Fresh osteochondral allograft transplantation is a technique that has been successfully used for primary treatment of a wide spectrum of articular injuries and joint diseases as well as for the salvage of failed cartilage repair. For the surgeon, use of fresh Osteochondral Allograft provides an opportunity to achieve durable biological joint restoration. For the patient, this procedure provides predictable symptomatic relief and lasting functional improvement with the possibility of delaying or eliminating the need for arthroplasty.
Osteochondral Allograft Transplantation Indications
Diagnosis
In general, conditions of the knee indicated for treatment with fresh Osteochondral Allograft include large chondral and osteochondral lesions secondary to the following:
- Osteochondritis dissecans
- Focal avascular necrosis
- Other conditions involving cartilage disease or absence of subchondral bone (ie, fracture malunion)
- Failed cartilage repair procedures (ie, microfracture, osteochondral autologous transfer, autologous chondrocyte implantation)
- Degenerative knee conditions (select cases) in which arthroplasty is relatively contraindicated
Lesion size and location
- Primary management of chondral or osteochondral defects (≤ 2 cm2)
- Larger/deeper lesions of the femoral condyles (> 2 cm2 to ≤ 10, 6 to 10 mm deep) for which other techniques may be less effective, contraindicated, and/or limited by availability of donor tissue
- Tibial chondral defects
- Entire tibial and meniscal surface may be transplanted
- Bipolar (ie, “kissing”) lesions of the femur and tibia
- Relatively indicated when secondary changes occur on the nontraumatized side of the lesion
- Less successful than treatment of unipolar cartilage defects
Salvage
- Management of clinical failure of primary Osteochondral Allograft transplantation
- Success rates comparable to primary allografting
See Also: Osteochondritis Dissecans
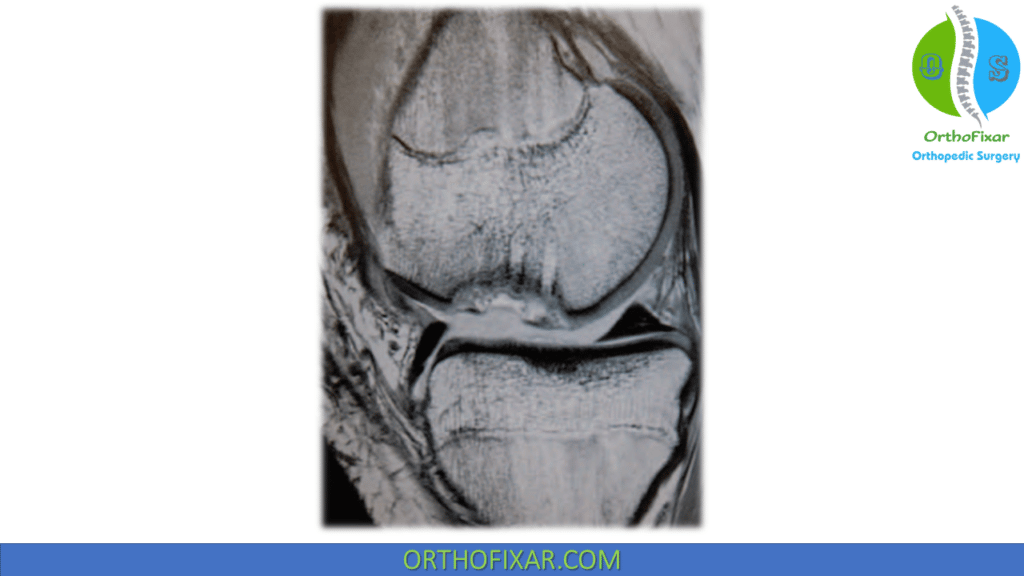
Relative Contraindications
- Age
- No absolute age limitations
- Inferior outcomes have been reported in older patients (ie, age > 40 years)
- Comorbid conditions
- Uncorrected joint malalignment and/or ligamentous instability
- Meniscal insufficiency
- Inflammatory arthropathy
- Diffuse degenerative arthrosis
- Morbid obesity, body mass index (BMI) > 30 kg/m
Osteochondral Allograft Transplantation Procedure
Equipment
The equipment required depends on the surface to be grafted and the surgical technique used. For most contained defects of the femoral condyles, a press-fit technique can be performed using commercially available systems (Arthrex) that simplifies site preparation, donor harvesting, and graft insertion. However, if the size or location of the lesion does not permit use of a dowel-type press-fit system, the surgeon should be prepared to perform the shell graft technique.
Because shell grafts require measured resection and sculpting of bone and cartilage, additional surgical equipment on hand should include calipers, depth-gauge, high-speed burr, reciprocating and oscillating saws, bone files, and/or rasps. In addition, use of fluoroscopy is critical for the treatment of certain large knee defects (ie, tibial plateau) and may enhance accuracy when treating other anatomic locations as well.
For either technique, the allograft is opened and inspected prior to surgical incision to ensure it is acceptable for implantation. Although most grafts can be pressfit without fixation, multiple options for graft fixation should be available, including bioabsorbable pins and/or low-profile interfragmentary screws 3 mm in diameter or less.
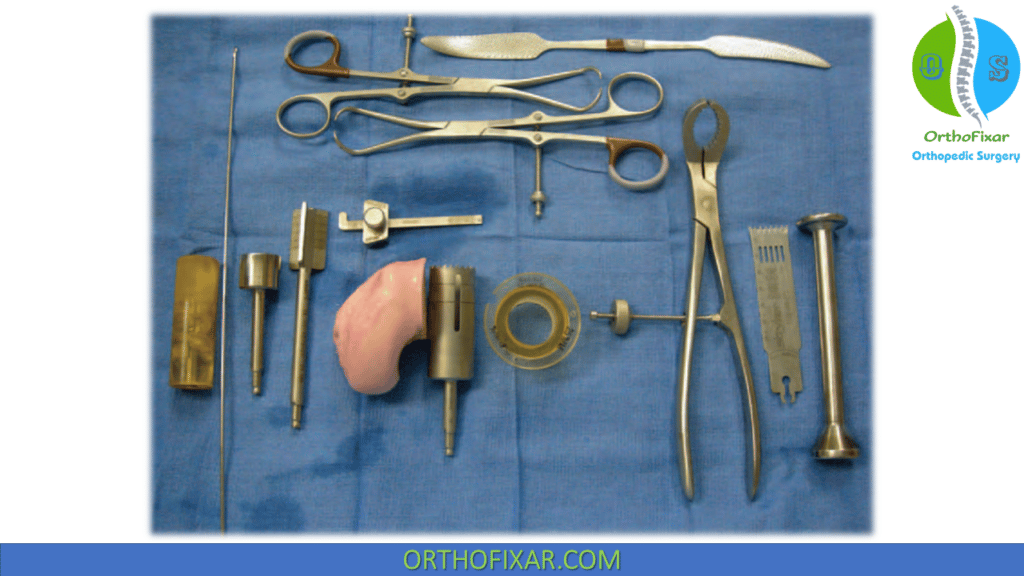
Positioning and Portals
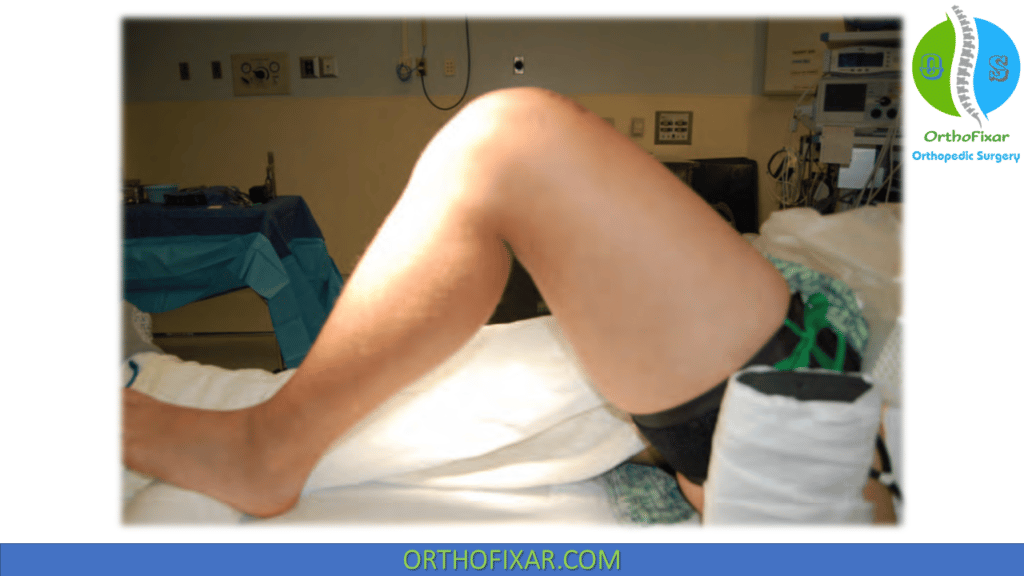
The patient is positioned supine with a proximal thigh tourniquet. A leg or foot holder helps to position and maintain the knee in flexion between 70 and 110 degrees. Prophylactic antibiotics are administered at the induction of anesthesia. The operative extremity is prepared and draped to permit an anterior approach to the knee.
Old incision sites are marked. If an osteotomy is planned, it may be advantageous to have access to the ipsilateral anterior superior iliac spine as a source of autograft bone and as a reference to evaluate alignment. A diagnostic arthroscopy may be performed before the Osteochondral Allograft transplantation to confirm lesion size and/or to treat coexisting pathology.
See Also: Elbow Osteochondritis Dissecans
Description of the Procedure
Management of Concomitant Pathology
For cartilage defects of the knee, if malalignment is present, realignment osteotomy is required to decrease the load on the graft. In general, opening wedge high tibial osteotomy is used to correct varus malalignment, and opening wedge lateral distal femoral osteotomy is used to correct valgus deformity.
For the patellofemoral joint, optimization of patellofemoral biomechanics may result in better outcomes, although this has not been proven in the context of osteochondral allografting. Therefore, in the setting of a patellofemoral lesion, tibial tubercle anteriorization or anteromedialization may be performed to transfer load and/or correct maltracking.
Management of ligament and meniscal deficiency is critical to normalization of compartment contact stresses and shear forces. Ligament reconstruction and/or meniscal allograft transplantation may be performed concomitantly with osteochondral transplantation to optimize graft survival and improve clinical outcome.
Surgical Exposure
A standard midline incision is made. Depending on lesion location, a medial or lateral arthrotomy may be used. Once the joint capsule has been incised and the retractors have been placed, the knee is brought into the degree of flexion that presents the lesion into the arthrotomy site.
In some cases, when the lesion is posterior, detachment and reflection of the meniscus may aid exposure. Angled retractors are placed medially and laterally to expose the condyle. A carefully placed retractor into the notch is useful to aid in patellar retraction. Extension of the deep incision proximally and distally aids in patellar mobilization.

Lesion Inspection and Preparation
The articular lesion is inspected to define the margins. Surrounding damaged cartilage and bone is debrided to facilitate accurate sizing of the lesion. The lesion is assessed to determine the allograft shape that will best match the defect. The 2 techniques for Osteochondral Allograft preparation include the press-fit circular plug technique and the shell graft technique.
Whenever possible, the press-fit technique is preferred based on the relative ease in achieving a precise graft fit and the low likelihood for need of supplemental internal fixation. If the lesion is not amenable to a press-fit Osteochondral Allograft , a shell graft may be used.
Dowel or Plug Technique
The size of the Osteochondral Allograft is estimated using the commercially available cannulated, cylindrical sizing guides. Each guide is positioned to encompass the defect and thereby determine the optimal plug diameter. The guide must sit flush with the surrounding normal cartilage to properly restore the geometry of the articular surface. If the lesion is between 2 sizes, begin with the smaller size.
Once a size has been determined, ensure that the available graft can accommodate the harvesting of this size graft as anatomic differences can occur that may change the surgical plan (ie, the surgeon may choose to place two 20-mm grafts rather than one 30-mm graft if the allograft condyle is too narrow to harvest a 30-mm diameter graft). Recipient site preparation begins with placement of a guide wire through the cylindrical sizing guide into the center of the lesion, perpendicular to the articular surface.
The cartilage surface is scored, and a cannulated counter bore reamer is used to remove the articular cartilage and 3 to 4 mm of subchondral bone. In deeper lesions, the pathologic bone is removed until there is healthy, bleeding bone. Generally, for treatment of chondral defects, depth does not exceed 6 to 8 mm. For treatment of osteochondral lesions, depth may reach up to 10 mm. The reamings are collected and may be used to graft osseous defects (cysts) or to optimize the position of the graft. At this point, the guide pin can be removed.
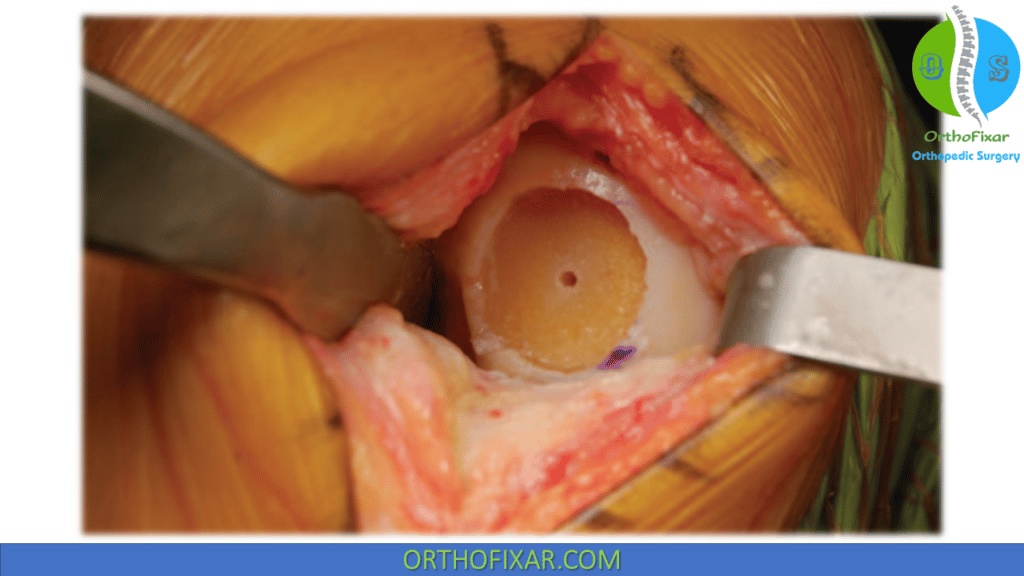
If necessary, multiple perforations can be made in the base of the defect using a K-wire to promote vascular inflow. A skin marker is used to mark the 12 o’clock position for reference, and depth measurements are made and recorded in the 4 quadrants of the recipient site. A ruler or depth gauge is used to measure and record the socket depth at the 3, 6, 9, and 12 o’clock positions. The recipient socket is now complete and ready for the press-fit Osteochondral Allograft .
The corresponding anatomic location of the recipient site is identified on the donor allograft. The allograft is then secured to the allograft workstation platform or held with clamps and positioned such that the appropriate diameter bushing may be positioned perpendicular to the articular surface, matching the orientation used to create the recipient site. The cylindrical sizing tube is used to confirm that the selected angle will match the contour of the defect, and the 12 o’clock position is marked with a surgical marker.
The appropriate size-coring reamer is passed through the bushing and advanced through the entire depth. Once harvested from the donor condyle, the graft is removed as a long cylindrical plug. An oscillating saw can be used to release the graft from the donor condyle.
The depths for the 4 quadrants of the recipient site are transferred to the graft, and the allograft plug thickness is customized using a microsagittal saw to trim excess bone to the thickness matching the recipient site. Just before insertion, it is beneficial to bevel the edges of the osseous portion with a small rongeur or rasp to facilitate the initial press-fit into the recipient socket.
The donor graft should be irrigated copiously with a pulsatile lavage to remove blood and marrow cells to decrease the risk of a host immune response. The donor graft is positioned by aligning the markings and is pressed into place by hand. If the graft does not fit, dilating the recipient site with a slightly oversized tamp or reinserting the guide wire and reaming deeper may be considered or the graft can be further trimmed or beveled.
The final resting position of the graft should be flush relative to the surrounding articular surface, although the authors accept stepoffs of less than 1 mm. If the graft is unstable or has an exposed edge, absorbable pins or biocompression screws are used. For large femoral defects, more than 1 press-fit Osteochondral Allograft plug may be required.
The “snowman technique” facilitates coverage of a greater condylar area using a second press-fit plug. In this technique, the first graft is secured with a small K-wire or, if necessary, definitively fixed with biocompression screws to prevent dislodgement during preparation of the second overlapping site.
Care is taken to minimize space between multiple grafts as this may lead to formation of biomechanically inferior fibrocartilage and/or lack of articular congruity (ie, cobble stoning) which may alter biomechanics and negatively affect clinical outcome.
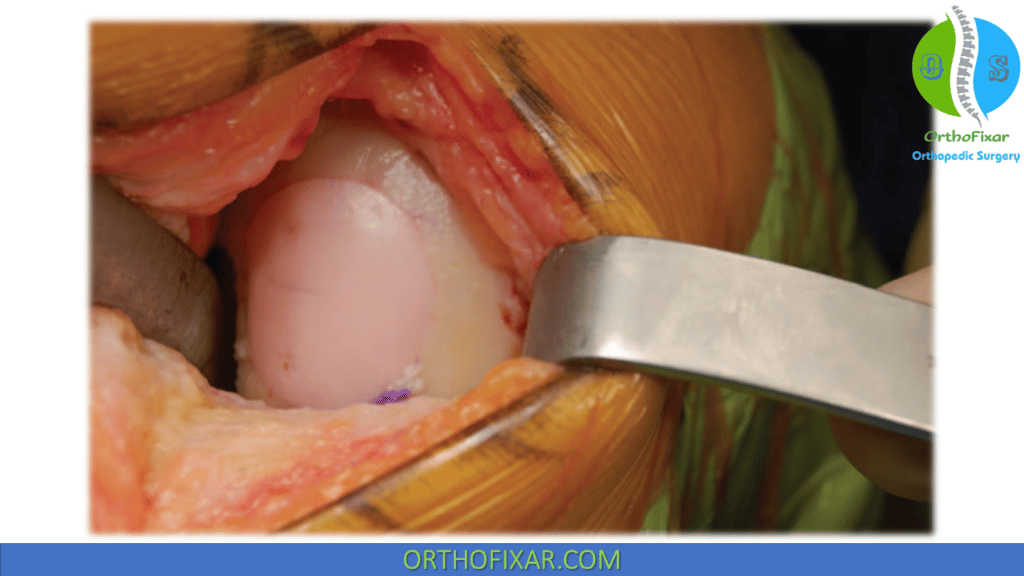
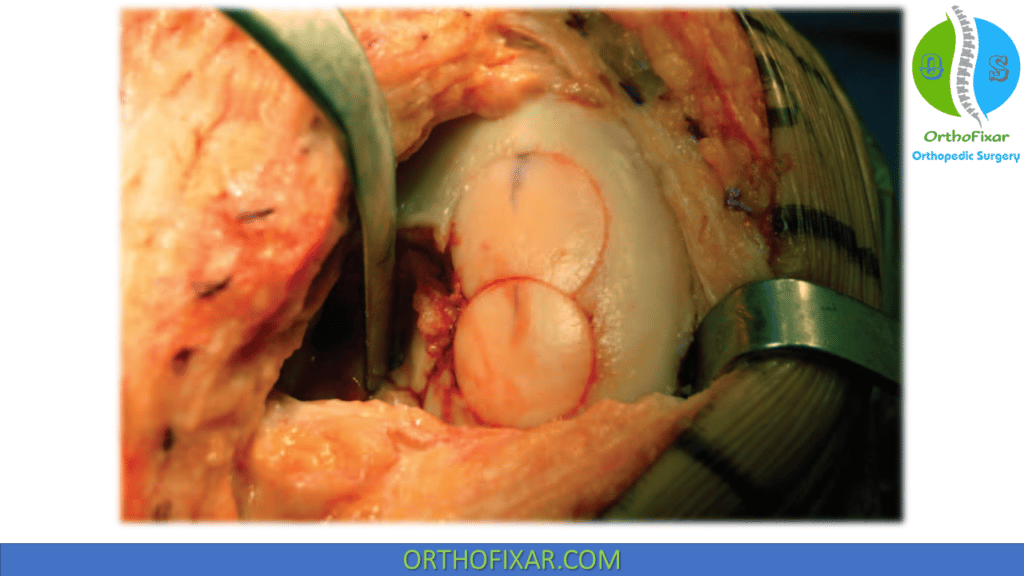
Shell Technique
For uncontained or asymmetric lesions or for lesions in locations that are difficult to access on the femur, a free-hand technique is required to match donor tissue to the recipient defect. A skin marker is used to outline the shape of the defect, and a 15-blade scalpel is used to incise the remaining cartilage, which is then removed using sharp curettes. A high-speed burr is then used to remove the underlying pathologic bone to expose healthy bleeding bone.
Creation of a simple recipient site geometry (ie, rectangle or trapezoid) simplifies subsequent freehand sizing of the Osteochondral Allograft . After the recipient site is prepared, the donor graft is roughly fashioned with a microsagittal saw. It is best to make the initial cuts slightly wider than measured to oversize the donor graft. A series of trial fittings and repeated measurement guide sculpting of the donor tissue to achieve a precise fit.
For the patella, although smaller lesions may be successfully managed with press-fit circular grafts, larger lesions are managed with a technique similar to that used in total knee arthroplasty. Patellar thickness is measured with calipers and resection of the articular surface is performed, maintaining at least 12 mm of residual bone. The donor graft is then resected in a similar fashion.
The allograft is then lavaged and seated in the appropriate position. The graft is then secured with interfragmentary screw fixation from the anterior surface of the patella into the subchondral bone beneath the median ridge of the graft. Afterward, an assessment of patellar tracking will determine the need for any additional soft tissue or bony realignment procedures.
Large post-traumatic tibial plateau lesions are managed with a technique similar to that used in unicompartmental knee arthroplasty. Under fluoroscopic guidance, en bloc resection of the meniscotibial unit with an “L-cut” is performed. Two freehand cuts are made to resect a minimal amount of subchondral bone. K-wires or arthroplasty jigs may be used to assist the surgeon with these cuts.
Measurements of the length and width of the resected surface and the joint space gap allow estimation of the required allograft dimensions. Next, the donor graft is secured in the graft holder, and the desired dimensions are marked. Ideally, tibial plateau grafts are 8 to 12 mm thick, which is typical for restoring plateau height after fracture malunion. A reciprocating saw is used to make the vertical cut, and an oscillating saw is used to make the horizontal cut referencing off the marks placed on the graft margins. Once sculpted to the optimal size and shape, the graft is lavaged and carefully inserted in the anatomic position adjacent to the femoral condyle.
The knee is taken through a ROM, and the graft is inspected visually and under fluoroscopy to assess graft position and restoration of the joint line and tibial slope. Revisions are made as necessary to optimize graft fit and position as well as overall joint alignment and mechanics. The graft is then fixed with 2 interfragmentary screws placed from the submeniscal articular margin at the midcoronal and anterior positions. After fixation of the bone, the meniscus is repaired in the standard fashion.
Postoperative Protocol
Phase I:
0 to 4 Weeks In the first phase of rehabilitation, patient goals are to control pain and swelling, restore muscle control, improve knee ROM, and protect the allograft. Patients are allowed unrestricted early nonweightbearing motion unless a concurrent procedure dictates otherwise. Weightbearing status varies based on lesion location, but the general goal is to avoid placing stress on the transplanted area. Patients with tibial or femoral grafts are restricted to toe-touch weightbearing for 6 weeks.
Patients with patellofemoral osteochondral allograft are permitted weightbearing as tolerated in extension but are limited to between 30 and 45 degrees of active flexion. In addition to passive- and active-assisted knee ROM, exercises include stretching and isometric strengthening of the quadriceps, hamstrings, and gluteus muscles. Although knee braces are not required, they may be useful for patients with patellofemoral grafts by limiting knee flexion to less than 45 degrees. For patients with bipolar knee lesions, an unloader brace may be useful as they progress to full weightbearing.
Phase II
4 to 12 Weeks In the second phase, patient goals are to regain full ROM, a normalized gait, and the ability to perform functional activities of daily life. Stretching and isometric strengthening exercises are continued as weightbearing is progressed. Typically, once the patient has adequate quadriceps control and can perform a straight leg raise without an extension lag, initiation of a stationary cycle is appropriate. Gait training and closed chain exercises are introduced. For focal lesion treated with a single plug osteochondral allograft, full weightbearing is generally allowed by 6 to 8 weeks. Patients with large or complex grafts are restricted to partial weightbearing for 8 to 12 weeks.
Phase III
12 to 18 Weeks The final phase of rehabilitation varies based on the goals and expectations of the patient. For the patient with a goal of performing activities of daily living, a transition is made to a maintenance home exercise program. Recreational sports are not reintroduced until joint rehabilitation is complete and radiographic healing has been demonstrated, which generally occurs no earlier than 4 to 6 months postoperatively.
In athletes, this phase focuses on advanced strengthening, core stabilization, proprioception, and gradual return to sport-specific training. At a minimum, athletes should demonstrate full knee ROM, no effusion, joint stability, excellent dynamic strength, and have clinical and radiographic evidence of complete graft incorporation before returning to the highest level of activity. Ideally, high-loading activities should be avoided until at least 6 to 12 months postoperatively.
References
- Heir S, Nerhus TK, Røtterud JH, Løken S, Ekeland A, Engebretsen L, Arøen A. Focal cartilage defects in the knee impair quality of life as much as severe osteoarthritis: a comparison of knee injury and osteoarthritis outcome score in 4 patient categories scheduled for knee surgery. Am J Sports Med. 2010 Feb;38(2):231-7. doi: 10.1177/0363546509352157. Epub 2009 Dec 30. PMID: 20042546.
- Moran CJ, Pascual-Garrido C, Chubinskaya S, et al. Restoration of articular cartilage. J Bone Joint Surg Am. 2014;96(4):336-344.
- Raz G, Safir OA, Backstein DJ, Lee PT, Gross AE. Distal femoral fresh osteochondral allografts: followup at a mean of twenty-two years. J Bone Joint Surg Am. 2014;96(13):1101-1107.
- Yu J, Bugbee WD. Osteochondral allograft transplantation. In: Williams RJ III, ed. Cartilage Repair Strategies. Totowa, NJ: Humana Press Inc; 2007:167-191.
- Horton MT, Pulido PA, McCauley JC, Bugbee WD. Revision osteochondral allograft transplantations: do they work? Am J Sports Med. 2013;41(11):2507-2511.
- Behery O, Siston RA, Harris JD, Flanigan DC. Treatment of cartilage defects of the knee: expanding on the existing algorithm. Clin J Sport Med. 2014;24(1):21-30.
- Sharma L, Dunlop DD, Cahue S, Song J, Hayes KW. Quadriceps strength and osteoarthritis progression in malaligned and lax knees. Ann Intern Med. 2003;138(8):613-619.
- Highgenboten CL, Jackson A, Aschliman M, Meske NB. The estimation of femoral condyle size. An important component in osteochondral allografts. Clin Orthop Relat Res. 1989;(246):225-233.
- Latterman C, Romine SE. Osteochondral allografts: state of the art. Clin Sports Med. 2009;28(2):281-301.
- Campbell AB, Knopp MV, Kolovich GP, et al. Preoperative MRI underestimates articular cartilage defect size compared with findings at arthroscopic knee surgery. Am J Sports Med. 2013;41(3):590-595.
- Mucha A, Dordevic M, Hirschmann A, et al. Effect of high tibial osteotomy on joint loading in symptomatic patients with varus aligned knees: a study using SPECT/CT [published online ahead of print May 11, 2014]. Knee Surg Sports Traumatol Arthrosc.
- Arthrex. Allograft OATS (Osteochondral Autograft Transfer System) Surgical Technique. Available at: http://jrfortho.org/images/prod-files/Allograft_OATS%C2%AE_(Osteochondral_Autograft_Transfer_ System).pdf. Accessed on July 30, 2015.
- Minzlaff P, Feucht MJ, Saier T, et al. Osteochondral autologous transfer combined with valgus high tibial osteotomy: long-term results and survivorship analysis. Am J Sports Med. 2013;41(10):2325-2332.
- Pascual-Garrido C, Slabaugh MA, L’Heureux DR, Friel NA, Cole BJ. Recommendations and treatment outcomes for patellofemoral articular cartilage defects with autologous chondrocyte implantation: prospective evaluation at average 4-year follow-up. Am J Sports Med. 2009;37(suppl 1):33S-41S.
- Harris JD, Cavo M, Brophy R, Siston R, Flanigan D. Biological knee reconstruction: a systematic review of combined meniscal allograft transplantation and cartilage repair or restoration. Arthroscopy. 2011;27(3):409-418.
- Hunt HE, Sadr K, Deyoung AJ, Gortz S, Bugbee WD. The role of immunologic response in fresh osteochondral allografting of the knee. Am J Sports Med. 2014;42(4):886-891.
- Koh JL, Wirsing K, Lautenschlager E, Zhang LO. The effect of graft height mismatch on contact pressure following osteochondral grafting: a biomechanical study. Am J Sports Med. 2004;32(2):317-320.
- Cole BJ, Pascual-Garrido C, Grumet RC. Surgical management of articular cartilage defects in the knee. Instr Course Lect. 2010;59:181-204.
- Krych AJ, Robertson CM, Williams RJ III; Cartilage Study Group. Return to athletic activity after osteochondral allograft transplantation in the knee. Am J Sports Med. 2012;40(5):1053-1059.
- Kainer MA, Linden JV, Whaley DN, et al. Clostridium infections associated with musculoskeletal-tissue allografts. N Engl J Med. 2004;350(25):2564-2571.
- American Association of Tissue Banks. Standards for tissue banking. Available at: http://www.aatb.org/. Accessed July 16, 2014.
- Centers for Disease Control and Prevention (CDC). Update: allograft-associated bacterial infections— United States, 2002. MMWR Morb Mortal Wkly Rep. 2002;51(10):207-210.
- Tugwell BD, Patel PR, Williams IT, et al. Transmission of hepatitis C virus to several organ and tissue recipients from an antibody-negative donor. Ann Intern Med. 2005;143(9):648-654.
- Ball ST, Amiel D, Williams SK, et al. The effects of storage on fresh human osteochondral allografts. Clin Orthop Relat Res. 2004;(418):246-252.
- Oakeshott RD, Farine I, Pritzker KP, Langer F, Gross AE. A clinical and histologic analysis of failed fresh osteochondral allografts. Clin Orthop Relat Res. 1988;(233):283-294