The Local Anesthetics is membrane-stabilizing drugs that act by causing a reversible block to conduction along nerve fibers.
The smaller nerve fibers are more sensitive, so that a differential block may occur where the small fibers carrying pain and autonomic impulses are blocked, sparing coarse touch and movement.
Uptake into the systemic circulation is important for terminating their action and also for producing toxicity. Following most regional anesthetic procedures, maximum arterial plasma concentrations of local anesthetic develop within about 10 to 25 minutes, so careful surveillance for toxic effects is recommended for the first 30 minutes after injection if significant volumes are used.
See Also: Local Steroid Injection
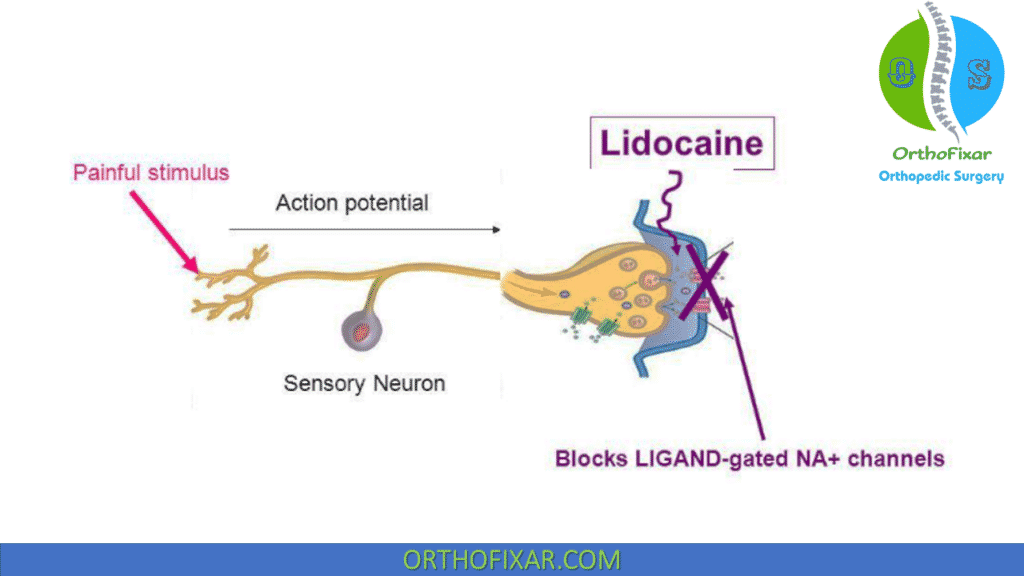
What is local anesthetic used for?
Analgesic
Although the local anesthetic effect is temporary, this may make the overall procedure less unpleasant for the patient, break the pain cycle (by reducing nociceptive input to the gate in the dorsal horn of the spinal cord) and increase the confidence of the patient in the clinician, the diagnosis and the treatment.
In one study, pain inhibition was better with bupivacaine than lidocaine during the first 6 hours, presumably because of its longer half-life; in later evaluations, no differences in outcomes were observed. In another study, bupivacaine was superior to lidocaine at 2 weeks, but not at 3 and 12 months.
Some practitioners inject a mixture of short- and long-acting local anesthetic to obtain both the immediate diagnostic effect and more prolonged pain relief.
Diagnostic
The pain relief following local anesthetics injection confirms the diagnosis and the correct placement of the solution. Sometimes, even the most experienced practitioner will be unsure exactly which tissue is at fault; in this situation, a small amount of local anesthetic may be injected into the most likely tissue and the patient re-examined after a few minutes. If the pain is relieved, then the source of the problem has been identified, and further treatment can be accurately directed.
See Also: Subacromial Injection Test
Dilution
The internal surface area of joints and bursae is surprisingly large because of the highly convoluted synovial lining, with its many villae, so an increased volume of the injected solution helps spread the steroid around this surface.
Distension
There is a beneficial volume effect in joints and bursae, which may be the physical stretching of the capsule or bursa with physical disruption of adhesions. There is silver level evidence that arthrographic distension with saline and steroid provides short-term benefits in pain, range of movement and function in adhesive capsulitis of the shoulder.
Distension is not required at entheses, so the smallest practicable volume should be used; distension in tendons by the bolus injection of a relatively large volume of solution may physically disrupt the fibers, compress the relatively poor arterial supply and also give rise to distension pain.
Local anesthesia drugs name
Local anesthesia drugs vary widely in their potency, duration of action and toxicity. The most commonly used anesthetics for joint and soft tissue injection are as follows:
Lidocaine hydrochloride:
This was previously lignocaine hydrochloride in the United Kingdom. It is the most widely used local anesthetic, acts more rapidly and is more stable than others. The effects occur within seconds and the duration of block is about 30 minutes after lidocaine injection.
Marcaine (bupivacaine):
It has a slow onset of action (≈30 minutes for full effect), but the duration of block is up to 8 hours. It is the principal drug used for spinal anesthesia in the United Kingdom. It’s not used for routine outpatient injections because the delayed onset of action precludes the immediate diagnostic effect available with lidocaine and, if there is an adverse effect, this will take a long time to dissipate.
There is no evidence of any long-term benefit from using bupivacaine instead of lidocaine. Compared with placebo, the effect of intraarticular bupivacaine wears off in less than 24 hours.
Prilocaine:
This has low toxicity, similar to that of lidocaine, but is not as commonly used. Procaine is now also seldom used. It is as potent as lidocaine but with a shorter duration of action.
Lidocaine (under the brand name Xylocaine) and Marcaine are also manufactured with added adrenaline, which causes vasoconstriction when used for skin anesthesia, and so prolongs the local anesthetic effect. These preparations are not recommended for procedures involving the appendages because of the risk of ischemic necrosis.
Recommended maximum doses of local anesthesia drugs
| Drug | Strength | Maximum dose and volume | Suggested maximum |
|---|---|---|---|
| Lidocaine | 0.5%, 5 mg/ml 1.0%, 10 mg/ml 2.0%, 20 mg/ml | 200 mg, 40 ml 200 mg, 20 ml 200 mg, 10 ml | 100 mg, 20 ml 100 mg, 10 ml 100 mg, 5 ml |
| Bupivacaine | 0.25%, 2.5 mg/ml 0.5%, 5 mg/ml | 150 mg, 60 ml 150 mg, 30 ml | 75 mg, 30 ml 75 mg,15 ml |
Side Effects
Local Anesthetics side effects are the same as corticosteroids side effects that include:
Local side effects
- Postinjection flare of pain
- Skin depigmentation
- Fat atrophy
- Bleeding, bruising
- Steroid chalk, calcification
- Steroid arthropathy
- Tendon rupture, atrophy
- Joint, soft tissue infection
Systemic side effects
- Facial flushing
- Impaired diabetic control
- Menstrual irregularity
- Hypothalamic-pituitary axis suppression
- Fall in erythrocyte sedimentation rate, C-reactive protein level
- Anaphylaxis (very rare)
References
- Speed CA. Injection therapies for soft-tissue lesions. Best Pract Res Clin Rheumatol. 2007 Apr;21(2):333-47. doi: 10.1016/j.berh.2006.11.001. PMID: 17512486. Pubmed
- British Medical Association and Royal Pharmaceutical Society. British National Formulary No. 72. London: British Medical Association and Royal Pharmaceutical Society; 2017:1181.
- Kannus P, Jarvinen M, Niittymaki S. Long- or short-acting anesthetic with corticosteroid in local injections of overuse injuries? A prospective, randomized, double-blind study. Int J Sports Med. 1990;11(5): 397–400.
- Sölveborn SA, Buch F, Mallmin H, et al. Cortisone injection with anaesthetic additives for radial epicondylalgia. Clin Orthop Relat Res. 1995;316:99–105.
- British Medical Association and Royal Pharmaceutical Society. British National Formulary No. 72.
- Ines LPBS, da Silva JAP. Soft tissue injections. Best Pract Res Clin Rheumatol. 2005;19(3):503–527.
- Buchbinder R, Green S, Forbes A, et al. Arthrographic joint distension with saline and steroid improves function and reduces pain in patients with painful stiff shoulder: results of a randomised, double-blind, placebo-controlled trial. Ann Rheum Dis. 2004;63:302–309.
- Jacobs LGH, Barton MAJ, Wallace WA, et al. Intraarticular distension and steroids in the management of capsulitis of the shoulder. BMJ. 1991;302:1498–1501.
- Ahmed I, Gertner E. Safety of arthrocentesis and joint injection in patients receiving anticoagulation at therapeutic levels. Am J Med. 2012;125(3):265–269.
- Creamer P, Hunt M, Dieppe P. Pain mechanisms in osteoarthritis of the knee: effect of intraarticular anesthetic. J Rheumatol. 1996;23:1031–1036.