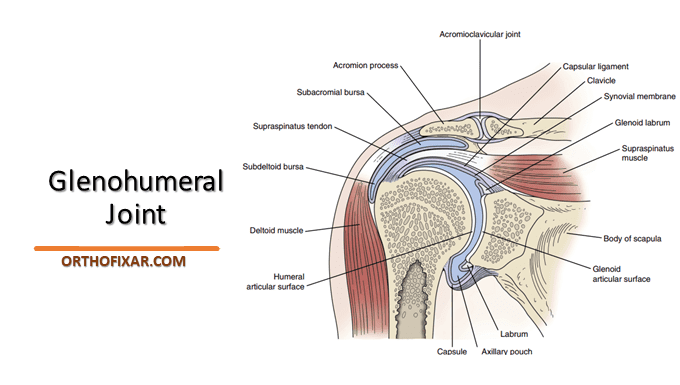
The Glenohumeral Joint is formed by the head of the humerus and the scapula’s glenoid fossa, it’s a multiaxial ball-and-socket synovial joint that depends primarily on the muscles and ligaments rather than bones for its support, stability, and integrity.
The Glenohumeral Joint is capable of three degrees of freedom of motion:
- Flexion and extension,
- Abduction and adduction,
- Internal and external rotation.
Although not true anatomical motions horizontal adduction and abduction (or horizontal flexion and extension) and circumduction also occur at the GH joint. Most upper extremity motions do not occur in a single isolated plane but, rather, are a combination of movements in two or more planes.
See Also: Normal Shoulder Range of Motion
Glenohumeral Bone Anatomy
The head of the humerus faces medially, posteriorly, and superiorly with the axis of the head forming an angle of 130– 150 degrees with the long axis of the humerus and the humeral head is retroverted 25° to 30° in adults (from about 75° in babies) relative to the line joining the epicondyles. In the frontal plane, the head of the humerus is angled posteriorly (retroverted) by 30–40 degrees. The joint capsule of the Glenohumeral Joint is lax inferiorly to permit full elevation of the arm.
The glenoid fossa of the scapula faces laterally, superiorly, and anteriorly at rest and inferiorly and posteriorly when the arm is in the dependent position. The glenoid fossa is flat and covers only one-third to one-fourth of the surface area of the humeral head. This arrangement allows for a great deal of mobility but little in the way of articular stability.
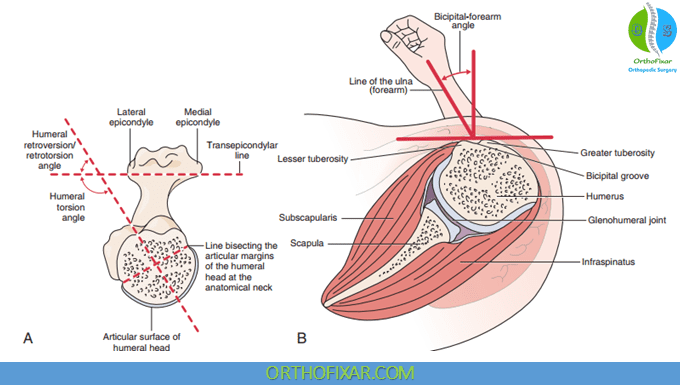
The greater and lesser tuberosities, which serve as attachment sites for the tendons of the rotator cuff muscles, are located on the lateral aspect of the anatomical neck of the humerus, an imaginary line that separates the humeral head from the rest of the humerus.
The lesser tuberosity serves as the attachment for the subscapularis. The greater tuberosity serves as the attachment for the supraspinatus, infraspinatus, and teres minor.
The greater and lesser tuberosities are separated by the intertubercular groove, through which passes the tendon of the LHB on its route to attach to the superior rim of the glenoid fossa. This groove has wide variance in the angle of its walls, but 70% fall within a 60–75-degree range. The roof of this groove is formed by the transverse ligament.
The transverse humeral ligament , which runs perpendicular over the biceps tendon, was once thought to function as a restraint to the biceps tendon within the intertubercular groove. However, this appears to be the role of the coracohumeral ligament. The region below the greater and lesser tuberosities, where the upper margin of the humerus joins the shaft of the humerus, is referred to as the surgical neck. The axillary nerve and posterior humeral circumflex artery lie in close proximity to the medial aspect of the surgical neck.
See Also: Clavicle Anatomy

GH Joint Capsule
The lateral attachment of the voluminous joint capsule of the GH joint attaches to the anatomical neck of the humerus . Medially, the capsule is attached to the periphery of the glenoid and its labrum. The overall strength of the joint capsule bears an inverse relationship with the patient’s age; the older the patient, the weaker the joint capsule. The fibrous portion of the capsule is very lax and has several recesses, depending on the position of the arm.
At its inferior aspect, the capsule forms an axillary recess, which is both loose and redundant. The recess permits normal elevation of the arm, although it can also be the site of adhesions when the shoulder is immobilized in adduction. The anterior aspect of the joint capsule is reinforced by three ligaments (Z ligaments). The tendons of the rotator cuff (supraspinatus, infraspinatus, teres minor, and subscapularis) reinforce the superior, posterior, and anterior aspects of the capsule, as does the LHB tendon.
An inner synovial membrane lines the fibrous capsule and secretes synovial fluid into the joint cavity. The synovium typically lines the joint capsule and extends from the glenoid labrum down to the neck of the humerus. It also forms variously sized bursae, the largest of which, the subacromial or subdeltoid bursa, lies on the superior aspect of the joint.
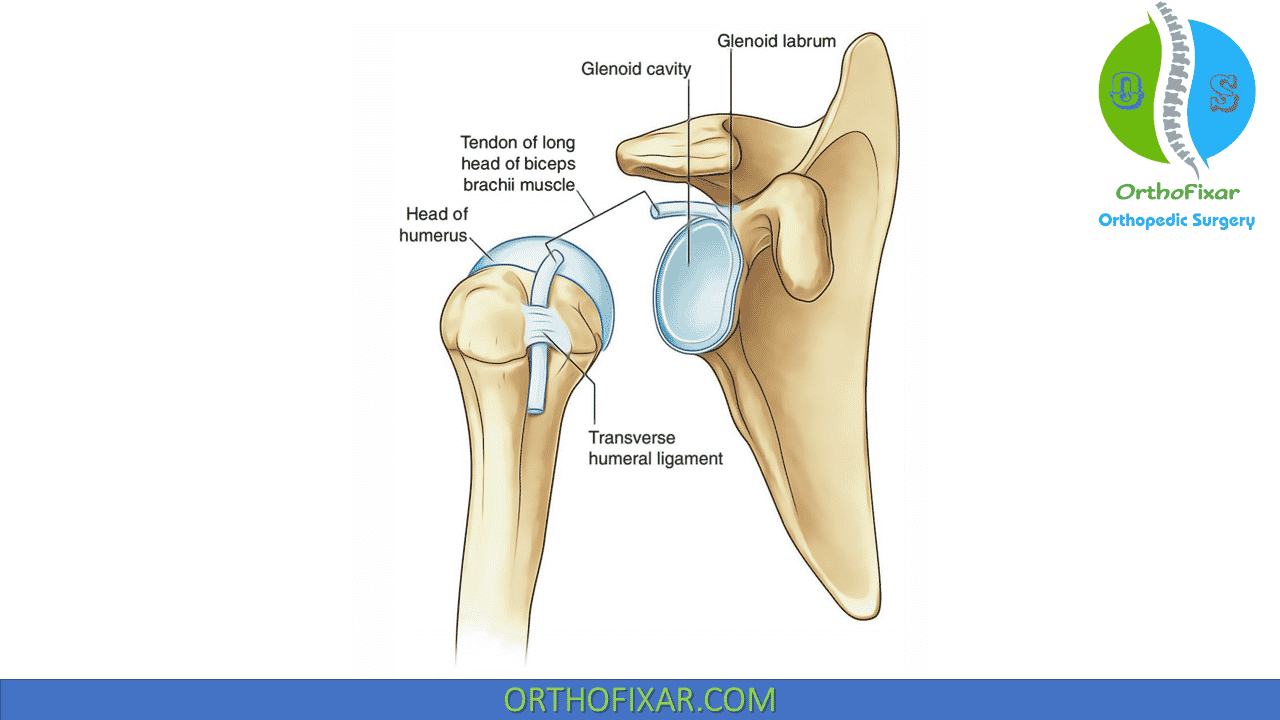
Glenoid Labrum Anatomy
However, the glenoid fossa is made approximately 30% to 50% deeper (doubling the depth of the glenoid fossa across its equatorial line) and more concave by a ring of fibrous cartilage and dense fibrous collagen called a labrum.
The labrum forms a part of the articular surface and is attached to the margin of the glenoid cavity and the joint capsule. It is also attached to the lateral portion of the biceps anchor superiorly. In addition, approximately 50% of the fibers of the long head of the biceps brachii originate from the superior labrum (the remainder originates from the superior glenoid tubercle), with four different variations identified, and continue posteriorly to become a periarticular fiber bundle, making up the bulk of the labrum.
The labrum enhances joint stability by increasing the humeral head contact areas to 75% vertically and 56% transversely.
The humeral–glenoid contact area provides two primary functions:
- It spreads the joint loading over a broad area,
- It permits movement of opposing joint surfaces with minimal friction and wear.
In conclusion, the labrum functions as a:
- Chock block,
- Increases the depth of the glenoid,
- Resists translation,
- Enables concavity compression (when the head of the humerus is compressed into the glenoid by the rotator cuff),
- Centralizes the humeral head in the glenoid,
- Helps to maintain a negative intraarticular pressure within the joint.
See Also: Shoulder SLAP Lesion
GH Stability
The GH joint is inherently unstable because of the relationship in the sizes of the articular surfaces of the glenoid fossa and the humeral head, a loose joint capsule, and relatively weak ligamentous support. The pear-shaped articulating surface of the glenoid fossa is significantly smaller than that of the humeral head and only vaguely resembles the ball-and-socket joint of the hip.
Possessing a volume twice the size of the humeral head, the glenohumeral joint capsule arises from the glenoid fossa and glenoid labrum to blend with the muscles of the rotator cuff. Studies on cadavers indicate that the laxity of the capsular arrangement allows the humeral head to be distracted 2 cm or more from the glenoid fossa.
Additional support is provided by both dynamic and static mechanisms. The dynamic mechanisms include the muscles of the rotator cuff (supraspinatus, infraspinatus, teres minor, and subscapularis muscles) and a number of muscle force couples. The static mechanisms include reinforcements of the joint capsule, joint cohesion and geometry, and ligamentous support.
See Also: Rotator Cuff of the Shoulder
Glenohumeral Joint Ligaments
A number of structures function as static stabilizers during motion of the arm to reciprocally tighten and loosen, thereby limiting translation and rotation of the Glenohumeral Joint surfaces in a load-sharing fashion. These include the GH ligaments and the posterior capsule. Further static stabilization is provided by the glenoid labrum. The posterior capsule is under tension when the shoulder is in flexion, abduction, IR (in particular, the superior and middle segments), or in any combination of these.
At the anterior portion of the outer fibers of the joint capsule, three local reinforcements are present: the superior, middle, and inferior GH ligaments. Together with the coracohumeral ligament, these ligaments form a Z-pattern on the anterior aspect of the shoulder. In the midrange of rotation, the GH ligaments are relatively lax and stability is maintained primarily by the action of the rotator cuff muscle group compressing the humeral head into the conforming glenoid articulation.
The Glenohumeral Joint ligaments appear to produce a major restraint during shoulder flexion, extension, and rotation:
- The anterior GH ligament is under tension when the shoulder is in extension, abduction, and/or external rotation (ER).
- The posterior GH ligament is under tension in flexion and ER.
- The inferior GH ligament is the most important of the GH ligaments. It is under tension when the shoulder is abducted, extended, and/or externally rotated. In addition, this ligament is a primary restraint against both anterior and posterior dislocations of the humeral head, and is the most important stabilizing structure of the shoulder in the overhead athlete. At 0-degree abduction, the subscapularis muscle, the labrum, and the superior GH ligament are the primary restraints against anterior translation. At 45 degree abduction, the subscapularis muscle and the middle and inferior GH ligaments, along with labrum, prevent anterior translation. When the arm is abducted more than 90 degrees, which is the most common position of anterior dislocation, the anterior fibers of the inferior GH ligament are the primary restraint anterior movement.
- The middle GH ligament is under tension when the shoulder is flexed and externally rotated. In addition, the middle GH ligament and the subscapularis tendon limit ER from 45 to 75 degrees of abduction, and are important anterior stabilizers.
| Position of the Humerus | Ligamentous Structures Limiting Movement |
|---|---|
| External rotation in 0° abduction | Superior GH ligament Coracohumeral ligament |
| External rotation in 45° abduction | Middle GH ligament Anterior band of the inferior GH ligament |
| External rotation in 90° abduction | Inferior GH ligament |
| Internal rotation in 90° abduction | Posterior band of the inferior GH ligament |
| Inferior displacement in 0° abduction | Superior GH ligament Coracohumeral ligament |
| Inferior displacement in 90° abduction | Inferior GH ligament |

Other ligaments help provide stability to the GH joint. These include the following:
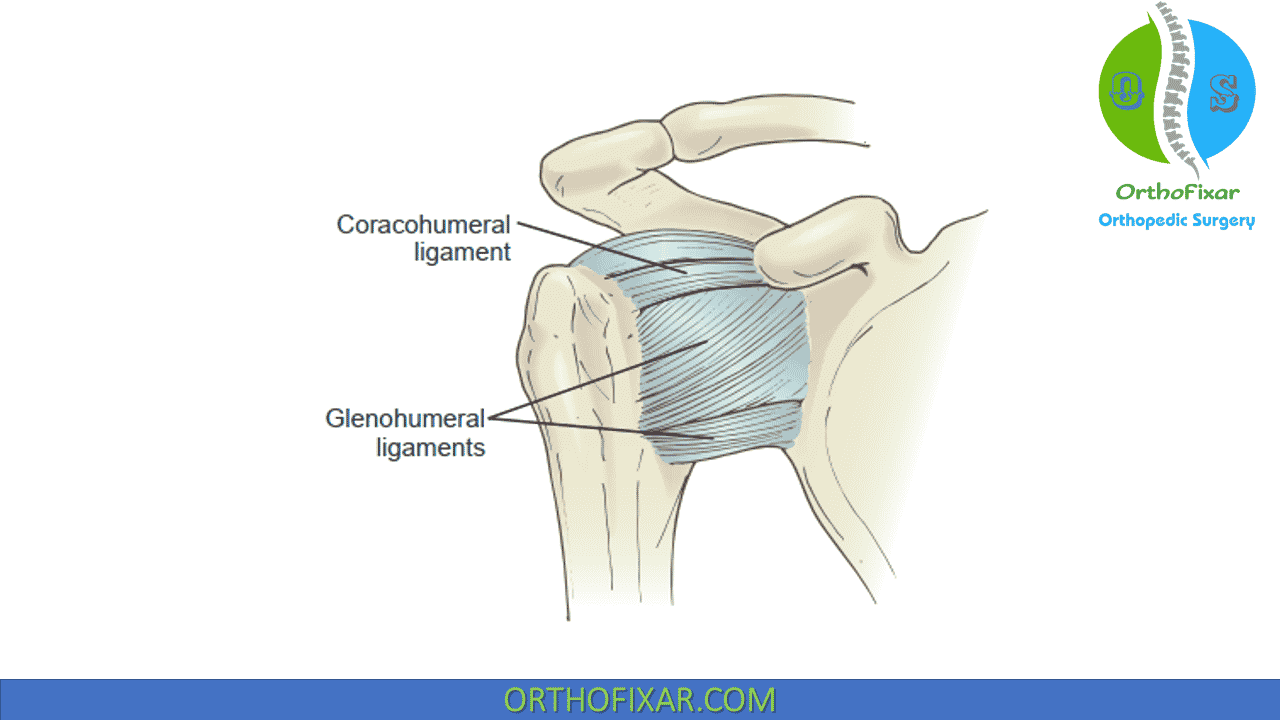
The coracohumeral ligament:
The coracohumeral ligament arises from the lateral end of the coracoid process and runs laterally, where it is split into two bands by the presence of the biceps tendon. The posterior band blends with the supraspinatus tendon to insert near the greater tuberosity, and the anterior band blends with the subscapularis tendon to insert near the lesser tuberosity.
The coracohumeral ligament covers the superior GH ligament anterosuperiorly and fills the space between the tendons of the supraspinatus and subscapularis muscles, uniting these tendons to complete the rotator cuff in this area. Tears of the cuff usually extend longitudinally between the supraspinatus and coracohumeral ligament so that the hood action of the cuff is lost. It is generally agreed that the posterior band of the coracohumeral ligament limits flexion, whereas the anterior band limits extension of the GH joint. Both the bands also limit inferior and posterior translation of the humeral head, strengthening the superoanterior aspect of the capsule.
The coracoacromial ligament:
The coracoacromial ligament is often described as the roof of the shoulder. It is a very thick structure that runs from the coracoid process to the anteroinferior aspect of the acromion, with some of its fibers extending to the A-C joint. The ligament consists of two bands that join near the acromion, and it is ideally suited, both anatomically and morphologically, to prevent separation of the AC joint surfaces. The coracoclavicular ligaments and the costoclavicular ligament are described in the AC joint section and the SC joint section, respectively.
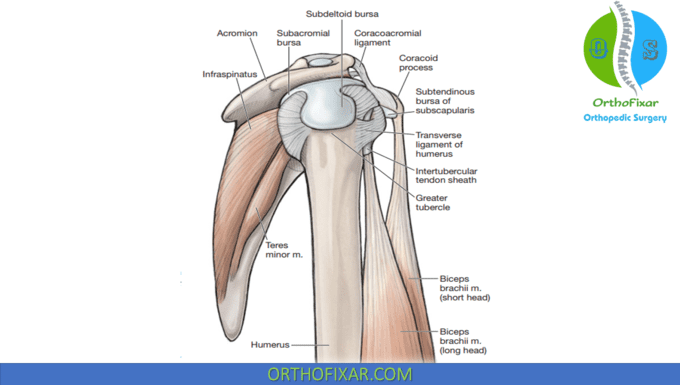
Coracoacromial Arch
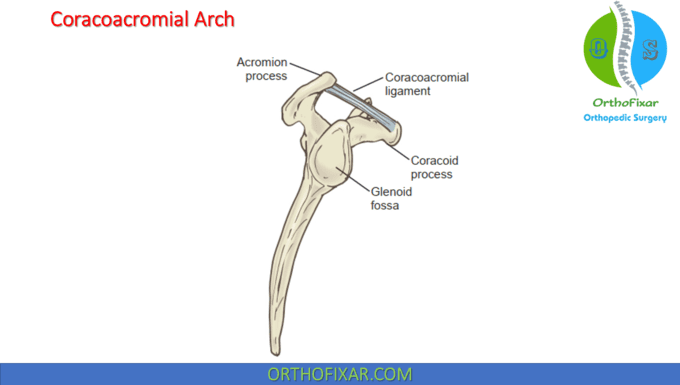
The coracoacromial arch is formed by the anteroinferior aspect of the acromion process, and the coracoacromial ligament, which connects the coracoid to the acromion and the inferior surface of the AC joint. A number of structures are located in the subacromial space between the coracoacromial arch superiorly and the humeral head inferiorly, and the coracoid process, anteromedially. These include (from inferior to superior) the following:
- the head of the humerus,
- the long head of biceps tendon (intra-articular portion),
- the superior aspect of the joint capsule,
- the supraspinatus and upper margins of subscapularis and infraspinatus,
- the subdeltoid–subacromial bursae, ” the inferior surface of coracoacromial arch.
References
- Kapandji IA: The Physiology of the Joints, Upper Limb. New York: Churchill Livingstone, 1991
- Perry J: Biomechanics of the shoulder. In: Rowe CR, ed. The Shoulder. New York: Churchill Livingstone, 1988:1–15. Pubmed
- Saha AK. Dynamic stability of the glenohumeral joint. Acta Orthop Scand. 1971;42(6):491-505. doi: 10.3109/17453677108989066. PMID: 5144199. Pubmed
- Perry J: Normal upper extremity kinesiology. Phys Ther 58:265–278, 1978.
- Bost F, Inman V: The pathological changes in recurrent dislocation of the shoulder. A report of Bankart’ s operative procedures. J Bone Joint Surg 24:595–613, 1942.
- Cooper DE, Arnoczky SP, O , Brien SJ, et al: Anatomy, histology, and vascularity of the glenoid labrum. An anatomical study. J Bone Joint Surg Am 74:46–52, 1992.
- Howell SM, Galinat BJ: The glenoid-labral socket: a constrained articular surface. Clin Orthop 243:122–125, 1989.
- Wilk KE, Reinold MM, Dugas JR, et al: Current concepts in the recognition and treatment of superior labral (SLAP) lesions. J Orthop Sports Phys Ther 35:273–291, 2005.
- Vangsness CT Jr, Jorgenson SS, Watson T, et al: The origin of the long head of the biceps from the scapula and glenoid labrum. An anatomical study of 100 shoulders. J Bone Joint Surg Br 76:951–954, 1994.
- Huber WP, Putz RV: Periarticular fiber system of the shoulder joint. Arthroscopy 13:680–691, 1997.
- Bradley JP, Tibone JE: Electromyographic analysis of muscle action about the shoulder. Clin Sports Med 4:789–805, 1991
- Gerber A, Warner JJ: Thermal capsulorrhaphy to treat shoulder instability. Clin Orthop Relat Res 400:105–116, 2002.
- Ferrari DA: Capsular ligaments of the shoulder. Am J Sports Med 18:20– 24, 1990.
- O , Brien SJ, Neves MC, Armoczky SP, et al: The anatomy and histology of the inferior glenohumeral complex of the shoulder. Am J Sports Med 18:449, 1990.
- Wilk KE, Arrigo C, Andrews JR: Current concepts in rehabilitation of the athlete , s shoulder. J South Orthop Assoc 3:216–231, 1994.
- Bowen MK, Warren RF: Ligamentous control of shoulder stability based on selective cutting and static translation experiments. Clin Sports Med 10:757–782, 1991.
- Turkel SJ, Panio MW, Marshall JL, et al: Stabilizing mechanisms preventing anterior dislocation of the glenohumeral joint. J Bone Joint Surg [Am] 63:1208–1217, 1981.
- Harryman DT III, Sidles JA, Harris SL, et al: The role of the rotator interval capsule in passive motion and stability of the shoulder. J Bone Joint Surg 74A:53–66, 1992.
- Matsen FA III, Arntz CT: Subacromial impingement. In: Rockwood CA Jr, Matsen FA III, eds. The Shoulder. Philadelphia, PA: WB Saunders, 1990:623–648.