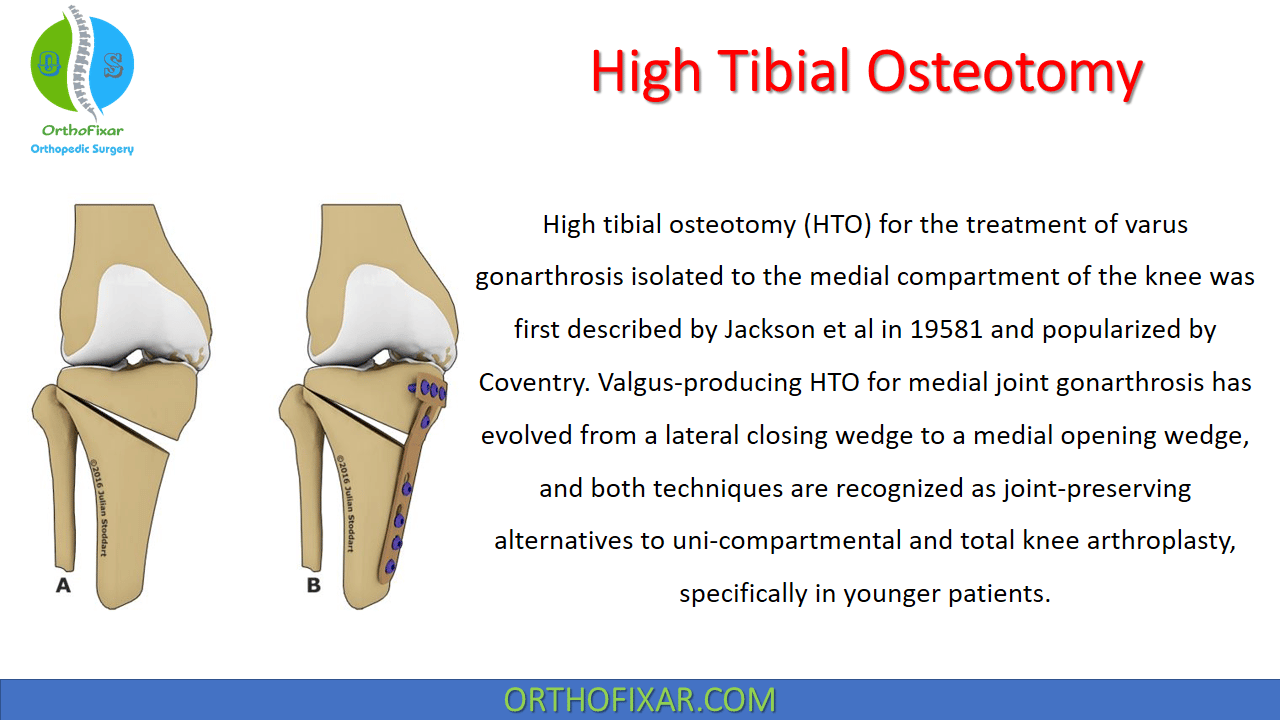
High tibial osteotomy (HTO) for the treatment of varus gonarthrosis isolated to the medial compartment of the knee was first described by Jackson et al in 19581 and popularized by Coventry. Valgus-producing HTO for medial joint gonarthrosis has evolved from a lateral closing wedge to a medial opening wedge, and both techniques are recognized as joint-preserving alternatives to uni-compartmental and total knee arthroplasty, specifically in younger patients.
Valgus-producing osteotomies to unload the medial compartment are typically performed with an HTO (medial opening wedge or lateral closing wedge), whereas varus producing-osteotomies to unload the lateral compartment are performed with a distal femoral osteotomy (DFO) (medial opening wedge or lateral closing wedge) or lateral opening wedge High Tibial Osteotomy HTO.
Osteotomies can also be used in the treatment of ligamentous instability in the setting of malalignment. Coronal plane realignment can be used to protect ligamentous reconstructions. In addition, altering the tibial slope on the sagittal plane can be performed to treat posterior (PCL) or anterior cruciate ligament (ACL) insufficiency. Corrections to the tibial slope can be performed with a direct anterior wedge osteotomy or through a medial or lateral wedge biplanar osteotomy (to address coronal and sagittal alignment)
High Tibial Osteotomy Indications
- Gonarthrosis isolated to the medial compartment with varus malalignment,
- Age younger than 60 years,
- Good range of motion (ROM),
- Ligamentous knee stability (but it is indicated in some ACL-/PCL-deficient patients),
- Associated with meniscal or osteochondral transplantation.
Controversial Indications
- Knee with significant motion loss,
- Inflammatory arthritis,
- Associated patellofemoral or low-grade contralateral compartment arthritis (compartment that the mechanical axis is shifting to needs to be relatively well preserved),
- Advanced age
- Obesity,
- Relative contraindications include smoking and diabetes mellitus given the increased rate of complications in these patient populations.
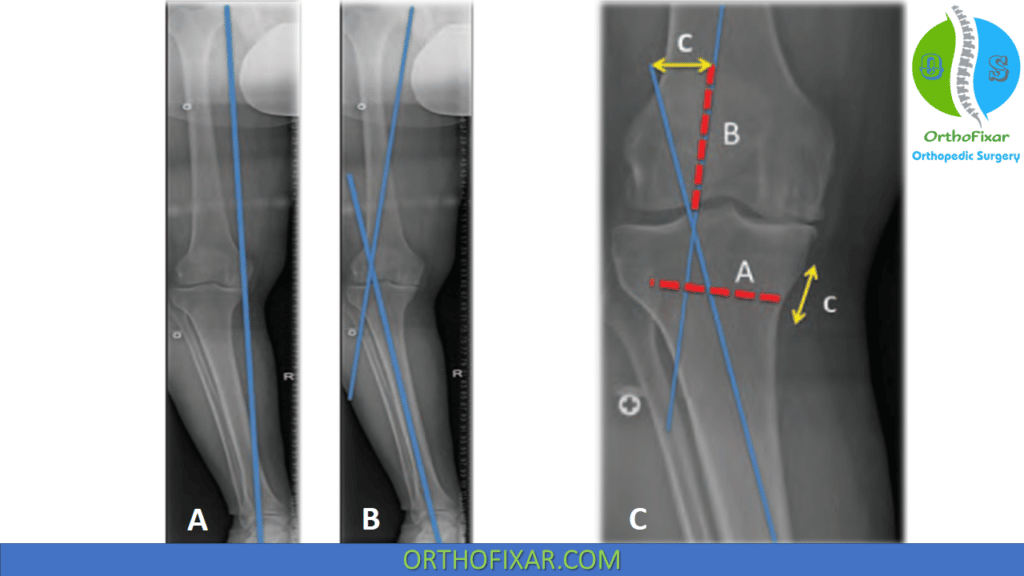
B: From the center of the hip, draw a line to the desired correction point in the lateral compartment and a line to that point from the center of the ankle.
C: Draw line A, which represents the osteotomy; this line stops 7 to 10 mm inside the lateral cortex of the tibia. Draw line B, which is identical in length to line A. Distance C represents the amount the osteotomy will need to be opened for the desired mechanical axis to be achieved.
High Tibial Osteotomy Surgery
Equipment
- Fluoroscopy
- Radiolucent operating room table
- Positioning bundle
- Large curved blunt Hohmann retractor for posterior retraction
- Narrow curved retractor for anterior retraction
- Calibrated pin (or break-away pins)
- Oscillating saw
- Wide and narrow flexible osteotomes
- Opening wedge
- Laminar spreader (optional)
- Plate fixation (TomoFix, Puddu plate, Contourlock, iBalance)
- Bone graft, synthetic or allograft (optional)

Positioning and Portals
The patient should be positioned supine on a radiolucent operating table. A tourniquet is applied to the thigh for intraoperative hemostasis. A sterile positioning bundle can be placed underneath the knee and leg during the osteotomy for optimum positioning during fluoroscopy. The same sterile positioning bundle can be placed under the heel to obtain knee extension prior to fixation. If knee arthroscopy is indicated, an arthroscopy setup can easily be added to the osteotomy setup.


Description of the Procedure
High Tibial Osteotomy starts with a well thought out preoperative plan, including calculating the desired correction in the coronal and sagittal planes as mentioned previously.
Medial Opening Tibial Wedge High Tibial Osteotomy
The surgical approach for a proximal Medial Opening Tibial Wedge high tibial osteotomy should respect future surgical approaches; for this reason, the medial longitudinal incision based midway between the tibial tubercle and the posteromedial border of the tibia is preferred.
See Also: Anterolateral Approach to Lateral Plateau
After dissection through skin and subcutaneous tissue, the first layer of fascia can be exposed using blunt dissection with a surgical sponge. The sartorius fascia is then incised just above and inline with the gracilis tendon and the pes anserine is released 1 cm off the tibial attachment. The surgeon will now have an excellent look at the MCL tibial attachment.
Using cautery, the PMC of the fascial attachment (popliteus) is elevated off the metaphyseal flare of the tibia posterior to the MCL for a length of 3 to 5 cm. Using a Cobb or a periosteal elevator, the soft tissue on the posterior aspect of the tibia can be gently elevated. During this step, be sure to direct the instrument toward the posterior cortex of the tibia.
Next, a blunt-tipped Hohmann retractor is placed across the tibia, feeling bone on the tip of the instrument as it is inserted. This instrument will be in direct line with the proposed osteotomy. The tibial tubercle is then identified, as is the medial border of the patellar tendon in the proximal aspect of the wound. Open the fascia longitudinally medial to the tendon to facilitate insertion of a blunt retractor (bent Lane or Hohmann) beneath the tendon. A small release of 5 mm or so of the medial aspect of the tendon insertion on the tubercle will enhance the view.
The C-arm is then brought into the surgical field to guide insertion of a break-away pin at the upper margin of where the surgeon plans to cut the tibia. At this stage, the tibial width is measured using the calibrated pin. Use a wide osteotome to plan the plane of the cut to pass just on the top of the tibial tubercle. In the sagittal plane, the cut can follow the tibial slope; therefore, angling back 10 degrees or so will give the surgeon more proximal bone for subsequent screw fixation.
Once the plane of the cut is chosen, use the osteotome as a cutting guide and mark the cut line with electrocautery. The MCL is not elevated but is cut through horizontally in the line of the osteotomy; if the surgeon prefers, the MCL can be elevated and allowed to fall back over the osteotomy at the end of the procedure. A small oscillating saw blade is chosen (45 mm long), and the cut is made staying perfectly inline and below the guide pin.
Commit to the plane of the cut, especially anterior to the pin, so that the surgeon does not wander more proximally toward the joint than desired. Once the initial cut is made with the saw, thin osteotomes can be used. Keep a 10-mm bridge of bone on the lateral side and use the C-arm to follow each step. During cutting, the retractors should remain in the same plane as the saw or osteotome for safety.
Once the surgeon feels he has completed the desired cut, a wide, firm osteotome can be inserted, and mobility of the osteotomy can be assessed by gently levering on this instrument. Usually, if minimal movement is noted, the posterior cortex needs to be cut a little further.
To open the osteotomy, you can use stacked osteotomes or wedges to open to the desired amount. Gauge the amount of opening off the posteromedial aspect of the osteotomy; to keep the slope neutral, do not use a wedge more anteriorly because this will open the front and increase the slope (this can be desirable in cases of PCL insufficiency but not in cases of ACL insufficiency or medial arthrosis).
It is important to try to maintain the integrity of the lateral column of bone to prevent translation and maintain stability. The tip of the osteotomy on the lateral side should always be closer to the lateral cortex than to the lateral joint line; this will avoid intra-articular fractures. Once the osteotomy is complete and is held open with a wedge or laminar spreader to the desired amount, one can then apply hardware to maintain the correction.
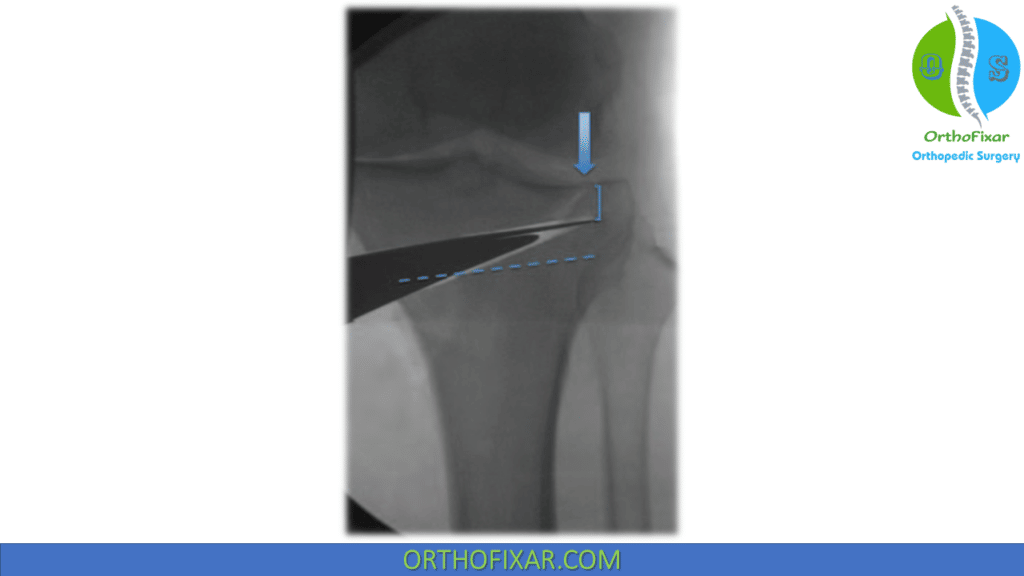
A locking plate is preferred to maintain axial and rotational stability during the consolidation period. The plate is placed on top of the fascial layer using spacer screws to hold the plate slightly off the bone. While inserting screws using the C-arm to confirm safe positioning, one can usually place 4 locking screws proximal and distal to the osteotomy with proper plate position.
Check the lateral fluoroscopic view to ensure that screws are not extending beyond the posterior cortex. After one is satisfied with the fixation, one may consider filling the defect with bone graft or a bone graft substitute. No graft is used for smaller corrections. The wound is closed over a oneeighth-in suction drain that is removed the following day. One may choose an icing sleeve and/or a hinged knee brace for added comfort.

Postoperative Protocol
Patients are kept overnight in most situations, although with healthy younger patients with good perioperative pain management, one can consider outpatient surgery. Prophylactic antibiotics and anticoagulation can be given per the surgeon’s preference. The brace is locked at 0 degrees overnight then unlocked after a dressing change and drain removal the following morning. The brace is set at 0 to 90 degrees.
During the first 2 weeks, the patient is on crutches and is feather-touch weightbearing. The patient is reassessed for wound healing at this stage and is then allowed to put as much weight as tolerated through the operative leg so long as no complications with the fixation are noted on x-rays. In general, it takes another 3 or 4 weeks of crutch usage before patients can walk without aids. The brace is removed for therapy, and full ROM and isometric quadriceps and hamstring exercises are encouraged.
The use of a stationary bike without resistance and water therapy are allowed when the wound is well healed. After 6 weeks, the brace is discontinued, and progressive closed chain strengthening is used. Patients are followed routinely at 2, 6, 12, 26, and 52 weeks. It is not uncommon for the osteotomy to take a full 6 months to unite and 1 year to remodel.
References
- Jackson JP, Waugh W, Green JP. High tibial osteotomy for osteoarthritis of the knee. J Bone Joint Surg Br. 1969 Feb 1;51(1):88-94. PMID: 5766363.
- Coventry MB. Osteotomy of the upper portion of the tibia for degenerative arthritis of the knee. A preliminary report. J Bone Joint Surg Am. 1965;47:984-990
- Smith TO, Sexton D, Mitchell P, Hing CB. Opening- or closing-wedged high tibial osteotomy: a metaanalysis of clinical and radiological outcomes. Knee. 2011;18(6):361-368.
- Hoell S, Suttmoeller J, Stoll V, Fuchs S, Gosheger G. The high tibial osteotomy, open versus closed wedge, a comparison of methods in 108 patients. Arch Orthop Trauma Surg. 2005;125(9):638-643.
- Amendola A, Bonasia DE. Results of high tibial osteotomy: review of the literature. Int Orthop. 2010;34(2):155-160.
- Floerkemeier S, Staubli AE, Schroeter S, Goldhahn S, Lobenhoffer P. Outcome after high tibial openwedge osteotomy: a retrospective evaluation of 533 patients. Knee Surg Sports Traumatol Arthrosc. 2013;21(1):170-180.
- Puddu G, Cipolla M, Cerullo G, Franco V, Gianni E. Osteotomies: the surgical treatment of the valgus knee. Sports Med Arthrosc. 2007;15(1):15-22.
- Noyes FR, Barber SD, Simon R. High tibial osteotomy and ligament reconstruction in varus angulated, anterior cruciate ligament-deficient knees. A two- to seven-year follow-up study. Am J Sports Med. 1993;21(1):2-12.
- Noyes FR, Barber-Westin SD, Hewett TE. High tibial osteotomy and ligament reconstruction for varus angulated anterior cruciate ligament-deficient knees. Am J Sports Med. 2000;28(3):282-296.
- Dejour H, Neyret P, Boileau P, Donell ST. Anterior cruciate reconstruction combined with valgus tibial osteotomy. Clin Orthop Relat Res. 1994;(299):220-228.
- Trojani C, Elhor H, Carles M, Boileau P. Anterior cruciate ligament reconstruction combined with valgus high tibial osteotomy allows return to sports. Orthop Traumatol Surg Res. 2014;100(2):209-212.
- Giffin JR, Shannon FJ. The role of the high tibial osteotomy in the unstable knee. Sports Med Arthrosc. 2007;15(1):23-31.
- McNamara I, Birmingham TB, Fowler PJ, Giffin JR. High tibial osteotomy: evolution of research and clinical applications—a Canadian experience. Knee Surg Sports Traumatol Arthrosc. 2013;21(1):23-31.
- Rossi R, Bonasia DE, Amendola A. The role of high tibial osteotomy in the varus knee. J Am Acad Orthop Surg. 2011;19(10):590-599.
- Collins B, Getgood A, Alomar AZ, et al. A case series of lateral opening wedge high tibial osteotomy for valgus malalignment. Knee Surg Sports Traumatol Arthrosc. 2013;21(1):152-160.
- Dugdale TW, Noyes FR, Styer D. Preoperative planning for high tibial osteotomy. The effect of lateral tibiofemoral separation and tibiofemoral length. Clin Orthop Relat Res. 1992;(274):248-264.
- Fujisawa Y, Masuhara K, Shiomi S. The effect of high tibial osteotomy on osteoarthritis of the knee. An arthroscopic study of 54 knee joints. Orthop Clin North Am. 1979;10(3):585-608.
- Amis AA. Biomechanics of high tibial osteotomy. Knee Surg Sports Traumatol Arthrosc. 2013;21(1):197-205.
- Martin R, Birmingham TB, Willits K, Litchfield R, Lebel ME, Giffin JR. Adverse event rates and classifications in medial opening wedge high tibial osteotomy. Am J Sports Med. 2014;42(5):1118-1126.