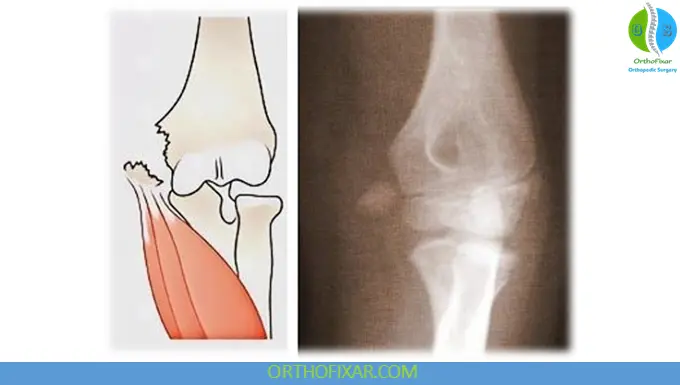
A pediatric medial epicondyle fracture is an avulsion injury involving the medial apophysis of the distal humerus. The injury typically occurs when valgus stress causes traction through the ulnar collateral ligament and flexor-pronator origin, pulling the ossification center away from the distal humerus.
These injuries are common in active children and adolescents, especially athletes involved in throwing sports, wrestling, and gymnastics. They may occur in isolation or in association with elbow dislocation.
Epidemiology
Medial epicondyle fractures account for approximately 12–14% of pediatric elbow fractures, making them one of the most common distal humeral injuries in children. Peak incidence occurs between 9 and 14 years, with the highest frequency around 11–12 years. Boys are affected more frequently than girls, with reported ratios approaching 4:1. Approximately 50–60% are associated with elbow dislocation.
Epidemiologic Highlights
- Represent ~14% of distal humerus fractures
- Peak age: 11–12 years
- Male predominance: 4:1
- Associated elbow dislocation: 50–60%
- Ulnar nerve symptoms: 10–15%
Anatomy and Ossification
The medial epicondyle serves as the attachment site for:
- The flexor-pronator muscle mass
- The ulnar collateral ligament (UCL)
Unlike the condyle, the medial epicondyle is a traction apophysis, meaning forces across the physis are primarily tensile rather than compressive.
The medial epicondyle:
- Begins ossification between 4 and 6 years
- Is the last elbow ossification center to fuse
- Typically closes around 14–15 years
Because the physis remains open during adolescence, it is vulnerable to avulsion injury.
See Also: Elbow Anatomy
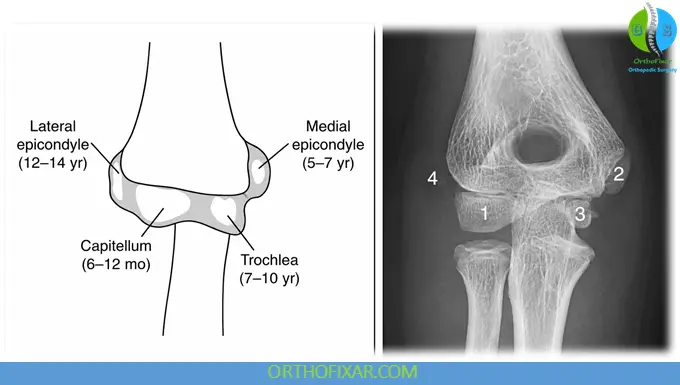
Pediatric Elbow Ossification Centers
The medial epicondyle is part of the CRITOE sequence:
- Capitellum
- Radial head
- Internal (medial) epicondyle
- Trochlea
- Olecranon
- External (lateral) epicondyle
Correct identification is essential to avoid mistaking a normal ossification center for fracture.
Mechanism of Injury
Indirect Mechanisms (Most Common)
1. Elbow Dislocation
A dislocated elbow can avulse the medial epicondyle through traction from the UCL.
2. FOOSH Injury
A fall on an outstretched hand creates valgus-extension stress, leading to avulsion.
3. Athletic Injury
Seen in:
- Baseball pitchers
- Javelin throwers
- Gymnasts
- Wrestlers
- Arm wrestlers
Direct Trauma
A direct blow to the posteromedial elbow may cause fragmentation, though this is uncommon.
Chronic Overuse
Repeated valgus loading may produce chronic traction injury, often called Little League elbow.
See Also: Pediatric Elbow – Lateral Condyle Fractures
Clinical Presentation
Patients with a medial epicondyle fracture usually present with:
- Medial elbow pain
- Swelling
- Point tenderness over the medial epicondyle
- Limited elbow motion
- Pain with resisted wrist flexion
In some cases, a fragment may become incarcerated within the joint, creating a mechanical block to motion.
Neurovascular Examination
The ulnar nerve lies immediately posterior to the medial epicondyle, making neurologic examination mandatory.
Evaluate:
- Sensation of the small finger
- Intrinsic hand strength
- Finger abduction/adduction
Ulnar nerve dysfunction occurs in roughly 10–15% of cases.
Radiographic Evaluation
Standard imaging includes:
- AP elbow radiograph
- Lateral radiograph
- Internal oblique view
Because the medial epicondyle lies posteromedially, slight obliquity may obscure the fragment.
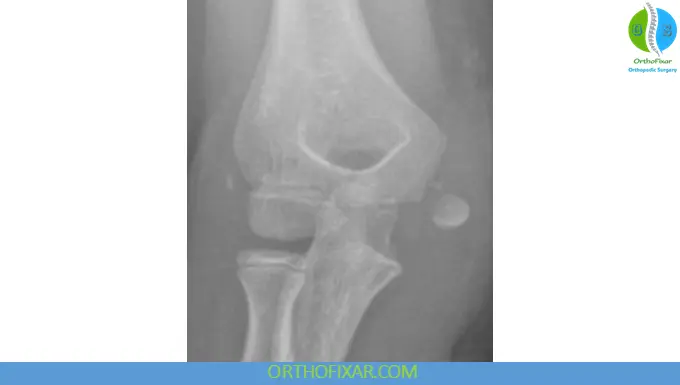
Key Radiographic Signs
Look for:
- Fragment displacement
- Elbow dislocation
- Missing ossification center
- Intra-articular incarceration
- Associated fractures
Comparison views of the contralateral elbow may be useful in younger children.
Differential Diagnosis
Always distinguish medial epicondyle fracture from:
- Medial condyle fracture
- Distal humeral physeal injury
- Elbow dislocation without fracture
- UCL avulsion
- Apophysitis in throwing athletes
If uncertain, MRI or arthrography may help identify intra-articular extension of the medial epicondyle fracture.
Medial Epicondyle Fracture Classification
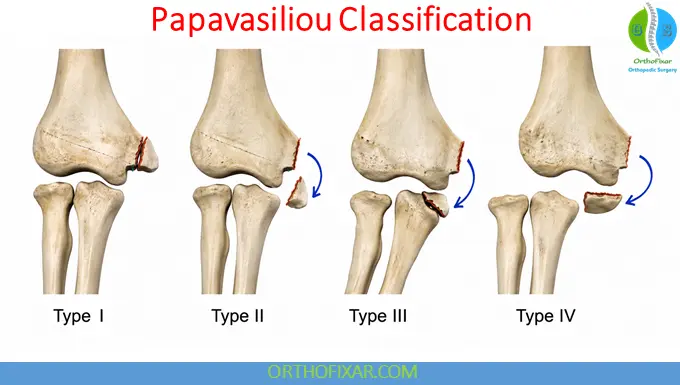
Papavasiliou Classification
- Type I: Minimal or slight avulsion displacement.
- Type II: Fragment is avulsed and displaced to the level of the joint line, but is not entrapped inside the joint.
- Type III: The fragment is incarcerated (entrapped) within the joint.
- Type IV: The fracture is associated with a dislocation of the elbow joint.
Chronic Injuries
- Stress avulsion
- Chronic traction apophysitis
Medial Epicondyle Fracture Treatment
Nonoperative Management
Most fractures can be treated nonoperatively.
Indications
- Nondisplaced fractures
- Minimal displacement
- Stable elbow
- Low-demand patients
Technique
- Posterior splint
- Elbow flexed to 90°
- Forearm neutral or pronated
Splinting typically lasts 3–7 days, followed by early active motion.
Studies show that even though fibrous union may occur in up to 60%, functional outcomes remain excellent in most children.
Operative Management
Absolute Indications
Intra-articular Incarceration: A trapped fragment within the ulnohumeral joint requires surgery.
Relative Indications
- Ulnar nerve dysfunction
- Gross valgus instability
- High-demand throwing athletes
- Significant displacement (>5 mm in many series)
- Associated elbow instability
Children with incarcerated fragments and displacement >5 mm generally achieve better outcomes with early surgery.
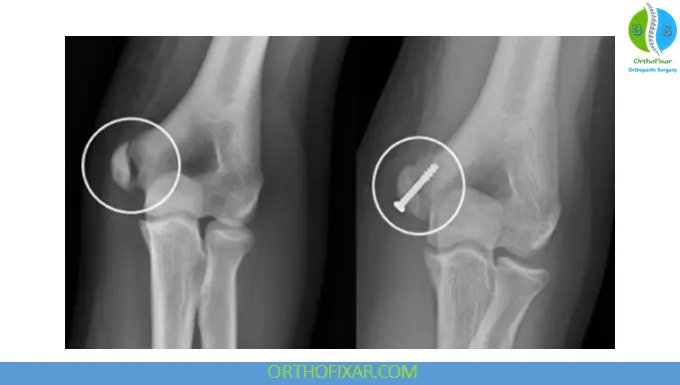
Surgical Fixation
Common Fixation Methods
- Cannulated screw fixation
- Lag screw ± washer
- Kirschner wires for small fragments
Key steps:
- Medial approach
- Identify and protect the ulnar nerve
- Anatomic reduction
- Stable fixation
- Early postoperative motion
Extensive ulnar nerve transposition is usually unnecessary.
Postoperative Rehabilitation
Typical protocol:
Week 0–1
- Posterior splint
Week 1–2
- Transition to removable splint
- Begin active ROM
Week 4–6
- Progressive strengthening
Formal therapy is often unnecessary in compliant children.
Complications
1. Fragment Incarceration
Missed incarceration can lead to stiffness and chronic loss of motion.
2. Ulnar Neuropathy
Occurs in approximately 10–15%.
3. Nonunion
Radiographic nonunion may occur in up to 60% after nonoperative care of displaced fractures, but is often asymptomatic.
4. Loss of Extension
Usually mild (5–10°).
5. Myositis Ossificans
Rare; often related to repeated manipulation.
Prognosis
Both operative and nonoperative treatment generally produce excellent outcomes when appropriately indicated.
Systematic reviews show:
- Operative union rates around 92%
- Nonoperative radiographic union approximately 49%
Despite this, clinical function is often excellent in both groups when elbow stability is maintained.
Key Clinical Pearls
✅ Always assess the ulnar nerve
✅ Search for fragment incarceration after elbow dislocation
✅ Compare with the opposite elbow if ossification centers are unclear
✅ Early motion reduces stiffness
✅ Radiographic nonunion does not always mean poor function
Frequently Asked Questions
Is surgery always needed for pediatric medial epicondyle fractures?
No. Most minimally displaced fractures heal well without surgery. Operative fixation is primarily indicated for incarcerated fragments, instability, nerve dysfunction, or high-demand athletes.
Can these fractures cause growth disturbance?
Rarely. The medial epicondyle contributes minimally to humeral longitudinal growth.
What is the most common missed diagnosis?
An incarcerated fragment after elbow dislocation.
References & More
- Barghi A, Burgess J, Lacoste X, Hyman MJ, Janicki JA, May C. Management of Pediatric Medial Epicondyle Fractures: Results of a Survey of the Pediatric Orthopaedic Society of North America (POSNA). J Pediatr Orthop. 2026 Jan 1;46(1):e1-e7. doi: 10.1097/BPO.0000000000003062. Epub 2025 Aug 12. PMID: 40793996; PMCID: PMC12688462. Pubmed
- Mollah R, Fallahi AKM. Medial Epicondylar Elbow Fractures. [Updated 2023 Jun 12]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: Pubmed
- Patel NM, Ganley TJ. Medial epicondyle fractures of the humerus: how to evaluate and when to operate. J Pediatr Orthop. 2012 Jun;32 Suppl 1:S10-3. doi: 10.1097/BPO.0b013e31824b2530. PMID: 22588097. Pubmed
- Egol KA. Handbook of fractures. 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2019.