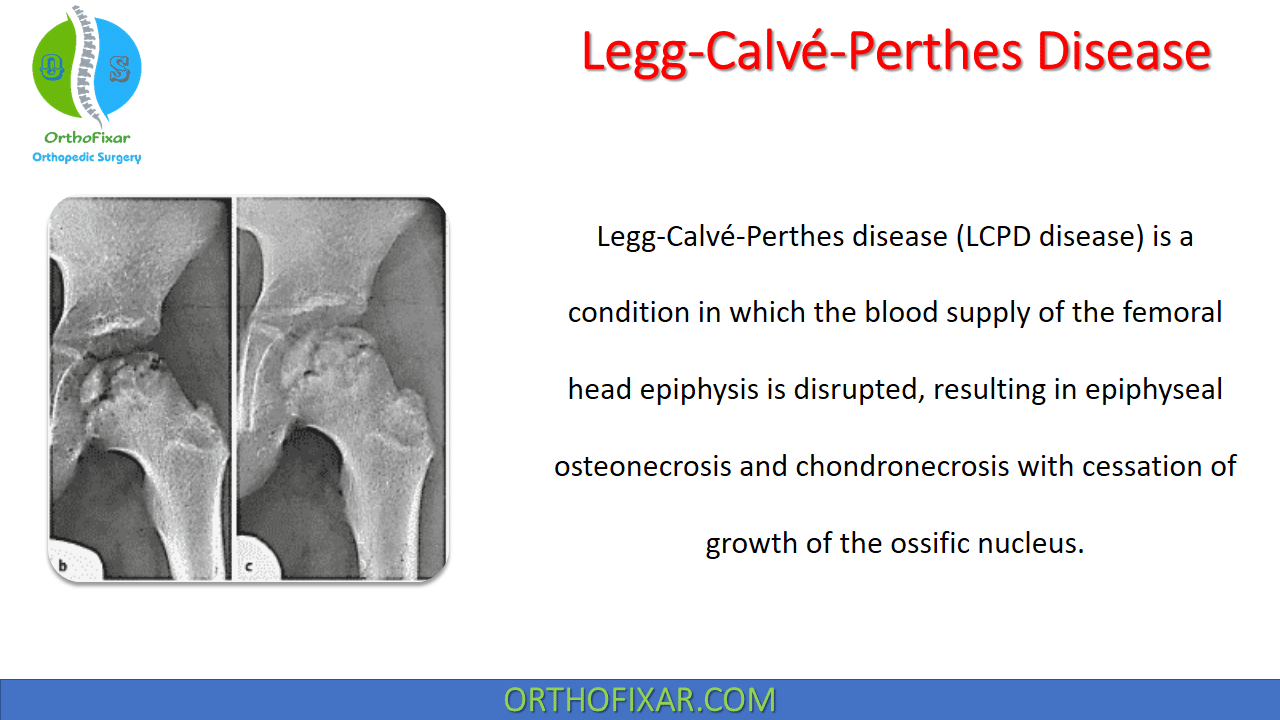
Legg-Calvé-Perthes disease (LCPD disease) is a condition in which the blood supply of the femoral head epiphysis is disrupted, resulting in epiphyseal osteonecrosis and chondronecrosis with cessation of growth of the ossific nucleus.
It was independently recognized in 1910 by Arthur Legg of the United States, Jacques Calvé of France, Georg Perthes of Germany, and Henning Waldenström of Sweden
It is most commonly seen in children between the ages of 4 and 8 years (It can be seen at any age between 18 months of age and skeletal maturity). It is more common in boys than in girls by a ratio of 4:1, and bilateral in 10% to 12% of patients.
Causes of Legg-Calvé-Perthes disease (LCPD)
The origin of Legg-Calvé-Perthes disease LCPD is probably multifactorial, and the exact cause is unknown.
1. Coagulation Abnormalities such as:
- Sickle cell disease
- Thalassemia
- Chronic myeloid leukemia
- Non-Hodgkin lymphoma
- Idiopathic thrombocytopenic purpura
- Hemophilia.
2. Arterial Status of the Femoral Head:
Normally, the primary blood supply to the capital epiphysis comes from two anastomotic arterial rings located around the neck of the femur. The medial and lateral femoral circumflex arteries form the extracapsular ring, and most of the blood is supplied by the medial circumflex artery.
As the vessel advances between the trochanter and the capsule, it courses through a narrow passage, an area particularly constricted in children younger than 8 years of age. In addition to the extracapsular ring, there is also a subsynovial intracapsular ring that has been found to be incomplete more often in boys than in girls.
The major source of blood flow to the femoral head in black African neonates is the inferior gluteal artery, that is why the disease is uncommon in black children.
3. Venous Drainage of the Femoral Head and Neck:
Venous drainage normally flows through the medial circumflex vein. Increased venous pressure in the affected femoral neck and associated venous congestion in the metaphysis have been observed in patients with Legg-Calvé-Perthes disease LCPD. Although these abnormalities in venous outflow are a consistent finding in Legg-Calvé-Perthes disease LCPD, it is unknown whether they are a cause of the disorder or a secondary effect of some other factors involved in the pathogenetic process.
4. Systemic Abnormalities “Predisposed Child”:
Systemic Abnormalities thought to make the child Predisposed to Legg-Calvé-Perthes disease LCPD, such as:
- A delay in bone age relative to the patient’s chronologic age is the most commonly observed abnormality.
- The manifestation of discrete abnormalities in the patient’s opposite femoral head.
- The birth weight of children with Legg-Calvé-Perthes disease LCPD was found to be significantly lower than that of unaffected children.
- Insulin-like growth factor (IGF) pathway dysfunction.
- Lower plasma somatomedin C (now IGF-I) levels have been reported in children with Legg-Calvé-Perthes disease LCPD who were small and had immature bone ages.
5. Hyperactivity or Attention Deficit Disorder:
Many children with Legg-Calvé-Perthes disease LCPD tend to be very active physically, and some are pathologically hyperactive or suffer from attention deficit disorder.
Hyperactivity would be associated with greater mechanical loading of the hip joint and increased subclinical “trauma” that could influence the pathogenesis of the femoral head deformity and its outcome.
6. Trauma:
In the developing proximal femur, the major lateral epiphyseal artery must course through a narrow passage, which could make the vessel susceptible to disruption after trauma to this area.
7. Hereditary Influences:
G-455-A polymorphism of the beta-fibrinogen gene has been associated with Legg-Calvé-Perthes disease LCPD, and passive smoking has been suggested to increase the
risk of development of the disorder.
8. Type II Collagenopathy:
A missense mutation in the type II collagen gene (replacement of glycine with serine at codon 1170 of COL2A1).
9. Environmental Influences:
Environmental influences have been reported, primarily in Great Britain, as a possible cause of Legg-Calvé-Perthes disease LCPD, which has a high occurrence in particular urban areas. Low levels of blood manganese were subsequently found in affected children.
Exposure to smoking has been suggested as an etiologic factor. This exposure is known to lower stimulated tissue plasminogen activator activity, thus leading to hypofibrinolysis and possibly to venous occlusion of femoral head vessels.
10. Synovitis:
Synovitis of the hip occurs early in Legg-Calvé-Perthes disease LCPD and may precede radiographic changes. A slight increase in pressure has been noted during the early stages of Legg-Calvé-Perthes disease LCPD. Pressures were moderately increased in patients with idiopathic synovitis and extremely high in those with septic arthritis.
See Also: Developmental Dysplasia of the Hip (DDH)
Stages of legg-calvé-perthes disease:
| Stage | Discription |
|---|---|
| I- EARLY STAGE | – Dead trabecular bone and marrow necrosis – Necrosis of deep layer of epiphyseal cartilage – Thickened articular cartilage – Collapsed trabeculae – Subchondral fracture or separation of cartilage and bone junction – Physeal disruption – Cartilage extending from the physis into the metaphysis |
| II- FRAGMENTATION STAGE | – Invasion of vascular granulation tissue in the marrow space. – Increased vessels in the cartilage – Increased osteoclasts and bone resorption in the bony epiphysis. – Restoration of endochondral ossification in the periphery of the epiphysis |
| III- REOSSIFICATION STAGE | – New bone forming on old trabeculae – Woven new bone formation |
| IV- HEALING STAGE | – New bone, woven and lamellar – Return to normal architecture |
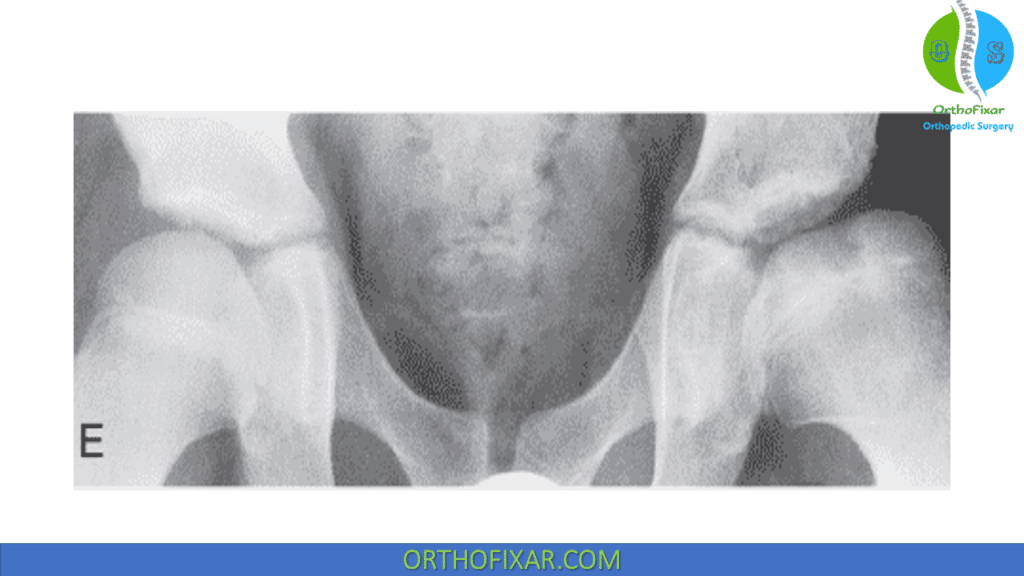
Classification:
Lateral Pillar Classification System:
Lateral Pillar Classification System is based on the height of the lateral pillar of the capital femoral epiphysis on AP imaging of the pelvis. This classification has best interobserver agreement. It’s designed to provide prognostic information.
| Group | Lateral Pillar Radiographic Findings | Prognosis |
|---|---|---|
| A | – No density change – No loss of height | Good outcome |
| B | – Some density change – Height ≥50% – Central pillar collapse | Poor outcome in patients with bone age > 6 years |
| B/C | – Thin lateral pillar – Borderline height | Poor outcome |
| C | – Height <50% | Poor outcome |
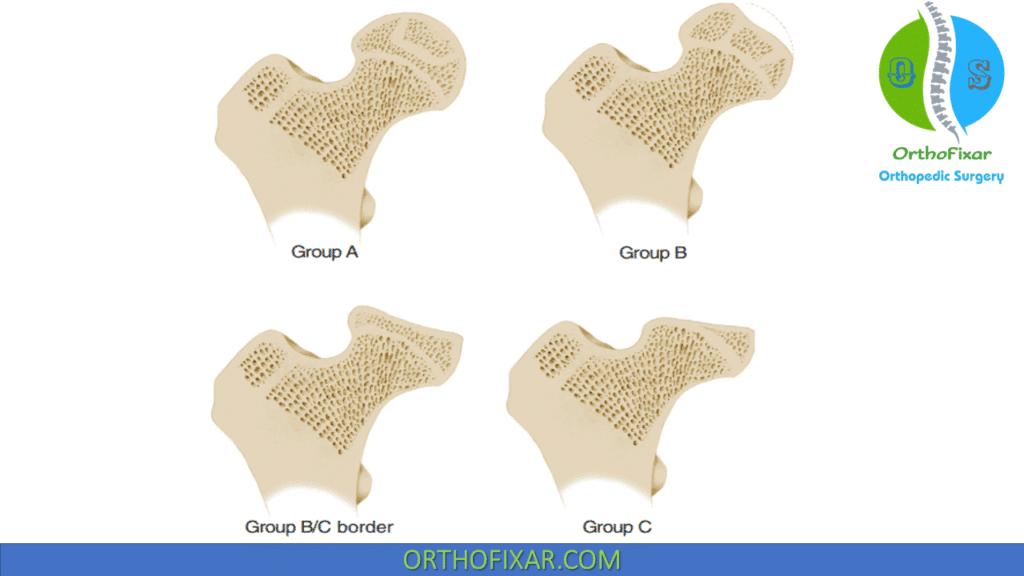
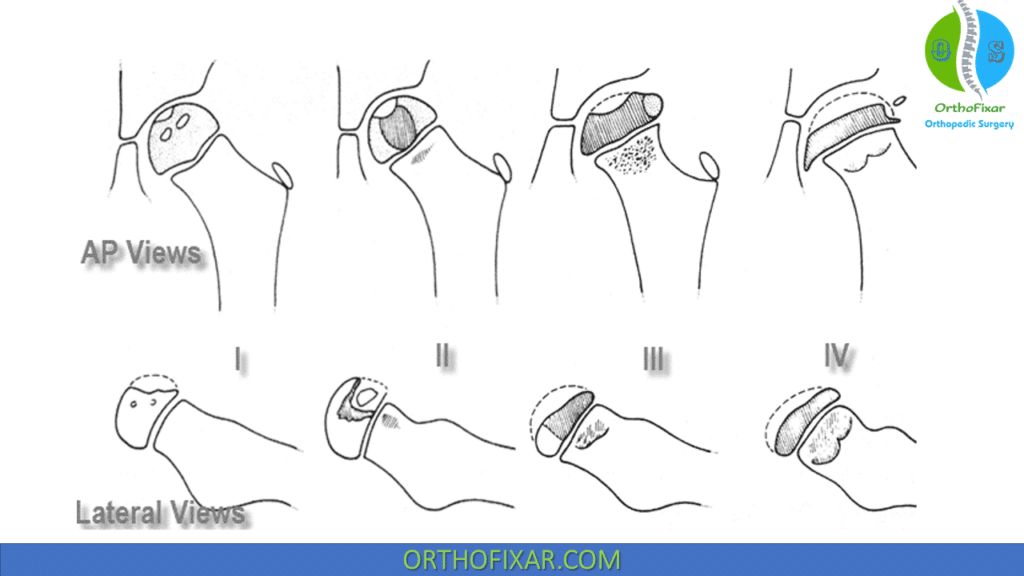
Catterall Classification:
Catterall classification is based on degree of head involvement:
| Group | Head Involvement |
|---|---|
| Group I | Involvement of the anterior epiphysis only |
| Group II | Involvement of the anterior epiphysis with a clear sequestrum |
| Group III | Only a small part of the epiphysis is not involved |
| Group IV | Total head involvement |
Stulberg Classification System
Catterall Classification is based on Anteroposterior and frog-leg lateral radiographs.
| Group | Radiographic Findings |
|---|---|
| I | Femoral head normal. |
| II | Femoral head round, within 2 mm of circle, same. circle both views. |
| III | Femoral head ovoid, acetabulum matches head |
| IV | Femoral head flattened more than 1 cm on weight-bearing areas, acetabulum also flattened. |
| V | Femoral head collapsed, acetabulum not flattened. |
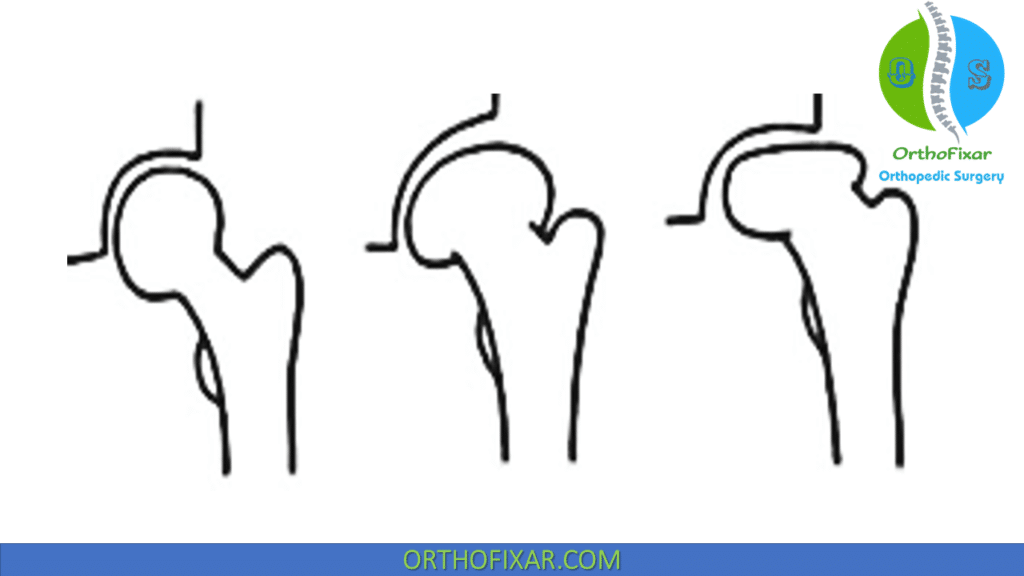
Prognosis:
Maintaining sphericity of femoral head is the most important factor in achieving a good result.
| Good Prognosis | Bad Prognosis |
|---|---|
| 1. Younger age (bone age) < 6 years at presentation 2. Preservation of Range of motion. | 1. Age (bone age) > 6 years at presentation. 2. Female sex 3. Decreased hip range of motion (decreased abduction). 4. Lateral column C classification (regardless of age). |
See Also: Hip Joint Osteoarthritis
Catterall “head at risk” signs include:
- Lateral calcification
- Gage sign (V-shaped defect at lateral physis)
- Lateral subluxation
- Metaphyseal cyst formation
- Horizontal growth plate
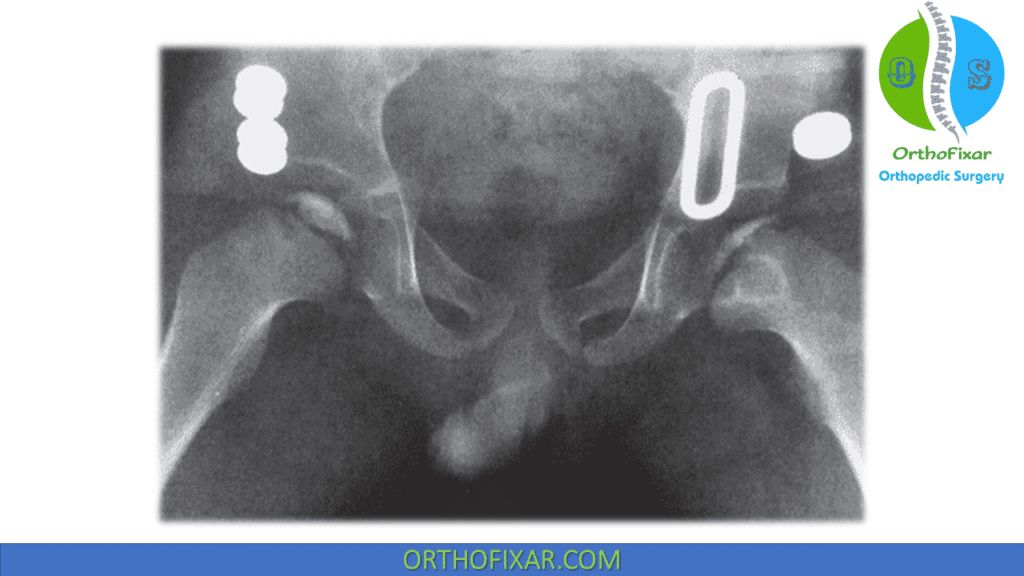
Symptoms and Signs:
Legg Calve Perthes disease symptoms include:
- Limping: usually first noticed by a parent.
- Hip pain: it may be located in the groin, anterior hip region, or laterally around the greater trochanter.
- Referred pain to the knee or anterior thigh.
- Possible history of trauma.
The pain is aggravated by increased physical activity and is usually worse late in the day. The child occasionally has night pain.
The clinical signs include:
- Limp: The child’s limp is normally a combination of an antalgic gait and a Trendelenburg gait (The Trendelenburg sign is positive)
- Decreased hip range of motion (abduction and internal rotation): it is caused by muscle spasm or involuntary guarding related to hip synovitis.
- Resistance to logroll
- Varying degrees of atrophy of the gluteus, quadriceps, and hamstring muscles (Depending on the duration and severity of the condition).
Imaging Study:
AP and Frog leg lateral Views is recommended, radiology findings include:
- Medial joint space widening (the earliest finding): it may be caused by synovitis and hypertrophy of articular cartilage.
- Irregularity of femoral head ossification.
- Cresent sign (represents a subchondral fracture).
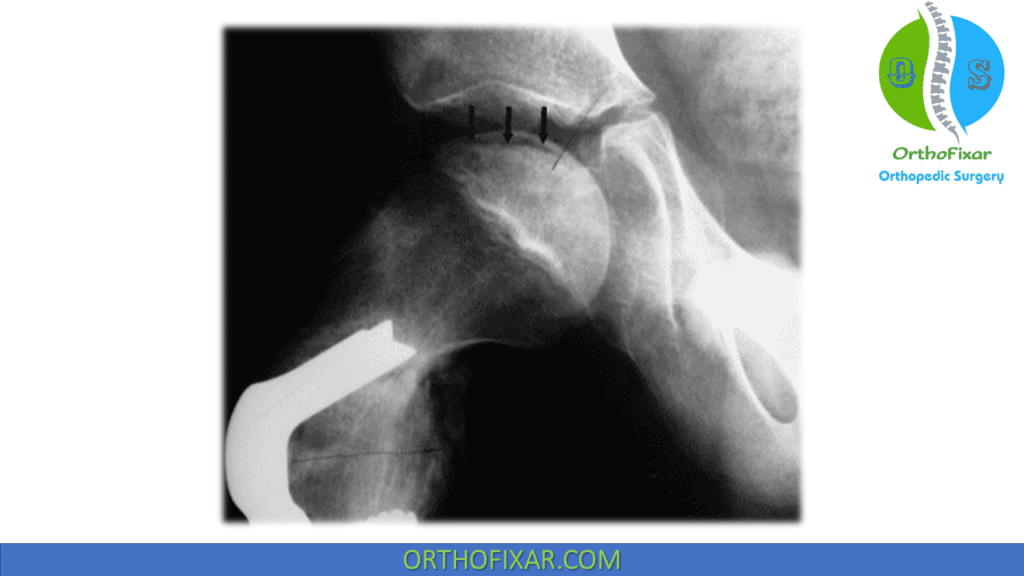
Waldenström Classification of the Stages of Legg-Calvé-Perthes Disease Based on Radiographic Changes in the Femoral Head:
| Stage | Features | Radiographic Changes |
|---|---|---|
| I | Stage of increased density | – Ossific nucleus initially smaller. – femoral head becomes uniformly dense. – a subchondral fracture may be seen. – radiolucencies appear in the mDe Sanctisetaphysis. |
| II | Fragmentation stage | – Varying patterns of lucency appear in epiphysis. – segments (pillars) of the femoral head demarcate. – the femoral head may flatten and widen. – metaphyseal changes resolve; acetabular contour may change. |
| III | Healing or reossification stage | – New bone appears in femoral head which gradually reossifies. – epiphysis becomes homogeneous |
| IV | Healed or remodeling stage | – Femoral head is fully reossified and remodels to maturity. – Acetabulum also remodels |
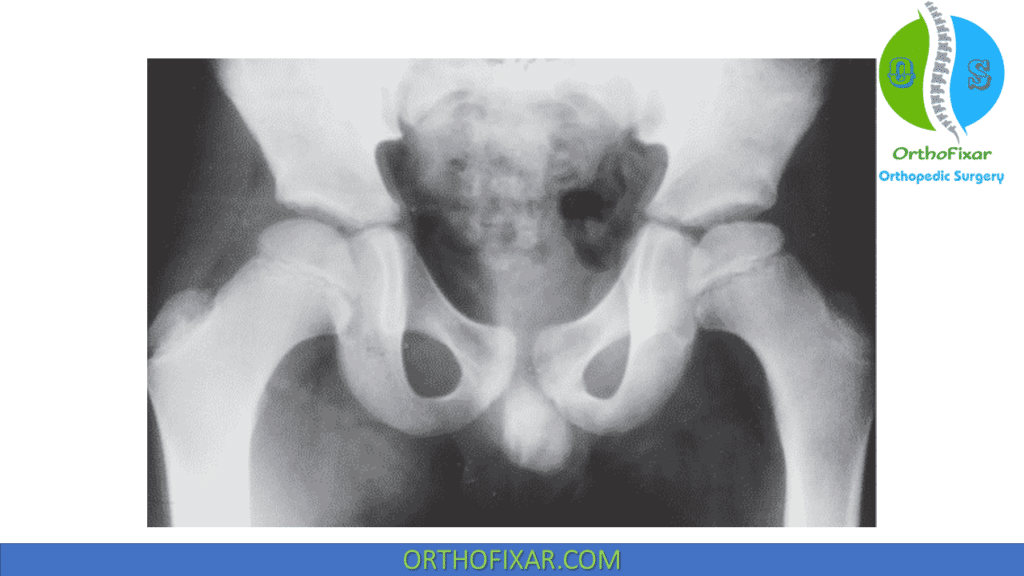
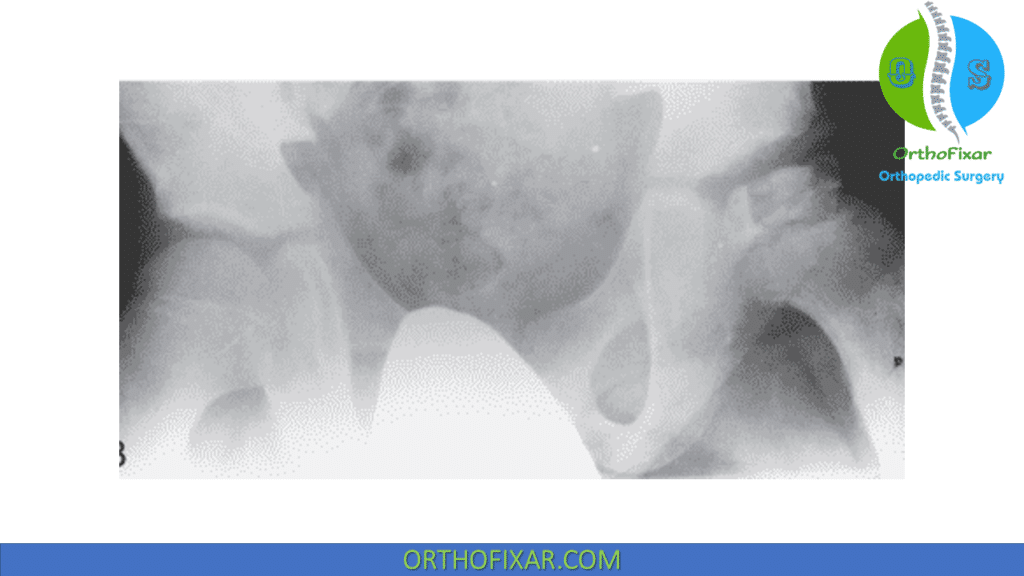
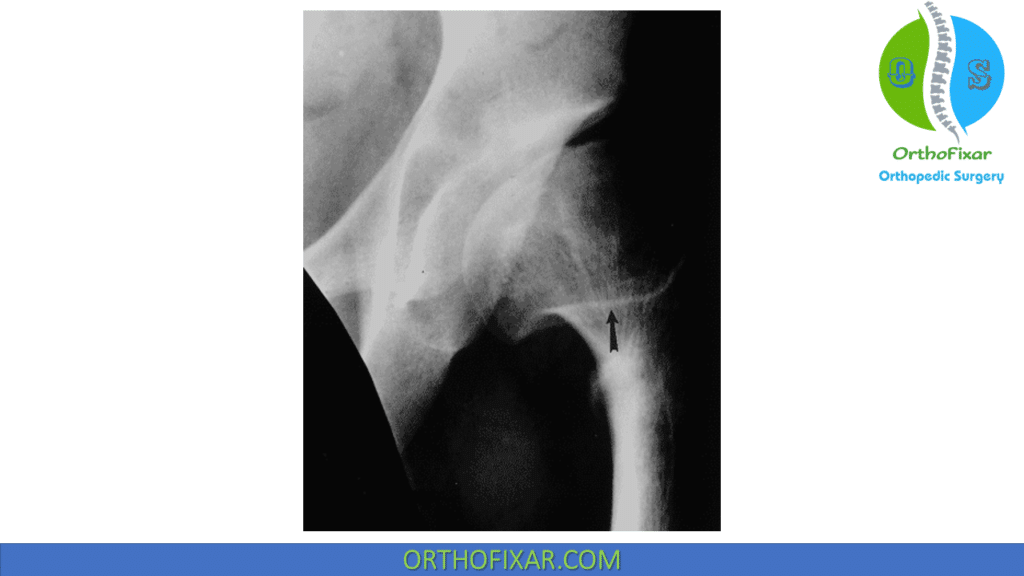
The “sagging rope” sign is a radiodense line overlying the proximal femoral metaphysis, is a result of physeal damage associated with significant metaphyseal response. The edge of the rope is in fact the anterior portion of the overlarge femoral head as it projects over the metaphysis.
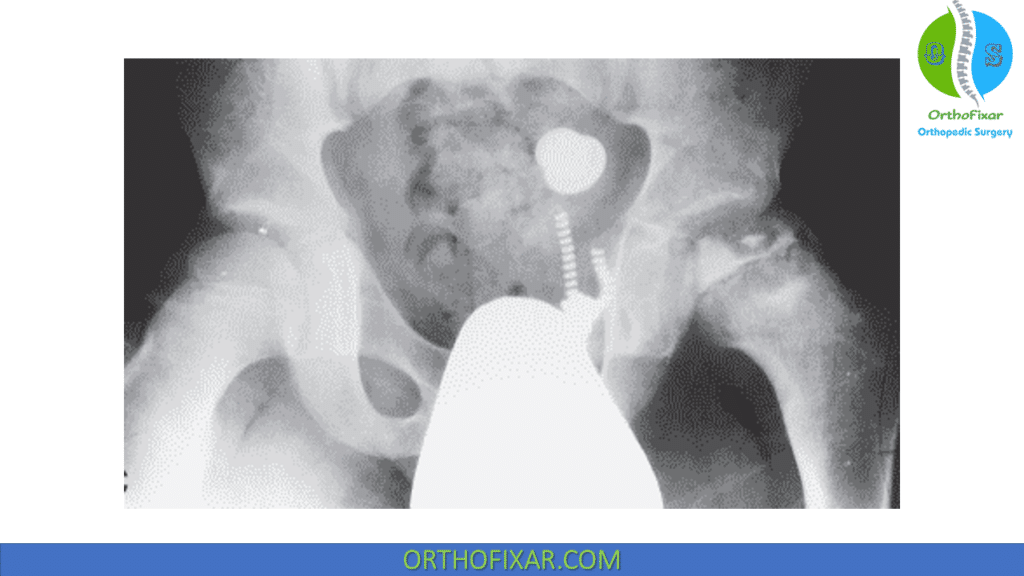
Changes in the Acetabulum include:
- When the femoral head protrudes from the acetabulum, the medial wall may form what looks like a second compartment for the head.
- Referred to as bicompartmentalization, this change was suggested to be an indication of a poor outcome.
- Acetabular retroversion is commonly found in patients with Legg-Calvé-Perthes disease LCPD.
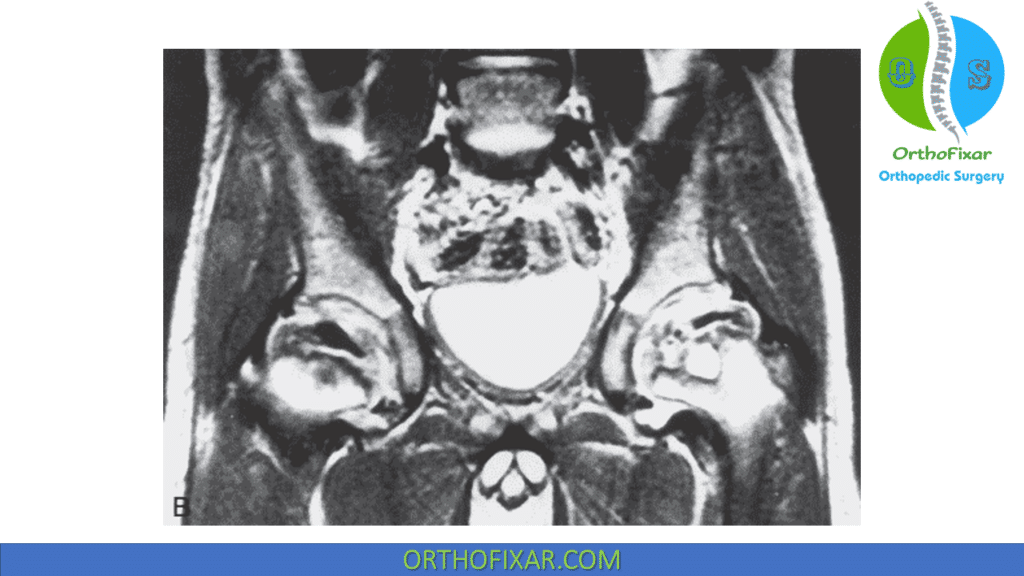
Magnetic Resonance Imaging (MRI)
Early diagnosis revealing alterations in the capital femoral epiphysis and physis. MRI is more sensitive than radiograph.
De Sanctis and colleagues proposed a classification based on MRI of percentage of head necrosis, lateral extrusion, and physeal disruption:
- Group A had less than 50% head involvement.
- Group B greater than 50% necrosis of the femoral head:
- B0 to B3 based on the degrees of lateral extrusion and physeal disruption.
- Groups B2 and B3 were associated with a poor prognosis.
Computed Tomography
CT can provide accurate three-dimensional images of the shape of the femoral head and acetabulum. It is not typically used on a routine basis to evaluate patients with Legg-Calvé-Perthes disease LCPD, and clinical decisions are not usually made on the basis of early CT findings.
A classification system was developed based on CT findings:
| Group | Findings |
|---|---|
| Group A | Only the periphery of the femoral head is affected |
| Group B | There is considerable necrosis of the central portion of the head but no posterior involvement. |
| Group C | The entire head is affected. |
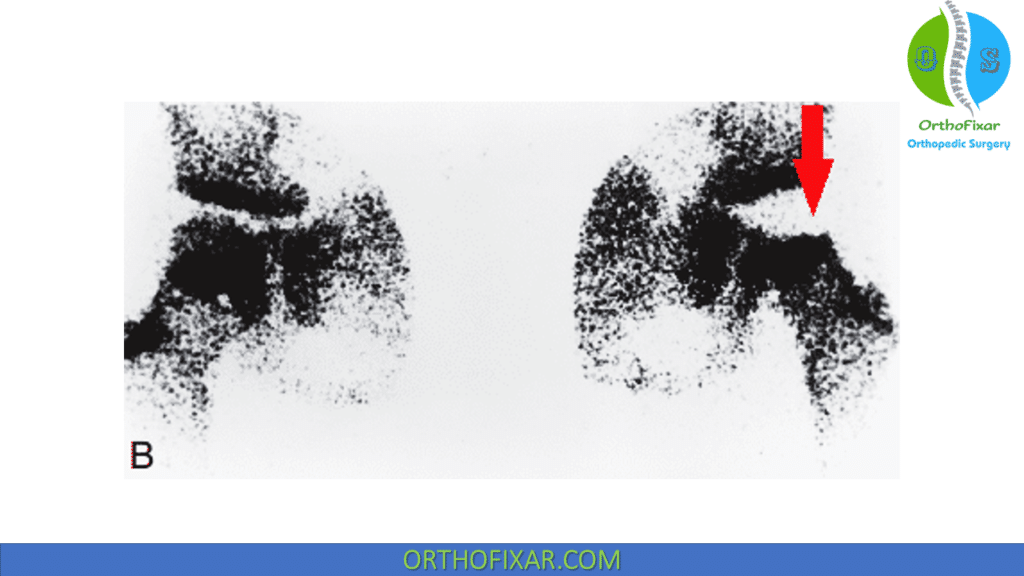
Bone scan can confirm suspected case of Legg-Calvé-Perthes disease LCPD. Decreased uptake (cold lesion) can predate changes on radiographs.
A dynamic arthrogram can demonstrate coverage and containment of the femoral head.
Ultrasonography is sometimes used in the early stages of Legg-Calvé-Perthes disease LCPD to demonstrate joint effusion and in later stages to assess the shape of the femoral head. Ultrasonography with microbubble contrast enhancement has been used to evaluate the vascularization of the femoral head.
Treatment
The goals of Legg Calve Perthes treatment are:
- Relief of symptoms.
- Restoration of ROM.
- Preserve Containment of the hip.
Nonoperative:
Nonoperative treatment is indicated in:
- Children < 8 years of age : (young patient do not benefit from any surgery)
- Children with lateral pillar A.
- Consider activity restriction and protected weight-bearing during earlier stages until reossification is complete
Nonoperative include:
- Observation.
- Activity restriction (non-weightbearing with a wheelchair, crutches, or a walker.
- Bed rest (with or without traction of the affected leg).
- Physical therapy to keep ROM of the hip.
- Orthotic devices to contain the femoral head nonsurgically (All braces abduct the affected hip, most allow for hip flexion, and some control rotation of the limb).
- Short-term use of nonsteroidal anti-inflammatory drugs for pain and discomfort.
Operative:
Surgical treatment is indicated in:
- Children > 8 years of age, especially lateral pillar B and B/C.
- Hinge abduction: lateral extrusion of the capital femoral epiphysis.
There are two types of procedures:
- Containment:
- Femoral osteotomy: proximal femoral varus osteotomy.
- Pelvic osteotomy: Salter osteotomy, triple osteotomy, Dega osteotomy, Pemberton osteotomy.
- Shelf osteotomy to prevent lateral subluxation and lateral epiphyseal overgrowth.
- Salvage:
- Valgus femoral osteotomy for hinge abduction.
- Chiari and/or shelf pelvic osteotomies for hips that can no longer be contained.
References & More
- Campbel’s Operative Orthopaedics 12th edition Book.
- Millers Review of Orthopaedics -7th Edition Book.
- Mills S, Burroughs KE. Legg Calve Perthes Disease. [Updated 2022 Jul 11]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK513230/
- Rodríguez-Olivas AO, Hernández-Zamora E, Reyes-Maldonado E. Legg-Calvé-Perthes disease overview. Orphanet J Rare Dis. 2022 Mar 15;17(1):125. doi: 10.1186/s13023-022-02275-z. PMID: 35292045; PMCID: PMC8922924.