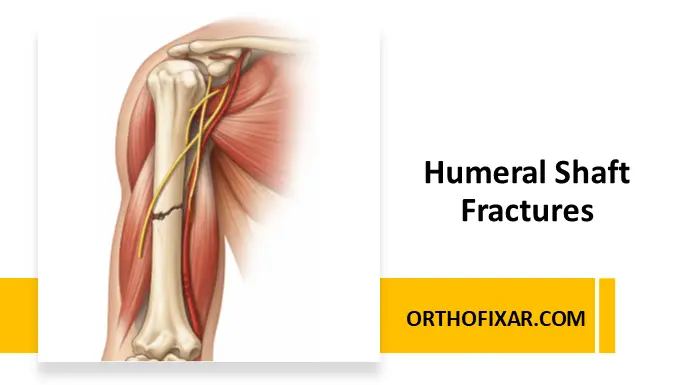
Humeral shaft fractures are relatively common injuries (account for 3–5% of all fractures occurring in the human body). Most of them occur after direct blows, and by motor vehicle accident. Other causes that account for less than 10% of humeral shaft fractures include sporting activities, working accidents, fall from a height, violence, and bone pathology.
Up to the age of 60 years, diaphyseal humeral fractures occur equally in men and women and the incidence does not seem to increase with age. After the age of 60 years 80% are women and humeral shaft fractures become more frequent.
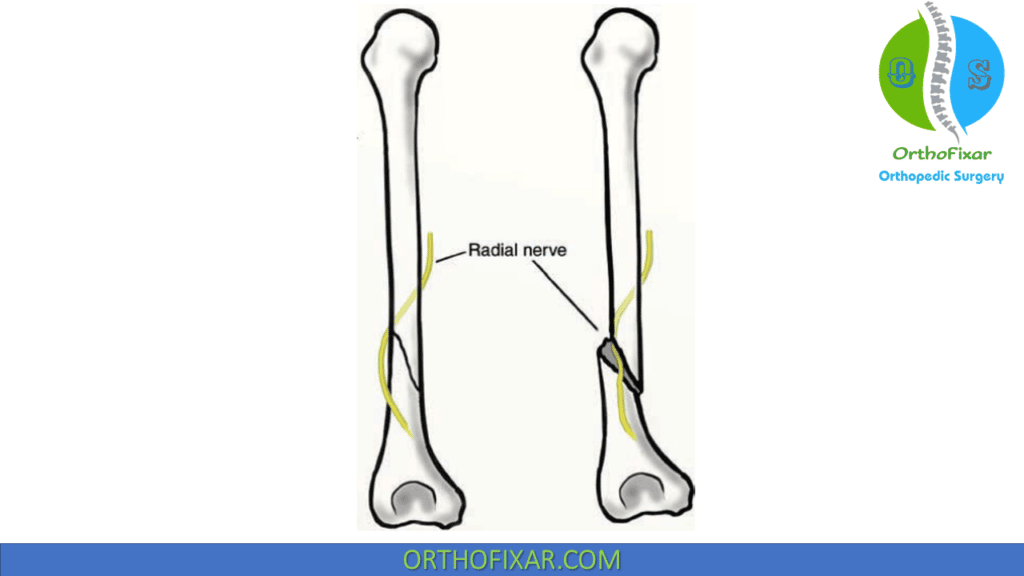
The radial nerve is prone to damage, either during the initial injury or during fracture reduction (10% to 12% of all closed humeral shaft fractures).
Related Anatomy
The humeral shaft extends from the insertion of pectoralis major to the supracondylar ridge.
The humeral shaft has a rich vascular supply, being densely covered with muscular attachments. The radial nerve along with the profunda brachii artery winds around the humeral shaft posteriorly in the spiral groove. At the region where it travels from the posterior to the anterior compartment, it is transfixed to the bone by the lateral intermuscular septum and is prone to injury by fractures in this region.
Depending on the level of fracture, the fracture fragments are displaced by the strong muscular attachments into different positions.
Mechanism of Injury
Direct trauma to the arm is the most common mode of injury and results in transverse or comminuted fractures. In elderly patients, indirect injury through a fall on an outstretched arm results in spiral or oblique fractures.
Clinical Evaluation
Patients with humeral shaft fractures typically present with pain, swelling, deformity and shortening of the affected arm.
A careful neurovascular examination is done with particular attention to radial nerve function and is documented.
Radiology Evaluation
Anteroposterior and lateral radiographs of the humerus, including the shoulder and elbow joints, are the only imaging studies usually required.
See Also: Proximal Humerus Fracture
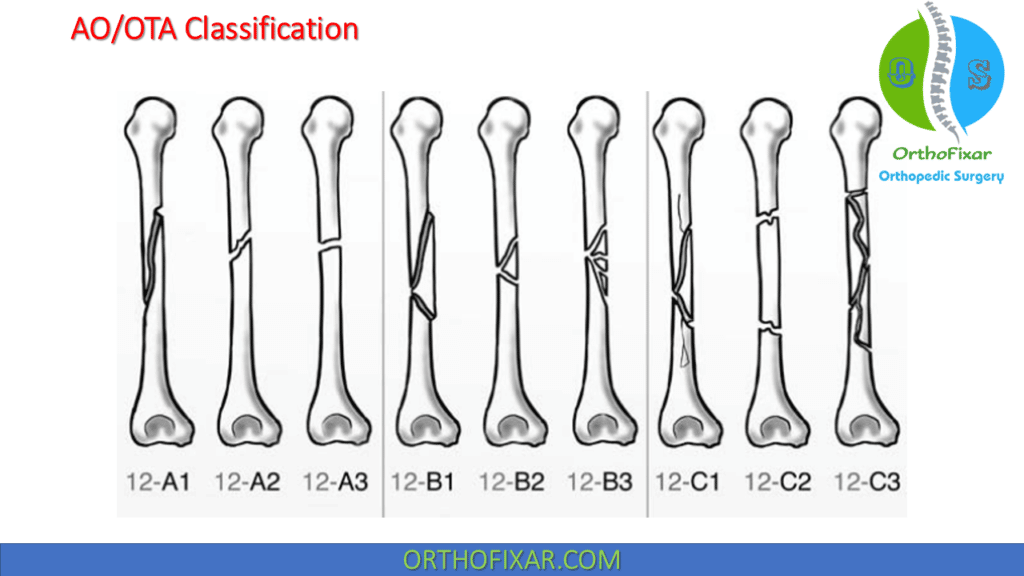
Humeral Shaft Fractures Classification
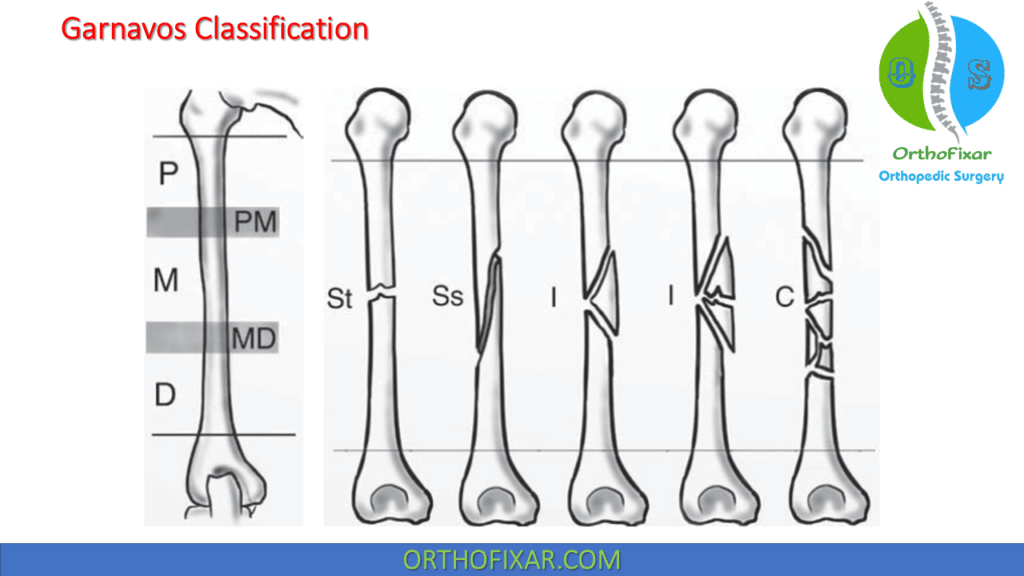
Garnavos classification of diaphyseal humeral fractures is based on:
- The location (proximal third, middle third, distal third),
- The degree of displacement or the fracture anatomy (transverse, oblique, spiral, segmental, comminuted).
In 1963, Holstein and Lewis associated a special type of fracture of the distal humerus, a simple displaced spiral fracture, with the distal end deviating toward the radial side occurring in about 7% of all humeral shaft fractures, with an increased rate of radial nerve palsy, it’s called a Holstein-Lewis fracture.
Humeral Shaft Fracture Treatment
The principles of humeral shaft fracture treatment are to achieve union with an acceptable alignment and to restore the patient quickly to pre-injury functional status. This is usually achieved by conservative measures in the majority of patients.
Non-Operative Treatment
Most humeral shaft fractures (>90%) will heal with non-surgical management. About 20° of angulation and up to 3 cm of apposition do not cause functional disability in the upper limb.
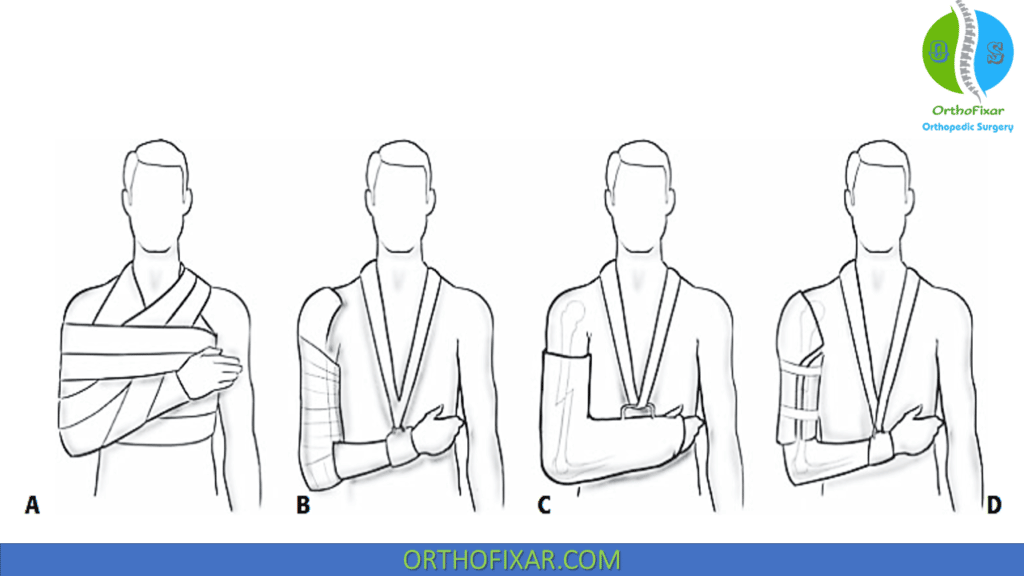
The methods of conservative care are:
- Hanging cast: This utilizes gravity-dependent traction by the weight of the cast and arm to effect fracture reduction. It is useful in displaced midshaft humerus fractures, particularly spiral or oblique patterns.
- Coaptation splint: This utilizes dependency traction to effect fracture reduction. It is indicated for the acute treatment of humeral shaft fractures with minimal shortening and for short oblique or transverse fracture patterns that may displace with a hanging arm cast.
- Thoracobrachial immobilization (Velpeau dressing): This is used in elderly patients or children who are unable to tolerate other methods of treatment and in whom comfort is the primary concern. It is indicated for minimally displaced or non-displaced fractures that do not require reduction.
- Functional bracing: This utilizes hydrostatic soft-tissue compression to effect and maintain fracture alignment while allowing motion of adjacent joints. It is typically applied 1–2 weeks after injury, after the patient has been initially placed in a hanging arm cast or coaptation splint and swelling has subsided. It consists of an anterior and posterior shell held together with Velcro straps. Success depends on an upright patient and tightening the brace daily. The functional brace is usually needed for a period of 8 weeks after fracture or until there is radiographic evidence of union. The treating orthopaedic surgeon should be wary of distraction in transverse humeral fractures, thus posing an increased risk of non-union.
Operative treatment
Although most humeral shaft fractures can be managed by non-operative methods, with 100% expected union rates, there are a few instances when surgical stabilization would be prescribed. The indications for operative treatment are polytraumatized patients, inadequate closed reduction, pathological fracture, associated vascular injury, floating elbow injury, segmental fractures, fractures with intraarticular extension, bilateral humeral fractures, open fractures, neurological loss following penetrating trauma, radial nerve palsy occurring after fracture manipulation and non-union.
The anterolateral approach is usually preferred for proximal third humeral shaft fractures. The posterior approach also provides an excellent exposure of the entire humerus and is preferred for distal third humeral fractures and whenever there is a need to explore the radial nerve.
Methodes of Humeral Shaft Fracture surgical stabilization:
Operative stabilization can be performed by:
- compression plate device,
- intramedullary fixation
- rarely, by external fixation.
Open reduction and internal fixation with a compression plate gives the best functional results and is the usual preferred method of fixatio. One should take care to preserve soft-tissue attachments of butterfly fragments during exposure and fixation.
Intramedullary fixation is indicated in segmental fractures, fractures in extremely osteopenic bone and pathological humeral fractures. Either flexible nails or rigid interlocked nails are used. Multiple flexible nails inserted antegrade or retrograde fill the canal to achieve an interference fit. They are primarily reserved for humeral shaft fractures with minimal comminution. Interlocked nails have proximal and distal interlocking facilities and are able to provide rotational and axial fracture stability. Antegrade nailing methods are associated with a high incidence of shoulder pain and efforts must be taken to avoid damage to the rotator cuff to minimize postoperative shoulder problems. The proximal aspect of the nail should also be countersunk to prevent subacromial impingement.
External fixation is indicated in special situations such as infected non-unions and open fractures with extensive soft-tissue loss.

Complications
Possible complication after Humeral Shaft Fractures include:
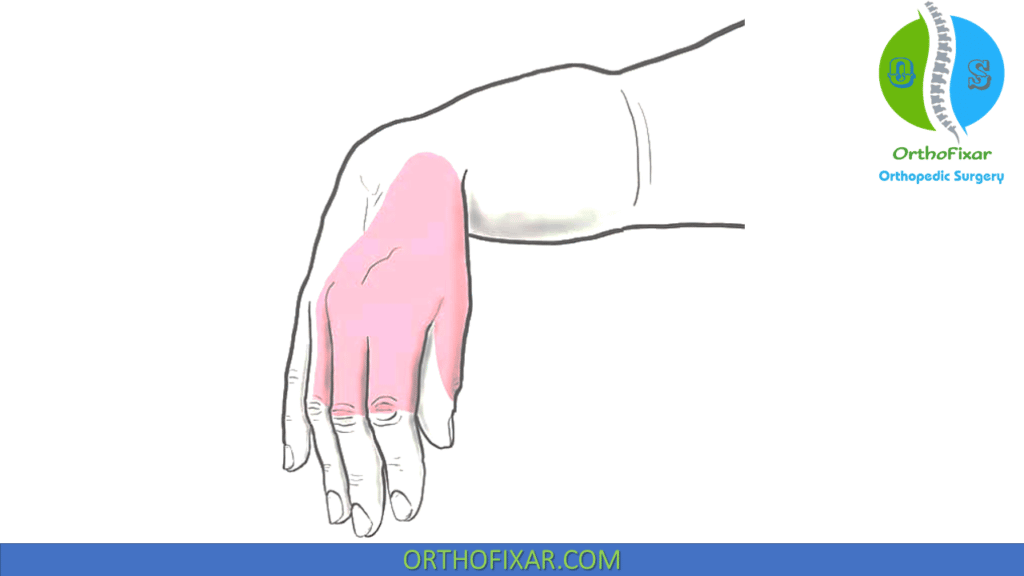
- Radial nerve injury occurs in up to 18% of cases. It is commonly seen with midshaft humerus fracture. Holstein–Lewis syndrome refers to spiral distal third humeral fractures, which may entrap or lacerate the nerve as it passes through the lateral intermuscular septum. The neurological injury can also occur during manipulation of the fracture. Most injuries are neurapraxia with spontaneous recovery within 5 months. Neurological recovery is assessed clinically by Tinel’s sign, electromyography and nerve conduction studies. If there is no recovery even after 6 months, tendon transfers to correct the wrist drop and loss of extension at the metacarpophalangeal joints of the fingers and thumb can be performed with good functional results.
- Vascular injury is uncommon in closed injuries but can occur in open injuries. The brachial artery has the greatest risk for injury in fractures at the junction of the proximal and distal third of the arm.
- Malunion is frequent after conservative fractures but usually does not produce functional disability.
- Non-unions may occur with over distraction during conservative treatment or following internal fixation due to decreased vascularity of the fractured ends or poor surgical techniques.
Q&A For Patients
How is a humeral shaft fracture treated?
Humeral shaft fracture can be treated non-operatively by a sling /splint or surgically by open surgery (plate fixation) or close reduction and nailing or external fixation. The type of treatment is based on the fracture type and associated soft tissue injuries (especially radial nerve injury that needs a surgical exploration).
Can a humerus fracture heal without surgery?
Most of the humerus shaft fracture can be managed non-operatively without surgery. In some cases, such as severely displaced fractures or in case of radial nerve injury, the fracture needs to be fixed surgically.
How long does it take a humeral shaft fracture to heal?
Usually, it takes 3-4 months to heal completely, but this also depends on the type of treatment.
How should you sleep with a broken shoulder?
In every position you take in daily life, your injured limb should be elevated above your heart, this prevents blood from pooling and causing swelling. In the bed, try to sleep on your back and support yourself with several pillows, or you can sleep on your other side if possible, and try not to sleep on your broken humerus

References & More
- Mercer’s Textbook of Orthopaedics and Trauma, Tenth edition.
- Rockwood and Green’s Fractures in Adults 8th Edition book.
- Mast JW, Spiegel PG, Harvey JP Jr, Harrison C. Fractures of the humeral shaft: a retrospective study of 240 adult fractures. Clin Orthop Relat Res. 1975 Oct;(112):254-62. PMID: 1192642.
- Holm CL. Management of humeral shaft fractures. Fundamental nonoperative techniques. Clinical Orthopaedics and Related Research 1970;91:132–9.
- Sarmiento A, Zagorski JB, Zych G, et al. Functional bracing for the treatment of fractures of the humeral diaphysis. Journal of Bone and Joint Surgery (American) 2000;82:478–86.
- Vander Griend RA, Tomasin J, Ward EF. Open reduction and internal fixation of humeral shaft fractures: results using AO plating techniques. Journal of Bone and Joint Surgery (American) 1986;68:430–3.
- Holstein A, Lewis GB. Fractures of the humerus with radial nerve paralysis. Journal of Bone and Joint Surgery (American) 1963;45:1382–8.