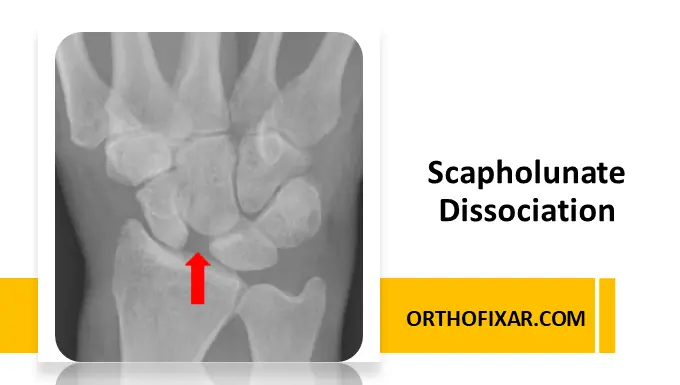
Scapholunate dissociation (SLD) is the most common and clinically significant ligament injury of the wrist. Often described as the ligamentous equivalent of a scaphoid fracture, it represents a critical disruption in carpal stability that can lead to long-term disability if not properly managed.
What Is Scapholunate Dissociation?
Scapholunate dissociation is a form of carpal instability caused by injury to the scapholunate ligament complex, particularly:
- The radioscapholunate ligament
- The dorsal scapholunate interosseous ligament (most important stabilizer)
This injury disrupts the normal relationship between the scaphoid and lunate bones, leading to abnormal motion and eventual degeneration.
See Also: Wrist Anatomy
Epidemiology and Importance
- The Scapholunate Dissociation is the most common ligamentous injury of the wrist
- Frequently missed in acute trauma settings
- Strongly associated with chronic wrist instability and arthritis
Untreated cases may progress to Scapholunate Advanced Collapse, a debilitating degenerative condition.
Mechanism of Injury
The classic mechanism of scapholunate dissociation involves:
- Forceful loading of the extended wrist
- Combined with ulnar deviation
This mechanism commonly occurs in:
- Falls on an outstretched hand (FOOSH)
- Sports injuries
- Motor vehicle accidents
Clinical Presentation
Symptoms
Patients typically present with:
- Wrist pain (especially dorsal and radial side)
- Weak grip strength
- Pain during activities requiring forceful grasp
Physical Examination Findings
- Localized tenderness over the scapholunate interval
- Ecchymosis around the wrist
- Prominent dorsal scaphoid (in some cases)
Key Clinical Signs:
- Pain with vigorous grip
- Decreased repetitive grip strength
- Painful wrist flexion–extension
- Pain during radial–ulnar deviation
Special Test
Radiographic Evaluation
Proper imaging is essential for diagnosis.
Recommended Views:
- PA (posteroanterior)
- Lateral
- Clenched-fist supinated PA
- Radial and ulnar deviation views
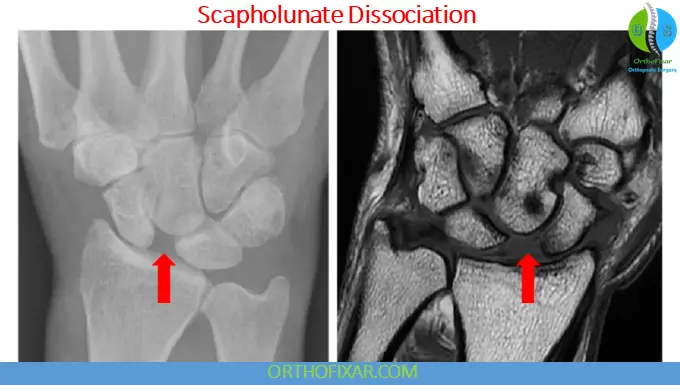
Classic Radiographic Signs
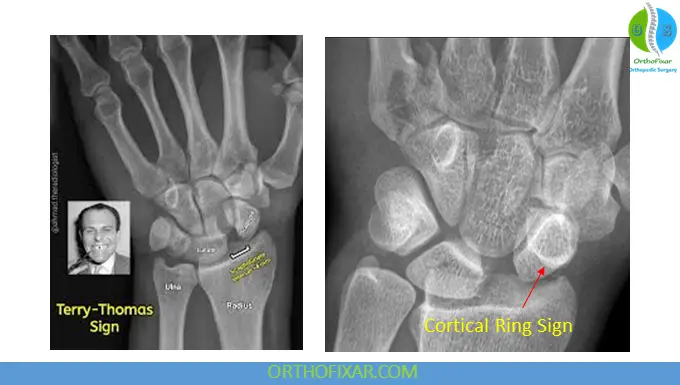
1. Terry Thomas Sign
- Widened scapholunate gap >3 mm (normal <2 mm)
2. Cortical Ring Sign
- Due to flexed scaphoid, creating a circular cortical appearance
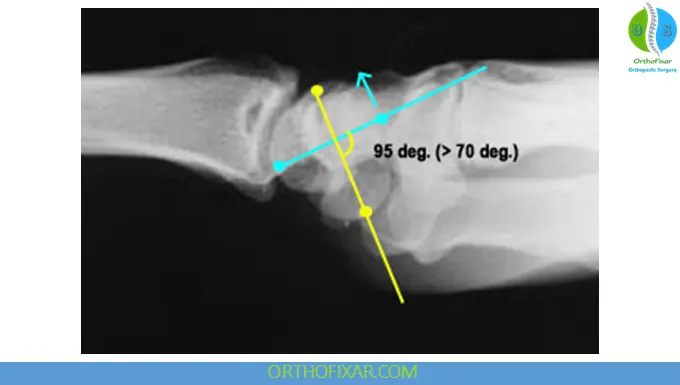
3. Increased Scapholunate Angle
- Angle >70° on lateral view
- Associated with Dorsal Intercalated Segment Instability
Classification
Scapholunate dissociation injuries can be categorized as:
- Acute (≤6 weeks)
- Subacute
- Chronic (>6 weeks)
Chronic injuries are significantly more difficult to treat.
Scapholunate Dissociation Treatment
Non-Surgical (Limited Role)
- Immobilization (for partial or stable injuries)
- Often insufficient for complete tears
Surgical Management
1. Arthroscopic Reduction and Pinning
- Minimally invasive
- Variable outcomes
- Suitable for early injuries
2. Open Reduction and Internal Fixation (ORIF)
Indicated when:
- Reduction cannot be achieved or maintained
Key steps:
- Dorsal surgical approach
- Reduction of scapholunate interval
- Repair of the scapholunate ligament (if possible)
- Dorsal capsulodesis
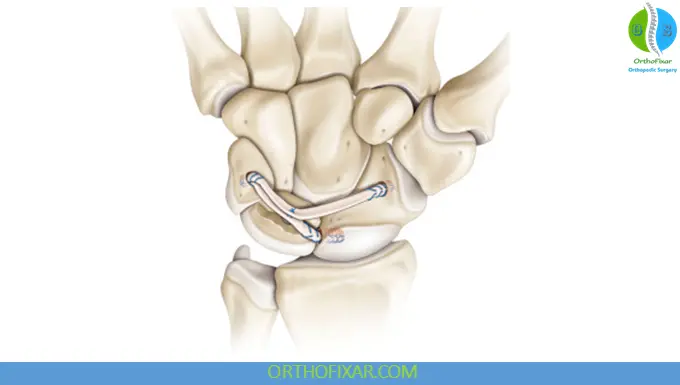
- Stabilization using Kirschner wires (K-wires)
Volar approach may be used when needed.
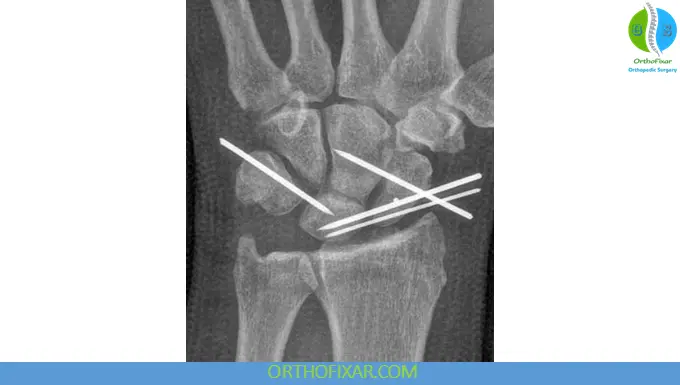
Management of Chronic Injuries
Chronic Scapholunate Dissociation is one of the most challenging conditions in hand surgery.
Common techniques include:
- Ligament reconstruction using tenodesis
- Capsulodesis procedures
- Bone–tendon–bone graft reconstruction
- Temporary screw fixation
- Suture anchors and fiber tape augmentation
⚠️ No single technique has proven definitively superior.
Complications
1. Recurrent Instability
Failure of scapholunate dissociation repair may require:
- Ligament augmentation
- Intercarpal fusion
- Proximal row carpectomy
- Total wrist fusion
2. Progressive Deformity
- Development of DISI pattern
3. Degenerative Arthritis
- Progression to SLAC wrist, leading to chronic pain and loss of function
Prognosis
- Early diagnosis = better outcomes
- Delayed treatment often leads to:
- Chronic instability
- Irreversible joint degeneration
Key Clinical Pearls
- Always suspect SLD in wrist trauma with persistent pain and normal X-rays
- Clenched-fist view can reveal subtle instability
- The dorsal scapholunate ligament is the primary stabilizer
- Chronic injuries are significantly harder to treat than acute ones
Conclusion
Scapholunate dissociation is a high-impact wrist injury that demands early recognition and appropriate management. Despite advances in surgical techniques, chronic cases remain difficult, reinforcing the importance of timely diagnosis and intervention.
References & More
- Lane R, Tafti D, Varacallo MA. Scapholunate Advanced Collapse. [Updated 2024 Jan 8]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: Pubmed
- Buck-Gramcko D. Die skapholunäre Dissoziation [Scapholunate dissociation]. Handchir Mikrochir Plast Chir. 1985 Jul;17(4):194-9. German. PMID: 4029763. Pubmed
- Wessel LE, Wolfe SW. Scapholunate Instability: Diagnosis and Management – Anatomy, Kinematics, and Clinical Assessment – Part I. J Hand Surg Am. 2023 Nov;48(11):1139-1149. doi: 10.1016/j.jhsa.2023.05.013. Epub 2023 Jul 14. PMID: 37452815. Pubmed
- Egol KA. Handbook of fractures. 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2019.