra-articular position.
- Once the aspiration is complete, a new sterile needle can be attached to the syringe allowing for distribution of the obtained fluid into culture tubes and blood tubes for later analysis (assistant can be helpful during this step to ensure maintenance of sterility).
For shoulder injections:
- the same approach can be used injecting the prepared medication once the needle is within the intra-articular space.
- When injecting medication into the subacromial space, the same starting point is used with the needle aimed superiorly at a 10 to 15° angle to end up just distal to the undersurface of the acromion process.
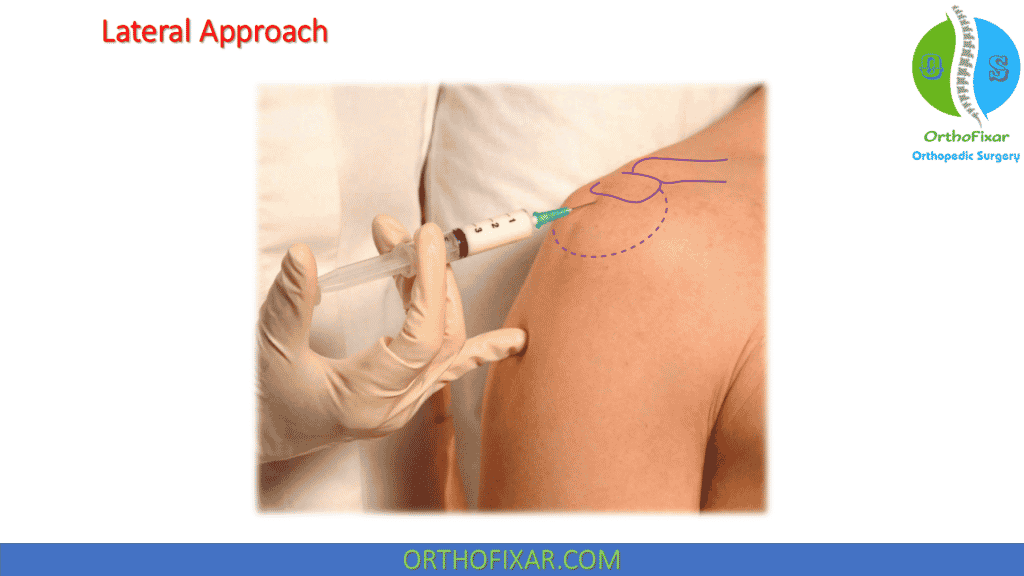
Lateral Approach
Patient sits with arm hanging to distract humerus from acromion, identify lateral edge of acromion. Insert needle at midpoint of acromion and angle slightly upwards under acromion to its full length and lowly withdraw needle while simultaneously injecting as a bolus wherever there is no resistance.
References
- Cardone DA, Tallia AF. Joint and soft tissue injection. Am Fam Physician. 2002 Jul 15;66(2):283-8. PMID: 12152964.
- Courtney P, Doherty M. Joint aspiration and injection and synovial fluid analysis. Best Pract Res Clin Rheumatol. 2009 Apr;23(2):161-92. doi: 10.1016/j.berh.2009.01.003. PMID: 19393565.
- Rifat SF, Moeller JL. Injection and aspiration techniques for the primary care physician. Compr Ther. 2002 Winter;28(4):222-9. Review.
- Emergency Room Orthopaedic Procedures: An Illustrative Guide for the House Officer Book by Eric J. Strauss and Kenneth A. Egol.