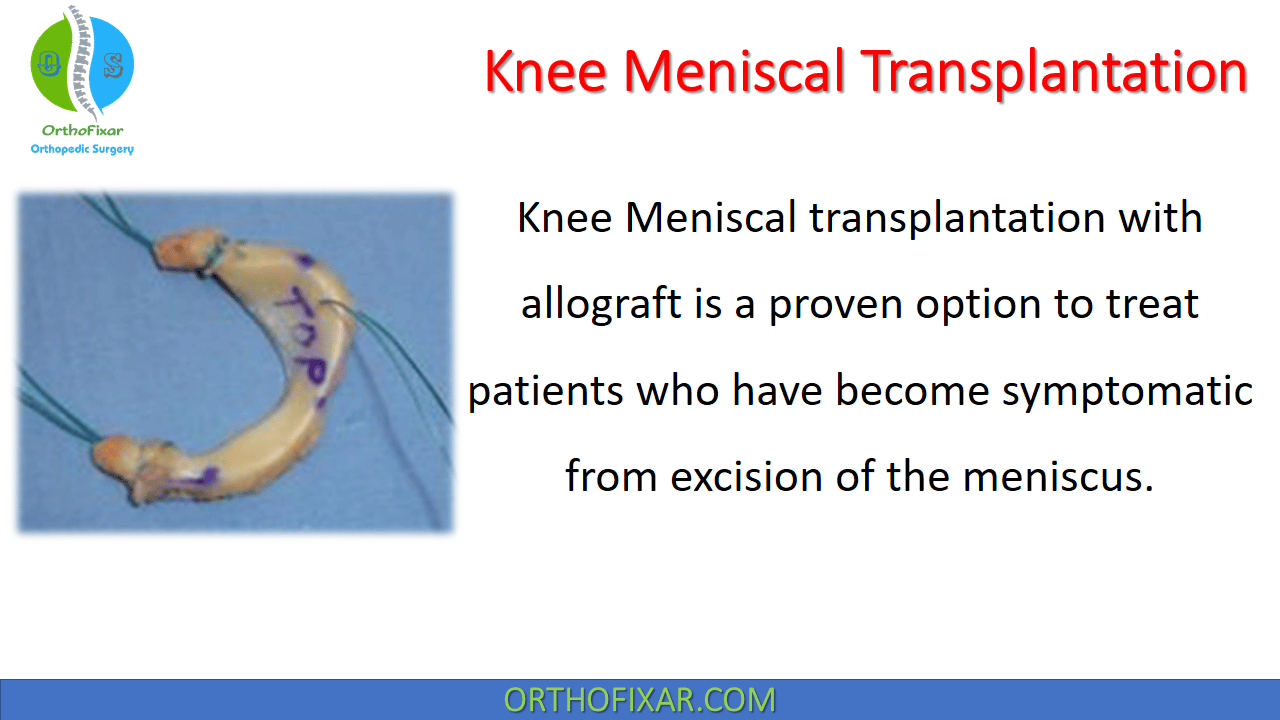
Knee Meniscal transplantation with allograft is a proven option to treat patients who have become symptomatic from excision of the meniscus.
The meniscus plays a vital role in preserving normal knee function, including shock absorption, load transmission, stability, joint lubrication, and nutrition. Thus, subtotal removal of the meniscus enhances the rate of degenerative arthritis in the knee. Although preservation of the meniscus should be the standard of care, most tears are treated with excision.
Since the first isolated meniscal transplant was performed in 1984, surgical techniques have continued to improve and have transitioned from open procedures to arthroscopic-assisted procedures. Although some authors have reported good outcomes with only soft tissue fixation of the meniscus to the host, biomechanical studies show that if the horn attachments are secured with bone, the allograft more closely replicates the normal meniscus. Thus, although it may be technically more difficult, it is currently recommended to use bone graft to bone tunnel fixation. The most commonly performed techniques to secure the horns through bone fixation are the bone bridge and bone plug methods.
Meniscal Transplantation Indications
A thorough history is of vital importance and should include information regarding previous knee injuries, specific symptoms, and prior treatments and surgical procedures. For consideration of meniscal allograft transplantation, the patient should have pain localized to the meniscus-deficient compartment, although joint effusions can result in some generalized discomfort. Particular emphasis should also be paid to any chondral lesions, limb alignment, and ligament stability. An effort should be made to obtain operative reports and intraoperative photographs, which can be useful in determining the amount of meniscus remaining and the condition of the articular cartilage.
Meniscal transplantation should be performed with the goal of reducing pain with the ability to increase activity level secondary. Because of the lack of evidence, patients should not be told to expect the procedure to delay or prevent the progression of osteoarthritis.
Meniscal transplantation should be considered only when nonsurgical measures to control pain have been exhausted and/or there is evidence that the involved compartment is degenerating. In general, a patient should have a history of symptoms localized to the meniscus-deficient compartment and not have advanced arthritic changes.
Grade IV chondromalacia is a contraindication unless a defect is focal and can be treated with a cartilage repair/replacement method. It is commonly recommended that patients should be younger than 50 to 55 years; however, this is controversial, and age restrictions should also be based on a patient’s physiologic age.
- Majority of meniscus excised
- Pain in the meniscus-deficient compartment
- Chondromalacia no greater than grade III
- Knee without ligament laxity
- Age typically younger than 55 years
Controversial Indications
Although not absolute contraindications, patients with ligament laxity, limb malalignment, and full-thickness chondral defects need to have these addressed to be considered. It is well known that the medial meniscus is an important secondary stabilizer in patients with an anterior cruciate ligament (ACL)-deficient knee. In addition, chronically ACL-deficient knees have been shown to be associated with increased rates of meniscal tears. Thus, patients with ACL-deficient knees require reconstruction before the meniscus is replaced or, more commonly, at the same time as the meniscus.
Limb alignment is another circumstance that can substantially affect the outcome of meniscal allograft transplantation. Although it is not uniformly agreed upon, many surgeons will perform an osteotomy to unload the involved compartment if the mechanical axis is a few degrees greater than the contralateral knee. The extent of the correction is typically to have the mechanical axis pass through the contralateral tibial spine rather than the more extensive correction recommended for arthritic knees. The procedure can be staged or performed at the same time as the meniscus, which is what the author prefers.
Full-thickness cartilage defects have previously been considered to be a contraindication for meniscal allograft transplantation. However, if the defect is isolated and can be corrected with a cartilage repair or restoration procedure, it is not contraindicated.
- Isolated full-thickness chondral defect
- Limb malalignment
- Age older than 55 years
The primary contraindication to meniscal allograft transplantation is advanced arthritis. A history of infection, inflammatory arthropathy, synovial disease, and morbid obesity represent other contraindications.
Meniscal Transplantation Procedure
Equipment
- Meniscus allograft
- Sized match graft (plain x-rays are typically sufficient)
- Fresh-frozen allograft preferred
- Arthroscopy tower and equipment for standard knee arthroscopy
- Meniscus repair devices (surgeon’s preference)
- Long-length, open-ended meniscus suturing needles
- Lateral meniscal allograft
- Dovetail instrumentation
- Oscillating saw
- Medial meniscal allograft
- ACL guide and drill system
- 0.062 K-wire
- Coring reamer (8 mm)
- Small motorized burr
- Polyethylene button or low-profile screw
Meniscal Allograft Sizing
The clinical outcomes following meniscal transplantation are dependent on matching the size of the allograft to the native meniscus. Allografts that are oversized lead to greater forces across the articular cartilage, whereas undersized allografts lead to normal forces across the articular cartilage but greater stress across the meniscus repair. Sizing of meniscal allografts can be done by using plain x-rays, computed tomography (CT), or MRI.
Sizing based on plain x-rays is most common with the Pollard method often followed and has been shown to correlate well with actual anatomical measurements.
- The meniscal width can be determined by measuring the distance from the peak of the tibial eminence to the edge of the tibial plateau on the AP x-ray.
- Meniscal length can be obtained by measuring the sagittal length of the tibial plateau on the lateral x-ray.
The medial and lateral meniscus length equals 80% and 70% of the tibial plateau, respectively. Although CT and MRI scans are more precise, they add additional cost with questionable benefit. A 5% difference in size is commonly stated as acceptable and able to be obtained with proper technique with plain x-rays. Although not uniformly agreed, it is probably better to err on the graft being bigger in size because shrinkage of the graft is common and shown to be on average of 7% shrinkage.
Meniscus Allograft Preservation
Four methods of preserving meniscal allografts are available and include fresh, cryopreserved, fresh frozen, and freeze dried (lyophilization). Fresh meniscus grafts carry an increased risk of infection and immune load. Cryopreservation adds an increased cost and has not shown to be of improved results. Lyophilization alters the meniscal properties of the meniscus and is not recommended.
Thus, fresh-frozen grafts are the most commonly used Meniscus allograft preservation method today. It is vital that the allografts are obtained from American Association of Tissue Banks–certified tissue banks, which require stringent procurement and processing methods to prevent contamination and infection of the grafts.
Additional concerns have been raised regarding the age of donors for meniscal allografts and the viability and tensile strength of the grafts. Current recommendations are for the transplantation of meniscal allografts from donors younger than 45 years. The tensile strength of meniscal tissue and the proteoglycan and collagen content have been shown to not vary with age among grafts examined from donors aged 15 to 44 years.
Positioning and Portals
The patient is placed in the supine position on a standard operating room table. After anesthesia is induced, a thorough examination of the knee under anesthesia should be performed to evaluate ROM and knee stability.
A tourniquet is placed on the thigh but often not used until the arthrotomy is made to insert the graft. Fluid extravasation can be significant and done under dry conditions, which can result in bleeding and impede visualization.
Depending on the surgeon’s preference, the leg may be left unsupported in the supine position or placed into a cushioned leg holder. Regardless of the technique, the posteromedial and posterolateral corners of the knee should be readily accessible for inside-out meniscal repair.
Description of the Procedure
Once the patient is prepped and draped, the arthroscopic portal opposite of the involved compartment should be made first. A spinal needle is used to make certain that the working portal is directly in line with the horn attachments and ease in making the channel straight rather than have some obliquity. The arthrotomy will incorporate this portal in the later stages of the procedure.
Diagnostic arthroscopy is then performed to evaluate the status of the articular cartilage, cruciate ligaments, and confirm meniscal deficiency. The meniscal allograft should not be opened until the patient is confirmed to be an appropriate candidate. Any meniscus remaining should be debrided to an outer rim of 1 to 2 mm, leaving a vascular source for healing and a reference for graft position.
If possible, the anterior and posterior horn attachments should be preserved to serve as guides for the drilling of the tunnels/channel. A limited notchplasty should be performed if there is any difficulty with visualization of the posterior attachment.
For passage of the graft, a mini-arthrotomy is performed adjacent to the patellar tendon on the affected side and in line with the insertion sites of the anterior and posterior horns. An additional posteromedial or posterolateral incision is necessary for retrieval of sutures.
Lateral: Dovetail Technique
Recipient Bed Preparation
The dovetail technique is preferred for lateral meniscus transplantation. Initial preparation is the same whether medial or lateral as well as dovetail or bone plug. Complete visualization of the meniscal remnant and horn attachments are necessary, and a small notchplasty may be needed to see the entire posterior root. Anatomic placement of the bony bridge is imperative to prevent extrusion of the meniscal allograft.
Once the attachments are identified, a 4-mm burr is used to make a shallow (1- to 2-mm) trough directly in line with the anterior and posterior horns of the meniscus. This initial trough functions as a path for placement of an osteotome in the sagittal plane. A referencing depth line on the osteotome helps to maintain proper orientation as the tibial plateau slopes inferiorly when advancing from anterior to posterior. The osteotome should be advanced under direct visualization until it contacts the posterior tibial cortex.
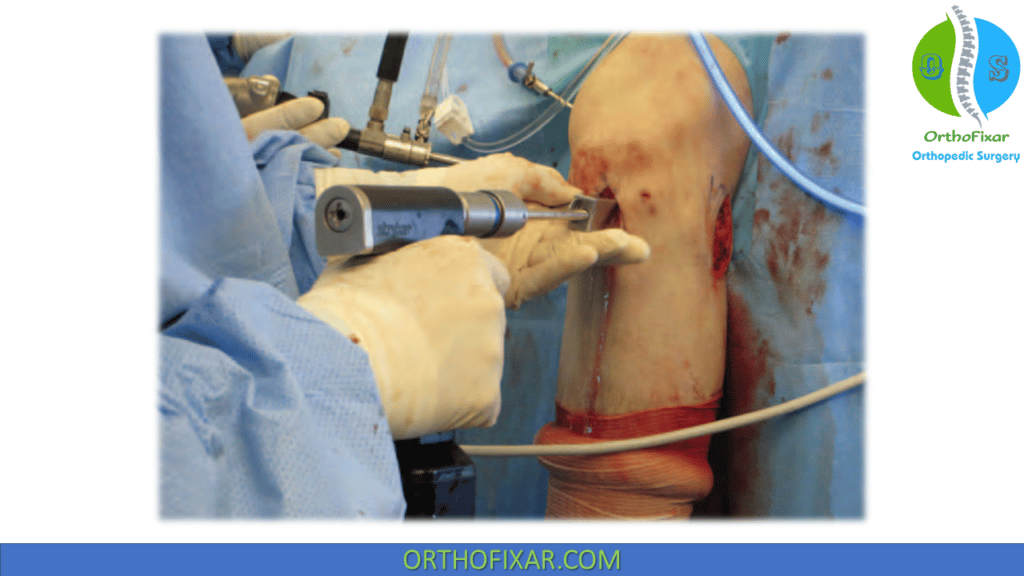
A 6-mm drill guide is fit over the osteotome, and the drill advanced. The guide enables the drill to be seen arthroscopically at all times, which helps maintain proper height and avoid breaking through the distal cortex. A second jig to accommodate a 7-mm drill at a height of 3 mm lower than the initial jig is then attached. The second drill is also seen at all times and is used to deepen the channel to 10 mm and expand the inferior aspect. A semitrapezoidal rasp is used to complete the dovetail slot.

It is important that the rasp should follow the AP slope of the tibia, and the top of the rasps should remain flush with articular surface. The channel should be cleared of all remaining bone debris, and the channel sizer should be used to ensure the channel preparation is complete. A posterolateral incision should then be made using the interval between the iliotibial band and the anterior margin of the biceps femoris tendon for access to the capsule. Although staying in front of the biceps femoris should prevent injury to the peroneal nerve, formal exposure of the nerve can always been made.

Meniscus Allograft Preparation
The meniscus allograft is typically sent by the tissue bank as a hemitibial plateau with the meniscus. It is imperative to see the entire horn attachments for proper bone cuts; thus, any excess soft tissue should be removed. The allograft bone should then be cut in an AP plane to the ends of the attachments. The end of the channel rasp is used to mark an outline of the desired dovetail design onto the ends of the bone as a reference for placing the graft in an upside-down position in the holding device.
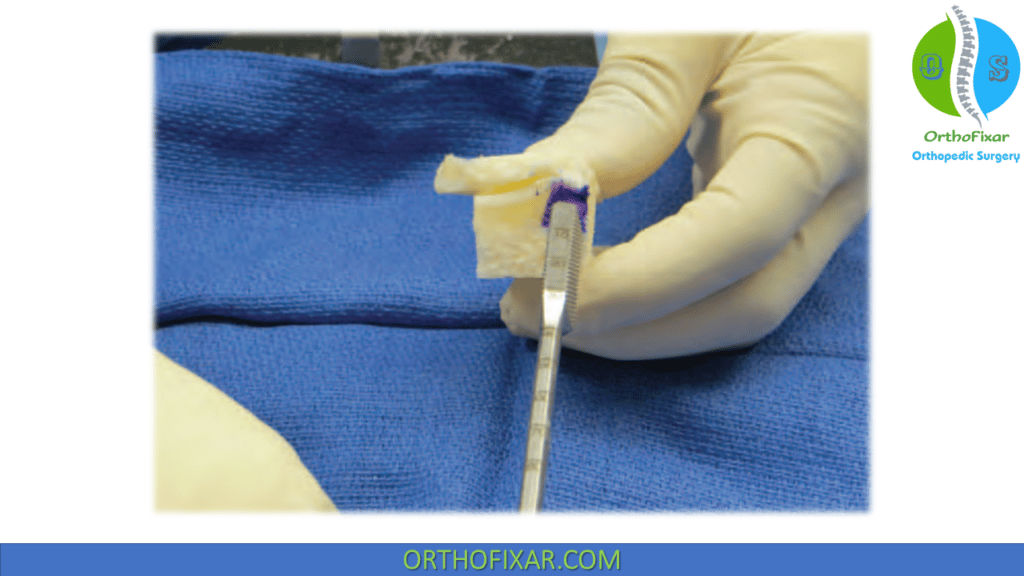
Three cutting jigs and an oscillating saw are used to complete the graft preparation. The first is a vertical cut on the medial aspect of the graft. Often, this is already precut during the meniscal allograft processing. Next, the inferior cut is made in orientation to match the depth of the slot. Finally, the third cutting guide is used to make the angled cut on the lateral aspect of the graft.


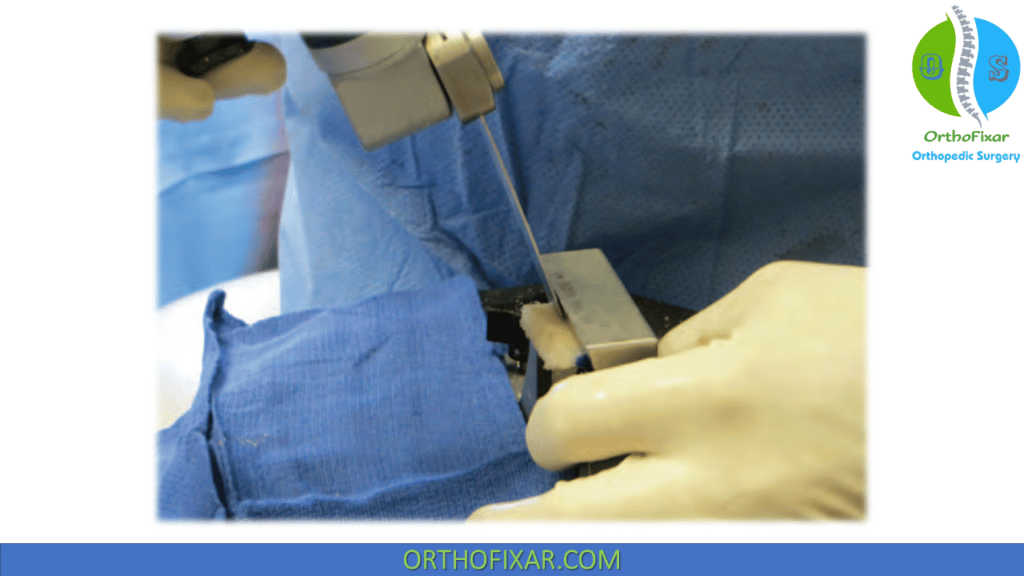
Once all cuts are complete, the sizing block is used to confirm it will allow a press fit, but the graft should also slide through smoothly. Any adjustments should be made at this time rather than trying to force the graft into the prepared channel. A 2-0 polydioxanone suture to be used as a reduction suture is placed through the posterior segment to complete the graft preparation.
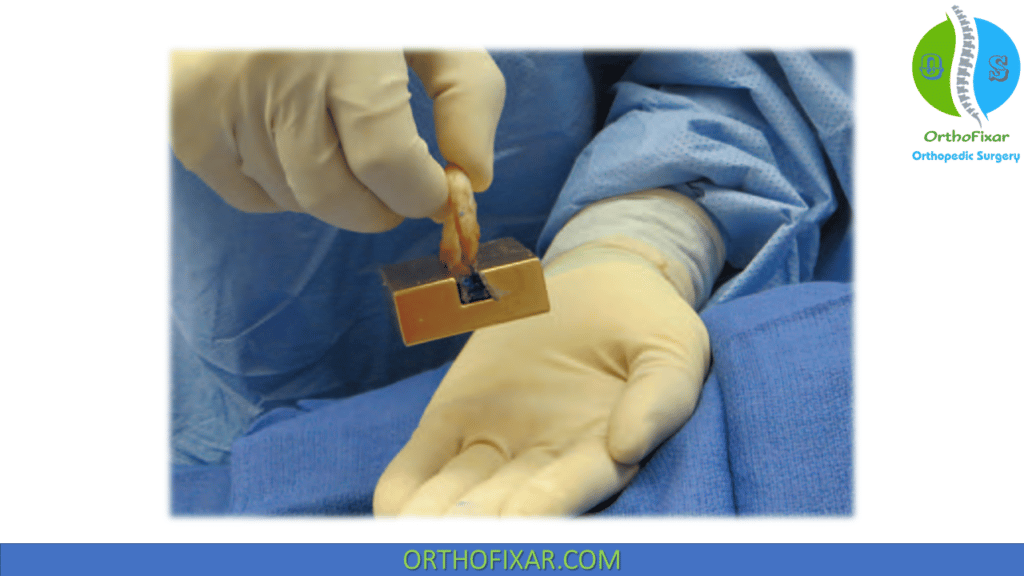
Meniscus Implant
The reduction suture is passed out through the posterolateral incision for application of gentle traction once the graft is inserted into the tibial channel. If needed, a bone tamp can be used to gently push the bone block further into the knee until contact with the posterior wall of the tibia.
At this point, the anterior arthrotomy is closed to prevent fluid extravasation, and the rest of the meniscus sutured. Various techniques can be used, but the surgeon’s preference for repairing a bucket handle meniscus tear is common. If only all-inside technique is used, special attention needs to be made to ensure that the graft is not extruded outward when tightening the fixation device. All-inside sutures will be used at the most posterior aspect if additional fixation near the root is needed. Absorbable and nonabsorbable sutures can be used, as second-look arthroscopies have shown that healing of the graft has not been a common problem. Usually, 8 to 10 sutures are required to completely secure the graft.

Medial: Double Bone Plug Technique
Recipient Bed Preparation
An ACL guide set at 60 degrees is used to place a guide pin into the anatomic posterior horn insertion of the old meniscus. A steep angle is selected to assist in reducing the plug, similar in reason to the tibial tunnel during posterior cruciate ligament surgery. The tibial tunnel is then drilled to a diameter of 7 mm, with the 1-mm difference allowing easy placement of the bone plug.
A shuttle suture is passed up the tibial tunnel, retrieved, and brought out of the knee. Although the suture can be removed through the scope portal, the author has found it easy to make the anterior arthrotomy prior to bringing the suture out. Often, soft tissue can be entrapped between the suture and a subsequent arthrotomy incision, which may impede bringing the graft into the knee. A posteromedial incision is then made and dissected down to the capsule in the same manner as one would for a medial meniscus repair using inside-out sutures.
Allograft Preparation
Initial graft preparation is similar to that of the lateral side, with any remaining capsular tissue attached to the meniscus removed to ensure complete visualization of the horn attachments. They are then marked for size and planned orientation. Typically, an 8-mm coring reamer will encompass the horn attachment. The posterior bone plug is performed first, with a 0.062-in K-wire passed to enter the center of the attachment at a roughly a 60-degree angle to mimic the angle of the tibial tunnel.
A collared pin is placed into the pilot hole, and the 8-mm coring reamer is used to create a bone plug. The bone plug end is then trimmed to be 6 mm in diameter and 8 mm in length. The size has been found to sufficiently secure the attachment but not be too large to impede reduction of the plug. Although a 6-mm coring reamer can be used, the author has found it easier to use the slightly larger corer to ensure fully encompassing the attachment and that it is less likely to damage the plug during harvest.
The anterior horn is obtained in a similar fashion, but the plug is maintained at an 8-mm diameter and 10-mm length because reduction is not difficult. To insert and secure the posterior bone plug, a 2-0 nonabsorbable suture is passed up through the bone plug, sutured through the meniscal horn attachment, and brought back down the plug.
It is imperative to include the edge of the meniscus during the suturing to add additional strength to the suture because the bone plug can be disrupted if pulled forcefully by itself. The anterior bone plug can be secured using the same suturing technique or placed in press-fit means, which are described later. As with the dovetail technique, a polydioxanone suture is placed through the meniscus to function as a reduction suture.

Meniscus Implant
The meniscus reduction sutures are passed into the knee and retrieved through the posteromedial incision using open-ended needles and inside-out technique. The posterior bone plug suture is placed through the tibial tunnel suture and subsequently brings the bone plug suture out the tibial tunnel entrance.
The surgeon applies gently on the bone plug suture and uses his or her index finger to carefully reduce the plug and bring the meniscus into the knee. At the same time, an assistant uses light tension on the reduction suture to help bring the meniscus into the knee, which also prevents the graft from flipping over.
Although the anterior plug can be placed right after the posterior plug, it is preferred to place a posterior then medial suture for initial fixation before securing the anterior horn. For example, if the anterior plug is secured first and the placement is incorrect, the difference needs to be made when suturing the remaining meniscus. It can thus result in a graft that is extruded outward or one in which there may be excess tension on the repair.
If the preliminary fixation is done posterior then middle, it is much easier to make adjustments for the anterior bone plug placement. Once the anterior bone plug site is determined, a guide pin is placed and overreamed with an 8-mm drill to a depth of 1 cm. The anterior bone plug can be secured with a suture or can be press-fit.
Until experience is gained, it is wise to use a suture because ensuring a secure press-fit has a learning curve. If the graft is to be secured with a bone plug stitch, a small hole to accommodate a suture-passing device is made in the anterior tibia and the plug sutures brought down reducing the plug into the socket. The sutures from the 2 plugs are then tied to one another for fixation. With the press-fit method, the tibia socket is made 1 to 2 mm less deep, and a tamp is used to compress the plug into the socket.
The suture for the posterior plug is tied down at tibia opening once it has been reduced. The author has found that a simple, inexpensive polyethylene button serves just as well as a more expensive fixation device. Subsequent suturing of the meniscus is the same as previously described for the dovetail method.
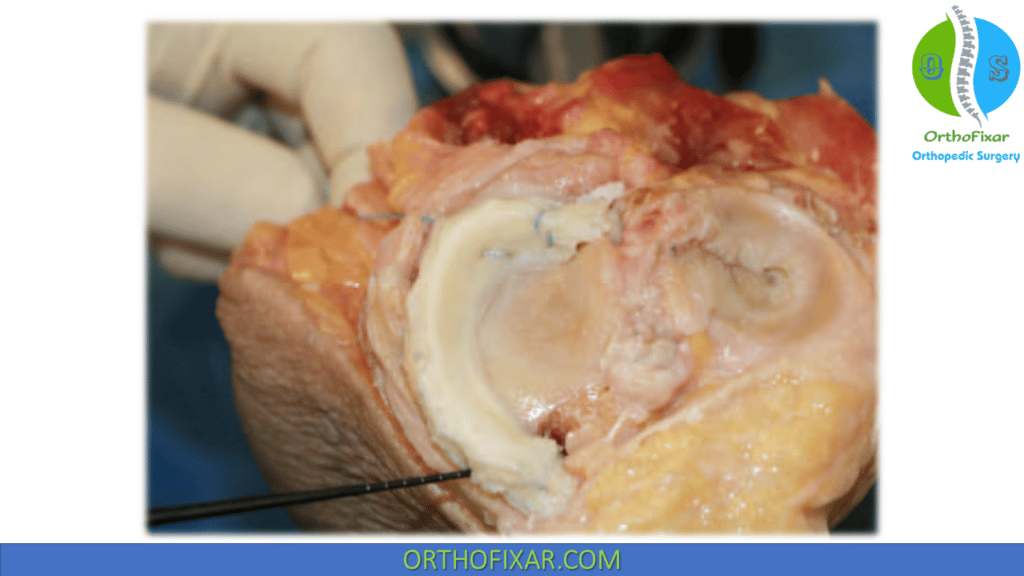
Postoperative Protocol
The initial postoperative care is to control pain, limit swelling, and obtain full extension. Weightbearing is limited for the initial 4 weeks. A postoperative ROM brace is worn during this period, with flexion limited to 90 degrees to minimize the meniscus translation and subsequent stress on the posterior repair.
At 4 weeks, patients are allowed full weightbearing and unrestricted ROM. Stationary biking with low resistance and straight leg swimming are also started at that time. Progressive, low-impact strengthening is implemented when the gait pattern has returned to normal. Most surgeons recommend waiting until 4 months to allow jogging, although the author has found no detriment if it is allowed as early as 12 weeks. Regardless of the time, patients with moderate arthritis are strongly discouraged to avoid high impact activities permanently.
From 4 to 6 months, leg strengthening is progressed as comfortable, with core and balance exercises stressed. Patients are released at 6 months if strength and endurance are comparable to the contralateral leg and agility testing is normal. Regardless of the degree of chondromalacia, patients’ expectations should not be to return to unlimited high-impact or contact sports.
References
- Renström P, Johnson RJ. Anatomy and biomechanics of the menisci. Clin Sports Med. 1990 Jul;9(3):523-38. PMID: 2199066.
- Baratz ME, Fu FH, Mengato R. Mensical tears: the effect of meniscectomy and of repair on intraarticular contact areas and stress in the human knee. A preliminary report. Am J Sports Med. 1986;14(4):270-275.
- Allen PR, Denham RA, Swan AV. Late degenerative changes after meniscectomy. Factors affecting the knee after operation. J Bone Joint Sur Br. 1984;66(5):666-671.
- Brophy RH, Matava MJ. Surgical options for meniscal replacement. J Am Acad Orthop Surg. 2012;20(5):265-272.
- Garrett JC. Meniscal transplantation: a review of 43 cases with two to seven year follow-up. Sports Med Arthrosc Rev. 1993;2:164-167.
- Cole BJ, Carter TR, Rodeo SA. Allograft meniscal transplantation: background, techniques, and results. Instr Course Lect. 2003;52:383-396.
- Abat F, Gelber PE, Erquicia JI, Pelfort X, Gonzalez-Lucena G, Monllau JC. Suture-only fixation technique leads to a higher degree of extrusion than bony fixation in meniscal allograft transplantation. Am J Sports Med. 2012;40(7):1591-1596.
- Berlet GC, Fowler PJ. The anterior horn of the medial meniscus. An anatomic study of its insertion. Am J Sports Med. 1998;26(4):540-543.
- Carter TR, Rabago M. Meniscal allograft transplantation: ten-year follow-up. Arthroscopy. 2012;28(suppl 1);e17-e18.
- LaPrade RF, Willis NJ, Spiridonov SI, Perkinson S. A prospective outcomes study of meniscal allograft transplantation. Am J Sports Med. 2010;38(9):1804-1812.
- Kim JG, Lee YS, Bae TS, et al. Tibiofemoral contact mechanics following posterior root of the medial meniscus tear, repair, meniscectomy, and allograft transplantation. Knee Surg Traumatol Arthrosc. 2013;21(9):2121-2125.
- Vundelinckx B, Vanlauwe J, Bellemans J. Long-term subjective, clinical, and radiographic outcome evaluation of meniscal allograft transplantation in the knee. Am J Sports Med. 2014;42(7):1592-1599.
- Harris JD, Cavo M, Brophy R, Siston R, Flanigan D. Biological knee reconstruction: a systematic review of combined meniscal allograft transplantation and cartilage repair or restoration. Arthroscopy. 2011;27(3):409-418.
- Noyes FR, Barber-Westin SD, Rankin M. Meniscal transplantation in symptomatic patients less than fifty years old. J Bone Joint Surg Am. 2004;86(7):1392-1404.
- Huang A, Hull ML, Howell SM. The level of compressive load affects conclusions from statistical analyses to determine whether a lateral meniscus allograft restores tibial contact pressure to normal: a study in human cadaveric knees. J Orthop Res. 2003;21(3):459-464.
- Pollard ME, Kang Q, Berg EE. Radiographic sizing for meniscal transplantation. Arthroscopy. 1995;11(6):684-687.
- Yoon YR, Kim TS, Lim HC, Lim HT, Yang JH. Is radiographic measurement of bony landmarks reliable for lateral meniscal sizing? Am J Sports Med. 2011;39(3):582-589.
- McDermott ID, Sharifi F, Bull AM, Gupte CM, Thomas RW, Amis AA. An anatomical study of meniscal allograft sizing. Knee Surg Sports Traumatol Arthrosc. 2004;12(2):130-135.
- Carter T, Economopoulos KJ. Meniscal allograft shrinkage—MRI evaluation. J Knee Surg. 2013;26(3):167-171.
- Rijk PC. Menisal allograft transplantation—part I: background, results, graft selection and preservation, and surgical considerations. Arthroscopy. 2004;20(7):728-743.
- Bursac P, York A, Kuznia P, Brown LM, Arnoczky SP. Influence of donor age on the biomechanical and biochemical properties of human meniscal allografts. Am J Sports Med. 2009;37(5):884-889.
- Choi NH, Yoo SY, Victoroff BN. Position of the bony bridge of lateral meniscal transplants can affect meniscal extrusion. Am J Sports Med. 2011;39(9):1955-1959.
- Hutchinson ID, Moran CJ, Potter HG, Warren RF, Rodeo SA. Restoration of the meniscus: form and function. Am J Sports Med. 2014;42(4):987-998.
- Wirth CJ, Peters G, Milachowski KA, Weismeier KG, Kohn D. Long-term results of meniscal allograft transplantation. Am J Sports Med. 2002;30(2):174-181.
- Elattar M, Dhollander A, Verdonk R, Almqvist KF, Verdonk P. Twenty-six years of meniscal allograft transplantation: is it still experimental? A meta-analysis of 44 trials. Knee Surg Sports Traumatol Arthrosc. 2011;19(12):147-157.
- Matava MJ. Meniscal allograft transplantation: a systematic review. Clin Orthop Relat Res. 2007;(455):142-157.
- Verdonk PC, Demurie A, Almqvist KF, Veys EM, Verbruggen G, Verdonk R. Transplantation of viable meniscal allograft. Survivorship analysis and clinical outcome of one hundred cases. J Bone Joint Surg Am. 2005;87(4):715-724