Facioscapulohumeral dystrophy (FSHD) is an autosomal dominant condition with characteristic weakness of the facial and shoulder girdle muscles. The affected gene is located on chromosome 4q35. It was first described by Landouzy and Dejerine in the late 1800s.
Facioscapulohumeral muscular dystrophy is the third most common type of muscular dystrophy (behind Duchenne muscular dystrophy and myotonic muscular dystrophy) occurring in approximately 1 in 20,000 individuals.
Onset of the disease may be in early childhood, in which case the disease runs a rapid, progressive course, confining most children to a wheelchair by age 8 to 9 years; alternatively, onset may occur in patients 15 to 35 years old, in which case the disease progresses more slowly.
FSHD Diagnosis
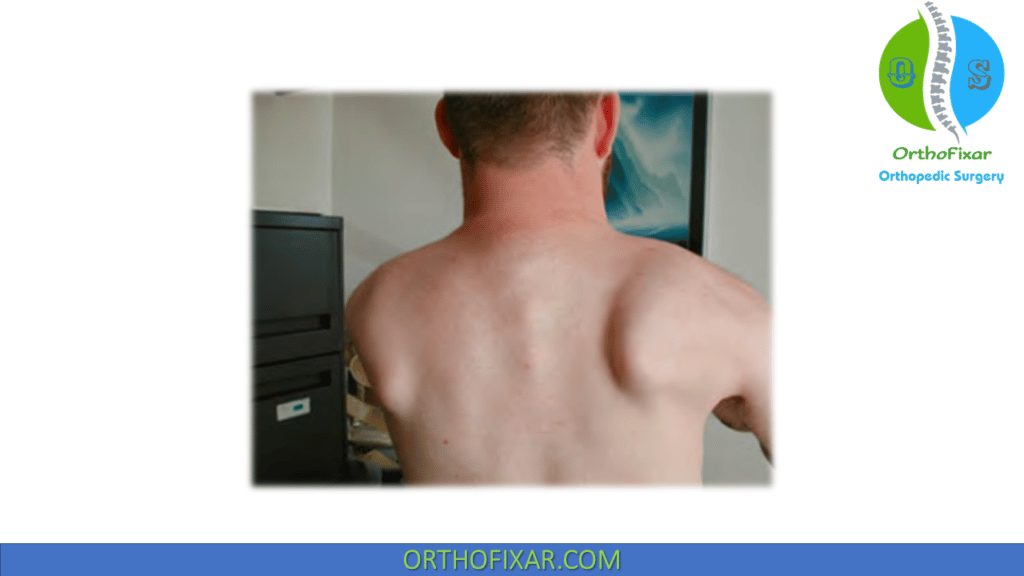
The most striking clinical manifestation is facial weakness with an inability to whistle, purse the lips, wrinkle the brow, or blow out the cheeks. The greatest functional impairments are the inability to abduct and flex the arms at the glenohumeral joints and winging of the scapula, both caused by progressive weakness of the muscles that fix the scapula to the thoracic wall, whereas the muscles that abduct the glenohumeral joint remain strong.
See Also: Scapular Winging Test
With specific reference to the shoulder, patients with fascioscapular muscular dystrophy often display evidence of atrophy and/or hypotonia of the middle and lower divisions of the trapezius muscle which forces the scapulae into significant elevation, protraction, upward rotation. Because the glenoid faces more anteriorly in this type of scapular malposition, the glenohumeral joint almost always assumes a position of increased internal rotation.
However, it is important to recognize that although patients with FSHD have bilateral periscapular weakness, the relative amount of weakness between each shoulder is typically asymmetric. In other words, active forward flexion and abduction of the shoulder in patients with FSHD usually reveals asymmetric scapular winging—a clinical finding which can be used to differentiate between patients with FSHD and those with other types of limb-girdle muscular dystrophies who most often present with symmetric scapular winging.
As the disease progresses, weakness of the lower extremities, especially in the peroneal and the anterior tibial muscles, results in a footdrop that requires the use of an ankle-foot orthosis. Sometimes the quadriceps muscle is involved, requiring expansion of the orthosis to a knee-ankle-foot orthosis. Scoliosis is rare, although increased lumbar lordosis is common.
In a retrospective study by Padberg , approximately 80 % of patients with FSHD initially complained of shoulder girdle weakness, 10 % initially complained of orofacial muscle weakness, and the remaining 10 % initially complained of ankle dorsiflexion weakness (i.e., foot drop). However, physical examination of these patients revealed objective weakness in all three of these muscle groups.
Although the recognition of fascioscapular muscular dystrophy during infancy and early childhood has been reported on occasion, the condition most often goes unrecognized until early adulthood (typically during the second or third decade of life).
Beevor sign is a common finding in patients with facioscapulohumeral dystrophy, even before functional weakness of abdominal wall muscles is apparent, but is absent in patients with other facioscapulohumeral disorders.
See Also: Beevor's sign
FSHD Treatment
The inability to flex and abduct the shoulder functionally usually is treated by stabilization of the scapula, with scapulothoracic arthrodesis.
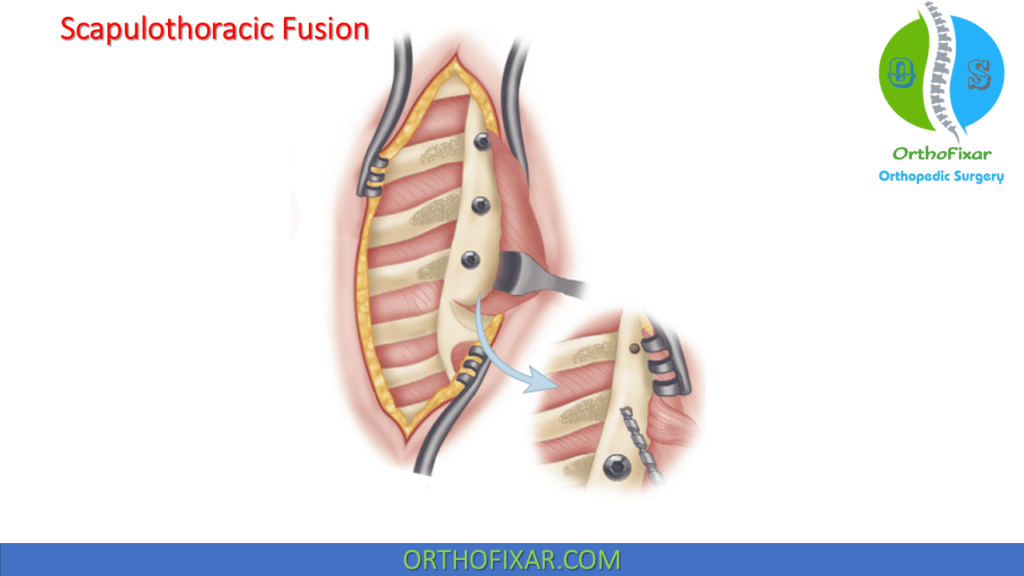
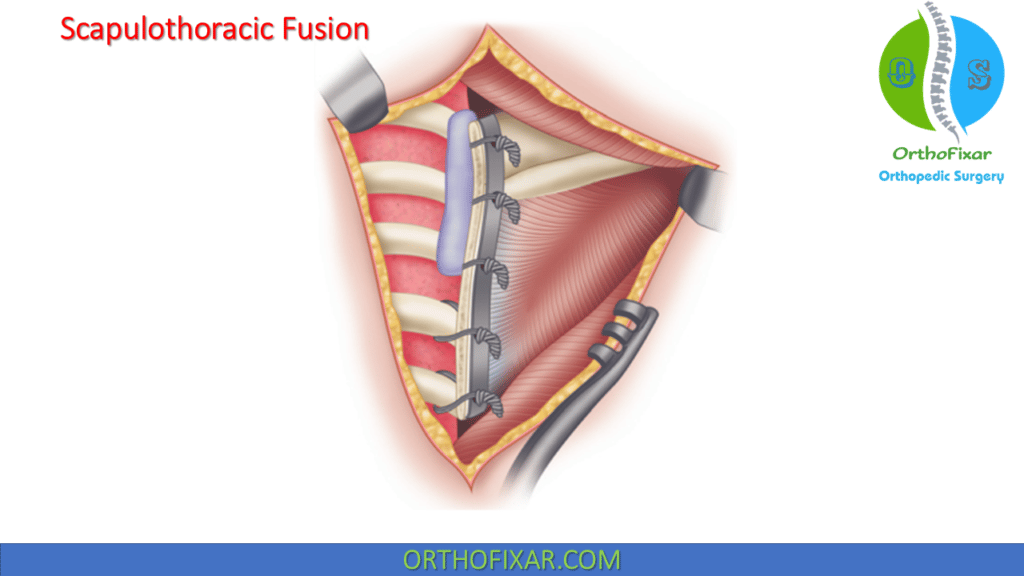
Scapulothoracic Fusion
Scapulothoracic fusion with strut grafts or with plates and screws provides a satisfactory fusion of the medial border of the scapula to the posterior thoracic ribs.
Cited indications for scapulothoracic fusion include:
- limited shoulder abduction and flexion of more than 90 degrees,
- scapular winging,
- shoulder discomfort;
Deltoid strength should be at least grade 4 of 5 at the time of surgery.
Techniques using wires for fixation have been described by Jakab and Gledhill, Twyman et al., and Diab et al. Copeland et al. described a similar fusion technique, but instead of wires they used screws to stabilize the scapula to the fourth, fifth, and sixth ribs.
Scapulothoracic fusion is associated with significant complications, including:
- pneumothorax,
- pleural effusion,
- atelectasis,
- pseudarthrosis.
In their 11 procedures in eight patients, the only complication reported by Diab et al. was prominent subcutaneous wires that required trimming in two patients. They noted that scapulothoracic fusion can relieve shoulder fatigue and pain, allow smooth abduction and flexion of the upper extremity, and improve the appearance of the neck and shoulder.
Although disease progression affecting the deltoid muscle can cause a loss of abduction, other benefits of the procedure are maintained long term.
Infantile Facioscapulohumeral Dystrophy
An early onset form of facioscapulohumeral muscular dystrophy has been described in which weakness is rapidly progressive and the lower extremities also are affected.
Patients become wheelchair bound by the second decade of life. Facial weakness is seen in infancy, and this is followed by sensorineural hearing loss at an average of 5 years of age. A progressive lumbar hyperlordosis develops and is almost pathognomonic for infantile facioscapulohumeral muscular dystrophy. The hyperlordosis leads to fixed hip flexion contractures.
Infantile FSHD treatment consists of accommodation of the lordosis in the wheelchair. Spinal bracing has been unsuccessful. Spinal fusion may be indicated to assist with sitting balance. Scapulothoracic fusion is usually not indicated in these patients because of the advanced weakness associated with this form of facioscapulohumeral muscular dystrophy.
References
- Emery AE. Population frequencies of inherited neuromuscular disease–a world survey. Neuromuscul Disord. 1991;1(1):19–29.
- Flanigan KM, Coffeena CM, Sexton L, Stauffer D, Brunner S, Leppert MF. Genetic characterization of a large, historically significant Utah kindred with FSHD. Neuromuscul Disord. 2001;11(6–7):525–9.
- Padberg GW, Frants RR, Brouwer OF, Wijmenga C, Bakker E, Sandkuijl LA. Facioscapulohumeral muscular dystrophy in the Dutch population. Muscle Nerve Suppl. 1995;2:S81–4.
- Padberg GW. Facioscapulohumeral disease [thesis]. Leiden, Netherlands: Leiden University; 1982.
- Chen TH, Lai YH, Lee PL, Hsu JH, Goto K, Hayashi YK, Nishino I, Lin CW, Shih HH, Huang CC, Liang WC, Wang WF, Jong YJ. Infantile facioscapulohumeral muscaular dystrophy revisited: expansion of clinical phenotypes in patients with a very short EcoRI fragment. Neuromuscul Disord. 2013;23(4):298–305.
- TYLER FH, STEPHENS FE. Studies in disorders of muscle. II Clinical manifestations and inheritance of facioscapulohumeral dystrophy in a large family. Ann Intern Med. 1950 Apr;32(4):640-60. doi: 10.7326/0003-4819-32-4-640. PMID: 15411118.
- Awerbuch GI, Nigro MA, Wishnow R. Beevor’s sign and facioscapulohumeral dystrophy. Arch Neurol. 1990 Nov;47(11):1208-9. doi: 10.1001/archneur.1990.00530110066018. PMID: 2146943.
- Diab M, Darras BT, Shapiro F: Scapulothoracic fusion for facioscapulohumeral muscular dystrophy, J Bone Joint Surg 87A:2267, 2005