The first use of local Steroid Injections for arthritic joints was reported in 1951, Hollander, in the United States.
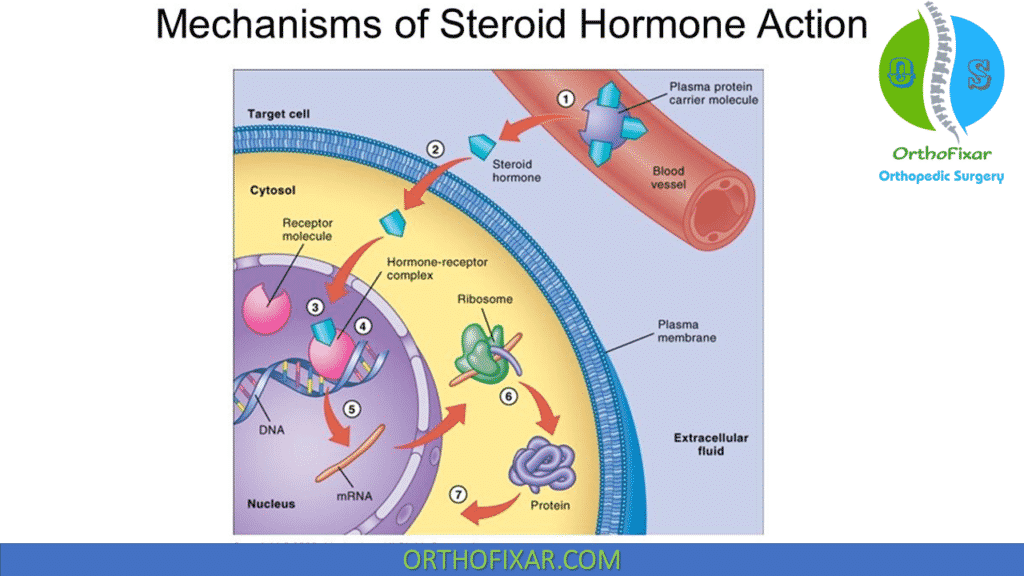
Steroid Mechanisms
Local Steroid Injections are thought to work by a number of mechanisms:
Suppressing inflammation
They suppress inflammation in inflammatory systemic diseases such as rheumatoid or psoriatic arthritis and gout. Synovial cell infiltration and proinflammatory cytokine expression are reduced in a multifaceted manner by intraarticular corticosteroid injection.
The role of inflammation in tendinopathy is controversial and in recent years, mainstream opinion has asserted that the condition is purely degenerative. However, this view is being challenged because it has been found that increased numbers of specific inflammatory cells are present in pathological tendons, consistent with a chronic inflammatory process.
See Also: Nerve Block For Hand Surgery
Suppressing inflammatory flares
They appear to suppress inflammatory flares in degenerative joint disease. However, the pathophysiology of osteoarthritis is poorly understood, and there are no reliable clinical features that predict which osteoarthritic joints will respond to injection. Often, the only way to find out is with an empirical trial of injection therapy.
Breaking up the inflammatory damage-repair-damage cycle
This is postulated to set up a continuous, low-grade, inflammatory response, inhibiting tissue repair and sound scar formation while forming adverse adhesions. However, there is little direct evidence to support this.
Protecting cartilage
There may be a direct chondroprotective effect on cartilage metabolism or other effects not related to the antiinflammatory activity of the steroids, such as promotion of articular surfactant production.
Direct analgesic effect
Inflammation is a complex cascade of molecular and cellular events. The precise role of inflammation in tendinitis is the subject of considerable debate, and many authors prefer the terms tendinosis or tendinopathy to describe the pathological changes.
Tendon pain may not be caused by inflammation (tendinitis) or structural disruption of the tendon fibres (tendinosis), but might instead be caused by the stimulation of nociceptors by chemicals such as glutamate, substance P and chondroitin sulphate released from the damaged tendon.
Corticosteroids (and possibly local anesthetics) may inhibit the release of noxious chemicals and/or the long-term behavior of local nociceptors. In vitro, corticosteroids have also been shown to inhibit the transmission of pain along unmyelinated C fibers by a direct membrane action.
Other effects
Intraarticular corticosteroid given over 3 months protects against periarticular bone loss in inflamed finger joints in rheumatoid arthritis.
Note: The authors strongly advise that all clinicians thoroughly study the most up to date manufacturers’ data sheets for the drugs that they propose to use for injection therapy and stay abreast of any subsequent modifications.
Types of Steroid Injection
The following are commonly used Steroid Injection:
Triamcinolone acetonide:
- Adcortyl (10 mg/ml, dilute)
- Kenalog (40 mg/ml, concentrated)
Triamcinolone acetonide – 40 mg is equivalent to the following:
- Triamcinolone hexacetonide, 20 mg
- Methylprednisolone, 40 mg
- Hydrocortisone, 200 mg
- Betamethasone, 7.5 mg
- Dexamethasone, 7.5 mg
- Prednisolone, 50 mg.
Kenalog can be used in very small quantities, so it is ideal for small joints and tendon entheses, in which distension may increase pain.
Adcortyl, however, is useful when a larger volume is required, as in larger joints and bursae. The duration of action of the drug is approximately 2 to 3 weeks.
Triamcinolone hexacetonide
Lederspan (20 mg/ml, concentrated)
The least soluble and longest lasting injectable corticosteroid, Pharmacokinetic studies have shown that the biological effect of triamcinolone acetonide is equivalent to that of triamcinolone hexacetonide if used at double the dosage, but even when triamcinolone acetonide is given at higher doses, triamcinolone hexacetonide has proven to be more effective, with a greater duration of action in head-to-head studies.
Methylprednisolone acetate
Depo Medrone (40 mg/ml, concentrated)
This drug may cause more post-injection pain than triamcinalone acetonide. It is also available premixed with local anesthetic as Depo Medrone (40 mg/ml) with lidocaine (10 mg/ml) in 1- and 2 ml vials, which we do not use because it is a fixed-dose combination and therefore difficult to adjust.

Betamethasone
Celestone Soluspan (United States; betamethasone sodium phosphate, 3 mg, and betamethasone acetate, 3 mg = 6 mg/ml, concentrated)
The dose of Celestone Chronodose in Australia is slightly different. Celestone is licensed to be mixed (in the syringe, not the ampoule) with 1% or 2% lidocaine.
Hydrocortisone
Hydrocortistab (25 mg/ml, very dilute).
This is very soluble and has the shortest duration of action of the corticosteroids mentioned here, perhaps as little as 6 days. It may be particularly useful for superficial injections in thin, dark-skinned patients, in whom depigmentation or local fat atrophy may be more noticeable.
Local side effects of Steroid Injection
Local steroid side effects may occur when an injection is misdirected or too large a dose in too large a volume is injected too often. Subcutaneous placement of the steroid and the injection of a drug bolus at entheses must both be avoided. Serious local side effects are rare.
Local side effects include the following:
Postinjection flare of pain
The quoted figures are from about 2 to 10%, but this is well in excess of our own experience. When it does happen, it is usually after a soft tissue injection and rarely follows a joint injection. When a corticosteroid is mixed with a local anaesthetic, the solution should be inspected carefully for flocculation or precipitation before injecting because this may be related to postinjection flare of pain.
It may also be caused by the rapid intracellular ingestion of the microcrystalline steroid ester and must always be distinguished from sepsis. There may be more frequent postinjection flares with methylprednisolone, but this may have more to do with the preservative in the drug than with the corticosteroid itself.
An early increase in joint stiffness following intraarticular corticosteroids is consistent with a transient synovitis. Multidose bottles of lidocaine contain parabens as a preservative. Many steroids will precipitate when added to it, and this precipitate may be responsible for some cases of postinjection flare of pain and steroid chalk.
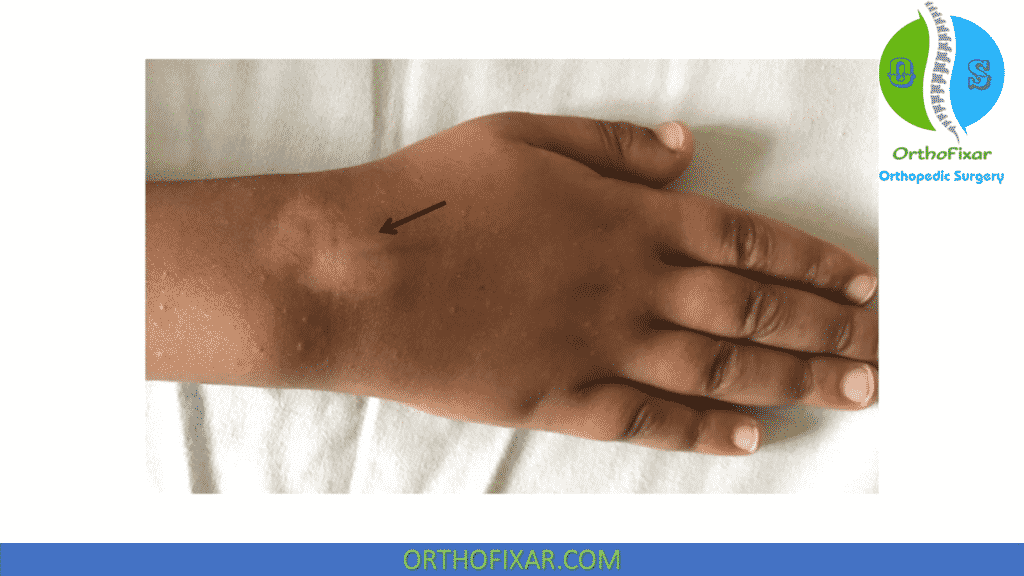
Subcutaneous atrophy and/or skin depigmentation
In one meta-analysis of shoulder and elbow injections, skin modification had a frequency of 4%. Skin changes may be more likely to occur when superficial lesions are injected, especially in dark-skinned patients.
The injected drugs should not be allowed to reflux back through the needle tract; pressure applied around the needle with cotton wool when withdrawing may help. Fat atrophy following corticosteroid injection may rarely have significant functional consequences.
Bleeding or bruising
This may occur at the injection site. Apply firm pressure to the injection site immediately following needle withdrawal. Joint and soft tissue injections and aspirations in selected patients taking stable doses of warfarin sodium are associated with a low risk of haemorrhage.
There is no need to stop this medication before injection therapy. There is little information to guide the clinician when considering injection therapy in patients taking an antiplatelet drug such as aspirin, dipyridamole or clopidogrel, an oral nonsteroidal antiinflammatory drug (NSAID) or a novel oral anticoagulant, nonvitamin K antagonist oral anticoagulant (NOAC).
Steroid chalk or paste
This may be found on the surface of previously injected tendons and joints during surgery. Suspension flocculation, resulting from the mixture of steroid with a local anaesthetic containing preservative, may be responsible. The clinical significance of these deposits is uncertain.
Soft tissue calcification
Periarticular calcification may be associated with large numbers of repeated injections into the small joints of the hand. Cortisone injection into osteoarthritic interphalangeal joints of the hand may possibly result in calcification or joint fusion because of pericapsular leakage of steroids as a result of raised intraarticular pressure.
Steroid arthropathy
This is a well-known and much feared complication of local cortisone injection treatment, but it is also largely a myth. In many cases, injected steroid can be chondroprotective rather than destructive. There is good evidence linking prolonged high-dose oral steroid usage with osteonecrosis, but almost all the reports linking injected steroids with accelerated nonseptic joint destruction are anecdotal and mainly relate to joints receiving huge numbers of injections.
Tendon rupture and atrophy
The literature does not provide precise estimates for complication rates following the therapeutic use of injected or systemic steroids in the treatment of athletic injuries, but tendon and fascial ruptures are reported complications of injection. Tendon and fascial rupture or atrophy is probably minimized by withdrawing the needle a little if an unusual amount of resistance is encountered and by using a peppering technique at entheses with the smallest effective dose and volume of steroid.
Delayed soft tissue healing
This may be associated with local steroid injection. In a study of rabbit ligaments, the tensile strength of the injected specimens returned to a value equal to that of the noninjected controls; however, the peak load of the injected specimens remained inferior, with a lag in histological maturation. This has implications for the timing of return to activity following injection therapy.
Sepsis
Joint sepsis is the most feared complication of steroid injection treatment; it may be lethal but is a rarity. Soft tissue infections and osteomyelitis can also occur after local soft tissue injection.
Following an injection, swelling at the site, increased pain, fever, systemic upset (e.g., sweating, headaches) and severe pain on all attempted active and passive movements should raise clinical suspicion of infection.
Fragments of skin may be carried into a joint on the tip of a needle and may be a source of infection
Joint infections may also possibly occur by haematogenous spread, rather than by direct inoculation of organisms into the joint. Steroid injection may create a local focus of reduced immunity in a joint, thus rendering it more vulnerable to bloodborne spread.
Rarely, injection of contaminated drugs or hormonal activation of a quiescent infection may be to blame.
Rare local side effects
These include nerve damage (severe pain and electric shocks if you needle a nerve), transient paresis of an extremity (from an inadvertent motor nerve block) and needle fracture.
References
- Kirwan JR, Bálint G, Szebenyi B. Anniversary: 50 years of glucocorticoid treatment in rheumatoid arthritis. Rheumatology (Oxford). 1999 Feb;38(2):100-2. doi: 10.1093/rheumatology/38.2.100. PMID: 10342620.
- Goulding NJ. Corticosteroids – a case of mistaken identity? Br J Rheumatol. 1998;37:477–480.
- Coombes GM, Bax DE. The use and abuse of steroids in rheumatology. Rep Rheum Dis. 1996;(Ser 3):1.
- Hollander JL, Brown EM Jr, Jessar RA, et al. Hydrocortisone and cortisone injected into arthritic joints; comparative effects of a use of hydrocortisone as a local anti-arthritic agent. JAMA. 1951;147(17):1629–1635.
- Creamer P. Intra-articular corticosteroid injections in osteoarthritis: do they work, and if so, how? Ann Rheum Dis. 1997;56:634–636.
- af Klint E, Grundtman C, Engström M, et al. Intraarticular glucocorticoid treatment reduces inflammation in synovial cell infiltrations more efficiently than in synovial blood vessels. Arthritis Rheum. 2005;52(12):3880–3889.
- Goulding NJ. Anti-inflammatory corticosteroids. Rep Rheum Dis. 1999;(Ser 3):1.
- Cutolo M. The roles of steroid hormones in arthritis. Br J Rheumatol. 1998;37:597–599.
- Speed CA. Injection therapies for soft-tissue lesions. Best Pract Res Clin Rheumatol. 2007;21(2):333–347.
- Ines LPBS, da Silva JAP. Soft tissue injections. Best Pract Res Clin Rheumatol. 2005;19(3):503–527.
- Cole BJ, Schumacher RH Jr. Injectable corticosteroids in modern practice. J Am Acad Orthop Surg. 2005;139(1):37–46.
- Price R, Sinclair H, Heinrich I, et al. Local injection treatment of tennis elbow – hydrocortisone, triamcinolone and lignocaine compared. Br J Rheumatol. 1991;30(1):39–44.
- Yoon SH, Lee HY, Lee HJ, et al. Optimal dose of intra-articular corticosteroids for adhesive capsulitis: a randomized, triple-blind, placebo-controlled trial. Am J Sports Med. 2013;41(5):1133–1139.
- Anon. Gout in primary care. Drugs Ther Bull. 2004;42(5):37–40.
- Gossec L, Dougados M. Intra-articular treatments in osteoarthritis: from the symptomatic to the structure modifying. Ann Rheum Dis. 2004;63:478–482.
- Kirwan JR, Rankin E. Intraarticular therapy in osteoarthritis. Baillieres Clin Rheumatol. 1997;11(4):769–794.
- Franz JK, Burmester GR. Antirheumatic treatment: the needle and the damage done. Ann Rheum Dis. 2005;64:798–800.
- Rees JD, Stride M, Scott A. Tendons – time to revisit inflammation. Br J Sports Med. 2014;48:1553–1557.
- Dean BJF, Gettings P, Dakin SJ, et al. Are inflammatory cells increased in painful human tendinopathy? A systematic review. Br J Sports Med. 2016;50:216–220.
- Rees JD. The role of inflammatory cells in tendinopathy: is the picture getting any clearer? Br J Sports Med. 2016;50:201– 202.
- Injection Techniques in Musculoskeletal Medicine.