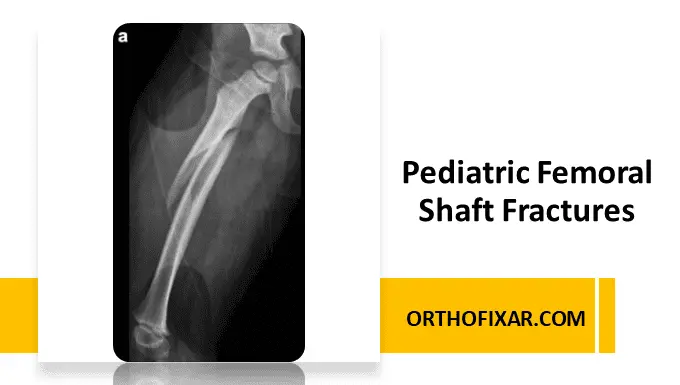
Pediatric femoral shaft fractures are among the most significant long-bone injuries in children and adolescents. These fractures require age-specific evaluation and treatment because remodeling potential, fracture biomechanics, and healing capacity differ substantially between infants, children, and teenagers.
Femoral shaft fractures can result from low-energy trauma in younger children or high-energy trauma in adolescents. Management ranges from Pavlik harness treatment in infants to flexible intramedullary nailing and rigid locked nails in older children.
Epidemiology
Pediatric femoral shaft fractures:
- Represent approximately 1.6% of all pediatric fractures
- Affect males more commonly than females at a ratio of approximately 2.6:1
- Demonstrate a bimodal age distribution:
- First peak: 2–4 years
- Second peak: mid-adolescence
- Occur more frequently during the summer months
Child Abuse Considerations
Nonaccidental trauma must always be considered, especially in younger children:
- In children younger than walking age, approximately 80% of femoral fractures are related to abuse
- In toddlers, the incidence decreases to roughly 30%
Adolescent Injuries
In adolescents:
- More than 90% of femoral shaft fractures are caused by motor vehicle accidents
Anatomy and Biomechanics
During skeletal maturation, the femur transitions from predominantly woven bone to stronger lamellar bone. Fracture displacement patterns depend largely on:
- Fracture location
- Muscle attachments
- Deforming muscular forces
Typical Deforming Forces
Proximal Shaft Fractures
The proximal fragment commonly assumes:
- Flexion — due to the iliopsoas
- Abduction — due to hip abductors
- External rotation — due to short external rotators
Midshaft Fractures
Deformity is less severe because:
- Adductor and extensor muscles provide partial balance
Distal Shaft Fractures
Minimal deformity occurs because:
- Most muscular attachments remain on the same fragment
Supracondylar Femur Fractures
Typically demonstrate:
- Hyperextension of the distal fragment
- Gastrocnemius muscle pull contributes to deformity
See Also: Pediatric Hip Fractures: Diagnosis, Classification & Treatment
Mechanism of Injury
Direct Trauma
Common causes include:
- Motor vehicle accidents
- Pedestrian injuries
- Falls
- Child abuse
Indirect Trauma
- Rotational injuries may produce spiral fractures
Pathologic Fractures
Underlying conditions include:
- Osteogenesis Imperfecta
- Nonossifying fibroma
- Bone cysts
- Bone tumors
- Severe osteopenia associated with:
- Myelomeningocele
- Cerebral palsy
Clinical Evaluation
Initial Assessment
Children with high-energy trauma require full trauma evaluation according to Advanced Trauma Life Support (ATLS) principles.
Typical findings include:
- Inability to ambulate
- Severe pain
- Swelling
- Gross deformity
- Shortened or externally rotated limb
Diagnosis may be challenging in:
- Polytrauma patients
- Head-injured children
- Nonambulatory children
- Severely disabled patients
Neurovascular Examination
A complete neurovascular assessment is mandatory.
Clinicians should evaluate:
- Distal pulses
- Capillary refill
- Motor function
- Sensory status
Soft Tissue Assessment
All splints and dressings applied in the field should be removed carefully to assess for:
- Open fractures
- Skin compromise
- Compartment syndrome
Associated Injuries
The ipsilateral hip and knee must be examined for:
- Femoral neck fractures
- Hip dislocation
- Distal femoral physeal injury
- Ligamentous knee injury
- Meniscal tears
- Tibial fractures
Waddell Triad
The classic Waddell triad includes:
- Head injury
- Thoracic or abdominal trauma
- Femoral shaft fracture
This combination strongly suggests severe vehicular trauma.
Radiographic Evaluation
Standard Imaging
Essential radiographs include:
- Anteroposterior femur view
- Lateral femur view
Additional Imaging
Radiographs of the:
- Hip
- Knee
are important to exclude associated injuries.
Advanced Imaging
MRI or CT scans are usually unnecessary but may help identify:
- Occult fractures
- Stress fractures
- Buckle fractures
- Nondisplaced injuries
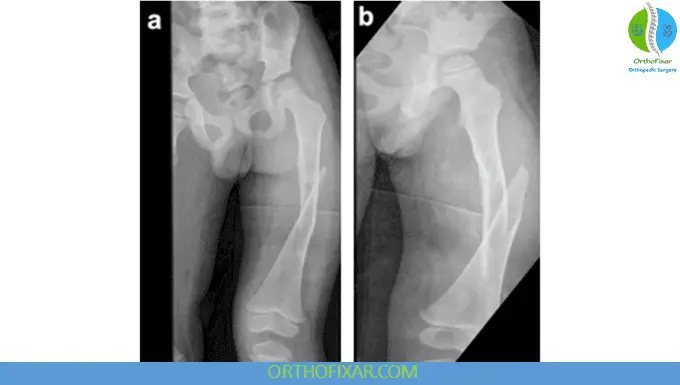
Classification
Descriptive Classification
Open vs Closed
- Open fractures involve communication with the external environment
- Closed fractures do not
Fracture Location
- Proximal third
- Middle third
- Distal third
Fracture Pattern
- Transverse
- Spiral
- Oblique
- Butterfly fragment
- Comminuted
Alignment Parameters
- Displacement
- Angulation
- Rotation
- Shortening
Anatomic Classification
Subtrochanteric Fractures
Occur distal to the lesser trochanter.
Femoral Shaft Fractures
Involve the diaphysis.
Supracondylar Fractures
Occur just proximal to the distal femoral condyles.
Treatment
Treatment depends primarily on:
- Patient age
- Weight
- Fracture pattern
- Stability
- Associated injuries
- Skeletal maturity
Treatment by Age Group
Age Less Than 6 Months
Preferred treatments include:
- Pavlik harness
- Posterior splint
Traction and spica casting are rarely required.
Ages 6 Months to 4 Years
Immediate Spica Casting
Immediate hip spica casting is the most common treatment and is successful in more than 95% of cases.
Benefits include:
- Excellent remodeling potential
- Rapid healing
- Avoidance of surgery
Traction Followed by Spica Cast
May be required if:
- Length cannot be maintained
- Alignment is unacceptable
Traction pins should be placed proximal to the distal femoral physis.
External Fixation
Considered for:
- Open fractures
- Polytrauma
- Severe soft tissue injury
Ages 4 to 12 Years
Flexible Intramedullary Nails
Flexible elastic nails inserted retrograde are widely used.
Advantages:
- Minimally invasive
- Preserve periosteal blood supply
- Allow early mobilization
Contraindications include:
- Weight >100 lb (45 kg)
- Highly comminuted fractures
- Significant shortening
Alternative Options
- External fixation
- Bridge plating
- Submuscular plating
- Spica casting for stable fractures
Rigid Intramedullary Nails
Some centers use rigid locked nails through:
- Greater trochanter
- Lateral trochanteric entry
However, this remains somewhat controversial in skeletally immature patients.
Adolescents (12 Years to Skeletal Maturity)
Intramedullary Nailing
Treatment of choice in most adolescents.
Options include:
- Flexible nails (selected cases)
- Locked rigid intramedullary nails
Important Principle
Piriformis entry nails are avoided in children with open physes because of the risk of:
- Femoral head osteonecrosis
- Proximal femoral growth disturbance
Plate Fixation
Submuscular locked plating may be preferred for:
- Subtrochanteric fractures
- Distal femur fractures
- Complex shaft fractures
External Fixation
Reserved mainly for:
- Open fractures
- Damage-control orthopedics
- Hemodynamically unstable patients
Acceptable Reduction Criteria
Acceptable Angulation
| Age Group | Varus/Valgus | Anterior/Posterior | Shortening |
|---|---|---|---|
| Birth–2 years | 30° | 30° | 15 mm |
| 2–5 years | 15° | 20° | 20 mm |
| 6–10 years | 10° | 15° | 15 mm |
| >11 years | 5° | 10° | 10 mm |
Acceptable Shortening
- Ages 2–11 years:
- Up to 2 cm overlap acceptable
- Older than 11 years:
- Up to 1 cm overlap acceptable
Acceptable Rotation
- Up to 10° rotational deformity
- External rotation is generally better tolerated than internal rotation
Operative Indications
Surgical treatment is indicated for:
- Multiple trauma
- Head injury
- Open fractures
- Vascular injury
- Pathologic fractures
- Inability to tolerate spica casting
- Obesity/body habitus limitations
- Uncooperative patients
Operative Techniques
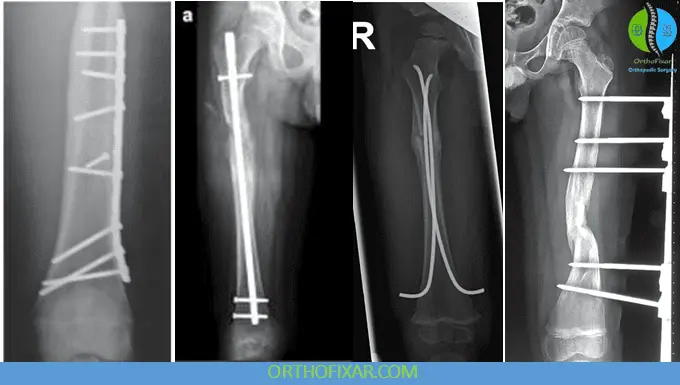
Flexible Intramedullary Nailing
Advantages:
- Less invasive
- Excellent healing rates
- Early mobilization
Nails are inserted:
- Retrograde
- Proximal to distal femoral physis
Locked Rigid Intramedullary Nails
Typically used in older adolescents.
Important considerations:
- Avoid crossing distal femoral physis
- Avoid piriformis entry in skeletally immature patients
External Fixation
Useful in:
- Open fractures
- Polytrauma
- Burn patients
Complications include:
- Pin tract infection
- Knee stiffness
- Refracture after removal
Plate Fixation
Traditional Compression Plating
Disadvantages:
- Large incision
- Periosteal stripping
- Muscle scarring
- Infection risk
Submuscular Locked Plating
Advantages:
- Less soft tissue disruption
- Good fixation in difficult fracture patterns
Complications
Malunion
- Rotational deformities do not remodel well
- Sagittal deformities remodel better than coronal deformities
Nonunion
Rare in children because of excellent healing potential.
Older children may require:
- Bone grafting
- Plate fixation
- Locked intramedullary nailing
Muscle Weakness
Temporary weakness may occur in:
- Quadriceps
- Hamstrings
- Hip abductors
Most deficits are clinically insignificant.
Leg Length Discrepancy
Most common complication.
Overgrowth
Typically:
- 1.5–2 cm
- Most common in children aged 2–10 years
- Usually occurs during first 2 years after injury
Shortening
Acceptable initial shortening varies with age because later overgrowth may compensate.
Osteonecrosis
A rare but serious complication associated with antegrade intramedullary nailing.
Risk factors include:
- Piriformis entry point
- Open proximal femoral physes
Radiographic changes may appear up to 15 months postoperatively.
Prognosis
Most pediatric femoral shaft fractures heal successfully with excellent long-term function.
Prognosis depends on:
- Patient age
- Fracture pattern
- Associated injuries
- Treatment quality
- Complications
Children generally possess remarkable remodeling potential and healing capacity compared with adults.
Key Points
- Pediatric femoral shaft fractures demonstrate age-dependent treatment strategies.
- Immediate spica casting remains standard for many young children.
- Flexible intramedullary nailing is commonly used in school-age children.
- Locked intramedullary nails are preferred in adolescents.
- Leg length discrepancy is the most common complication.
- Piriformis entry nails should be avoided in skeletally immature patients.
References & More
- Sun J, Wang T, Zhao N, Chen H, Chen C. Pediatric femoral shaft fractures: the American Academy of Orthopaedic Surgeons clinical practice guidelines versus actual management in a teaching hospital. Transl Pediatr. 2024 Jun 30;13(6):938-945. doi: 10.21037/tp-24-175. Epub 2024 Jun 20. PMID: 38984021; PMCID: PMC11228901. Pubmed
- Greenhill DA, Herman MJ. Treatment of Pediatric Femoral Shaft Fractures. J Am Acad Orthop Surg. 2022 Nov 15;30(22):e1443-e1452. doi: 10.5435/JAAOS-D-22-00415. Epub 2022 Sep 13. PMID: 36107122. Pubmed
- Liau GZQ, Lin HY, Wang Y, Nistala KRY, Cheong CK, Hui JHP. Pediatric Femoral Shaft Fracture: An Age-Based Treatment Algorithm. Indian J Orthop. 2020 Oct 10;55(1):55-67. doi: 10.1007/s43465-020-00281-6. PMID: 33569099; PMCID: PMC7851225. Pubmed
- Egol KA. Handbook of fractures. 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2019.